Australia is currently in the midst of an expansionist phase in medical workforce supply, driven by a range of policies designed to encourage growth in the medical workforce, including significant increases to medical school intakes. Already there are expressions of concern about the flow-on effect of these increases through medical education pathways.1 Here, we place current policies in their historical context, quantify the immediate outcomes with respect to the number of graduates over the next decade, and consider the broader implications of larger graduate cohorts.
Historically, the long-term picture indicates evident cycles in Australian medical workforce supply policy, with periodic shifts between phases of containment and growth. In 1973, increases to medical school intakes were recommended in response to perceived workforce shortages.2 Intakes were expanded, and graduations from medical schools rose steadily during the 1970s, from 851 in 1970 to 1278 in 1980. By then, the medical workforce was believed to be in oversupply, and reductions to medical school intakes were recommended and subsequently implemented.3 Effects of this on graduate numbers were seen from the mid 1980s, with 1030 graduates in 1990. The medical workforce was considered to be in surplus throughout the 1980s and into the 1990s, and medical school intakes remained static.4,5 In the late 1990s, opinion began to swing back to a view of medical workforce shortage, and after a 20-year period of no change, intakes to medical schools were once again rigorously augmented. Five new medical schools have opened since the year 2000, with a further seven programs planned by 2008 (see Box 1), doubling the number of medical schools since 2000. Combined with increases to intake numbers in existing medical schools, this represents a square wave shift that is in stark contrast to the static pattern of graduate numbers over the previous two decades.
The profile of Australian university medical school graduates is also changing, with increasing numbers of international students. The effect of this increase is amplified by changes in policy which, since 2003, have enabled international graduates to remain in Australia and obtain access to general medical registration here. Adding to this increase is a new student group: domestic full-fee-paying students. Since 2004, medical schools may enrol domestic full-fee-paying students in addition to their Commonwealth-funded domestic places; more than half of Australia’s medical schools have taken up this option (Box 1). This allowance was originally limited to the equivalent of 10% of domestic places provided, but has increased to 25% from 2007.
We projected graduate numbers using data from Medical Deans Australia and New Zealand (formerly the Committee of Deans of Australian Medical Schools) for Australian university medical schools from 2001 to 2005.6 This dataset provides the number of students by year of course, university, sex, and student type (domestic or international). This dataset was supplemented by information on stated government and university plans for new programs or expansions, obtained from media releases, websites and other sources.7
These simple extrapolations of expected numbers were adjusted to account for non-completion of degrees. We used the “apparent completion rate” method presented by Parkhouse, in which intake to medical schools in the United Kingdom was compared with output 5 years later.8 We used an apparent completion rate of 93.1%, based on previous analysis of actual commencements and completions in Australian university medical schools from 1994 to 2003.9
The projected number of graduates is shown in Box 2, with actual graduate numbers of domestic students from 1970 and international students from 1989 to 2005 for comparison. There is a clear jump in 2008, when the first graduates from Griffith University and the University of Notre Dame (Fremantle) will join those from the Australian National University (2007). All of the planned changes will have flowed through to the medical workforce by 2012, when graduate numbers are projected to stabilise once again. Overall, the number of domestic graduates is projected to increase by 81%, from 1348 in 2005 to 2442 in 2012.
Western Australia, Queensland, New South Wales and Tasmania are projected to have the largest percentage changes in total (domestic and international) graduates from 2005 to 2012, and South Australia the smallest (Box 3).
Our estimated projections are conservative, due to the assumptions of a 93.1% completion rate and no increases in international or domestic full-fee-paying students. The Medical Specialist Training Steering Committee projected about 2500 Commonwealth-funded graduates by 2012,10 and the Australian Medical Association has projected 3023 domestic graduates,11 compared with our projection of 2442 total domestic students, including full-fee-paying.
These figures paint a clear picture: the wave of students flowing into the Australian medical workforce represents substantial growth, and we must plan carefully — now — if we are to ride the wave, rather than being swamped by it. There are significant implications for medical training pathways, patterns of career choice, and workforce supply levels.
One of the most immediate concerns is the number of places and the resources available at the prevocational training stage. This is looming as a potential bottleneck in the system as more students than ever compete for junior medical officer positions. Although the states and territories have agreed, as part of the Council of Australian Governments (COAG) Health Workforce initiative, to provide sufficient intern-level positions, this does not address the need for similar increases in resources for the subsequent postgraduate training years (PGY2 and PGY3). Urgent attention is required to ensure that availability of clinical teachers, teaching time, access to patients, and necessary infrastructure is sufficient for the increased trainee numbers throughout this critical period of training.12
A number of strategies have been proposed to address this, including using simulation and a wider range of clinical teaching settings, such as community-based health services and the private health sector.12 A commitment to use private clinical settings for specialist training was made at the July 2006 COAG meeting;10 a similar approach is likely to be needed for the prevocational stage. The now well established rural clinical schools network provides another option for expanding clinical training beyond the traditional urban hospital setting. Innovations in clinical training, such as private sector settings or simulation, will need to be accompanied by mechanisms to safeguard quality and broad equivalence of training experiences.
Increased numbers of overseas-trained doctors are also entering the Australian medical workforce by the Australian Medical Council pathway, up from around 200 per year in the 1990s to over 500 in 2004.13 This will add to the demands for clinical supervision and postgraduate training.
Changes in the student body may influence patterns of career choice within medicine (specialty distribution). Women’s career choices have been found to be different to men’s,14,15 and it is also possible that GMP graduates will have different patterns of career choice than those from undergraduate programs. Although research in the UK indicates only slight differences,16 medical schools have been shown to vary in patterns of graduate career choices.17 The increasingly diverse “character” of Australia’s medical schools suggests that changes to patterns of career choice are likely, and should be monitored closely. There are currently few data available to explore this issue, but it is possible that specialties experiencing difficulties in recruitment may benefit from a different graduate cohort profile. Many new regional medical schools specifically aim to produce graduates interested in rural and general practice.7 It is also possible that generational shifts in work participation patterns and preferences may overshadow sex-based differences in the future. The Medical Schools’ Outcomes Database project being overseen by Medical Deans Australia and New Zealand may provide further insight, by providing national data on the career intentions and demographics of medical students (commencing from 2006) and tracking their progress over time.
Balancing the interests of medical school graduates with the health care needs of the Australian community will become an increasingly important task. In the past, planning for individual specialist training programs was done separately, but this will need to be more integrated in the future to ensure an appropriate balance. Incentives may be needed to ensure that specialties perceived by graduates as less attractive have a sufficient workforce, similar to existing rural and remote workforce incentives. Greater flexibility in training pathways may also be required, both to accommodate interrupted and part-time training and to increase the flexibility of the medical workforce to move between specialties.18,19 Younger cohorts of professionals are increasingly mobile, not just between jobs and locations, but also between occupations.20 Medical career structures must be adapted to avoid losing too many from the medical profession altogether.
The effect of increases in numbers of graduates on the availability of clinical service providers is likely to be offset by a number of factors exerting downward pressure on workforce supply. Continual increases in the proportion of women in the medical workforce (32% of the total Australian medical workforce in 2004)21 is the first of these, as women have lower levels of workforce participation across their career compared with men.21,22 Average working hours are decreasing, influenced both by cohort effects in preferences for shorter working hours, and campaigns for “safe working hours”. Finally, increased non-clinical activity by doctors reduces the time available to provide clinical services.23
While declines in medical workforce participation levels may counteract increases in real numbers of workforce entrants, they also have implications for the number of places in, and the quality of, specialist training. Moves towards competency-based models of training, rather than time-defined programs, may assist in ensuring quality of training is maintained.24 In the future, postgraduate medical education may involve greater centralisation of governance, as has occurred in the UK.25 There may also be increased university involvement. Ideally, this should build on existing precedents for cooperative arrangements with the medical specialist colleges, for example in fields such as psychiatry, occupational medicine and palliative care. The limiting factor in expanding postgraduate medical training is the availability of clinical environments and supervisors. There are, therefore, no benefits in competition between universities and colleges as providers of that training. There are clearly significant challenges ahead for colleges and other parties involved in specialist training.
For policymakers, the current growth phase in medical training necessitates careful monitoring. The lessons of history tell us that, to some extent, a boom–bust cycle in workforce supply is inevitable. But we must avoid an overcorrection like that of the early 1980s, the effects of which are felt now as workforce shortages. There are often unintended or unforeseen consequences of major policy changes. For example, the limits placed on entry to the Australian medical workforce in the early 1980s contributed to a massive rise in the number of overseas-trained doctors entering Australia on temporary resident visas during the 1990s.26 Policymakers will need to be watching for the emergence of any similar unintended effects of current policies.
1 Basic medical training programs in Australia, 2006*
Victorian Extended Rural Cohort (Monash University & University of Melbourne) |
|||||||||||||||
University of New England (Joint program with University of Newcastle) |
|||||||||||||||
2 Australian university medical school graduates: actual and projected, 1970–2016
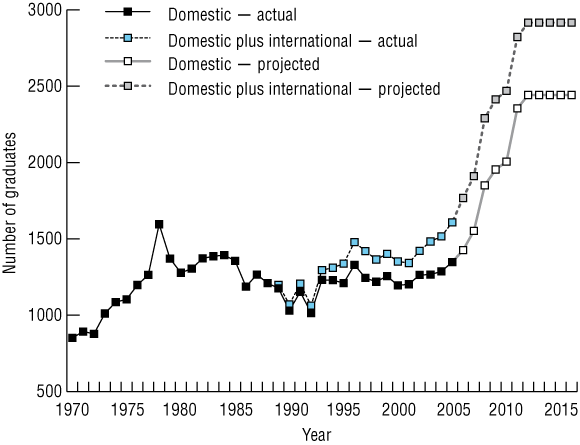
Sources: Karmel;2 Doherty;4 Medical Deans Australia and New Zealand;6 Department of Science, Education and Training, University Statistics Section, higher education data (customised dataset RFI 03/312). |
- Catherine M Joyce1
- Johannes U Stoelwinder2
- John J McNeil3
- Leon Piterman4
- Monash University, Melbourne, VIC.
None identified.
- 1. Van Der Weyden MB. Increased medical school places: a crisis in the making? [From the Editor’s desk]. Med J Aust 2006; 185: 129. <MJA full text>
- 2. Karmel P (Chairman). Expansion of medical education. Report of the Committee on Medical Schools to the Australian Universities Commission. (Parliamentary Paper No. 110.) Canberra: AGPS, 1973.
- 3. Sax S (Chairman). Medical manpower supply. Report of the Committee of Officials. Canberra: AGPS, 1980.
- 4. Doherty RL (Chairman). Committee of Inquiry into Medical Education and the Medical Workforce. Australian medical education and workforce into the 21st century. Canberra: AGPS, 1988.
- 5. Australian Medical Workforce Advisory Committee and Australian Institute of Health and Welfare. Australian medical workforce benchmarks. AMWAC Report 1996.1. Sydney: AMWAC, 1996. http://www.health. nsw.gov.au/amwac/amwac/pdf/benchmarks.pdf (accessed Jan 2007).
- 6. Medical Deans Australia and New Zealand. Medical student statistics 2005. http://www.medicaldeans.org.au/projects.html#topic7 (accessed Jan 2007).
- 7. Lawson KA, Chew M, Van Der Weyden MB. The new Australian medical schools: daring to be different. Med J Aust 2004; 181: 662-666. <MJA full text>
- 8. Parkhouse J. UK medical school intake and output 1985–99. Med Educ 2001; 35: 137-138.
- 9. Joyce CM. The health workforce in Australia: aspects of current and future supply [PhD thesis]. Melbourne: Department of Epidemiology & Preventive Medicine, Monash University, 2005.
- 10. Medical Specialist Training Steering Committee. Expanding settings for medical specialist training, MSTSC report 2006. Canberra: Australian Government Department of Health and Ageing, 2006. http://www.health.gov.au/internet/wcms/publishing.nsf/Content/work-edu-spectr-mstsc-rept (accessed Jan 2007).
- 11. Australian Medical Association. Training and support for the future medical workforce. AMA briefing paper. Canberra: AMA, August 2006.
- 12. Crotty BJ. More students and less patients: the squeeze on medical teaching resources [editorial]. Med J Aust 2005; 183: 444-445. <MJA full text>
- 13. Australian Medical Workforce Advisory Committee. Annual report 2004–05. AMWAC Report 2005.4. Sydney: AMWAC, 2005. http://www.health.nsw.gov.au/amwac/amwac/pdf/ar_0405.pdf (accessed Jan 2007).
- 14. Lambert EM, Holmboe ES. The relationship between specialty choice and gender of US medical students, 1990-2003. Acad Med 2005; 80: 797-802.
- 15. Harris MG, Gavel PH, Young JR. Factors influencing the choice of specialty of Australian medical graduates. Med J Aust 2005; 183: 295-300. <MJA full text>
- 16. Lambert TW, Goldacre MJ, Davidson JM, Parkhouse J. Graduate status and age at entry to medical school as predictors of doctors’ choice of long-term career. Med Educ 2001; 35: 450-454.
- 17. Goldacre MJ, Turner G, Lambert TW. Variation by medical school in career choices of UK graduates of 1999 and 2000. Med Educ 2004; 38: 249-258.
- 18. Skinner CA. Re-inventing medical work and training: a view from generation X. Med J Aust 2006; 185: 35-36. <MJA full text>
- 19. Dowton SB. Imperatives in medical education and training in response to demands for a sustainable workforce. Med J Aust 2005; 183: 595-598. <MJA full text>
- 20. Alexander JA, Ramsay JA, Thomson SM. Designing the health workforce for the 21st century. Med J Aust 2004; 180: 7-9. <MJA full text>
- 21. Australian Institute of Health and Welfare. Medical labour force 2004. Canberra: AIHW, 2006. (AIHW Catalogue No. HWL 39.) http://www.aihw.gov.au/publications/index.cfm/title/10379 (accessed Feb 2007).
- 22. Joyce CM, McNeil JJ. Participation in the workforce by Australian medical graduates. Med Educ 2006; 40: 333-339.
- 23. Joyce CM, McNeill JJ, Stoelwinder JU. Time for a new approach to medical workforce planning. Med J Aust 2004; 180: 343-346. <MJA full text>
- 24. Dahlenburg GW. Medical education in Australia: changes are needed [editorial]. Med J Aust 2006; 184: 319-320. <MJA full text>
- 25. UK National Health Service. Modernising medical careers — the next steps. The future shape of Foundation, Specialist and General Practice Training Programmes. London: NHS, 2004. http://www.mmc.nhs.uk/pages/resources/keydocuments#7 (accessed Nov 2006).
- 26. Birrell B, Hawthorne L. Medicare Plus and overseas-trained medical doctors. People and Place 2004; 12: 83-99.





Abstract
The number of domestic graduates from Australian medical schools is set to increase by 81% in 7 years, from 1348 in 2005 to 2442 by 2012.
Including international students, medical school graduates will total almost 3000 by 2012.
Planning must begin now to ensure that the significant flow-on effects of these increases are managed effectively.
Most urgently, postgraduate medical training will require a substantial injection of resources to expand opportunities for clinical training, without compromising quality.
Patterns of career choice by medical graduates and workforce supply levels must be monitored to ensure responsiveness to the effects of substantially larger, and more diverse, graduate cohorts.