Since the emergence of the first internet programs for mental disorders, there have been several systematic or quasi-systematic reviews of the effectiveness of depression and anxiety internet interventions.1-10 Three of these reviews focused specifically on randomised controlled trials (RCTs) of internet interventions. In particular, our 2006 review of RCTs of internet interventions for mental health and related disorders1 and a subsequent 2007 update2 identified 10 trials focusing either on depression (four trials) or anxiety (six trials). Two of the four depression trials and four of the six anxiety trials yielded evidence of reduced symptoms. Subsequently, Spek and colleagues conducted a quantitative meta-analysis of 12 published and in-press RCTs of internet-based cognitive behaviour therapy (CBT) for depression and anxiety, reporting mean effect sizes for these conditions of 0.32 and 0.96, respectively.9
We updated our previous reviews of internet interventions for mental health and related conditions1,2 using the methodology described in the original article.1 In particular, recent eligible trials were identified by searching the PubMed, PsycINFO and Cochrane Central Register of Controlled Trials databases using the two key search terms (“Internet” OR “Web”) for the period since the last search.2 However, the most recent PubMed search was limited to “randomized controlled trials”, and a methodological search filter11 was used to focus the PsycINFO search on randomised controlled trials.
Studies were included only if they: (i) involved a self-help website intervention or a website intervention that incorporated a self-help component; (ii) described the website application as targeting a depression or anxiety condition; (iii) tested the efficacy or effectiveness of the intervention; (iv) incorporated a measure of symptom outcome for the targeted condition; (v) employed an RCT design; (vi) included a control group that was not subjected to an active intervention such as a behavioural or cognitive therapy intervention, peer-to-peer forum or medication; and (vii) had been peer-reviewed and published. Dissertations and posters were excluded. Studies involving the guided delivery of a self-help intervention or in which the intervention was partly delivered by a therapist were included. All eligible reports from our original reviews1,2 and those of more recent eligible trials (collected in two waves, in February 2009 and mid June 2009) were included, together with any additional relevant trials identified by a search of the health intervention web portal Beacon (see Christensen et al),12 a search of the contents of the Journal of Medical Internet Research and our personal knowledge of the field.
Each eligible paper was independently rated by K M G and a research assistant on three items of the Cochrane Collaboration’s tool for assessing risk of bias:13 sequence generation (Did the study employ an appropriate randomisation process? Yes, No, Unclear); allocation concealment (Did the study use an appropriate method of concealing the allocation of participants to conditions? Yes, No, Unclear); and incomplete outcome data (Were incomplete outcome data adequately addressed? Yes, No, Unclear).
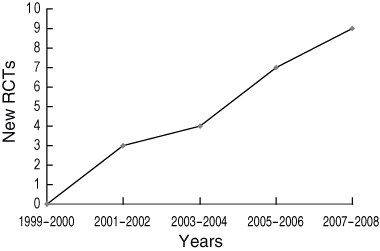
Box 1 shows that the number of new RCTs of efficacy or effectiveness of depression and anxiety internet interventions has increased approximately linearly over time, since the first trials appeared in the literature in 2001.
Twenty-six trials (described in 29 reports) satisfied the inclusion criteria.14-42 Of these, eight targeted depression, 16 targeted an anxiety disorder (panic disorder, 5; social phobia, 5; post-traumatic stress disorder, 4; unspecified anxiety disorder, 2), and two studies targeted both depression and anxiety (Box 2). All trials employed a CBT intervention program (or a component of CBT41), with program durations ranging from 1 to 13 weeks. One trial also included an evidence-based depression education intervention.14
Two of the eight depression trials and almost all of the anxiety trials employed some level of therapist input, with two of the anxiety trials incorporating a face-to-face component.25,32 Mean therapist time per participant ranged from 90 to 376 minutes across studies (median, 155 minutes).
Twenty-three of the 26 trials were community-based, with one based in a clinic25 and two undertaken in the context of a health maintenance organisation in the United States.23,24 None of the studies were undertaken in a general practice setting. Most of the samples involved adults with a mean age in the range of 30–50 years. Only one trial targeted an older sample,17,18 and two trials involved children or adolescents.25,26 None of the studies investigated outcomes for rural participants, although one specifically recruited both rural and city participants.27 Sample sizes ranged from 23 to 786. The median sample size was 300 for depression, and 32, 73 and 66 for panic disorder, social phobia and post-traumatic stress disorder, respectively. Only two of the trials employed longer-term follow-up (at least 6 months) involving a randomised controlled design.16,18
Most of the studies employed an intention-to-treat design. However, recruitment methods varied across studies, as did criteria for study inclusion. Some studies only included participants with a formal diagnosis of a depressive or anxiety disorder, while others selected participants on the basis of a clinically significant cut-off score on a self-report measure. Others selected people with elevated but not necessarily clinically significant levels of symptoms, and one study employed a sample of participants with subthreshold depression, specifically excluding those with a diagnosis of depressive disorder.17 Finally, some studies recruited those who self-selected as requiring self-help.
Box 2 summarises the outcomes for short-and long-term follow-up, including the short-term ESDs, for each study. Of the 26 trials, 23 demonstrated some evidence of effectiveness. The two trials that investigated long-term effectiveness using an RCT design reported that the interventions were effective over the long term.16,18
Six of the eight trials targeting depression yielded positive effects for CBT. One also demonstrated evidence of efficacy for an evidence-based depression information internet site relative to an attention control,14 suggesting that passive psychoeducational information may be an effective intervention for depression. As a consequence, trials in Box 2 were separated on the basis of whether they employed a psychoeducational control condition. All five depression trials that used a wait-list, treatment-as-usual or attention placebo control group were effective in both the short term and, for the two RCTs that investigated it, the long term. Of the three trials that exposed the control group to psychoeducational information about depression, one, which employed reminders and involved minimal information, was effective.
All of the anxiety interventions yielded positive results on at least one measure, regardless of the type of control group they employed, except for the non-therapist arm of one social phobia study.36 With this exception, all the anxiety programs without psychoeducational controls employed diagnostic criteria or therapist input and, in most cases, both. The ESDs of all anxiety programs ranged from 0.29 to 1.74, with most exceeding 0.65.
Only five of the programs included in this review are available in the English language. Of the English-language programs, three depression applications are currently publicly accessible on the web without charge to consumers (ODIN,23,24 MoodGYM and BluePages;14-16 see Bennett et al).43 A fourth depression program (Sadness20) and a social phobia program (Shyness34-36) are available under restricted licence at a small cost (see Andrews and Titov).44 With the exception of ODIN, each of these English-language programs was developed in Australia and is supported by evidence from additional intervention studies not reported here.
The findings of this review clearly demonstrate that the internet can be an effective medium for the delivery of interventions designed to reduce the symptoms of depression and anxiety conditions. Moreover, the effect sizes for the depression trials, both with and without therapist input, were at least as large as the standardised effect sizes relative to controls reported in recent meta-analyses of psychological treatment in primary care (0.31)45 and antidepressant treatment of depression (0.37).46 Similarly, the anxiety effect sizes reported here are consistent with controlled effect sizes reported for face-to-face treatment of panic disorder47,48 and social phobia.49
Based on the current available data, it is not possible to reliably draw conclusions about the factors that predict better outcomes. The effect sizes for anxiety trials appear larger than those for depression trials, but participants in the former trials were more often self-selected volunteers and were typically only included in the trial if they also satisfied diagnostic criteria at screening. In addition, as noted in a previous review,9 participants in the anxiety trials were more likely to receive therapeutic input in addition to the internet self-help program. Moreover, a greater proportion of the anxiety trials employed less conservative wait-list control designs, and the potential for study bias was greater in the anxiety trials.
A question of considerable practical and policy importance is whether internet programs yield better results if they include input from therapists or lay facilitators, or email reminders. Previous reviews have reported greater effect sizes for internet9 and other self-help programs50 when the intervention incorporated therapist assistance. However, the latter meta-analysis found no clear advantage of therapeutic support compared with simple monitoring.50 The findings from our review and other trials51 suggest that internet programs can be effective without therapist input. However, due to the variation in the methodologies of the studies reviewed, such as participant and control group characteristics, it was not possible to evaluate the effect of the presence, type or intensity of guidance by comparing effect sizes across studies.
One of the reviewed studies did directly compare self-guided with therapist-guided delivery of a program,36 finding superior outcomes for the latter. In this study, participants with social phobia received a 6-week, web-based, self-help CBT program and chat group, or the same intervention with the addition of email contact with a therapist (requiring an average of 2.5 hours of therapist time per participant). Unfortunately, the study did not include a condition involving an equivalent degree of guidance from a lay facilitator or the use of an automated ongoing email reminder system. Including these conditions would have assisted in determining the effect of substituting automated reminders or trained lay facilitators for trained therapists in delivering these programs. Moreover, it is not known how much guidance is optimal. A recent study reported no advantage of substantial therapist input compared with minimal therapist input.52
One study recently reported that an internet program for panic disorder was as effective when administered by general practitioners as by clinical psychologists.53 However, a methodological weakness of the study was that the participants seen by the GPs were recruited from a primary care setting, whereas those seen by the psychologists were not. Moreover, since the GPs involved had received mental health training, the result may not be generalisable to GPs without such training.
Well controlled studies are required to investigate the relative efficacy of automated reminder systems compared with human guidance, the relationship between outcomes and training, and the extent to which time spent facilitating self-help determines outcomes. In addition, there is a need to investigate whether internet mental health interventions work equally well for different individuals and groups and in different settings. In our original review, we found no trials involving rural residents, older people or children and adolescents.1 Little has changed, with none of the studies reviewed here targeting older adolescents, rural residents, or people with low educational backgrounds, and only one trial targeting older people. There is still much that we do not know.
What we do know is that many people who might benefit from conventional face-to-face psychological treatment or preventive intervention will not receive it, either by preference or because of geographical or mobility barriers or a shortage of trained therapists.54-57 In such circumstances, it is justified for a health care provider to prescribe an internet intervention that has been shown in community trials to have efficacy at least equivalent to that resulting from treatment as usual in primary care; and self-referral of a consumer to a self-help internet service of demonstrated efficacy is similarly justified.
1 Growth in randomised controlled trials (RCTs) of the efficacy or effectiveness of depression and anxiety internet interventions
2 Summary of randomised controlled trials (RCTs) of internet intervention programs targeted at (i) depression, (ii) anxiety and (iii) both depression and anxiety (continued)
- Kathleen M Griffiths1
- Louise Farrer2
- Helen Christensen3
- Centre for Mental Health Research, Australian National University, Canberra, ACT.
Kathleen Griffiths is supported by National Health and Medical Research Council (NHMRC) Fellowship 525413, Helen Christensen is supported by NHMRC Fellowship 525411, and Louise Farrer is supported by an Australian Research Council Linkage Australian Postgraduate Award (Industry) scholarship. We would like to thank Kanupriya Kalia for rating the included studies for risk of bias.
Kathleen Griffiths and Helen Christensen are coauthors of several depression internet programs, including MoodGYM and BluePages.
- 1. Griffiths KM, Christensen H. Review of randomised controlled trials of Internet interventions for mental disorders and related conditions. Clin Psychol 2006; 10: 16-29.
- 2. Griffiths K, Farrer L, Christensen H. Clickety-click: e-mental health train on track. Australas Psychiatry 2007; 15: 100-108.
- 3. Ybarra ML, Eaton WW. Internet-based mental health interventions. Ment Health Serv Res 2005; 7: 75-87.
- 4. Postel MG, de Haan HA, De Jong CA. E-therapy for mental health problems: a systematic review. Telemed J E Health 2008; 14: 707-714.
- 5. Bee PE, Bower P, Lovell K, et al. Psychotherapy mediated by remote communication technologies: a meta-analytic review. BMC Psychiatry 2008; 8: 60.
- 6. Mataix-Cols D, Marks IM. Self-help with minimal therapist contact for obsessive-compulsive disorder: a review. Eur Psychiatry 2006; 21: 75-80.
- 7. Kaltenthaler E, Brazier J, De Nigris E, et al. Computerised cognitive behaviour therapy for depression and anxiety update: a systematic review and economic evaluation. Health Technol Assess 2006; 10 (33): 1-168.
- 8. Hailey D, Roine R, Ohinmaa A. The effectiveness of telemental health applications: a review. Can J Psychiatry 2008; 53: 769-778.
- 9. Spek V, Cuijpers P, Nyklicek I, et al. Internet-based cognitive behaviour therapy for symptoms of depression and anxiety: a meta-analysis. Psychol Med 2007; 37: 319-328.
- 10. Andersson G. Internet-based cognitive-behavioral self help for depression. Expert Rev Neurother 2006; 6: 1637-1642.
- 11. Weightman AL, Mann MK, Sander L, Turley RL. A systematic approach to identifying the evidence. Project Methodology 5. Health Evidence Bulletins Wales. Cardiff: Information Services, University of Wales College of Medicine, 2004.
- 12. Christensen H, Murray K, Calear AL, et al. Beacon: a web portal listing high-quality mental health websites for use by health professionals and the public. Med J Aust 2010; 192 (11 Suppl): S40-S44. <MJA full text>
- 13. Higgins JPT, Altman DG, editors. Chapter 8: Assessing risk of bias in included studies. In: Higgins JPT, Green S, editors. Cochrane handbook for systematic reviews of interventions. Version 5.0.1 (updated Sep 2008). The Cochrane Collaboration, 2008. http://www.cochrane-handbook.org (accessed Oct 2009).
- 14. Christensen H, Griffiths KM, Jorm AF. Delivering interventions for depression by using the internet: randomised controlled trial. BMJ 2004; 328: 265-270.
- 15. Griffiths KM, Christensen H, Jorm AF, et al. Effect of web-based depression literacy and cognitive-behavioural therapy interventions on stigmatising attitudes to depression: randomised controlled trial. Br J Psychiatry 2004; 185: 342-349.
- 16. Mackinnon A, Griffiths KM, Christensen H. Comparative randomised trial of online cognitive-behavioural therapy and an information website for depression: 12-month outcomes. Br J Psychiatry 2008; 192: 130-134.
- 17. Spek V, Nyklicek I, Smits N, et al. Internet-based cognitive behavioural therapy for subthreshold depression in people over 50 years old: a randomized controlled clinical trial. Psychol Med 2007; 37: 1797-1806.
- 18. Spek V, Cuijpers P, Nyklicek I, et al. One-year follow-up results of a randomized controlled clinical trial on internet-based cognitive behavioural therapy for subthreshold depression in people over 50 years. Psychol Med 2008; 38: 635-639.
- 19. Warmerdam L, van Straten A, Twisk J, et al. Internet-based treatment for adults with depressive symptoms: randomized controlled trial. J Med Internet Res 2008; 10 (4): e44.
- 20. Perini S, Titov N, Andrews G. Clinician-assisted Internet-based treatment is effective for depression: randomized controlled trial. Aust N Z J Psychiatry 2009; 43: 571-578.
- 21. Meyer B, Berger T, Caspar F, et al. Effectiveness of a novel integrative online treatment for depression (Deprexis): randomized controlled trial. J Med Internet Res 2009; 11 (2): e15.
- 22. Patten SB. Prevention of depressive symptoms through the use of distance technologies. Psychiatr Serv 2003; 54: 396-398.
- 23. Clarke G, Reid E, Eubanks D, et al. Overcoming Depression on the Internet (ODIN): a randomized controlled trial of an Internet depression skills intervention program. J Med Internet Res 2002; 4 (3): e14.
- 24. Clarke G, Eubanks D, Reid E, et al. Overcoming Depression on the Internet (ODIN) (2): a randomized trial of a self-help depression skills program with reminders. J Med Internet Res 2005; 7 (2): e16.
- 25. Spence SH, Holmes JM, March S, Lipp OV. The feasibility and outcome of clinic plus internet delivery of cognitive-behavior therapy for childhood anxiety. J Consult Clin Psychol 2006; 74: 614-621.
- 26. March S, Spence SH, Donovan CL. The efficacy of an internet-based cognitive-behavioral therapy intervention for child anxiety disorders. J Pediatr Psychol 2009; 34: 474-487.
- 27. Klein B, Richards JC. A brief internet-based treatment for panic disorder. Behav Cogn Psychother 2001; 29: 113-117.
- 28. Carlbring P, Westling BE, Ljungstrand P, et al. Treatment of panic disorder via the internet: a randomized trial of a self-help program. Behav Ther 2001; 32: 751-764.
- 29. Carlbring P, Bohman S, Brunt S, et al. Remote treatment of panic disorder: a randomized trial of internet-based cognitive behavior therapy supplemented with telephone calls. Am J Psychiatry 2006; 163: 2119-2125.
- 30. Klein B, Richards JC, Austin DW. Efficacy of internet therapy for panic disorder. J Behav Ther Exp Psychiatry 2006; 37: 213-238.
- 31. Richards JC, Klein B, Austin DW. Internet cognitive behavioural therapy for panic disorder: does the inclusion of stress management information improve end-state functioning? Clin Psychol 2006; 10: 2-15.
- 32. Andersson G, Carlbring P, Holmström A, et al. Internet-based self-help with therapist feedback and in vivo group exposure for social phobia: a randomized controlled trial. J Consult Clin Psychol 2006; 74: 677-686.
- 33. Carlbring P, Gunnarsdottir M, Hedensjö L, et al. Treatment of social phobia: randomised trial of internet-delivered cognitive-behavioural therapy with telephone support. Br J Psychiatry 2007; 190: 123-128.
- 34. Titov N, Andrews G, Schwencke G, et al. Shyness 1: distance treatment of social phobia over the Internet. Aust N Z J Psychiatry 2008; 42: 585-594.
- 35. Titov N, Andrews G, Schwencke G. Shyness 2: treating social phobia online: replication and extension. Aust N Z J Psychiatry 2008; 42: 595-605.
- 36. Titov N, Andrews G, Choi I, et al. Shyness 3: randomized controlled trial of guided versus unguided Internet-based CBT for social phobia. Aust N Z J Psychiatry 2008; 42: 1030-1040.
- 37. Lange A, Rietdijk D, Hudcovicova M, et al. Interapy: a controlled randomized trial of the standardized treatment of posttraumatic stress through the internet. J Consult Clin Psychol 2003; 71: 901-909.
- 38. Hirai M, Clum GA. An Internet-based self-change program for traumatic event related fear, distress, and maladaptive coping. J Trauma Stress 2005; 18: 631-636.
- 39. Knaevelsrud C, Maercker A. Internet-based treatment for PTSD reduces distress and facilitates the development of a strong therapeutic alliance: a randomized controlled clinical trial. BMC Psychiatry 2007; 7: 13-22.
- 40. Lange A, van de Ven JP, Schrieken B, Emmelkamp PM. Interapy, treatment of posttraumatic stress through the internet: a controlled trial. J Behav Ther Exp Psychiatry 2001; 32: 73-90.
- 41. van Straten A, Cuijpers P, Smits N. Effectiveness of a web-based self-help intervention for symptoms of depression, anxiety and stress: randomized controlled trial. J Med Internet Res 2008; 10 (1): e7.
- 42. Billings DW, Cook RF, Hendrickson A, Dove DC. A web-based approach to managing stress and mood disorders in the workforce. J Occup Environ Med 2008; 50: 960-968.
- 43. Bennett K, Reynolds J, Christensen H, Griffiths KM. e-hub: an online self-help mental health service in the community. Med J Aust 2010; 192 (11 Suppl): S48-S52. <MJA full text>
- 44. Andrews G, Titov N. Is internet treatment for depressive and anxiety disorders ready for prime time? Med J Aust 2010; 192 (11 Suppl): S45-S47. <MJA full text>
- 45. Cuijpers P, van Straten A, Warmerdam L, Andersson G. Psychological treatment of depression: a meta-analytic database of randomized studies. BMC Psychiatry 2008; 8: 36.
- 46. Turner EH, Matthews AM, Linardatos E, et al. Selective publication of antidepressant trials and its influence on apparent efficacy. N Engl J Med 2008; 358: 252-260.
- 47. Haby MM, Donnelly M, Corry J, Vos T. Cognitive behavioural therapy for depression, panic disorder and generalized anxiety disorder: a meta-regression of factors that may predict outcome. Aust N Z J Psychiatry 2006; 40: 9-19.
- 48. Kiropoulos LA, Klein B, Austin DW, et al. Is internet-based CBT for panic disorder and agoraphobia as effective as face-to-face CBT? J Anxiety Disord 2008; 22: 1273-1284.
- 49. Acarturk C, Cuijpers P, van Straten A, de Graaf R. Psychological treatment of social anxiety disorder: a meta-analysis. Psychol Med 2009; 39: 241-254.
- 50. Gellatly J, Bower P, Hennessy S, et al. What makes self-help interventions effective in the management of depressive symptoms? Meta-analysis and meta-regression. Psychol Med 2007; 37: 1217-1228.
- 51. Christensen H, Griffiths KM, Mackinnon AJ, Brittliffe K. Online randomized controlled trial of brief and full cognitive behaviour therapy for depression. Psychol Med 2006; 36: 1737-1746.
- 52. Klein B, Austin D, Pier C, et al. Internet-based treatment for panic disorder: does frequency of therapist contact make a difference? Cogn Behav Ther 2009; 38: 100-113.
- 53. Shandley K, Austin DW, Klein B, et al. Therapist-assisted, Internet-based treatment for panic disorder: can general practitioners achieve comparable patient outcomes to psychologists? J Med Internet Res 2008; 10 (2): e14.
- 54. Shapiro DA, Cavanagh K, Lomas H. Geographic inequity in the availability of cognitive behavioural therapy in England and Wales. Behav Cogn Psychother 2003; 31: 185-192.
- 55. Andrews G, Issakidis C, Carter G. Shortfall in mental health service utilisation. Br J Psychiatry 2001; 179: 417-425.
- 56. Lowe S, O’Kane A. National allied health workforce report. Canberra: Services for Australian Rural and Remote Allied Health, 2004.
- 57. Australian Institute of Health and Welfare. Rural, regional and remote health: Indicators of health. Canberra: AIHW, 2005. (AIHW Cat. No. PHE 59.)





Abstract
Objective: To review the outcomes, nature and quality of published randomised controlled trials of preventive and treatment internet interventions for depression and anxiety disorders, and to document the availability of effective interventions.
Data sources: Previous reviews of internet interventions for mental health and related conditions were updated using an extension of the original methodology. All studies included in the original reviews and more recent eligible trials (published before June 2009) were included, together with any trials identified from a search of the health intervention web portal Beacon and the Journal of Medical Internet Research.
Study selection: A total of 29 reports describing 26 trials satisfied the inclusion criteria.
Data synthesis: All trials employed a cognitive behaviour therapy intervention program. Of the 26 trials, 23 demonstrated some evidence of effectiveness relative to controls. Effect size differences ranged from 0.42 to 0.65 for depression interventions involving participants with clinically significant symptoms of depression, and 0.29 to 1.74 for anxiety interventions involving participants with a diagnosed anxiety disorder. Of the five effective English-language programs, three are available to the public without charge and two can be accessed at a small cost through health practitioner referral.
Conclusion: Internet interventions for depression and anxiety disorders offer promise for use as self-help applications for consumers or as an adjunct to usual care.