Obtaining a primary training position in a specialist field is just one of the many outcomes of undergraduate medical education. Decisions to undertake primary training (the first level of formal or basic postgraduate medical training after medical school) and subspecialty training are affected not only by personal preference, but also by the available pathways between undergraduate and postgraduate training. Facets of the undergraduate curriculum reported to affect the career paths of graduates include the use of problem-based learning,1 different grading systems2 and depth of basic sciences teaching.3 The selection process in medical colleges is highly competitive. We surveyed doctors who were registered to practise in New South Wales between 1995 and 2006, to investigate the factors that graduates perceive to help them obtain a training position.
Although there is little about this issue in the literature, it is relevant to current debates about specialist training and career pathways. There is a need for greater collaboration between stakeholders, such as medical schools, specialist training colleges and postgraduate medical education councils, to better understand and meet the expectations and needs of new graduates.4 The results presented here will enhance such collaborations.
The demographic details in Box 1 show that a high proportion of graduates had their results reported as a grade or mark on graduation (193/308 [63%]); just over a third were registrars (124/316 [39%]); and just over half were practising in a capital city (175/322 [54%]). Of 321 valid responses, 242 (75%) had applied to enter a training program at the time of data collection and 240 (99%) of those had been accepted, with 217/240 (90%) specifying this was their first choice and the remainder leaving the question unanswered. Using independent samples t tests, we found no significant difference in obtaining a training position by sex (F = 7.26; P = 0.186), graduating with honours compared with not graduating with honours (F = 2.81; P = 0.408), or graduating from a graded compared with an ungraded program (F = 3.25; P = 0.370).
personal study or weekly study groups (73 responses);
investigations into particular training programs (43 responses);
preparation courses (29 responses); and
curriculum vitae and interview skills (28 responses).
Factors that had helped them to achieve their career goals to date were grouped into five key areas:
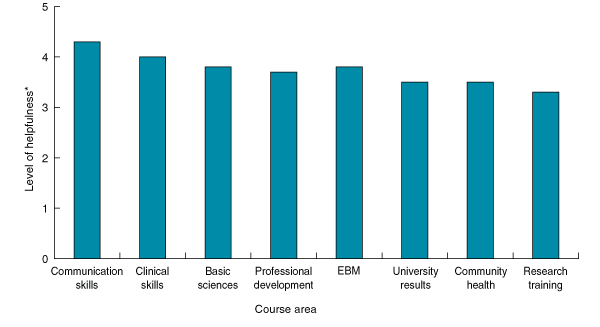
Respondents were asked the extent to which they perceived various factors within their medical degree as helpful or not in obtaining a training position. All areas of the medical course were perceived as helpful, with none rated as “not helpful”. Communication skills and clinical skills were considered the most helpful areas (Box 2).
the importance of basic sciences (or lack of) in their course (equal comments each way);
perceptions that their degree had very little effect on their access to further training, apart from being a prerequisite to complete;
positive perceptions of their medical school overall; and
the role of research in practice.
a strong background in medical science;
ability to manage stress and setbacks;
ability to maintain extracurricular interests;
access to, or involvement in, relevant research projects;
exposure to the medical specialty of interest as a resident;
choice of hospital where registrar training is done — clinical or didactic support for getting the study done to pass exams makes a big difference; and
continued support from mentors and senior staff.
In helping to prepare graduates and junior doctors for primary training, the importance of mentors cannot be overemphasised. This was commented on throughout the survey and has also been reported by others.5,6 There is a clear need to foster and preserve this relationship in all training institutions, perhaps through the establishment of structured mentor programs in internship that can be followed through long term. This relationship is especially important given the changes in training that are currently occurring and the possibility of completing training over a shorter period of time. Nevertheless, there are issues in ensuring that there is equal opportunity for junior doctors to engage with supportive mentors.
In line with previous research, our study found that age, graduation with honours, or having a grade rather than “pass/fail” on one’s transcript had no effect on access to further training.2 This finding needs to be widely publicised among medical students to reduce anxiety about choosing a medical school. There is much discussion and debate about grading in particular,2,7 and more research is needed on this issue in the Australian context.
In terms of preparation for primary training, personal and weekly study groups were considered to be a positive influence and a major source of preparation. This observation extends previous research on the role of study groups in medical school8 and suggests that junior doctors may need support, allocated time, encouragement and space to participate in these activities.
Our findings may also have implications for undergraduate program planning. First, it was clear that graduates felt their personal attributes of motivation and persistence carried them through and were the main reasons for their success. Strategies may need to be devised to foster the development of these skills, especially the ability to deal with stress and the capacity to cope in the long term. Second, most graduates commented that communication and clinical skills were the most helpful aspects of their undergraduate degree program. This was an interesting finding, given the evidence that students frequently complain about the amount of time courses spend on teaching communication skills.9,10 Revealing our findings to medical students may enhance their appreciation and understanding of the significance of communication skills in accessing postgraduate training. Finally, there was an emerging trend for junior doctors to recognise the importance of research to their future careers. The role of research was not emphasised in some undergraduate courses, and consequently those students failed to realise its significance at the time. This observation aligns with previous research that indicated most Australian medical students had narrow perceptions of what research involved. Previous involvement in research offered both opportunities for, and constraints against, further consideration of a career involving this pathway.11 Some junior doctors lamented the lack of exposure to research in their undergraduate degree and recognised that more opportunities to engage in research would have been an advantage.
Although most graduates obtained their first preference for a training position during the period of the study (96%), the expected increase in new medical graduates seeking a position between now and 2012 may affect the nature of these results. New approaches are needed to ensure access to training, and new training positions will need to commence immediately.12 After 2008, junior doctors from three of the seven medical schools in NSW will be from graduate-entry programs and may therefore have different perceptions and preferences for certain career pathways.13 It will be important to review these issues.
The findings also need to be interpreted in light of the limitations of our study, including the low response rate, characteristics of the sample, and interpretation of questions about meeting career goals. Although the low response rate is a threat to validity, the results of the study are similar to those of other studies of junior doctors with no follow-up.14 At the time the survey was distributed, acceptance rates to medical colleges for vocational training were 100% for all but three.15 This is reflected in our findings, where 99% of graduates were accepted into their preferred training program at first attempt. Further, the sample reflects the distribution of graduates from 1995 to 2004, also noted by the Medical Training Review Panel.15 This enhances the validity of the findings. However, our survey results require greater validation and will be enhanced by future follow-up focus groups with a cross-section of graduates to explore the issues raised in more detail. Our sample may have over-represented those who were successful at gaining entry to the courses of their choice on first attempt and may be biased by those who felt their personal characteristics carried them through. There was also an over-representation of respondents from urban areas and at the registrar level.
- Sarah J Hyde1
- Pippa L Craig2
- Ann J Sefton3
- Greg L Ryan3
- Stephanie J Arnold4
- Vasi Naganathan3,5
- 1 School of Biomedical Sciences, Charles Sturt University, Orange, NSW.
- 2 ANU Medical School, Australian National University, Canberra, ACT.
- 3 University of Sydney, Sydney, NSW.
- 4 Royal Prince Alfred Hospital, Sydney, NSW.
- 5 Concord Repatriation General Hospital, Sydney, NSW.
The authors would like to thank the NSW Medical Registration Board for sharing data, the survey respondents, and Professor Ian Wilson, who provided a critical review of the article and insightful comments.
Our study began while Sarah Hyde, Pippa Craig, Ann Sefton and Greg Ryan were employed by the Office of Medical Education at the University of Sydney. All efforts have been made to look at the data objectively. Only one of the researchers (Vasi Naganathan) currently has any direct affiliation with the University of Sydney’s medical education program.
- 1. Dowton SB. Imperatives in medical education and training in response to demands for a sustainable workforce. Med J Aust 2005; 183: 595-598. <MJA full text>
- 2. Bloodgood R, Short J, Jackson J, et al. A change to pass/fail grading in the first two years at one medical school results in improved psychological well-being. Acad Med 2009; 84: 655-662.
- 3. Milgate S. Submission on Australian medical education. Australian Doctors’ Fund Submission 29, 2006. http://www.dest.gov.au/NR/rdonlyres/037E4C20-8C57-4CEC-AC47-406DE90C2815/12852/Submission29.pdf (accessed Jan 2010).
- 4. Dowton SB, Stokes M-L, Rawstron EJ, et al. Postgraduate medical education: rethinking and integrating a complex landscape. Med J Aust 2005; 182: 177-180. <MJA full text>
- 5. Macafee DAL. Is there a role for mentoring in surgical specialty training? Med Teach 2008; 30: 55-59.
- 6. Thorndyke LE, Gusic ME, Milner RJ. Functional mentoring: a practical approach with multilevel outcomes. J Contin Educ Health Prof 2008; 28: 157-164.
- 7. Gonnella JS, Erdmann JB, Hojat M. An empirical study of the predictive validity of number grades in medical school using three decades of longitudinal data: implications for a grading system. Med Educ 2004; 38: 425-434.
- 8. Hendry GD, Hyde SJ, Davy P. Independent student study groups. Med Educ 2005; 39: 672-679.
- 9. Rees CE, Sheard CE, McPherson AC. A qualitative study to explore undergraduate medical students’ attitudes towards communication skills learning. Med Teach 2002; 24: 289-293.
- 10. Rees CE, Sheard CE. Evaluating first-year medical students’ attitudes to learning communication skills before and after a communication skills course. Med Teach 2003; 25: 302-307.
- 11. Hyde SJ. Australian medical students’ interest in research as a career [internet]. Focus Health Prof Educ 2007; 9: 27-38.
- 12. Fox GJ, Arnold SJ. The rising tide of medical graduates: how will postgraduate training be affected? Med J Aust 2008; 189: 515-518. <MJA full text>
- 13. Joyce CM, Stoelwinder JU, McNeil JJ, Piterman L. Riding the wave: current and emerging trends in graduates from Australian university medical schools. Med J Aust 2007; 186: 309-312. <MJA full text>
- 14. Dent AW, Crotty B, Cuddihy HL, et al. Learning opportunities for Australian prevocational hospital doctors: exposure, perceived quality and desired methods of learning. Med J Aust 2006; 184: 436-440. <MJA full text>
- 15. Medical Training Review Panel. Tenth report. November 2006. Canberra: Commonwealth of Australia, 2006. http://www.health.gov.au/internet/main/publishing.nsf/Content/0C3D 4391BC6A3392CA2573AA00214043/$File/mtrpall.pdf (accessed Mar 2010).





Abstract
Objective: To investigate the specific factors that graduates perceive to influence their success in obtaining primary training in a chosen field.
Design, setting and participants: The New South Wales Medical Registration Board provided data on doctors who were registered to practise between 1995 and 2006. A brief, paper-based survey was sent to a random selection of 2000 doctors.
Main outcome measures: Doctors’ self-reported perceptions on the impact of demographic details, specialty training applied for, university training and other factors on opportunities for further training after medical school.
Results: Of the 375/1915 doctors (19.6%) who responded, most had completed a 6-year undergraduate degree from the University of Sydney, University of NSW or University of Newcastle, and most were at registrar level. Of 242/321 doctors (76%) who had applied for a training position, 240 (99%) had been accepted. The support of a mentor was considered the most positive influence on meeting long-term career goals (255/318 [80%]). Learning how to communicate with patients was valued as the most helpful aspect of medical school (270/318 [85%]).
Conclusion: The personal attributes of graduates were considered more influential in achieving career goals and accessing further training than perceived features of a medical program. This suggests that more emphasis and research should be devoted to selecting the most appropriate candidates, rather than restructuring medical curricula to meet a presumed need for more content knowledge before graduation.