To be introduced into the health care environment, a new treatment should reduce symptoms and improve outcomes in a way that is comparable to, or better than, existing treatments. Based on this criterion, computerised treatment over the internet seems close to being ready to become part of the mainstream health system. A project assessing cost-effectiveness in mental health calculated that the commonest treatment for depression, social phobia, panic disorder/agoraphobia, and generalised anxiety disorder — selective serotonin reuptake inhibitors — produced improvement at a cost of $25 000–$30 000 per disability-adjusted life-year gained.1 We contend that internet therapies seem to perform much better in terms of cost and efficacy.
Does it work? (ie, does it reduce symptoms, distress and disability in the shorter term and inhibit relapse in the longer term?);
Is it affordable to the consumer? (ie, are direct payments for treatment affordable for most people?);
Is it acceptable to most people, as measured by adherence (the proportion of people completing treatment)?;
Are the costs to the funder within the allocated budget?;
Is it acceptable to the provider, as measured by the uptake in the workforce?; and
Is it immune to gaming by unscrupulous providers or consumers?
Here, we examine the evidence concerning internet treatment for the common internalising mental disorders — depressive and anxiety disorders. This includes treatment programs designed for people who meet diagnostic criteria for anxiety or depressive disorders, not those for people with anxiety or depressive symptoms. The internalising disorders account for some 6% of the burden of disease in Australia, more than twice the impact of diabetes mellitus, and are a serious public health issue, as less than a quarter of affected patients receive evidence-based treatment.2,3 If effective treatment is lacking, then alternatives have to be found — internet treatment programs could be one answer. There are several such programs available in Australia: FearFighter, Beating the Blues, Anxiety Online, and the CRUfAD programs that we have developed and evaluated.
Marks and colleagues comprehensively reviewed the field of computer-aided psychotherapy in 2008.4 Their own principal program is FearFighter (http://www.fearfighter.com; CCBT Ltd, Birmingham, UK), a text-based cognitive behaviour therapy (CBT) program that is commercially available in the United Kingdom to treat people with phobias. It has been identified by the UK National Institute for Health and Clinical Excellence as cost-effective for use in primary care.5 The cost to the individual for a self-help version is around $800 (all costs reported here are in Australian dollars), with clinician-guided versions being more expensive and licences to health authorities less expensive. Currently there are no programs supported in Australia, but they are available from http://www.fearfighter.com.
Beating the Blues (http://www.beatingtheblues.co.uk; Ultrasis, London, UK) is an interactive text, graphics and video CBT program for anxiety and depressive disorders that is available through the National Health Service in the UK and is also commercially available in the UK and some other countries. It has been identified by the UK National Institute for Health and Clinical Excellence as cost-effective for use in primary care.5 In the UK, it is free to individuals and paid for by participating health authorities at costs starting from $80 per patient. Beating the Blues is available privately at a cost of $595 (this includes 24/7 unlimited telephone access to trained counsellors over 12 months, and lifetime access to the program).
Anxiety Online (http://www.anxietyonline.org.au; National eTherapy Centre, Swinburne University, Melbourne, Vic) is an extensive set of online, interactive, text, audio- and video-based CBT programs for each of the anxiety disorders, that has been principally developed as a clinician-assisted (via email) format. Additionally, a fully automated online clinical assessment is offered and is compulsory before any treatment program is undertaken. The clinician-assisted version costs $120 per user, and the online assessment and self-help treatment programs are free of charge.
People can apply for treatment at the VirtualClinic (http://www.virtualclinic.org.au) and, if they meet diagnostic criteria for the relevant disorder, they will be included in an evaluation program. These courses are free, and a thousand people are treated each year. Courses are researched in the VirtualClinic, and improvements made as a result. The improved version then becomes a standard course at the CRUfADclinic (http://www.crufadclinic.org). Access to CRUfADclinic courses for patients is by a prescription from a clinician, usually their general practitioner or psychologist. There is a service fee of $5 per course at the CRUfADclinic, but for clinicians registered under the Australian Government’s Access to Allied Psychological Services (ATAPS) program, this service fee is waived until July 2011.
The programs that have been or are being researched in the VirtualClinic are described below.
The Shyness research program began with a randomised controlled trial (RCT) in which a group of 55 participants undergoing clinician-guided CBT was compared with a group of 50 participants whose treatment was delayed for 3 months. Adherence in the treatment group was 78%, and the intention-to-treat effect size (ITT ES) superiority over the delayed treatment group was 0.95; 2.12 hours of clinician time per patient was provided.6 The control group was then treated, and adherence and outcome were similar to those in the intervention group. This trial was replicated with 88 participants, with similar results (adherence, 80%; ITT ES, 1.2; 2.12 hours of clinician time).7 In a third trial involving 98 participants, another condition was added — access to the program without clinician guidance. The clinician-guided group progressed as expected (adherence, 77%; ITT ES, 1.04; 2.8 hours of clinician time) but, compared with the control group, the self-help group did less well (adherence, 33%; ITT ES, 0.66).8
An effective, fully automated program was clearly desirable, and the Shyness program was revised to include automated reminders by email and text messaging, and forum comments derived from people in the first three trials that were de-identified to inform each lesson. The next RCT included these improvements and compared 82 participants undergoing an automated self-help program with 81 participants using the same program plus weekly 4-minute telephone reminders from a technician.9 The outcome in the latter group was significantly better than the fully automated group, but both groups achieved results comparable to or better than those obtained in face-to-face treatment of social phobia in our clinic.10
The question therefore remained of whether clinician guidance was necessary. We conducted a further RCT involving 42 participants given clinician guidance versus 43 participants using self-help plus technician reminders. Both the clinician-guided and self-help groups did well (adherence, 79% in both groups; ITT ES, 1.5 and 1.3, respectively).11 Given this satisfactory result, this program was transferred to the CRUfADclinic for use by GPs and other clinicians, with the advice that they use a clinic manager or practice nurse to give patients a weekly phone call to encourage progress. However, clinicians were also advised that, even without this encouragement, patients were likely to do as well as those referred to specialised clinics that provide face-to-face CBT or drug treatment, and at less cost.
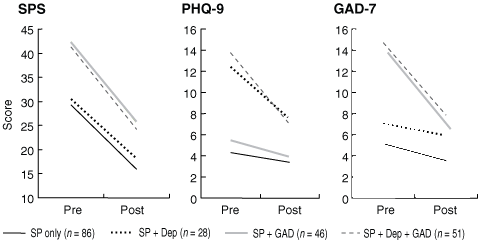
Some questions remained. Were these good results stable over time, and did the internet therapy take account of the conditions that are commonly comorbid with social phobia? At 6-month follow-up of the people in the first three RCTs, it was evident that improvement had continued; there was no relapse.12 We then examined people who had comorbid depression or generalised anxiety disorder. These results showed that people with social phobia, with or without comorbid depression or anxiety, had significantly reduced social phobia scores; people with comorbid depression also had reduced depression scores, and people with comorbid generalised anxiety disorder also had reduced anxiety scores.13 It was clear that the internet treatment was not only effective in the short and long term, but that it enabled people to combat their comorbid disorders (see Box).
The Sadness research program began with an open trial of clinician-guided CBT (recovery story plus homework) involving 13 participants, and the results were good (adherence, 77%; ITT ES, 1.00; 3.5 hours of clinician time per patient).14 We then conducted an RCT in which 27 participants undergoing clinician-guided CBT were compared with a group of 18 participants whose treatment was delayed for 3 months. Adherence in the treatment group was 74%, and the ITT ES superiority over the delayed treatment group was 0.98; 1.9 hours of clinician time per patient was provided.15 The control group was then treated, and adherence and outcome were similar to those in the intervention group, even though clinician input was reduced to 1 hour per patient. In a trial that is underway at present, we have added a third condition — a fully automated program plus weekly telephone calls from the clinic manager — to explore whether depression can be treated satisfactorily without clinician input.
In the Panic program, we have found similar results for clinician-guided CBT in an open trial of 10 participants with panic disorder and agoraphobia (adherence, 80%; ITT ES, 1.14; 3.4 hours of clinician time per patient)16 and from an RCT.17 Similarly, in the Worry program, an RCT of clinician-guided CBT for people with generalised anxiety disorder has produced excellent results.18 Whether an automated program will be efficacious in these two disorders remains to be seen.
The CRUfADclinic web-based service programs were designed for patients of busy GPs.19,20 As described above, the CRUfADclinic now contains treatment programs for people with social phobia, panic disorder/agoraphobia, generalised anxiety disorder and major depressive disorder, that GPs and other clinicians can use to supplement their own treatment of patients with these disorders. The CRUfADclinic also contains education programs that GPs and other clinicians might recommend to their patients, including programs for patients with alcohol misuse problems, arthritis, asthma, breast cancer, diabetes, heart failure, and incontinence; for carers of people with dementia; and for teenagers with substance use and emotional difficulties.
Clinicians can log in to http://www.crufadclinic.org and use a credit card to purchase a special prescription book (for $100) that contains instructions and 20 prescriptions with individual keys to allow patients to log in to the website. The system measures patient wellbeing each time he or she logs in and reports this information in an email to the prescribing clinician, so that appropriate actions can be taken. We are presently visiting all rural Divisions of General Practice in Australia that participate in the ATAPS program, to educate GPs and allied health personnel about CRUfADclinic.
The results from all these programs show that they are more effective and much less expensive than standard therapy with medication.21,22 While we have striven to develop programs that require little clinician input, simply because clinicians are in short supply, we do think that these programs should be prescribed in a clinical environment. We would like to see them become part of a stepped-care sequence that proceeds from diagnosis and advice to internet programs for those for whom the advice was insufficient, then to face-to-face specialist treatment for those for whom the internet program was insufficient. We are aware of specialists who are now using CRUfADclinic courses to help severely ill people to understand and become ready for face-to-face specialist treatment. In this way, CRUfADclinic courses are becoming a natural part of the therapeutic armamentarium.
Pre- and post-treatment scores on the Social Phobia Scale (SPS), Patient Health Questionnaire-9 (PHQ-9), and Generalized Anxiety Disorder 7-item (GAD-7) scale for the CRUfADclinic Shyness program*
- Gavin Andrews1
- Nickolai Titov2
- Clinical Research Unit for Anxiety and Depression, School of Psychiatry, University of New South Wales at St Vincent’s Hospital, Sydney, NSW.
We are both involved in producing CRUfAD not-for-profit internet treatment programs for anxiety and depression.
- 1. Vos T, Haby MM, Magnus A, et al. Assessing cost-effectiveness in mental health: helping policy-makers prioritize and plan health services. Aust N Z J Psychiatry 2005; 39: 701-712.
- 2. Sanderson K, Andrews G. Mental disorders and burden of disease: how was disability estimated and is it valid? Aust N Z J Psychiatry 2001; 35: 668-676.
- 3. Begg S, Vos T, Barker B, et al. The burden of disease and injury in Australia 2003. Canberra: Australian Institute of Health and Welfare, 2007. (AIHW Cat. No. PHE 82.)
- 4. Marks IM, Cavanagh K, Gega L. Hands-on-help: computer-aided psychotherapy. Maudsley Monograph 49. Hove, UK: Psychology Press, 2007.
- 5. Kaltenthaler E, Brazier J, De Nigris E, et al. Computerised cognitive behaviour therapy for depression and anxiety update: a systematic review and economic evaluation. Health Technol Assess 2006; 10 (33): 1-168.
- 6. Titov N, Andrews G, Schwencke G, et al. Shyness 1: distance treatment of social phobia over the Internet. Aust N Z J Psychiatry 2008; 42: 585-594.
- 7. Titov N, Andrews G, Schwencke G. Shyness 2: treating social phobia online: replication and extension. Aust N Z J Psychiatry 2008; 42: 595-605.
- 8. Titov N, Andrews G, Choi I, et al. Shyness 3: randomized controlled trial of guided versus unguided Internet-based CBT for social phobia. Aust N Z J Psychiatry 2008; 42: 1030-1040.
- 9. Titov N, Andrews G, Choi I, et al. Randomized controlled trial of web-based treatment of social phobia without clinician guidance. Aust N Z J Psychiatry 2009; 43: 913-919.
- 10. McEvoy PM. Effectiveness of cognitive behavioural group therapy for social phobia in a community clinic: a benchmarking study. Behav Res Ther 2007; 45: 3030-3040.
- 11. Titov N, Andrews G, Schwencke G, et al. An RCT comparing effect of two types of support on severity of symptoms for people completing Internet-based cognitive behaviour therapy for social phobia. Aust N Z J Psychiatry 2009; 43: 920-926.
- 12. Titov N, Andrews G, Johnston L, et al. Shyness programme: longer term benefits, cost-effectiveness, and acceptability. Aust N Z J Psychiatry 2009; 43: 36-44.
- 13. Titov N, Gibson M, Andrews G, McEvoy P. Internet treatment for social phobia reduces comorbidity. Aust N Z J Psychiatry 2009; 43: 754-759.
- 14. Perini S, Titov N, Andrews G. The Climate Sadness program: an open trial of Internet-based treatment for depression. E-J Appl Psychol [online] 2008; 4 (2): 18-24. http://ojs.lib.swin.edu.au/index.php/ejap/article/view/135 (accessed Jan 2009).
- 15. Perini S, Titov N, Andrews G. Clinician-assisted Internet-based treatment is effective for depression: randomized controlled trial. Aust N Z J Psychiatry 2009; 43: 571-578.
- 16. Wims E, Titov N, Andrews G. The Climate Panic program: an open trial of Internet-based treatment for panic disorder. E-J Appl Psychol [online] 2008; 4 (2): 26-31. http://ojs.lib.swin.edu.au/index.php/ejap/article/view/134 (accessed Jan 2009).
- 17. Wims E, Titov N, Andrews G, Choi I. Clinician-assisted internet-based treatment is effective for panic: randomized controlled trial. Aust N Z J Psychiatry 2010; in press.
- 18. Titov N, Andrews G, Robinson E, et al. Clinician-assisted Internet-based treatment is effective for generalized anxiety disorder: randomized controlled trial. Aust N Z J Psychiatry 2009; 43: 905-912.
- 19. Andrews G. ClimateGP – web based patient education. Aust Fam Physician 2007; 36: 371-372.
- 20. Andrews G, Titov N. Changing the face of mental health care through needs-based planning. Aust Health Rev 2007; 31 Suppl 1: S122-S128.
- 21. Heuzenroeder L, Donnelly M, Haby MM, et al. Cost-effectiveness of psychological and pharmacological interventions for generalized anxiety disorder and panic disorder. Aust N Z J Psychiatry 2004; 38: 602-612.
- 22. Vos T, Corry J, Haby MM, et al. Cost-effectiveness of cognitive-behavioural therapy and drug interventions for major depression. Aust N Z J Psychiatry 2005; 39: 683-692.





Abstract
Internet treatment programs for anxiety and depressive disorders are becoming available and offer cost-effective alternatives to face-to-face treatment with medication or cognitive behaviour therapy.
The Clinical Research Unit for Anxiety and Depression at St Vincent’s Hospital, Sydney, offers internet treatment courses at the VirtualClinic (http://www.virtualclinic.org.au) for people who meet diagnostic criteria for major depression, social phobia, panic disorder and generalised anxiety disorder. These courses are free to people recruited for research.
The results of VirtualClinic trials show a high level of patient adherence and strong reductions in symptoms, and that very little clinician time is required.
The four treatment programs that have been successfully evaluated in the VirtualClinic have been made available on a not-for-profit basis ($5 service fee) at the CRUfADclinic (http://www.crufadclinic.org) for general practitioners and other clinicians to use with their patients.
These programs could be the first level of treatment in a stepped-care environment, where patients who do not benefit sufficiently could then receive face-to-face treatment from their clinician or be referred for specialist treatment.