Rates of chronic suppurative otitis media (CSOM) among Aboriginal children living in remote areas in Australia are the highest in the world.1,2 A survey of 29 Aboriginal communities in the Northern Territory found that 40% of children had a tympanic membrane perforation (TMP) by 18 months of age.3 About 50%–80% of Aboriginal children with CSOM suffer from moderate to severe hearing loss.4,5 This occurs while language and speech are developing and may persist throughout primary school.
There is evidence suggesting that the recommended treatment for ear discharge (twice-daily cleaning and topical ciprofloxacin) can produce cure rates of 70%–90%.6-8 However, a study of Aboriginal children with CSOM in the NT found that less than 30% of children had resolution of ear discharge after 8 weeks of similar treatment.9 This study suggested that ongoing treatment for long periods was difficult for many Aboriginal families living in underresourced and stressful conditions. When children in high-risk communities do not receive appropriate medical treatment for ear disease, using swimming pools to limit levels of ear discharge and possibly reduce bacterial transmission becomes an attractive option.
Traditionally, children with perforated eardrums have been restricted from swimming because of fears of infection. However, it is hypothesised that swimming helps cleanse discharge from the middle ear, nasopharynx and hands and that this benefit may outweigh the risk of introducing infection. Several observational studies have examined the relationship between swimming and levels of skin and ear disease among Aboriginal children.10-14 In a cross-sectional survey, close proximity to a swimming area was associated with reductions of up to 40% in otitis media.10 Two systematic reviews have found that swimming without ear protection does not affect rates of recurrent ear discharge in children with tympanostomy tubes (grommets).15,16 Despite these findings, surveys indicate uncertainty among clinicians regarding water precautions for children with grommets.17-19
Our aim was to conduct a randomised controlled trial (RCT) to better understand the impact of swimming on children with CSOM, and to address a lack of data on ear discharge in older Aboriginal children (aged 5–12 years) with CSOM. We also aimed to obtain microbiological profiles of the nasopharynx and middle ear to help elucidate the cleansing hypothesis.
Swabs were taken from the nasopharynx and middle ear at both the baseline and final ear examinations. All swabs were cultured on selective media for respiratory bacteria. The bacteria specifically targeted were Streptococcus pneumoniae, non-typeable Haemophilus influenzae, Moraxella catarrhalis and Staphylococcus aureus. Ear discharge swabs were also cultured for Streptococcus pyogenes (Group A Streptococcus), Pseudomonas aeruginosa and Proteus spp.
Swabs stored in skim-milk tryptone glucose glycerol broth20 were thawed and mixed, and 10 μL aliquots were cultured on the following plates: full chocolate agar, 5% horse blood agar containing colistin and nalidixic acid, and chocolate agar with bacitracin, vancomycin, and clindamycin (Oxoid Australia). Ear discharge swabs were also cultured on MacConkey agar plates. Blood plates were incubated at 37°C in 5% CO2, and MacConkey plates at 35°C in air. Bacterial isolates were identified according to standard laboratory procedures.
The density of each of the bacteria on each plate was categorised as: 1) < 20; 2) 20–49; 3) 50–100; 4) > 100 or confluent in the primary inoculum; 5) as for 4, but colonies also in second quadrant of the plate; 6) as for 5, but colonies also in third quadrant; 7) as for 6, but colonies also in fourth quadrant. Dichotomous measures for bacterial load were categorised as low density (< 100 colonies) or high density (≥ 100 colonies).
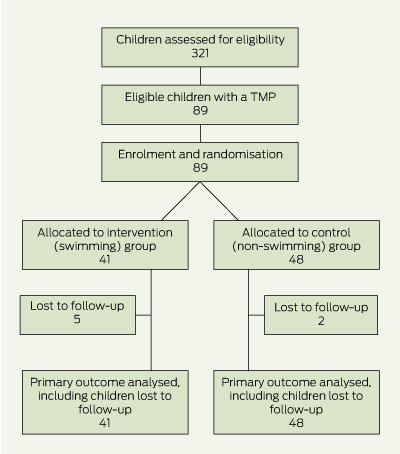
Parental consent was obtained for 89 eligible children: 41 children in the swimming group and 48 children in the non-swimming group (Box 1). At 4-week follow-up, final ear examinations were conducted on 82 children (36 swimmers and 46 non-swimmers).
At baseline, the study groups were similar in age, sex, perforation size, the presence and degree of ear discharge, and the prevalences of ear diagnoses (Box 2). Although there were no statistically significant differences in the baseline prevalence of bacteria in the nasopharynx or middle ear, swimmers had lower rates of H. influenzae in the nasopharynx and higher rates of S. aureus in both the nasopharynx and middle ear. Of the 89 children, 58 (26 swimmers and 32 non-swimmers) had ear discharge at baseline.
At 4-week follow-up, 56 children had ear discharge: 24 of 41 swimmers compared with 32 of 48 non-swimmers (RD, − 8%; 95% CI, − 28% to 12%). Excluding children lost to follow-up, 21 of 36 swimmers had ear discharge compared with 31 of 46 non-swimmers (RD, − 9%; 95% CI, − 30% to 12%).
Between baseline and 4-week follow-up, there was no statistically significant change in the prevalence of bacteria in the nasopharynx (Box 2). P. aeruginosa infection in the middle ear increased in swimmers, compared with no change in non-swimmers. Non-typeable H. influenzae isolated from ear discharge increased in both groups. Overall, the dominant organisms were S. pneumoniae and H. influenzae in the nasopharynx, and H. influenzae, S. aureus and P. aeruginosa in the middle ear.
Per-protocol analysis of swimmers attending > 75% of swimming classes and non-swimmers adhering to swimming restrictions > 75% of the time indicated that 16 of 24 swimmers had ear discharge at 4-week follow-up, compared with 29 of 44 non-swimmers (RD, 1%; 95% CI, − 23% to 23%).
Rates of discharge were significantly lower in children who were prescribed ciprofloxacin and in children with smaller perforations (Box 3).
Of the 89 children, 65 had no change from their original diagnosis (by child’s worst ear) at 4-week follow-up. Ear discharge failed to resolve in 31 of the 35 participants with moderate to profuse ear discharge at baseline (Box 3). Seven of the 89 children had a perforation that healed (Box 4).
We found that regular swimming in a chlorinated pool for 4 weeks did not aid resolution of ear discharge in Aboriginal children with CSOM. At the end of the trial, rates of ear discharge were similar between swimmers and non-swimmers. Our microbiological data also suggest that swimming is unlikely to be effective in removing discharge from the middle ear and nasopharynx, with rates and densities of organisms generally comparable between swimmers and non-swimmers, with little change during the study. Among swimmers, there was an increase in P. aeruginosa middle ear infection, but this was not correlated with new episodes of ear discharge.
Our study is the first RCT to examine the effects of swimming on Aboriginal children with CSOM and also addresses the need for more RCTs examining the impact of swimming on children with grommets. Further, the microbiological data enabled an assessment of the effect of regular swimming on infection in the nasopharynx and middle ear. Other strengths include the blinding of examiners, prespecified subgroup analysis and a follow-up rate of more than 90%.
Our study also has some limitations. We planned to randomly assign 100 children and anticipated that 90% of participants would have ear discharge at follow-up, but we had only 89 participants and 63% with discharge at follow-up, meaning the study was underpowered. Some difficulties were encountered in recruiting children who did not attend school in one community. The possibility of contamination among non-swimmers was also a concern. Parents and school and pool staff assisted in ensuring that non-swimmers did not swim at the pool or at any other water sites, and alternative activities were provided for non-swimmers after school, as this was a popular swimming time. Attendance at swimming and activity classes were monitored, and two portable media players were offered as incentives to children with the highest attendance.
The lack of objective measures for the degree of discharge, perforation size and bacterial density may have contributed to measurement error. It is unlikely that these limitations would prevent a large clinical effect being identified. However, our small sample size means that modest benefits or harms associated with daily swimming may still be possible.
Our results are not consistent with research from two remote communities in Western Australia, which found that rates of TMPs among Aboriginal children halved from about 30% to 15% after swimming pools were installed.11 The potential to improve on our results with longer exposure to swimming is possible. However, the WA study did not follow individual children, and after 5 years the reductions were sustained in only one community.14 Further, the likelihood of significant clinical improvements over a longer period is not supported by our microbiological data. A recent South Australian study also found that the installation of swimming pools in six communities did not affect rates of TMPs among children.12
While swimming may remove some ear and nasal discharge, there is evidence to suggest that cleansing practices alone will not cure CSOM. A Cochrane review of studies conducted in developing countries found that wet irrigation or dry mopping was no more effective than no treatment in resolving ear discharge in children with CSOM (odds ratio, 0.63; 95% CI, 0.36–1.12).21 The review recommended that aural cleansing should be conducted in conjunction with topical antibiotic therapy.21 Future studies could look at the effectiveness of swimming in combination with the application of topical antibiotic therapy.
Over the 4 weeks of our intervention, rates of H. influenzae middle ear infection substantially increased in both swimmers (from 35% to 70%) and non-swimmers (from 50% to 65%). Previous topical antibiotic trials of Aboriginal children (aged 1–16 years) have reported lower baseline rates of H. influenzae in the middle ear, ranging from 5% to 25%.6,9 In contrast, a vaccination trial of Aboriginal infants aged < 24 months found H. influenzae in 85% of new perforations.22 The high levels of H. influenzae ear and nasopharyngeal infection may mean that there is a role for the use of oral antibiotics in combination with topical antibiotics to treat Aboriginal children with CSOM. There may also be benefits from vaccines against H. influenzae in Aboriginal children at high risk of progressing to CSOM.
Simultaneous hand contamination and nasal carriage of S. pneumoniae and H. influenzae is a reliable indicator of TMP in Aboriginal children under 4 years of age.23 Future research could examine rates of hand contamination in relation to swimming, particularly targeting younger children (aged 2–5 years), who are most likely to transmit otitis media bacteria to infants.
In conclusion, it seems unlikely that regular swimming in pools will resolve ear discharge and heal TMPs in the short term. We also found no clear indication that swimming reduces rates of respiratory and opportunistic bacteria in the nasopharynx or middle ear. However, we did not find swimming to be associated with an increased risk of ear discharge. We would not support the practice of restricting children with a TMP from swimming unless it was documented that ear discharge developed directly after swimming (for that particular child). More RCTs are needed to assess more modest (or longer-term) effects of swimming on middle ear disease in Aboriginal children. The combination of swimming and ciprofloxacin treatment may also produce better clinical outcomes and should be investigated.
2 Participant characteristics at baseline and 4-week follow-up
|
Baseline |
Follow-up |
|||||||||||||
|
Swimmers (n = 41) |
Non-swimmers (n = 48) |
Swimmers (n = 41) |
Non-swimmers (n = 48) |
Risk difference (95% CI)* |
||||||||||
Mean age in years (SD) |
8.9 (2.4) |
8.6 (1.9) |
— |
— |
|
||||||||||
Male |
27 (66%) |
31 (65%) |
— |
— |
|
||||||||||
Ear diagnosis |
n = 41 |
n = 48 |
n = 41† |
n = 48† |
|
||||||||||
Bilateral closed tympanic membranes |
— |
— |
1/41 (2%) |
6/48 (13%) |
− 10% (− 23% to 2%) |
||||||||||
Unilateral dry TMP |
11/41 (27%) |
11/48 (23%) |
11/41 (27%) |
5/48 (10%) |
16% (0 to 33%) |
||||||||||
Bilateral dry TMPs |
4/41 (10%) |
5/48 (10%) |
5/41 (12%) |
5/48 (10%) |
2% (− 12% to 17%) |
||||||||||
Unilateral wet TMP |
12/41 (29%) |
13/48 (27%) |
10/41 (24%) |
12/48 (25%) |
− 1% (− 18% to 18%) |
||||||||||
Wet TMP and dry TMP |
2/41 (5%) |
2/48 (4%) |
5/41 (12%) |
5/48 (10%) |
2% (− 12% to 17%) |
||||||||||
Bilateral wet TMPs |
12/41 (29%) |
17/48 (35%) |
9/41 (22%) |
15/48 (31%) |
− 9% (− 27% to 10%) |
||||||||||
Median size of TMP as percentage of pars tensa (IQR) |
20% (8%–38%) |
18% (6%–40%) |
15% (4%–32%) |
20% (5%–49%) |
P = 0.39 |
||||||||||
Any ear discharge (primary outcome) |
26/41 (63%) |
32/48 (67%) |
24/41 (59%) |
32/48 (67%) |
− 8% (− 28% to 12%) |
||||||||||
Moderate or profuse discharge |
16/41 (39%) |
19/48 (40%) |
20/41 (49%) |
25/48 (52%) |
− 3% (− 24% to 17%) |
||||||||||
Nasopharyngeal bacteria |
n = 41 |
n = 46‡ |
n = 35‡ |
n = 41‡ |
|
||||||||||
Streptococcus pneumoniae |
28/41 (68%) |
33/46 (72%) |
19/35 (54%) |
27/41 (66%) |
− 12% (− 33% to 1%) |
||||||||||
Non-typeable Haemophilus influenzae |
17/41 (41%) |
28/45 (62%) |
21/35 (60%) |
30/41 (73%) |
− 13% (− 34% to 8%) |
||||||||||
Moraxella catarrhalis§ |
17/40 (43%) |
17/46 (37%) |
6/35 (17%) |
14/41 (34%) |
− 17% (− 36% to 3%) |
||||||||||
Any respiratory pathogen |
28/41 (68%) |
41/46 (89%) |
24/35 (69%) |
37/41 (90%) |
− 22% (− 40% to − 4%) |
||||||||||
Staphylococcus aureus |
8/41 (20%) |
5/46 (11%) |
9/35 (26%) |
4/41 (10%) |
16% (− 1% to 34%) |
||||||||||
At least one high-density respiratory pathogen§ |
17/35 (49%) |
23/43 (53%) |
16/35 (46%) |
16/41 (39%) |
7% (− 15% to 28%) |
||||||||||
Middle ear bacteria |
n = 24‡ |
n = 30‡ |
n = 23‡ |
n = 32‡ |
|
||||||||||
Streptococcus pneumoniae§ |
1/24 (4%) |
4/30 (13%) |
0/23 |
2/32 (6%) |
− 6% (− 20% to 9%) |
||||||||||
Non-typeable Haemophilus influenzae |
8/23 (35%) |
14/28 (50%) |
16/23 (70%) |
20/31 (65%) |
5% (− 21% to 29%) |
||||||||||
Moraxella catarrhalis§ |
0/22 |
0/29 |
1/21 (5%) |
0/31 |
5% (− 4% to 14%) |
||||||||||
Staphylococcus aureus |
8/24 (33%) |
5/30 (17%) |
8/23 (35%) |
4/32 (13%) |
22% (0 to 45%) |
||||||||||
Group A Streptococcus |
3/24 (13%) |
1/30 (3%) |
5/23 (22%) |
2/32 (6%) |
15% (− 3% to 37%) |
||||||||||
Pseudomonas aeruginosa |
3/24 (13%) |
10/30 (33%) |
10/23 (43%) |
10/32 (31%) |
12% (− 13% to 37%) |
||||||||||
Proteus spp. |
3/24 (13%) |
2/30 (7%) |
2/23 (9%) |
2/32 (6%) |
2% (− 13% to 22%) |
||||||||||
TMP = tympanic membrane perforation. IQR = interquartile range. * Unless otherwise indicated. † Includes children lost to follow-up, whose diagnoses were assumed not to have changed from baseline. ‡ Denominators are reduced due to children lost to follow-up, children refusing to have swab taken, or swab being damaged in transportation. § Some plates were contaminated by Proteus spp. |
|||||||||||||||
3 Children with ear discharge at final ear examination, by subgroup at baseline
|
Overall |
Swimmers |
Non-swimmers |
Risk difference (95% CI) |
|||||||||||
All children with ear discharge at final ear examination |
56/89 (63%) |
24/41 (59%) |
32/48 (67%) |
− 8% (− 28% to 12%) |
|||||||||||
Subgroup |
|
|
|
|
|||||||||||
Aged 5–7 years |
14/24 (58%) |
6/11 (55%) |
8/13 (62%) |
− 7% (− 44% to 31%) |
|||||||||||
Aged 8–12 years |
42/65 (65%) |
18/30 (60%) |
24/35 (69%) |
− 9% (− 31% to 15%) |
|||||||||||
Not prescribed topical ciprofloxacin |
46/67 (69%) |
20/30 (67%) |
26/37 (70%) |
− 4% (− 26% to 18%) |
|||||||||||
Prescribed topical ciprofloxacin |
10/22 (45%) |
4/11 (36%) |
6/11 (55%) |
− 18% (− 54% to 23%) |
|||||||||||
Nil discharge |
9/31 (29%) |
3/15 (20%) |
6/16 (38%) |
− 18% (− 47% to 15%) |
|||||||||||
Scant discharge |
16/23 (70%) |
5/10 (50%) |
11/13 (85%) |
− 35% (− 66% to 4%) |
|||||||||||
Moderate or profuse discharge |
31/35 (89%) |
16/16 (100%) |
15/19 (79%) |
− 21% (− 1% to 44%) |
|||||||||||
Small (< 25%) perforation |
19/49 (39%) |
9/24 (38%) |
10/25* (40%) |
− 3% (− 29% to 24%) |
|||||||||||
Large (≥ 25%) perforation |
35/38 (92%) |
15/17 (88%) |
20/21 (95%) |
− 7% (− 31% to 13%) |
|||||||||||
* Perforation size was not estimated for two children in the non-swimming group at baseline. |
|||||||||||||||
4 Change in diagnosis (by child’s worst ear) from baseline to final ear examination
Outcome |
Overall (n = 89) |
Swimmers (n = 41) |
Non-swimmers (n = 48) |
||||||||||||
Dry TMP to closed tympanic membrane |
4 (5%) |
1 (2%) |
3 (6%) |
||||||||||||
Dry TMP to dry TMP |
18 (20%) |
11 (27%) |
7 (15%) |
||||||||||||
Dry TMP to wet TMP |
9 (10%) |
3 (7%) |
6 (13%) |
||||||||||||
Wet TMP to closed tympanic membrane |
3 (3%) |
0 |
3 (6%) |
||||||||||||
Wet TMP to dry TMP |
8 (9%) |
5 (12%) |
3 (6%) |
||||||||||||
Wet TMP to wet TMP |
47 (53%) |
21 (51%) |
26 (54%) |
||||||||||||
Improved |
15 (17%) |
6 (15%) |
9 (19%) |
||||||||||||
Same |
65 (73%) |
32 (78%) |
33 (69%) |
||||||||||||
Got worse |
9 (10%) |
3 (7%) |
6 (13%) |
||||||||||||
TMP = tympanic membrane perforation. |
|||||||||||||||
Received 24 April 2013, accepted 15 June 2013
- Anna T N Stephen1
- Amanda J Leach2
- Peter S Morris3
- Child Health Division, Menzies School of Health Research, Royal Darwin Hospital, Darwin, NT.
The Sidney Myer Fund and National Health and Medical Research Council provided funding for our study. We thank families and children who participated in the study, the NT Department of Health and Families, the community health boards, NT Catholic Education, staff at Murrupurtiyanuwu Catholic Primary School (Nguiu) and Our Lady of the Sacred Heart Thamarrurr Catholic College (Wadeye), pool staff at Wadeye and Nguiu, and Swimming NT. We also thank the following collaborators for their contributions to the field and laboratory data collection and analysis: Joseph McDonnell (statistical analysis), Christine Cooper, Christine Wigger (ear examiners), Kim Hare and Vanya Hampton (laboratory scientists) and Jemima Beissbarth (data management).
Amanda Leach receives funding from Wyeth/Pfizer and GlaxoSmithKline Australia. Peter Morris receives funding from GlaxoSmithKline Australia.
- 1. Leach AJ. Otitis media in Australian Aboriginal children: an overview. Int J Pediatr Otorhinolaryngol 1999; 49 Suppl 1: S173-S178.
- 2. Coates HL, Morris PS, Leach AJ, Couzos S. Otitis media in Aboriginal children: tackling a major health problem [editorial]. Med J Aust 2002; 177: 177-178. <MJA full text>
- 3. Morris PS, Leach AJ, Silberberg P, et al. Otitis media in young Aboriginal children from remote communities in Northern and Central Australia: a cross-sectional survey. BMC Pediatr 2005; 5: 27.
- 4. McPherson B. Hearing loss in Australian Aborigines: a critical evaluation. Aust J Audiol 1990; 12: 67-68.
- 5. Morris PS. Management of otitis media in a high risk population. Aust Fam Physician 1998; 27: 1021-1029.
- 6. Couzos S, Lea T, Mueller R, et al. Effectiveness of ototopical antibiotics for chronic suppurative otitis media in Aboriginal children: a community-based, multicentre, double-blind randomised controlled trial. Med J Aust 2003; 179: 185-190. <MJA full text>
- 7. Miro N. Controlled multicenter study on chronic suppurative otitis media treated with topical applications of ciprofloxacin 0.2% solution in single-dose containers or combination of polymyxin B, neomycin, and hydrocortisone suspension. Otolaryngol Head Neck Surg 2000; 123: 617-623.
- 8. Wintermeyer SM, Hart MC, Nahata MC. Efficacy of ototopical ciprofloxacin in pediatric patients with otorrhea. Otolaryngol Head Neck Surg 1997; 116: 450-453.
- 9. Leach A, Wood Y, Gadil E, et al. Topical ciprofloxin versus topical framycetin-gramicidin-dexamethasone in Australian aboriginal children with recently treated chronic suppurative otitis media: a randomized controlled trial. Pediatr Infect Dis J 2008; 27: 692-698.
- 10. Hudson HM, Rockett IR. An environmental and demographic analysis of otitis media in rural Australian Aborigines. Int J Epidemiol 1984; 13: 73-82.
- 11. Lehmann D, Tennant MT, Silva DT, et al. Benefits of swimming pools in two remote Aboriginal communities in Western Australia: intervention study. BMJ 2003; 327: 415-419.
- 12. Sanchez L, Carney S, Estermann A, et al. An evaluation of the benefits of swimming pools for the hearing and ear health status of young Indigenous Australians: a whole-of-population study across multiple remote Indigenous communities. Adelaide: Flinders University, 2012.
- 13. Carapetis JR, Johnston F, Nadjamerrek J, Kairupan J. Skin sores in Aboriginal children. J Paediatr Child Health 1995; 31: 563.
- 14. Lehmann D, Alpers K, Stephen A. Impact of swimming pools in remote Aboriginal communities in Western Australia. Public Health Bulletin SA 2010; 7 (3): 32-37.
- 15. Carbonell R, Ruiz-Garcia V. Ventilation tubes after surgery for otitis media with effusion or acute otitis media and swimming. Systematic review and meta-analysis. Int J Pediatr Otorhinolaryngol 2002; 66: 281-289.
- 16. Lee D, Youk A, Goldstein NA. A meta-analysis of swimming and water precautions. Laryngoscope 1999; 109: 536-540.
- 17. Davison MJ, Fields MJ. Ventilation tubes, swimming and otorrhoea: a New Zealand perspective. N Z Med J 1993; 106: 201-203.
- 18. Derkay CS, Shroyer MN, Ashby J. Water precautions in children with tympanostomy tubes. Am J Otolaryngol 1992; 13: 301-305.
- 19. Poss JM, Boseley ME, Crawford JV. Pacific Northwest survey: posttympanostomy tube water precautions. Arch Otolaryngol Head Neck Surg 2008; 134: 133-135.
- 20. O’Brien KL, Nohynek H; World Health Organization Pneumococcal Vaccine Trials Carriage Working Group. Report from a WHO Working Group: standard method for detecting upper respiratory carriage of Streptococcus pneumoniae. Pediatr Infect Dis J 2003; 22: e1-e11.
- 21. Macfadyen CA, Acuin JM, Gamble C. Systemic antibiotics versus topical treatments for chronically discharging ears with underlying eardrum perforations. Cochrane Database Syst Rev 2006; (1): CD005608.
- 22. Mackenzie GA, Carapetis JR, Leach AJ, Morris PS. Pneumococcal vaccination and otitis media in Australian Aboriginal infants: comparison of two birth cohorts before and after introduction of vaccination. BMC Pediatr 2009; 9: 14.
- 23. Stubbs E, Hare K, Wilson C, et al. Streptococcus pneumoniae and noncapsular Haemophilus influenzae nasal carriage and hand contamination in children: a comparison of two populations at risk of otitis media. Pediatr Infect Dis J 2005; 24: 423-428.





Abstract
Objectives: To measure the impact of 4 weeks of daily swimming on rates of ear discharge among Aboriginal children with a tympanic membrane perforation (TMP) and on the microbiology of the nasopharynx and middle ear.
Design, setting and participants: A randomised controlled trial involving 89 Aboriginal children (aged 5–12 years) with a TMP, conducted in two remote Northern Territory Aboriginal communities from August to December 2009.
Intervention: 4 school weeks of daily swimming lessons (45 minutes) in a chlorinated pool.
Main outcome measures: Proportions of children with ear discharge and respiratory and opportunistic bacteria in the nasopharynx and middle ear.
Results: Of 89 children randomly assigned to the swimming or non-swimming groups, 58 (26/41 swimmers and 32/48 non-swimmers) had ear discharge at baseline. After 4 weeks, 24 of 41 swimmers had ear discharge compared with 32 of 48 non-swimmers (risk difference, − 8% (95% CI, − 28% to 12%). There were no statistically significant changes in the microbiology of the nasopharynx or middle ear in swimmers or non-swimmers. Streptococcus pneumoniae and non-typeable Haemophilus influenzae were the dominant organisms cultured from the nasopharynx, and H. influenzae, Staphylococcus aureus and Pseudomonas aeruginosa were the dominant organisms in the middle ear.
Conclusions: Swimming lessons for Aboriginal children in remote communities should be supported, but it is unlikely that they will substantially reduce rates of chronic suppurative otitis media and associated bacteria in the nasopharynx and middle ear. However, swimming was not associated with increased risk of ear discharge and we found no reason to discourage it.
Trial registration: Australian New Zealand Clinical Trials Registry ACTRN12613000634774.