At the age of 32, after completing 14 years of training, a surgical registrar at a major Melbourne hospital needed to pass only one more exam to become a surgeon. However, on a Saturday in March 2006, he went into the registrars’ quarters at his hospital and took his own life.1
The medical profession is one with a significant risk of stress,2,3 substance misuse and suicide,4,5 due to the nature of the work. This is combined with the committed, conscientious, obsessive personalities of our medical professionals.6 However, young doctors give their own health care a low priority, and feel great pressure not to miss shifts because of ill health.7
Despite a conference in 2001 focusing on the junior doctor in distress,8 and various programs9,10 to assist impaired doctors (including the Victorian Doctors Health Program11 [VDHP]), a recent national survey of the health and wellbeing of junior doctors outlined existing areas of concern within hospitals. Fifty-four per cent of respondents reported excessive workloads, and 70% reported experiencing high levels of stress. Importantly, 46% believed that their hospital administration was not supportive.12
RMH is the busiest hospital in Australia,13 providing a full range of adult medical specialties (excluding obstetrics and gynaecology), including acute and subacute care, community liaison and mental health facilities. The hospital employs over 500 junior medical staff in intern, hospital medical officer and registrar positions. It complies with safe-hours guidelines,14 accreditation of prevocational15 and vocational training positions,16 and incorporates best-practice recommendations from quality and safety inquiries.13
Junior medical training is challenging, due to the nature of the work,6 pressures of exam preparation17 and maintaining a work–life balance. Significant responsibility is inherent in the work of caring for patients, particularly in life-or-death situations, resulting in significant stress and physical demands.18 The RMH program has targeted modifiable factors that impact on junior staff stress, such as rostering, supervision, and workplace culture. Drug and alcohol use and physical19 and mental illness will also impact on performance, and require prompt identification and referral for appropriate treatment.11 We also acknowledge that some individuals will be more emotionally and physically resilient to the rigours of junior medical life (including the after-hours shifts, broken sleep and physical demands of being on one’s feet for a full shift) than others. We further acknowledge that the most important support mechanisms are not from within the organisation, but involve family, friends and the individual’s general practitioner or other health professional. Thus, an individually tailored program is important. Although the program focuses on junior staff, such principles are also applicable to senior staff.
The program’s preventive strategies generally expand on best-practice medical staff working conditions.14,15 Following the Melbourne registrar’s suicide, awareness of working conditions for medical staff was heightened among RMH hospital board members and executive staff, and this reinforced leadership “buy-in” and accountability.
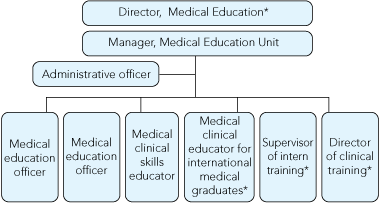
A focus on enhancing and ensuring adequate medical education for junior doctors led to additional staffing appointments in the RMH Medical Education Unit (MEU), the most important of which were the Director of Clinical Training (DCT) and an additional Medical Education Officer (MEO) for individual20 and system-level21 support (Box 1). The program relies heavily on the skills, expertise and personalities of the MEOs, DCT and supervisor of training. The MEU monitors trends and numbers of doctors seeking assistance; assists with planning of preventive programs and resource allocation; and oversees the competency of junior medical staff in liaison with the medical colleges and the Postgraduate Medical Council of Victoria. The MEOs and medical clinical skills educator provide mentoring, pastoral care, clinical skills training and career advice, and assist with designing education programs for junior medical staff. The medical clinical educator for international medical graduates (originally an international graduate), supervisor of intern training and DCT are senior medical staff who perform mentoring and educative roles for junior medical staff. MEU positions are mostly part-time appointments.
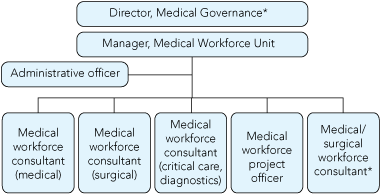
Hospital medical staff are also supported by a Medical Workforce Unit (MWU), with approachable, appropriately trained staff (Box 2). The MWU provides a single, on-site, open-door reference point for medical staff issues (recruitment and appointments, credentialling, safe rostering, and vacancy and leave management) and liaises with human resources personnel to facilitate employment of international medical graduates at RMH via a qualified migration agent. Human resources personnel are also involved in professional behaviour and disciplinary issues. The MWU manager provides peer support and support for industrial and professional issues. Medical workforce consultants and project officers provide a point of accountability and continuity over the junior medical training years and facilitate relationships with medical staff. They are responsible for recruitment, rostering and human resources support for junior and senior medical staff.
Most hospitals have systems for appointments, rostering and performance management, and these new RMH initiatives further support the welfare of young doctors. Safe-hours rostering protects work–life balance, minimises fatigue and decreases stress,22 and proactive leave replacement via a 24-hour on-call MWU prevents excessive overtime and prolonged shifts.5 Specific clinical competence and orientation programs target overseas-trained medical graduates.23 Effective supervision by accountable senior medical staff is essential.24 The hospital provides 24-hour resident quarters with computers and kitchen facilities for those in the hospital after hours.
Ideally, poorly performing junior doctors self-present,25 either directly or indirectly, by requesting roster modifications, career advice or clinical skills training. Usually, however, issues of underperformance20 are identified by a fellow resident, registrar or a consultant supervisor, either during rotations or as part of formal assessments.26 Occasionally, they are identified through complaints from non-medical staff, patients or their families (particularly if there are issues regarding communication27). Notification of professional or impaired-practitioner issues is sometimes made to the Medical Board of Australia (MBA) (formerly to the Medical Practitioners Board of Victoria).28
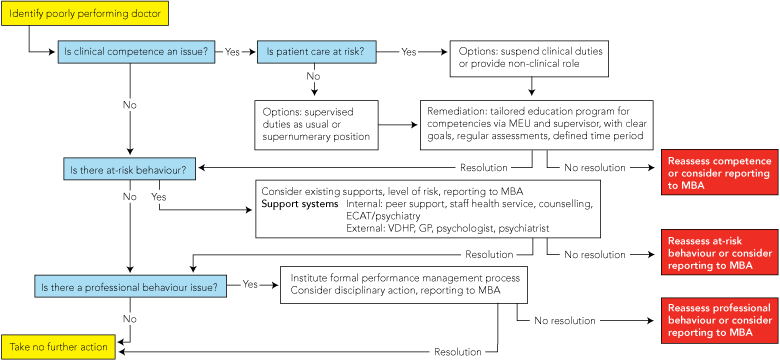
Preferably, junior doctors with performance issues or at-risk behaviour should actively seek assistance and collaborate with the organisation in their rehabilitation and remediation. To facilitate this, certain key questions need to be asked. These include questions about risks to patient safety and to the doctor concerned, and questions about issues of clinical competence and professional behaviour. Differing responses require different support pathways. Confidentiality is essential through all stages of management.29,30 A flowchart of the organisational approach is outlined in Box 3, but each case needs to be tailored to the individual’s needs and may involve one or all of the issues.
While determining the most appropriate pathway for supporting and managing the young doctor, it is essential to determine whether patient safety is at risk. If patient care is not at risk, then the individual can maintain his or her usual role while management and support programs are instituted. If patient care is potentially at risk, then the individual needs strict clinical supervision, or to be removed from clinical duties altogether. This may include removing him or her from night duty or weekend duty when there is limited on-site supervision. Alternative non-clinical duties can be sought for the individual (eg, assisting with quality improvement and clinical risk management initiatives within medical administration). If time away is required, it is important that the doctor returns to work as soon as possible.31 It has been asserted that “there is nothing wrong with doing non-medical work for a while, and it can even assist in the recovery process”.32
Clinical competence issues are coordinated confidentially by the relevant supervisor of training (to ensure appropriate clinical supervision), the MEO (for tailored clinical competence programs) and the MWU (to modify rosters and leave, if required). A clinical learning contract21 based on the Australian Curriculum Framework for Junior Doctors33 is established, with opportunities for self-reflection and supervisor assessment. Individual clinical skills training may also be required. Monthly meetings between MWU and MEU team members track the progress of poorly performing junior medical staff to ensure that current support systems are optimal.
These issues will require assistance from the human resources department for disciplinary action or referral to the MBA. Mandatory reporting of professional incompetence34 is now required under the regulations of the MBA; however, referral to the MBA at any stage may be required for individual or patient safety.
Despite existing supports, junior staff are extremely reluctant to seek assistance for fear of harming future career prospects.35
If junior staff seek assistance, it is often sought privately.
Confidentiality is essential.
Some senior staff still foster an “in-my-day” attitude, which discourages doctors from seeking assistance.
Provenance: Not commissioned; externally peer reviewed.
- Alison J Dwyer1
- Peter Morley1,2
- Esther Reid1
- Cassandra Angelatos1
- 1 Royal Melbourne Hospital, Melbourne Health, Melbourne, VIC.
- 2 Clinical School, University of Melbourne, Melbourne, VIC.
We thank the staff of the Medical Workforce and Medical Education Units and the training supervisors and senior medical staff whose support is critical to the success of the support program. We also thank the Victorian Doctors Health Program for assistance with referred junior medical staff.
Peter Morley receives financial support from the American Heart Association, Melbourne Health, the University of Melbourne and Queensland Health.
- 1. Fyfe M. Young doctors succumb to killing pressures on the ward. The Age (Melbourne) 2006; 13 Sep: 1. http://www.theage.com.au/articles/2006/09/12/1157826941987.html (accessed Apr 2011).
- 2. Schernhammer ES, Colditz GA. Suicide rates among physicians: a quantitative and gender assessment (meta-analysis). Am J Psychiatry 2004; 161: 2295-2302.
- 3. Center C, Davis M, Detre T, et al. Confronting depression and suicide in physicians: a consensus statement. JAMA 2003; 289: 3161-3166.
- 4. Arnetz BB, Hörte LG, Hedberg A, et al. Suicide patterns among physicians related to other academics as well as to the general population. Results from a national long-term prospective study and a retrospective study. Acta Psychiatr Scand 1987; 75: 139-143.
- 5. Essex C. Doctor’s suicide prompts look at hours. BMJ 1994; 309: 1037.
- 6. Riley GJ. Understanding the stresses and strains of being a doctor. Med J Aust 2004; 181: 350-353. <MJA full text>
- 7. Shadbolt NE. Attitudes to healthcare and self-care among junior medical officers: a preliminary report. Med J Aust 2002; 177 (1 Suppl): S19-S20. <MJA full text>
- 8. Dahlenburg GW. Conference overview: a duty of care. Med J Aust 2002; 177 (1 Suppl): S3-S4. <MJA full text>
- 9. Schattner P, Davidson S, Serry N. Doctors’ health and wellbeing: taking up the challenge in Australia. Med J Aust 2004; 181: 348-349. <MJA full text>
- 10. Tennant CC. A student mental health and welfare program in a medical faculty. Med J Aust 2002; 177 (1 Suppl): S9-S10. <MJA full text>
- 11. Warharft N. The Victorian Doctors Health Program: the first 3 years. Med J Aust 2004; 181: 376-379. <MJA full text>
- 12. Markwell AL, Wainer Z. The health and wellbeing of junior doctors: insights from a national survey. Med J Aust 2009; 191: 441-444. <MJA full text>
- 13. Department of Human Services, Victoria. Royal Melbourne Australia’s busiest. Human Services News. Melbourne: DHS, 2008.
- 14. Australian Medical Association. National code of practice: hours of work, shiftwork and rostering for hospital doctors. Sydney: AMA, 2002. http://www.ama.com.au/web.nsf/doc/SHED-5G2UUA (accessed Apr 2011).
- 15. Postgraduate Medical Council of Victoria. Hospital/health service accreditation instruments: Part 2: Assessment against functions & standards. Melbourne: PMCV, 2010. http://www.pmcv.com.au/accreditation/accreditation-visits/accreditation-instruments (accessed Apr 2011).
- 16. Royal Australasian College of Surgeons. Accreditation of hospitals and posts for surgical education and training: process and criteria for accreditation. Melbourne: RACS, 2008. http://www.surgeons.org/racs/education--trainees/training-post-accreditation (accessed Apr 2011).
- 17. Sreeramareddy CT, Shandar PR, Binu VS, et al. Psychological morbidity, sources of stress and coping strategies among undergraduate medical students of Nepal. BMC Med Educ 2007; 7: 26.
- 18. Wilhelm KA. The student and junior doctor in distress. Med J Aust 2002; 177 (1 Suppl): S5-S8. <MJA full text>
- 19. Firth-Cozens J. Doctors, their wellbeing and their stress. BMJ 2003; 326: 670-671.
- 20. Grace K. The junior doctor in distress: the role of a medical education officer at the individual level. Med J Aust 2002; 177 (1 Suppl): S22-S24. <MJA full text>
- 21. Martin AA. The junior doctor in distress: the role of a medical education officer at the systems level. Med J Aust 2002; 177 (1 Suppl): S20-S22. <MJA full text>
- 22. Rasminsky S, Lomonaco A, Auchincloss E. Work hours regulations for house staff in psychiatry: bad or good for residency training? Acad Psychiatry 2008; 32: 54-60.
- 23. Pilotto LS, Duncan GF, Anderson-Wurf J. Issues for clinicians training international medical graduates: a systematic review. Med J Aust 2007; 187: 225-228. <MJA full text>
- 24. Forsyth KD. Critical importance of effective supervision in postgraduate medical education. Med J Aust 2009; 191: 196-197. <MJA full text>
- 25. Tackling stress in ourselves. BMJ 1996; 312: 784.
- 26. Lake FR, Ryan G. Teaching on the run tips 8: assessment and appraisal. Med J Aust 2005; 182: 580-581. <MJA full text>
- 27. Taylor DMcD, Wolfe RS, Cameron PA. Analysis of complaints lodged by patients attending Victorian hospitals 1997–2001. Med J Aust 2004; 181: 31-35. <MJA full text>
- 28. Reid AM. Overview: the experience of the New South Wales Medical Board. Med J Aust 2002; 177 (1 Suppl): S25-S26. <MJA full text>
- 29. Oxley J, Brandon S. Getting help for sick doctors. BMJ 1997; 314: S2-7092.
- 30. Chambers R, Maxwell R. Helping sick doctors. BMJ 1996; 312; 722.
- 31. Armstrong E. Rehabilitating troubled doctors. BMJ 1997; 314: S2-7095.
- 32. Farmer JF. Return to work for junior doctors after ill-health. Med J Aust 2002; 177 (1 Suppl): S27-S29. <MJA full text>
- 33. Graham IS, Gleason AJ, Keogh GW, et al. Australian Curriculum Framework for Junior Doctors. Med J Aust 2007; 186 (7 Suppl): S14-S19. <MJA full text>
- 34. Arnold PC. Mandatory reporting of professional incompetence. Med J Aust 2008; 189: 132-133. <MJA full text>
- 35. Williams LS. Manitoba suicides force consideration of stresses facing medical residents. CMAJ 1997; 156: 1599-1602.





Abstract
Despite “safe-hours” campaigns and doctors health programs, “at-risk” behaviour and suicides still occur in junior doctors.
A recent national survey found that 46% of junior doctors believed that their hospital administration was not supportive.
The Royal Melbourne Hospital has developed a comprehensive program for preventing and identifying at-risk behaviour and supporting junior doctors, tailored to the individual’s needs.
Patient and individual doctor safety is paramount, and confidential collaboration between medical workforce and medical education structures, clinical supervisors and the Victorian Doctors Health Program is required.
The boundaries of the hospital’s “duty of care” for those who do not want assistance is unclear, and balancing increased supervision within a limited workforce is challenging.