Indonesian fishermen have fished in Australian waters since the mid 18th century.1 In 1974, a Memorandum of Understanding identified five areas on Australia’s north-west shelf to which traditional fishermen were given continuing access. However, since the early 1990s, fishermen have not limited themselves to the so-called “MOU Box”, and illegal incursions into Australian waters have increased. It is thought that this is because of the sustained high price of shark fin in the Asian market and the depletion of shark populations in Indonesian waters by large commercial operators and poor fisheries management.2
The Australian Government’s controversial response to this threat to marine resource sustainability3 has been to apprehend and destroy illegal vessels, confiscate the catch and fishing equipment and, in some cases, prosecute the fishermen.2 Before 2005, apprehended fishermen were detained on their vessels pending deportation or prosecution. This avoided the need for government-funded housing, physically separated the fishermen from the Australian public, and the open-air ventilation minimised the risk of transmission of airborne infections such as tuberculosis (TB) to custodial personnel. Communicable disease screening was undertaken only for fishermen who developed an acute illness or were entering Darwin Correctional Centre in Australia’s Northern Territory.4 Although limited health data were collected, Darwin’s Centre for Disease Control (CDC) TB database shows that nine illegal fishermen were diagnosed with TB between October 2000 and September 2005.
Anthropological studies suggest that most illegal fishermen are from resource-poor coastal villages with overcrowded living conditions, poor water quality and sanitation facilities, and limited access to health and education services.1 Consequently, when the Australian Government announced that, from September 2005, fishermen were to be detained in land-based settings, a comprehensive public health screening process was developed to discharge the duties of care to the individual fishermen and to the Australian public.4 Here, we evaluate the TB control aspects of this health assessment process as undertaken in Darwin.5
Illegal fishermen entering Darwin undergo a two-stage health assessment in accordance with clinical and procedural guidelines.5 The first stage is a targeted “TB and General Health Questionnaire”. Designed to be administered by non-medical personnel and an interpreter, it aims to identify fishermen who have symptoms of TB (cough for more than 2 weeks, recent haemoptysis or fever), a past history of TB, or a close family contact with a case of pulmonary TB. These fishermen are required to wear a surgical mask until their formal health assessments with a CDC medical officer.6
The TB component of the formal assessment involves a chest x-ray and clinical review (with an interpreter) to exclude active pulmonary TB.5 No fishermen refused to consent to the assessment. The decision was made to x-ray all, rather than only symptomatic, fishermen because of the expected high prevalence of TB and the difficulty of eliciting symptoms in a screening interview. Chest x-rays are read by TB medical officers and, as a quality assurance measure, a radiologist later reports on all films.
Fishermen with radiological signs of TB are hospitalised in respiratory isolation and three sputum samples are taken for acid-fast bacilli (AFB) smear and culture. No more than two samples are taken in a 24-hour period. Initial laboratory testing occurs at Royal Darwin Hospital, and culture-positive samples are sent to the Victorian Infectious Diseases Reference Laboratory for identification and sensitivity testing. Fishermen diagnosed with smear-positive pulmonary TB commence first-line antituberculosis therapy7 and, being potentially infectious, remain isolated until they produce three consecutive smear-negative sputum samples. Fishermen found to have multidrug-resistant (MDR) TB remain in isolation until three consecutive culture-negative sputum results are obtained.
Fishermen with TB do not have the option to remain in Australia to complete 6 months’ treatment. They are deported once they test smear-negative (or culture-negative in the case of MDR-TB8,9), provided they have tolerated at least 1 month of antituberculosis treatment. Thus, clinical and radiological improvement cannot be assessed, nor treatment completion confirmed. Attempts are made to facilitate continuity of care after deportation by providing a 1-month supply of medication, a letter translated into the fisherman’s local language and by attempting to contact a local TB treatment provider.
We examined the data on all fishermen who underwent health assessments in Darwin between 28 September 2005 and 31 December 2006. As this study was a clinical audit for quality assurance purposes, ethical approval was not required.10
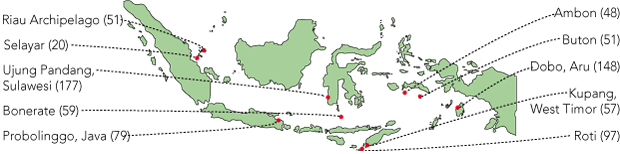
In the 15-month study period, 1471 illegal fishermen underwent health assessments in Darwin. Demographic and TB data are presented in Box 1. The most common islands of origin for Indonesian fishermen were Aru, Roti and Sulawesi (Box 2).
All 20 fishermen diagnosed with TB were Indonesian; their average age was 33.9 years (SD, 11.8 years; range, 20–54 years). The prevalence of TB in this population was 534.8 per 100 000 fishermen for smear-positive cases, 1019.7 per 100 000 for culture-positive cases, and 1359.6 per 100 000 for all TB diagnoses. In comparison, the estimated overall TB prevalence in Indonesia in 2004 was 275 per 100 000.11
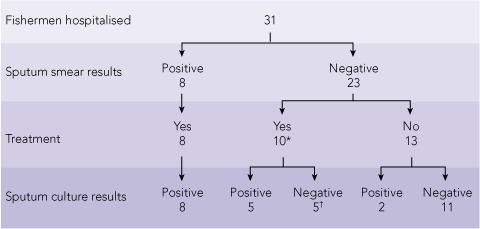
Whether or not a fisherman was given a mask did not help predict a diagnosis of TB (positive predictive value [PPV] for smear-positive disease, 0.04; and for culture-positive disease, 0.07). Self-reported cough was less predictive of culture-positive TB (PPV, 0.03) than was a suggestive chest x-ray warranting hospital admission (PPV, 0.48). In hospitalised patients, sputum smear and culture results were the most accurate indicator of the need for TB treatment12 (Box 3).
Illegal fishermen are predominantly young Indonesian males from villages dependent on fishing revenue. As shown by the high percentage of those aged under 18 years (11.4%), many fishermen leave school early to learn “the way of the sea”,1 and their mobile lifestyles lead to limited access to health care from a young age. Given that TB disproportionately affects people from poorly resourced areas,13,14 it is not surprising that the prevalence of TB in this study population is so high.
The relatively high rate of smear-positive cases (53% of culture-positive cases) in this study provides further evidence of a high prevalence of TB in Indonesian fishing communities.15,16 As smear-negative disease is thought to reflect early infection with few pulmonary lesions and low bacillary load,16 it can be postulated that while our smear-negative diagnoses may represent early detection of newly reactivated or relapsed cases (perhaps secondary to under-nutrition and stress during sea voyages), the smear-positive cases reflect a high prevalence of established pulmonary TB in the villages of origin.
This has public health consequences for Australia. Illegal fishermen, like other populations from areas of high TB prevalence who have no predeparture screening (such as asylum seekers17 and evacuees from regional disasters15), arrive in a very low TB prevalence country that is currently experiencing an exaggerated fear of communicable disease transmission from new arrivals.18 It is vital for both the actual protection of public health and for community confidence that comprehensive TB screening of arrivals from areas of high TB prevalence is undertaken.
Our findings suggest that the TB screening process undertaken by the CDC in Darwin fulfils these requirements. Developed by a consultative process, it has been accepted by agencies involved in apprehending and detaining illegal fishermen,4 is endorsed by the Communicable Diseases Network of Australia,5 and provides continual opportunities to educate custodial personnel about TB transmission. The TB and General Health Questionnaire, in particular, allows agencies to “own” a part of the process leading to increased cooperation and understanding, and lending support to retaining the questionnaire despite its low predictive value.
Our finding that all 117 spot sputum tests were smear-negative and culture-negative for TB is more difficult to interpret. Although no cases of pulmonary TB were later diagnosed in fishermen cleared by the health assessment process, the yield of a single sputum sample is low.12 To ensure that screening is maximising case detection, it may be that spot sputum tests should be replaced with three samples. As it has low infectivity, we did not screen for extra-pulmonary TB. The total burden of TB in illegal fishermen will therefore have been underestimated by our study.
The World Health Organization’s Stop TB Strategy sets two interim targets: a global TB case-detection rate of 70% and a cure (successful treatment completion) rate of 85% of detected cases.13 In 2004, the WHO estimated that Australia had a case-detection rate of 94%14,19 and cure rate of 95%.20 Indonesia’s official figures for the same year show that 39% of all cases and 53% of new smear-positive cases were detected, and 87% of these successfully completed treatment.11 Our study indicates that, for illegal fishermen, these figures may be as extreme as 100% case detection and zero cure.
The reason for this finding is that Australian illegal fishing policy does not consider the individual and public health implications of deporting fishermen before curative treatment is completed. The barriers to fishermen accessing treatment after deportation are significant. Departing fishermen are flown to Kupang or Bali and expected to make their own way home, potentially hundreds of kilometres away. During this time their treatment is not directly observed13 and, once they arrive home, TB clinics are rarely accessible. One patient reported that his closest clinic was on a neighbouring island and it would take a week to pick up his medications. Fishermen also stated that most TB clinics in Indonesia charge for medications, and that they are unable to afford them. Second-line medications remain entirely unavailable. Other barriers to a prolonged treatment course include stigma, and the fact that fishermen accumulate significant debt while they are detained in Australia, and are usually contractually bound to their next fishing voyage.1
Failure to complete treatment leads to a higher risk of relapse, with subsequent potential transmission of TB, and an increased disease burden. Partial treatment where any of the treatment is unsupervised may also lead to the emergence of drug-resistant TB, with consequences for the individual as well as the capacity of TB control programs.21 By failing to consider these issues Australia is, in effect, transferring risk to Indonesia; a country with a higher TB burden and less capacity to manage it. It also ignores the high rate of recidivism among fishermen, which may lead to partially treated patients returning to Australia with resistant strains of TB, requiring long periods of intensive and expensive second-line treatment.
Continuity of care for undocumented migrants diagnosed with TB in developed countries is of international concern, and there is increasing pressure for these countries to take greater responsibility for regional TB control.22,23 For Australia, this would mean allowing fishermen to remain until they complete curative treatment. There are precedents for this. Canada, in consultation with its immigration department, has recently changed its Air Travel Guidelines to allow people subject to deportation orders to remain in Canada until their TB treatment is completed, stating that it would be “irresponsible” to do otherwise.24 The United States25 and Norway26 have similar provisions. This approach is also consistent with the World Care Council’s patients’ charter for tuberculosis care, which affirms that all people have the right to “free and equitable access” to TB treatment “from diagnosis through treatment completion”, irrespective of their legal status.27
1 Demographic and tuberculosis-health characteristics of 1471 illegal fishermen who underwent health assessments in Darwin, 28 September 2005 to 31 December 2006
2 Most common places of origin of illegal Indonesian fishermen who underwent health assessments in Darwin, 28 September 2005 to 31 December 2006
 | |||||||||||||||
3 Sputum results and treatment of the 31 hospitalised illegal foreign fishermen
- Natalie J Gray1
- Meredith Hansen-Knarhoi2
- Vicki L Krause3
- Centre for Disease Control, Darwin, NT.
We acknowledge the assistance of Dr Nathan Zweck, Dr Clif Van Der Oest, Dr Joanne Judd, Dr Julie Graham, Dr Kerryn Gijsbers, Dr Rosalind Webby and the Centre for Disease Control TB Unit nursing staff who undertook health assessments and provided valuable input into refining the health assessment process.
None identified.
- 1. Fox JJ, Sen S. A study of socio-economic issues facing traditional Indonesian fishers who access the MOU box: a report for Environment Australia. 2002. http://rspas.anu.edu.au/people/personal/foxxj_rspas/Fishermen_MOU_BOX.pdf (accessed Sep 2007).
- 2. Australian Fisheries Management Authority. $388.9 million boost in Australia’s fight against illegal foreign fishing. Fishing Future 2006; 4 (2): 4-6.
- 3. Balint R. A death in the harbour: policing Australia’s northern waters. The Monthly 2007; Apr: 32-38. http://www.themonthly.com.au/pastIssues/index.html# (accessed Sep 2007).
- 4. Gray N. Assessing the health of unauthorised fisherpersons apprehended off the Northern Territory coast — developing procedures and protocols. Northern Territory Dis Control Bull 2006; 13 (1): 6-10. http://www.nt.gov.au/health/docs/march_2006.pdf (accessed Sep 2007).
- 5. Gray N. Assessing the health of unauthorised fisherpersons apprehended off the Northern Territory coast — developing procedures and protocols. Figure. Procedure for health assessments of unauthorised fisherpersons apprehended off the north coast of Australia. Northern Territory Dis Control Bull 2006; 13: 9-10. http://www.nt.gov.au/health/docs/march_2006.pdf (accessed Dec 2007).
- 6. Jensen PA, Lambert LA, Iademarco MF, et al; CDC. Guidelines for preventing the transmission of Mycobacterium tuberculosis in health-care settings, 2005. MMWR Recomm Rep 2005; 54 (17): 1-141.
- 7. Centre for Disease Control. Guidelines for the control of tuberculosis in the Northern Territory. Darwin: Department of Health and Community Services, 2002.
- 8. World Health Organization. Tuberculosis and air travel: guidelines for prevention and control. Geneva: WHO, 2006.
- 9. Scott L, Gray N, Graham J, Krause V. Multidrug-resistant tuberculosis in an Indonesian fisherman. Northern Territory Dis Control Bull 2006; 13 (4): 9-15. http://www.nt.gov.au/health/docs/cdc_bulletin_dec_2006.pdf (accessed Sep 2007).
- 10. National Health and Medical Research Council. When does quality assurance in health care require independent ethical review? Advice to Institutions, Human Research Ethics Committees and Health Care Professionals. 2003. http://www.nhmrc.gov.au/publications/synopses/e46syn.htm (accessed Sep 2007).
- 11. World Health Organization. Global tuberculosis control report — country profile Indonesia 2006. http://www.who.int/tb/publications/global_report/2006/pdf/ind.pdf (accessed Sep 2007).
- 12. Schoch OD, Rieder P, Tueller C, et al. Diagnostic yield of sputum, induced sputum, and bronchoscopy after radiologic tuberculosis screening. Am J Respir Crit Care Med 2007; 175: 80-86.
- 13. Raviglione MC, Uplekar MW. WHO’s new Stop TB Strategy. Lancet 2006; 367: 952-955.
- 14. World Health Organization. Strategic plan to stop TB in the Western Pacific 2006–2010. Geneva: WHO, 2006.
- 15. Kelly PM, Scott L, Krause VL. Tuberculosis in East Timorese refugees: implications for health care needs in East Timor. Int J Tuberc Lung Dis 2002; 6: 980-987.
- 16. Colebunders R, Bastian I. A review of the diagnosis and treatment of smear-negative pulmonary tuberculosis. Int J Tuberc Lung Dis 2000; 4: 97-107.
- 17. King K, Vodicka P. Screening for conditions of public health importance in people arriving in Australia by boat without authority. Med J Aust 2001; 175: 600-602. <MJA full text>
- 18. Leask J, Sheikh-Mohammed M, MacIntyre CR, et al. Community perceptions about infectious disease risk posed by new arrivals: a qualitative study. Med J Aust 2006; 185: 591-593. <MJA full text>
- 19. World Health Organization. Compendium of indicators for monitoring and evaluating national tuberculosis programs. 2004. http://www.who.int/tb/publications/tb_compendium_of_indicators/en/index.html (accessed Sep 2007).
- 20. Roche PW, Bastian I, Krause V, et al. Tuberculosis notifications in Australia, 2005. Commun Dis Intell. In press.
- 21. Gandhi NR, Moll A, Sturm AW, et al. Extensively drug-resistant tuberculosis as a cause of death in patients co-infected with tuberculosis and HIV in a rural area of South Africa. Lancet 2006; 368: 1575-1580.
- 22. Perone SA, Bovier P, Pichonnaz C, et al. Tuberculosis in undocumented migrants, Geneva. Emerg Infect Dis 2005; 11: 351-352.
- 23. World Health Organization. International migration, health and human rights. Health and Human Rights Publication Series. Issue 4. Geneva: WHO, 2003.
- 24. Public Health Agency of Canada. Tuberculosis prevention and control. Guidelines regarding departure from Canada of persons with suspected respiratory tuberculosis (TB), untreated active respiratory TB or partially treated active respiratory TB. 2006. http://www.phac-aspc.gc.ca/tbpc-latb/tb_guide-ld_depart_e.html (accessed Feb 2007).
- 25. Centres for Disease Control (CDC), National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention. Prevention and control of tuberculosis in correctional and detention facilities: recommendations from CDC. MMWR Recomm Rep 2006; 55 (RR-9): 1-44.
- 26. Kloumann E, Winje BA, Heldal E. [Routines to ensure that asylum seekers with tuberculosis can remain in Norway during treatment] [Norwegian]. MSIS-rapport 2005; 33: 29.
- 27. World Care Council. The patients’ charter for tuberculosis care: patients’ rights and responsibilities. 2006. http://www.worldcarecouncil.org/pdf/PatientsCharterEN2006.txt (accessed Sep 2007).





Abstract
Objective: To document demographic details, prevalence of tuberculosis (TB), and completion of TB treatment in illegal foreign fishermen detained in Australia.
Design and participants: Clinical audit of 1471 illegal foreign fishermen who underwent health assessments in Darwin between 28 September 2005 and 31 December 2006.
Main outcome measures: Demographic details, diagnoses of smear-positive and culture-positive TB, drug sensitivity results and treatment completion.
Results: 1471 illegal fishermen underwent health assessments, including chest x-ray screening. All were male and 93.8% were from Indonesia. Of the 31 fishermen (2.1%) admitted to hospital with chest x-rays suggestive of TB, 20 were diagnosed with TB (15 culture-proven; 5 according to clinical and radiological criteria) and 18 commenced treatment. There were 8 smear-positive cases and one multidrug-resistant TB case. The prevalence of culture-positive TB was very high at 1020 per 100 000 patients. All fishermen were deported before treatment completion, and all were lost to follow-up.
Conclusions: The health assessment process successfully detected cases of TB in illegal foreign fishermen, enabling treatment to commence and the local public’s health to be protected. Treatment completion in illegal foreign fishermen may be as low as zero; deporting fishermen before curative treatment is completed undermines TB control efforts and may lead to an emergence of drug resistance and an increased burden of active TB disease in our region.