The health status of doctors is better than average; like other higher socioeconomic groups, they are less likely than the general population to suffer lifestyle-related illnesses, such as heart and smoking-related disease.1-3 However, they are at greater risk of mental illness and stress-related problems and are more susceptible to the “3 Ds” — depression (including suicide), drink and drugs.4,5
Junior doctors (interns through to completion of training) are a subgroup of the medical profession who may be at greater risk of poorer health. They face specific pressures related to their professional stage and development, including coping with the demands of each new clinical placement, furthering their medical career, and maintaining social and personal networks. Junior doctors do not prioritise their own health care and feel pressured not to miss shifts because of ill health.6 They can be unwilling to admit illness or accept that they are not coping with the demands of their career. This can lead to a failure to recognise, acknowledge and act on the early warning signs of illness.
Recent data on the attitudes of junior doctors to work–life balance suggest that they now are less willing to accept the personal costs traditionally associated with a career in medicine. In response, recent initiatives have endeavoured to improve the support available to junior doctors.7 Medical colleges are providing wellbeing programs for trainees and Fellows, and medical schools increasingly include self-care programs in their curricula.8
The AMA’s junior doctor health survey was adapted from the 2007 Junior Medical Officer Welfare Study (developed by Dr Daniel Heredia, Dr Suzanne English and Ms Sheree Keech, and funded by the Postgraduate Medical Council of Western Australia).9 The 96-item confidential, online, self-reporting survey was conducted between 6 February and 20 April 2008. Junior doctors in postgraduate year 2 and above participated.
The survey assessed several areas related to junior doctors’ health and wellbeing, including:
intention to continue to practise medicine;
perceptions of morale and wellbeing;
career satisfaction;
workload and the working environment;
coping strategies when faced with work-related stress; and
self-care and work–life balance.
The open-source Professional Quality of Life (ProQOL) scale was included in the survey.10 This instrument uses three discrete psychometric scales to determine the prevalence of secondary trauma (compassion fatigue) and burnout, and job satisfaction levels.
Most respondents (98%) indicated they would continue to practise medicine.
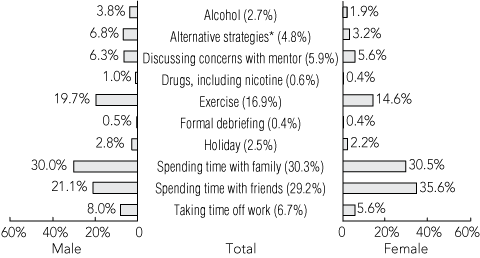
The key findings from the questions on morale, job satisfaction, workload and working environment are summarised in Box 1. A majority of respondents (59%) reported spending time with family or friends as their main coping strategy, and 17% used exercise (Box 2).
This survey confirms that junior doctors have a high level of career satisfaction; however, it is of concern that 38% of respondents indicated that they were not prepared for life as a doctor, and 17% would not choose medicine as a career if they had their time again. This is consistent with 2006 British Medical Association data, which established that 15% of medical graduates had a low desire to practise medicine.11 The coping strategies nominated by most junior doctors were appropriate, although they relied heavily on the ability to maintain relationships, which could leave junior doctors vulnerable if they became isolated through heavy work and study demands.
The ProQOL prevalence figures for burnout, job satisfaction and compassion fatigue are consistent with those reported in other studies, and comparable with an earlier study using a different instrument.4,12-14
That 71% of respondents were concerned about their own health, and 63% were concerned about the health of a colleague, confirms that junior doctors are aware of their health care needs and require access to independent medical care. That said, the survey found that fewer junior doctors (66%) have their own GP compared with the general population (80%).15 The rates of self-medication and prescription probably reflect that junior doctors have difficulty accessing independent medical care, and that the culture of medicine promotes self-care. No formal data are available on the use of doctors’ health advisory services by junior doctors, so the rate of 5% provides a baseline for future reference.
Although adults require between 7 and 9 hours of quality sleep in a 24-hour period, most junior doctors were sleeping 7 hours per night or less.16 Likewise, the Australian National Physical Activity Guidelines recommend that adults do 30 minutes of moderate-intensity physical activity on most days; only about a quarter of survey respondents were able to follow this recommendation.17 As most junior doctors were working up to 60 hours per week (as well as studying), it is not surprising that exercise and sleep are given a low priority.
To address the concerns raised by this survey, the AMA Council of Doctors in Training has put forward a series of recommendations (Box 4) and resolutions (Box 5), which were endorsed by the Federal Council of the AMA in March 2009.18 A poster campaign designed to raise awareness was also launched in October 2008. The full report of the survey is available on the AMA website at <http://www.ama.com.au/node/4217>.
On the basis of this survey, it is clear that the AMA has an ongoing role in
improving the support provided to doctors;
undertaking further research into the health and wellbeing of junior doctors; and
ensuring that systematic problems contributing to doctors’ poor health are rectified and the inherent risks mitigated.
1 General experience as a doctor
38% believed that medical school had not prepared them for life as a doctor; and 17% admitted that, given their time again, they would not have studied medicine
45% felt that working as a doctor was what they had expected it to be
77% enjoyed working as a doctor, and 73% were looking forward to working as a doctor that year
54% reported their workload had been excessive; 53% believed that an adverse event could occur as a result of their high workload; and 41% believed that their workload compromised patient safety
70% had experienced high levels of stress at work; 56% had been concerned about the welfare of their colleagues because of the working conditions; and 31% believed that they regularly worked unsafe hours
3 Junior doctors’ work–life balance
97% worked full-time; of the 3% working part-time, 65% were women
76% worked 41–60 hours per week; half (49% female, 53% male respondents) had worked an average of ≥ 50 hours per week during the previous year
23% had taken ≤ 1 week and 67% had taken ≤ 4 weeks’ annual leave in the previous year. Reasons cited included lack of cover (20%), more leave not being sought (20%), insufficient leave accrued, or a change in employment
76% had taken < 1 week of personal leave; respondents were more likely to take leave for their own health (84%) than to care for others (35%)
4 Recommendations from the Australian Medical Association (AMA) Council of Doctors in Training18*
take responsibility for their own physical and psychological health
establish a continuing relationship with a general practitioner they trust
incorporate regular leave, good nutrition, exercise, leisure and family time into a healthy and balanced lifestyle
recognise there are dangers to others associated with (i) a reluctance to admit illness or failing competence, and (ii) continued or regular self-medication and prescribing
To support junior doctors — hospitals, medical colleges, medical boards and government should:
promote good health and the adoption of a healthy lifestyle for junior doctors throughout their medical training and career
ensure access to confidential and high-quality medical and health services
establish professional debriefing, support and mentorship
identify internal and/or external stress factors contributing to, and recognise the warning signs and behaviour patterns of, poor health in junior doctors
promote access to early and expert assistance from professional services and providers
incorporate skills such as stress and time management into continuing medical education
establish clear referral pathways for junior doctors in need of assistance
adopt a “no-blame” culture that supports those in difficulty, so that junior doctors are confident that seeking help will not damage their career progression
ensure that the training and workplace environment does not adversely affect a doctor’s health, conduct or performance, which in turn could place patients at risk
implement and support safe rostering practices† and safe working hours
* Adapted from the AMA position statement, The health and wellbeing of medical students and practitioners — 2006.18
† The AMA publication, National code of practice. Hours of work, shiftwork and rostering for hospital doctors, provides guidance on safe rostering practice.19
- Alexandra L Markwell1
- Zoe Wainer2
- Australian Medical Association Council of Doctors in Training, Canberra, ACT.
The survey was funded by the AMA and undertaken with the assistance and support of the AMA Federal Secretariat. We thank the doctors in training who completed the survey, and acknowledge the ongoing support and inspiration of the Council of Doctors in Training. We also thank Professor Tony Brown for his editorial input in the development of this article.
Alexandra Markwell, as a former board member of the Federal AMA, has received an allowance and travel assistance to attend meetings on behalf of the AMA. Work on this survey was undertaken on behalf of the AMA. She has received travel assistance from the Medical Council of Tasmania to present at their conference, and from Queensland Health to present the survey results at the International Doctors’ Health Conference in London, 2008.
- 1. Balarajan R. Inequalities in health within the health sector. BMJ 1989; 299: 822-825.
- 2. Carpenter L, Swerdlow A, Fear N. Mortality of doctors in different specialties: findings from a cohort of 20 000 NHS hospital consultants. Occup Environ Med 1997; 54: 388-395.
- 3. Clode D. The conspiracy of silence: emotional health among medical practitioners. Melbourne: Royal Australian College of General Practitioners, 2004.
- 4. Willcock SM, Daly MG, Tennant CC, Allard BJ. Burnout and psychiatric morbidity in new medical graduates. Med J Aust 2004; 181: 357-360. <MJA full text>
- 5. Schattner P, Davidson S, Serry N. Doctors’ health and wellbeing: taking up the challenge in Australia. Med J Aust 2004; 181: 348-349. <MJA full text>
- 6. Shadbolt NE. Attitudes to healthcare and self-care among junior medical officers: a preliminary report. Med J Aust 2002; 177 (1 Suppl): S19-S20. <MJA full text>
- 7. Australian Medical Association. Work–life flexibility survey: report of findings. Canberra: AMA, 2008. http://www.ama.com.au/node/4168 (accessed Aug 2009).
- 8. Hassed C, de Lisle S, Sullivan G, Pier C. Enhancing the health of medical students: outcomes of an integrated mindfulness and lifestyle program. Adv Health Sci Educ Theory Pract 2009; 14: 387-398.
- 9. Heredia D, English S, Keech S. The JMO welfare study: a snapshot of intern life in Western Australia. Presented at the Inaugural Australian Postgraduate Medical Education and Training Forum: anzMET; 2007 Oct 28–31; Sydney, Australia.
- 10. Stamm B. The ProQOL manual. The professional quality of life scale: compassion satisfaction, burnout and compassion fatigue/secondary trauma scales. Lutherville, Md: Sidran Press, 2005.
- 11. British Medical Association. Health Policy and Economic Research Unit. The cohort study of 2006 medical graduates. First report. Chap 4, Interest in medicine. London: BMA, 2007: 14. http://www.cardiff.ac.uk/pgmde/resources/BMA-CohortStudyFirstReport.pdf (accessed Aug 2009).
- 12. Heredia D, English S, Keech S, Van Graan A. The 2007 JMO welfare study: a snapshot of intern life in Western Australia. Presented at the 13th National Prevocational Medical Education Forum; 2008 Nov 9–12; Hobart, Australia.
- 13. Honeyball F, Lee MY. The national JMO welfare study: a NSW perspective. Presented at the 13th National Prevocational Medical Education Forum; 2008 Nov 9–12; Hobart, Australia.
- 14. Law D, McElrea A, Heredia D. Life as an intern in Queensland Health: the 2008 Junior Medical Officer Welfare Study. Poster presented at the 13th National Prevocational Medical Education Forum; 2008 Nov 9–12; Hobart, Australia.
- 15. Magnus P, Killion S, editors. Australia’s health 2008. The eleventh biennial health report of the Australian Institute of Health and Welfare. Canberra: AIHW, 2008. (AIHW Cat. No. AUS 99.)
- 16. Ferrara M, De Gennaro L. How much sleep do we need? Sleep Med Rev 2001; 5: 155-179.
- 17. Australian Government Department of Health and Ageing. The National Physical Activity Guidelines for Australians. Canberra: DoHA, 2007.
- 18. Australian Medical Association. Position statement. The health and wellbeing of medical students and practitioners — 2006. Canberra: AMA, 2006. http://www.ama.com.au/node/2553 (accessed Aug 2009).
- 19. Australian Medical Association. National code of practice. Hours of work, shiftwork and rostering for hospital doctors. Canberra: AMA, 2002. http://www.ama.com.au/node/3756 (accessed Aug 2009).





Abstract
Junior doctors face specific pressures related to their professional stage and development and can be at risk of poor health.
A confidential survey conducted in 2008 by the Australian Medical Association Council of Doctors in Training investigated the health and wellbeing of junior doctors.
There were 914 completed surveys: 71% of junior doctors were concerned about their own health, and 63% about the health of a colleague.
A majority of junior doctors met well established criteria for low job satisfaction (71%), burnout (69%) and compassion fatigue (54%).
The early stages of a medical career are demanding, and the health and wellbeing of junior doctors must be a personal priority, as well as the responsibility of the medical profession in general, to ensure a healthy medical workforce in the future.