The known: Australian guidelines define intermediate risk of cardiovascular disease more restrictively than overseas guidelines. CT coronary artery calcium scoring can be used to re‐classify patients at intermediate risk, but is not widely used in Australia.
The new: Overseas risk prediction tools were superior to the Australian cardiovascular disease risk calculator with respect to identifying people with family histories of early onset coronary artery disease who have coronary artery calcium.
The implications: CT calcium scoring could be used to identify a considerable number of people who could benefit from statin treatment as primary prevention, but are currently excluded by Australian guideline‐directed treatment thresholds.
Fewer than 30% of people in Australia at high risk of a primary cardiovascular event receive guideline‐recommended statin therapy.1 This missed opportunity for preventing cardiovascular disease motivated introducing the Medical Benefits Scheme (MBS) item for heart health checks in early 2019 to encourage cardiovascular risk assessment and statin prescribing according to Australian primary prevention guidelines.2,3 However, the National Vascular Disease Prevention Alliance (NVDPA) guidelines for managing absolute cardiovascular disease risk were most recently updated in 2012, and they differ in important details from overseas guidelines.4 Firstly, the Australian absolute cardiovascular disease risk (ACVDR) calculator,5 used to select patients for primary prevention statin therapy, is a locally calibrated version of the Framingham risk equation, which has been superseded in the United States by the pooled cohort equation (PCE).6 Secondly, the definition of intermediate risk, the threshold for considering statin therapy, is lower in US guidelines (10‐year risk, 7.5% – < 20%)6 than in Australian guidelines (5‐year risk, 10–15%).3
Further, the Australian guidelines do not mention computed tomography (CT) coronary artery calcium scoring. Coronary artery calcium is a sensitive marker of subclinical coronary atherosclerosis, and calcium scoring is an accepted re‐classification tool for assessing risk in middle‐aged people.7 A zero calcium score indicates that the risk of cardiovascular disease is lower than 0.5% per year,8,9 while the risk reduction achieved by statin therapy in asymptomatic people with calcium scores of 100 or more is similar to the benefit of statins prescribed as secondary prevention.10,11 US guidelines include calcium scoring as a decision aid, recommending statin therapy for people over 55 with non‐zero calcium scores and for anybody with scores of 100 or more (class IIa recommendation); they recommend not initiating statins for people with zero calcium scores.6
The high cost of coronary CT calcium scanning in Australia (it is not subsidised by the MBS) and the radiation exposure involved should influence referral decisions. These considerations are particularly pertinent for people with family histories of early onset coronary artery disease (CAD), for whom statin therapy should be considered if they have subclinical atherosclerosis, as their outcomes are poorer than for the general population.9
We compared the performance of the ACVDR calculator and other standard cardiovascular disease risk tools with respect to identifying people who have non‐zero coronary artery calcium scores and may therefore benefit from statin therapy. We also assessed the value of calcium scoring for guiding treatment of people with a family history of early onset CAD.
Methods
Study design and participants
We analysed screening data from the Coronary Artery calcium score: Use to Guide management of Hereditary Coronary Artery Disease (CAUGHT‐CAD) trial (ACTRN 12614001294640), a randomised controlled trial assessing the utility of coronary artery calcium scoring for guiding risk evaluation and primary prevention statin therapy in patients with family histories of early onset CAD.12 Briefly, participants aged 40–70 years and free of clinical cardiovascular disease at baseline were recruited from the community at the Royal Hobart Hospital, Royal Perth Hospital, Royal Adelaide Hospital, the Baker Heart and Diabetes Institute and Austin Hospital (Melbourne), the Sunshine Coast University Hospital, and Ipswich Hospital during 1 October 2016 – 31 January 2019. Self‐reported family history of early onset CAD was defined as having a first degree relative under 60 years of age or a second degree relative under 50 with CAD. Inclusion criteria were a 5‐year ACVDR predicted risk of 2–15%, never having received statin therapy, total cholesterol not exceeding 6.5 mmol/L, and low‐density lipoprotein cholesterol below 5.0 mmol/L. Exclusion criteria included Pharmaceutical Benefits Scheme eligibility for statin therapy (Box 1), major systemic illness, impaired renal function, atrial fibrillation, and high risk of statin‐induced myopathy, as well as contraindications for CT scanning.
All participants underwent baseline clinical and standard pathology assessments, including lipid profile. Coronary artery calcium was measured with low‐dose (1 mSv), electrocardiogram‐gated, non‐contrast, dual‐source 128‐slice CT machines, and reported as Agatston scores according to the area and density of visually identified coronary calcium lesions.
Risk score calculation
We calculated risk scores for our participants with seven cardiovascular risk models cited in guidelines and with publicly available risk algorithms14,15,16,17,18,19,20,21 (Box 2), and compared their identification of people with non‐zero calcium scores (as a measure of subclinical atherosclerosis) with that of the 5‐year ACVDR calculator. We also calculated 10‐year ACVDR risk to compare risk assignment with the Multi‐Ethnic Study of Atherosclerosis (MESA).18 We calculated both fatal coronary event risk (SCORE‐CAD) and combined fatal coronary event and stroke risk with the European Systematic Coronary Risk Evaluation (SCORE) tool.17 ASSIGN (Scotland)14 and PREDICT (New Zealand)16 include postcode‐based measures of socio‐economic status (Scottish Index of Multiple Deprivation [SIMD]; New Zealand Index of Socioeconomic Deprivation). We derived corresponding scores for our participants by inverting the 2016 Index of Relative Advantage and Disadvantage (IRSAD) rankings (Australian Bureau of Statistics).26 The SIMD scores for Australian postcodes were derived from the 2012 SIMD dataset.
Outcomes
The primary outcome was coronary artery calcification (ie, non‐zero calcium score), interpreted as a marker of CAD risk.8 The secondary outcome was a calcium score of 100 or more (calcification warranting lipid therapy). Predicted 10‐year risk in the MESA model (which incorporates calcium scoring and has been validated with respect to cardiovascular events)18 was used as an independent surrogate measure of true cardiovascular risk.
Statistical analysis
Values for continuous variables are summarised as means with standard deviations (SDs) or medians with interquartile ranges (IQRs); categorical variables are summarised as numbers and proportions, with confidence intervals (CIs) calculated with the binomial method. The statistical significance of differences between proportions by calcium score group or test classification were assessed in χ2 or McNemar tests (categorical variables) and t or rank sum tests (continuous variables). Areas under the receiver operator curves (AUCs) for prediction models were compared using the Hanley–McNeil method.27 The optimal cut‐points of risk were determined according to the Youden J statistic (sensitivity + specificity – 1; this optimises discrimination when sensitivity and specificity are equally weighted28); we also estimated the cut‐points needed for achieving 80% sensitivity.
The effect of coronary artery calcium scoring for adjusting predicted ACVDR or PCE risk (as independent variables) was assessed in multivariable linear regression models, with the MESA score as the dependent variable. We then assessed changes in risk classification in models comparing the combination of ACVDR or PCE and calcium score with the MESA score. The association of age of CAD onset in relatives with subclinical disease was assessed by univariable logistic regression. Risk classification performance was based on US guideline 10‐year risk categories: low/borderline (< 7.5%), intermediate (7.5% to less than 20%), and high risk (≥ 20%). Statistical analyses were conducted in Stata 15.1 and with the ROCR package in R 3.5.1.
Ethics approval
Our study was approved by the Tasmanian Human Research Ethics Committee (reference, 14‐281) and by all participating institutions. All participants provided written informed consent.
Results
Coronary artery calcium was measured in 1059 participants; 477 had non‐zero Agatston scores (45%; median score, 41.7; IQR, 8–124), including 151 with scores of 100 or more (14%). The median age of participants with non‐zero scores was higher than for the 582 (55%) with zero scores; the proportions who were men (60% v 39%) or receiving anti‐hypertension therapy (21% v 15%) were also larger. The median 5‐year ACVDR was higher for participants with non‐zero than for those with zero scores (4.8%; IQR, 2.9–7.6% v 3.2%; IQR, 2.0–4.6%). Smoking rates, lipid profiles, and prevalence of diabetes were similar in the two groups (Box 3).
Classifying risk: Australian and United States guidelines
Of the 477 participants with non‐zero calcium scores, Australian criteria3 classified 61 as being at intermediate 5‐year risk (13%; 95% CI, 10–16%), whereas the US criteria6 classified 190 as being at intermediate 10‐year risk (40%; 95% CI, 36–44%). Were non‐zero calcium score the criterion for statin therapy, the US guidelines appropriately guided management — that is, recommended statins for patients with non‐zero scores and not for patients with zero calcium scores — for 706 of 1059 participants (67%); the Australian guidelines did so for 629 of 1059 (59%) (Box 4).
The median ACVDR for the 151 participants with calcium scores of 100 or more was 6.0% (IQR, 3.6–9.8%); 116 of these participants (77%) were deemed to be at low cardiovascular risk by Australian guidelines. Were a calcium score of 100 Agatston units the criterion for statin therapy, the 5‐year ACVDR threshold of 10% would be appropriate for 903 of 1059 participants (85%) (Box 4).
Applying US calcium scoring‐based guidelines6 would increase the number of participants eligible for statin therapy, from 75 at intermediate ACVDR risk to a total of 397 participants, an increase of 322 (116 with calcium scores of 100 or more and 206 participants aged 55 or more with non‐zero calcium scores below 100). The median 10‐year MESA risk for the 322 statin‐eligible participants was 6.5% (IQR, 4.4–10%).
Optimal risk thresholds for identifying people with coronary artery calcium
The optimal risk thresholds for identifying people with non‐zero calcium scores (sensitivity and specificity equally weighted) were 4.8% for 5‐year ACVDR (sensitivity, 51%; specificity, 77%) and 6.1% for PCE 10‐year risk (sensitivity, 50%; specificity, 82%). Treating all patients with 5‐year ACVDR of 5% or more would increase the proportion of patients with non‐zero calcium scores receiving appropriate treatment (from 61 [13%] to 219 of 477 [46%]), but would also increase the proportion of people at intermediate risk with zero calcium scores receiving statin treatment from 14 of 75 (19%) to 118 of 337 (35%). With a 5‐year ACVDR threshold of 5%, the number needed to scan to identify one person with a non‐zero calcium score (inverse of the positive predictive value) was 1.5; at this threshold, all 20 participants with a MESA risk of 20% or more would be identified (Box 8). With the PCE 10‐year risk threshold of 7.5%, 66 of 256 patients at intermediate risk (26%) had zero calcium scores (Box 4). The 5‐year ACVDR threshold needed to capture 80% of participants with non‐zero calcium scores would be 2.6% (data not shown).
The optimal risk threshold for identifying people with calcium scores of 100 or more was 6.6% for both 5‐year ACVDR (sensitivity, 49%; specificity, 84%) and PCE 10‐year risk (sensitivity, 60%; specificity, 76%). Numbers needed to scan to identify one person with a calcium score of 100 of more were 7.0 with an ACVDR risk threshold of 2%, 3.9 at a threshold of 5%, and 2.1 at a threshold of 10%.
Sensitivity of risk score models for identifying people with coronary artery calcium
The sensitivity of the ACVDR (AUC, 0.674) for identifying people with non‐zero calcium scores was lower than that of the PREDICT (AUC, 0.697; v ACVDR: P = 0.005), CUORE (AUC, 0.704; P < 0.001), SCORE (AUC, 0.706; P = 0.003), PCE (AUC, 0.711; P < 0.001), and SCORE‐CAD tools (AUC, 0.712; P < 0.001). All tools were better at identifying people with calcium scores of 100 or more, but the PCE (AUC, 0.728, P = 0.026) and SCORE‐CAD (AUC, 0.733; P = 0.05) were superior to the ACVDR (AUC, 0.709). Tools that included family history as a predictor (ASSIGN, PREDICT) were not superior to other risk models (Box 5).
Associations between subclinical atherosclerosis and age of CAD onset in the index family member or the closeness of the relationship were not statistically significant (Box 6).
Differences between tools in 10‐year risk classification
Ten‐year risk classification with the PCE was lower than with the ACVDR for 497 of 1059 participants (47%); the median calcium score for the 420 participants classified as intermediate risk by the ACVDR but as low risk by the PCE was 0 (IQR, 0–13) (Box 7; Supporting Information, table 1). Of 582 participants with zero calcium scores, the PCE classified 516 (88%) and the ACVDR 264 (45%) as being at low risk. Ten‐year risk classification with the MESA was lower than with the ACVDR for 530 (50%) and higher for 18 participants (2%).
The median 10‐year risk for all 1059 participants was 2.9% (IQR, 2.0–6.0%) with MESA, 4.2% (IQR, 2.1–7.3%) with the PCE, and 9.4% (IQR, 6.0–14%) with the ACVDR. The PCE‐ and MESA‐predicted risk categories concurred for 831 participants (78.5%); the ACVDR‐ (10‐year) and MESA‐predicted risk categories concurred for 511 participants (48.3%) (Box 8; Supporting Information, table 1). After combining the ACVDR (10‐year) with calcium scores, concordance with MESA‐predicted risk categories rose to 87.3% (925 participants), mainly by reclassifying people at intermediate risk as being at low risk (Box 8).
In the multivariable linear model, performance of the PCE and the ACVDR calculator was similar before (PCE, R2 = 0.40; ACVDR, R2 = 0.39) and after adding coronary artery calcium score to the clinical score (PCE, R2 = 0.82; ACVDR, R2 = 0.83). The β coefficient was greater for the PCE than for the ACVDR both before (PCE, 0.66; 95% CI, 0.62–0.72; ACVDR, 0.48; 95% CI, 0.44–0.51) and after standardisation and adjustment for calcium score (PCE, 0.36; 95% CI, 0.33–0.39; ACVDR, 0.28; 95% CI, 0.25–0.30) (Supporting Information, table 2).
Discussion
We have identified two problems with the assessment of cardiovascular disease risk according to Australian guidelines. First, the statin treatment threshold (5‐year risk of 10%) is higher than overseas and excludes many patients with both family histories of early onset CAD and subclinical atherosclerosis. Second, all the cardiovascular risk tools examined were moderately sensitive for identifying people with coronary artery calcium, but the ACVDR calculator was among the least sensitive in this regard.
Comparison of the performance of the ACVDR and other risk estimation tools
The various risk models are based on different populations, algorithms, risk factors, and predicted cardiovascular outcomes. While we did not compare the prognostic performance of the ACVDR in Australian patients with that of other tools, we found that it tends to rate coronary risk in Australian patients higher than most overseas models.
The CUORE, PCE, and SCORE models were better at discriminating between people with and without subclinical atherosclerosis than the locally calibrated ACVDR and more comprehensive models that include family history and social deprivation as factors (PREDICT, ASSIGN). The PCE, CUORE and SCORE models are based on different risk algorithms and study populations. The endpoints for the PCE, CUORE and SCORE are limited to major cerebrovascular and coronary events. In contrast, the Framingham model and its derivatives, the ACVDR and PREDICT, include softer endpoints, such as elective revascularisation, angina pectoris, peripheral artery disease, renovascular disease, and heart failure; the ASSIGN model endpoints include any hospital discharge diagnosis of coronary heart disease or coronary artery intervention (Box 2). These endpoints entail more subjective clinician decisions and are therefore less reliable, perhaps explaining the lower specificity of these models for identifying subclinical disease. Further, we did not find an association between postcode‐based socio‐economic status (IRSAD) and subclinical atherosclerosis, in contrast to other studies.29 These differences in endpoints and the inclusion of risk factors not independently associated with subclinical disease in our sample may also explain the tendency of some tools to generate higher risk estimates, one of the motives for developing the PCE.19 While prediction models validated in local cohorts can perform better than those validated overseas with respect to symptomatic CAD,30 local calibration may be insufficient to overcome deficiencies in the parent model.
Tools that performed better than the ACVDR included markers of cumulative exposure to risk factors, such as treatment for hypertension, that may help identify established subclinical disease.31 The median risk estimate in our study was 50% lower with the PCE than that with the ACVDR (4.2% v 9.4%), and the PCE risk classification was lower for about half of our participants. This is important for people with family histories of early onset CAD; absolute coronary risk may be their primary concern and the proportional reduction in absolute risk achievable with statin therapy is central to management discussions with their clinicians.
Risk thresholds for statin therapy
Risk thresholds for statin therapy in Australian guidelines are higher than in more recent US and European guidelines that may better reflect falling drug prices and greater evidence of clinical benefit.3,6 As cardiovascular event rates for people with family histories of early onset CAD and coronary calcification exceed those associated with US guideline‐defined intermediate risk thresholds, our findings suggest that Australian patients are undertreated by international standards.9 However, the ACVDR identifies people with coronary artery calcium poorly, so that lowering the treatment threshold alone would lead to unnecessary treatment for a considerable number of patients.
Coronary artery calcium scoring
More than one‐half of our participants, despite family histories of early onset CAD and other risk factors, had zero calcium scores. Further, calcium scores could inform decisions about statin therapy and risk factor control in 430 participants (41%): statins might be considered for 416 below the 10% ACVDR 5‐year risk threshold with non‐zero calcium scores (only 61 of 477 people with non‐zero scores were identified by this threshold), but their use reconsidered for 14 treatment‐eligible participants with zero scores. Our data support the Cardiac Society of Australia and New Zealand position statement that calcium scores are most helpful in patients at intermediate 10‐year risk (10–20%).32 We propose a 5‐year ACVDR risk of 5% as a suitable threshold for coronary artery calcium scoring for patients with family histories of early onset CAD: in our study, this threshold identified all participants with a MESA risk exceeding 20%, and would minimise the proportion of scans yielding zero calcium scores.
ACVDR performance data are limited, but it has been reported that overestimation of 10‐year risk in an Australian population was greater with the 1991 and 2008 Framingham risk tools than with the PCE.33 In our study, the β coefficient for predicting the coronary risk‐specific MESA score was smaller for the ACVDR than the PCE, probably reflecting the inclusion of non‐coronary endpoints by the ACVDR. Further, the proportions of participants re‐classified at low 10‐year risk after including coronary artery calcium score were similar for the ACVDR and PCE. Improved ACVDR risk prediction may affect the cost‐effectiveness of systematic coronary calcium score testing. The numbers needed to scan to identify people with 5‐year ACVDR risk of 5% with calcium scores above zero (1.5) or 100 (3.9) could assist discussions about referring patients with family histories of early onset CAD for calcium scoring.
Limitations
Risk was based on a single clinical assessment of dynamic variables (blood pressure, lipid profile). Socio‐economic status inputs for PREDICT and ASSIGN risk scores were based on the Australian Bureau of Statistics IRSAD, which may not be an appropriate substitute for the original markers. Family history was self‐reported and ethnic background not routinely recorded for our participants, which may affect risk calculations, particularly with the PREDICT model, which includes these factors. As our data were derived from a randomised controlled trial (CAUGHT‐CAD), selection bias may affect the generalisability of our findings. As CT coronary artery calcium scanning was performed at various imaging services, inter‐observer variability and misclassification are possible. We assessed only risk models with publicly available algorithms.
We used the MESA tool as an external comparator because the prediction and management of coronary risk (rather than other events) is the main driver of clinical decision making in familial CAD and coronary artery calcium is a powerful predictor of coronary risk. The addition of calcium scoring may personalise the application of the ACVDR calculator, but the MESA tool has not been validated in an Australian population, and further outcome studies will be needed before changes to risk assessment and statin treatment thresholds in Australia can be recommended.
Conclusion
Risk estimation is central to primary prevention of cardiovascular disease. Australian guidelines for statin therapy minimise overtreatment, but can also lead to not treating patients with family histories of early onset CAD. The ACVDR is inferior to the PCE, SCORE, and CUORE models with respect to identifying people with non‐zero calcium scores. Coronary artery calcium scores could be used to re‐classify risk in one‐half of our sample, and could change decisions about statin treatment in 41%. A 5‐year predicted ACVDR of 5% for symptomatic atherosclerotic disease may be a suitable threshold for referring patients for coronary artery calcium scoring.
Box 1 – Pharmaceutical Benefits Schedule (PBS) statin therapy eligibility criteria at the commencement of our study (2016)13,*
|
Category |
Eligibility criteria (any) |
||||||||||||||
|
|
|||||||||||||||
|
Diabetes mellitus |
|
||||||||||||||
|
Hypertension |
|
||||||||||||||
|
Aboriginal or Torres Strait Islander |
|
||||||||||||||
|
Family history of symptomatic coronary heart disease† |
|
||||||||||||||
|
|
|||||||||||||||
|
* The PBS indication for statin therapy for primary prevention has since been extended to all people over 60 years of age with diabetes and to people of any age with systolic blood pressure of 180 mmHg or more or diastolic blood pressure of 110 mmHg or more, and also includes other people excluded from our study (eg, people with chronic kidney disease or a 5‐year risk of cardiovascular disease greater than 15%).13 † First degree relative under 60 or second degree relative under 50 years of age. |
|||||||||||||||
Box 2 – Characteristics of the cardiovascular disease risk prediction models discussed (adapted from reference 4)
|
Characteristic |
MESA18 |
||||||||||||||
|
|
|||||||||||||||
|
Age range (years) |
40–65 |
30–75 |
30–74 |
20–79 |
30–74 |
35–69 |
45–85 |
Indigenous Australians: 35–74 |
|||||||
|
Sex |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
|||||||
|
Total cholesterol |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
|||||||
|
High‐density lipoprotein cholesterol |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
|||||||
|
Statin therapy |
No |
No |
No |
No |
Yes |
No |
Yes |
No |
|||||||
|
Smoking |
Yes |
Yes |
Cigarettes per day |
Yes |
Non‐, ex‐, current smoker |
Yes |
Yes |
Yes |
|||||||
|
Systolic blood pressure |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
|||||||
|
Treatment for hypertension |
Yes |
Yes |
No |
Yes |
Yes |
Yes |
Yes |
No |
|||||||
|
Diabetes mellitus |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
|||||||
|
Country |
Yes (high/low risk) |
USA |
Scotland |
USA |
New Zealand |
Italy |
USA |
Australia |
|||||||
|
Socio‐economic status |
No |
No |
Yes (SIMD) |
No |
Yes |
No |
No |
No |
|||||||
|
Family history |
No |
No |
Yes (first‐degree relative under 60) |
No |
Yes |
No |
Yes |
No |
|||||||
|
Other |
No |
No |
No |
Ethnic background |
Ethnic background, atrial fibrillation, anti‐thrombotic therapy |
No |
Coronary artery calcium score |
Electrocardiography: left ventricular hypertrophy |
|||||||
|
Study date |
2003 |
2008 |
2008 |
No |
2018 |
2007 |
2015 |
2009 |
|||||||
|
Study data |
12 pooled prospective studies |
Framingham Heart and Offspring Studies |
SHHEC prospective study |
4 pooled prospective studies |
Single prospective cohort study |
Prospective (fixed Italian cohort of 12 random samples) |
Prospective MESA study; validated: HNR, DHS |
Based on Australian disease rates |
|||||||
|
Sample size |
117 098 men; |
3969 men; |
6540 men; |
10 745 men; |
226 053 men; |
7056 men; |
6814 participants |
Calibrated with FRS |
|||||||
|
Time course |
10 years |
10 years |
10 years |
10 years |
5 years |
10 year |
10 years |
5 years |
|||||||
|
Outcome |
Cardiovascular disease mortality (coronary artery disease‐ and stroke‐specific mortality) |
Fatal and non‐fatal cardiovascular events (coronary, coronary insufficiency, angina, stroke, peripheral artery disease, heart failure) |
Fatal and non‐fatal major coronary and stroke events, any hospital discharge diagnosis of coronary heart disease or coronary interventions |
Fatal and non‐fatal myocardial infarction, coronary artery disease death, fatal or non‐fatal stroke |
Fatal and non‐fatal cardiovascular disease, including stroke, peripheral vascular disease and heart failure; coronary insufficiency, angina |
Fatal and non‐fatal major coronary and stroke events; revascularisation included, but not angina |
Incident hard coronary heart disease (myocardial infarction, cardiac arrest, fatal coronary heart disease, revascularisation for prior or concurrent angina) |
Based on FRS: fatal and non‐fatal cardiovascular disease, including peripheral artery disease, stroke, renovascular disease, heart failure, angina, coronary insufficiency |
|||||||
|
Risk categories |
Low: < 1% |
Low: < 10% |
Low: < 20% |
Low: < 5% |
Low: < 5% |
Low: < 3% |
Not stated |
Low: < 10% |
|||||||
|
|
|||||||||||||||
|
ACVDR = Australian absolute cardiovascular disease risk calculator; DHS = Dallas Heart Study; HNR = Heinz Nixdorf Recall Study; MESA = Multi‐Ethnic Study of Atherosclerosis; SCORE = European Systematic Coronary Risk Evaluation; SIMD = Scottish Index of Multiple Deprivation; SHHEC = Scottish Heart Health Extended Cohort Study. |
|||||||||||||||
Box 3 – Baseline characteristics of the 1059 study participants, by coronary artery calcium score
|
|
Coronary artery calcium score |
|
|||||||||||||
|
Zero |
Non‐zero |
P |
|||||||||||||
|
|
|||||||||||||||
|
Number of participants |
582 |
477 |
|
||||||||||||
|
Age (years), median (IQR) |
54 (48–59) |
59 (54–63) |
< 0.001 |
||||||||||||
|
Age of relative at CAD onset (years), median (IQR)* |
52 (48–57) |
52 (48–57) |
0.55 |
||||||||||||
|
Sex (men) |
228 (39%) |
286 (60%) |
< 0.001 |
||||||||||||
|
Total cholesterol (mmol/L), median (IQR) |
5.5 (5.0–6.0) |
5.6 (5.1–6.0) |
0.41 |
||||||||||||
|
High‐density lipoprotein cholesterol (mmol/L), median (IQR) |
1.5 (1.2–1.8) |
1.4 (1.2–1.7) |
0.15 |
||||||||||||
|
Smoking |
|
|
0.38 |
||||||||||||
|
Non‐smoker |
344 (60%) |
269 (56%) |
|
||||||||||||
|
Ex‐smoker |
203 (35%) |
182 (38%) |
|
||||||||||||
|
Weekly smoker |
9 (2%) |
4 (1%) |
|
||||||||||||
|
Daily smoker |
20 (4%) |
22 (5%) |
|
||||||||||||
|
Systolic blood pressure (mmHg), mean (SD) |
130 (14) |
130 (13) |
0.76 |
||||||||||||
|
Treated for hypertension |
87 (15%) |
101 (21%) |
0.011 |
||||||||||||
|
Diabetes mellitus |
8 (1%) |
9 (2%) |
0.68 |
||||||||||||
|
IRSAD, median (IQR) |
1029 (985–1072) |
1034 (985–1073) |
0.52 |
||||||||||||
|
5‐year ACVDR, median (IQR) |
3.2% (2.0–4.6%) |
4.8% (2.9–7.6%) |
< 0.001 |
||||||||||||
|
|
|||||||||||||||
|
ACVDR = Australian Absolute Cardiovascular Disease Risk; CAD = coronary artery disease; IQR = interquartile range; IRSAD = Index of Relative Social Advantage and Disadvantage; SD = standard deviation. * Age of the youngest relevant relative; first degree preferred to second degree relative when both eligible. |
|||||||||||||||
Box 4 – Cardiovascular risk thresholds in Australia and the United States, and coronary artery calcification
|
|
Australia: 5‐year risk |
US: 10‐year risk |
|||||||||||||
|
ACVDR: ≥ 10% |
ACVDR: ≥ 5% |
PCE: ≥ 7.5% |
|||||||||||||
|
|
|||||||||||||||
|
Number of participants |
75 |
337 |
256 |
||||||||||||
|
Coronary calcium score > 0 |
61 |
219 |
190 |
||||||||||||
|
Accuracy (of risk tool)* |
629/1059 (59%) |
683/1059 (65%) |
706/1059 (67%) |
||||||||||||
|
Sensitivity |
61/477 (13%) |
219/477 (46%) |
190/477 (40%) |
||||||||||||
|
Specificity |
568/582 (98%) |
464/582 (80%) |
516/582 (89%) |
||||||||||||
|
Positive predictive value |
61/75 (81%) |
219/337 (65%) |
190/256 (74%) |
||||||||||||
|
Negative predictive value |
568/984 (58%) |
464/722 (64%) |
516/803 (64%) |
||||||||||||
|
Coronary calcium score ≥ 100 |
35 |
86 |
80 |
||||||||||||
|
Accuracy (of risk tool) |
903/1059 (85%) |
743/1059 (70%) |
812/1059 (77%) |
||||||||||||
|
Sensitivity |
35/151 (23%) |
86/151 (57%) |
80/151 (53%) |
||||||||||||
|
Specificity |
868/908 (96%) |
657/908 (72%) |
732/908 (81%) |
||||||||||||
|
Positive predictive value |
35/75 (47%) |
86/337 (26%) |
80/256 (31%) |
||||||||||||
|
|
|||||||||||||||
|
ACVDR = Australian absolute cardiovascular risk; PCE = pooled cohort equation. * Accuracy = (true positives + true negatives)/total population, whereby “true positive” is defined as concurrence of the respective risk level being reached and the presence of coronary calcium, and “true negative” as the concurrence of the respective risk level not being reached and the absence of coronary calcium. |
|||||||||||||||
Box 5 – Sensitivity of risk prediction models with respect to including people with non‐zero coronary calcium scores: receiver operator characteristic curves
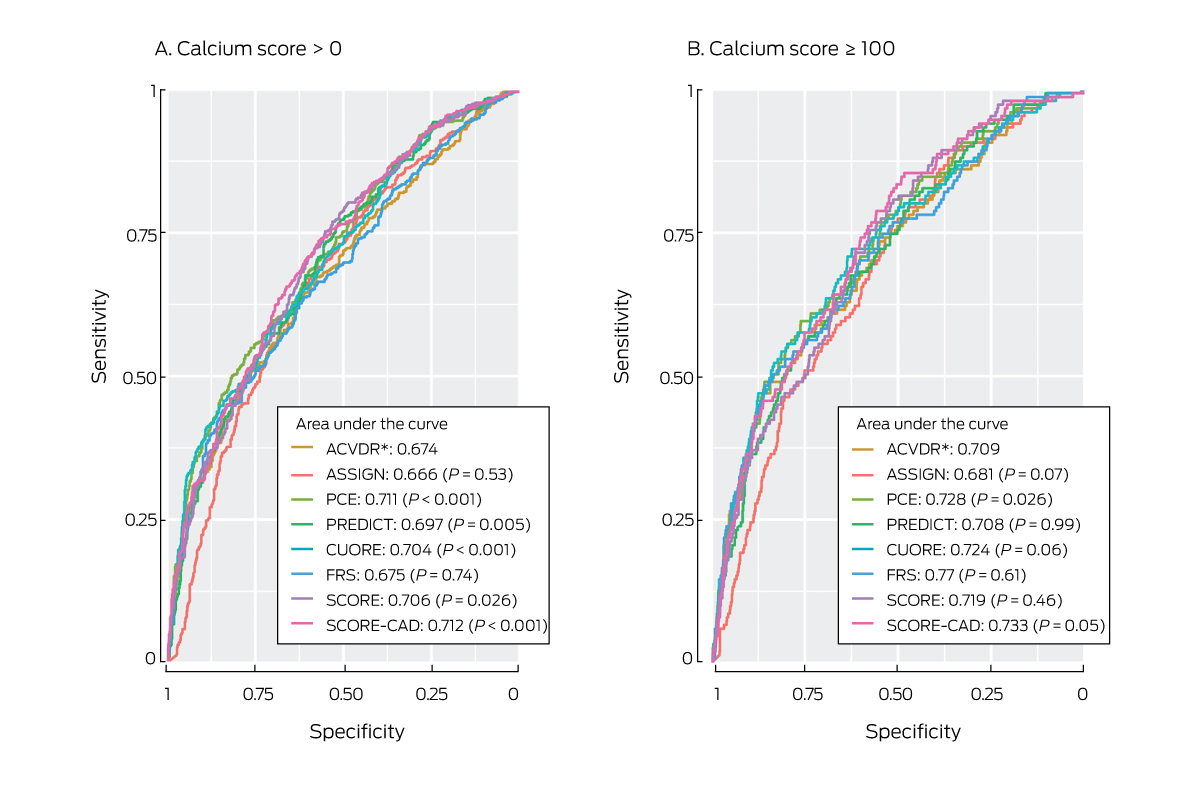
ACVDR = Australian absolute cardiovascular disease risk calculator; AUC = area under the receiver operator curve; FRS = Framingham risk score; PCE = pooled cohort equation; SCORE = European Systematic Coronary Risk Evaluation.
* Reference for comparison with other models.
Box 6 – Associations between coronary artery calcium score and the age and proximity of index relatives: odds ratios with 95% confidence intervals
|
Characteristic of index relative |
Coronary artery calcium score |
||||||||||||||
|
Non‐zero |
100 or more |
||||||||||||||
|
|
|||||||||||||||
|
Age: 40 years or less (v older than 40 years) |
0.93 (0.63–1.37) |
0.97 (0.54–1.65) |
|||||||||||||
|
Age: 50 years or less (v older than 50 years) |
0.98 (0.77–1.25) |
0.95 (0.67–1.34) |
|||||||||||||
|
First (v second) degree relative |
1.30 (0.83–2.09) |
0.97 (0.53–1.90) |
|||||||||||||
|
|
|||||||||||||||
|
|
|||||||||||||||
Box 7 – Comparison of predicted 10‐year cardiovascular risk by the Australian absolute cardiovascular disease risk (ACVDR) calculator and the pooled cohort equation, and coronary artery calcium scores
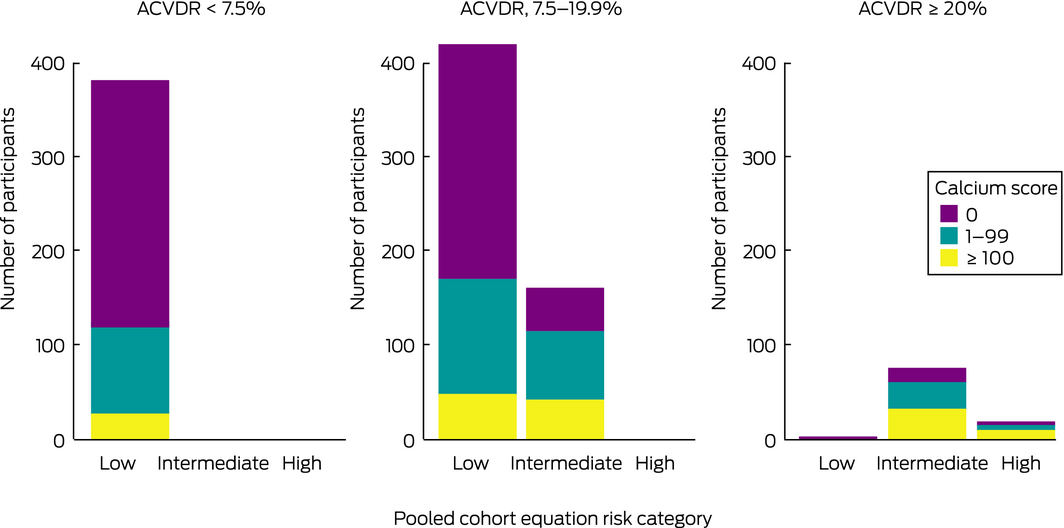
Box 8 – Comparison of predicted 10‐year cardiovascular risk by the Australian absolute cardiovascular disease risk (ACVDR) calculator* and the pooled cohort equation with Multi‐Ethnic Study of Atherosclerosis (MESA) risk classification
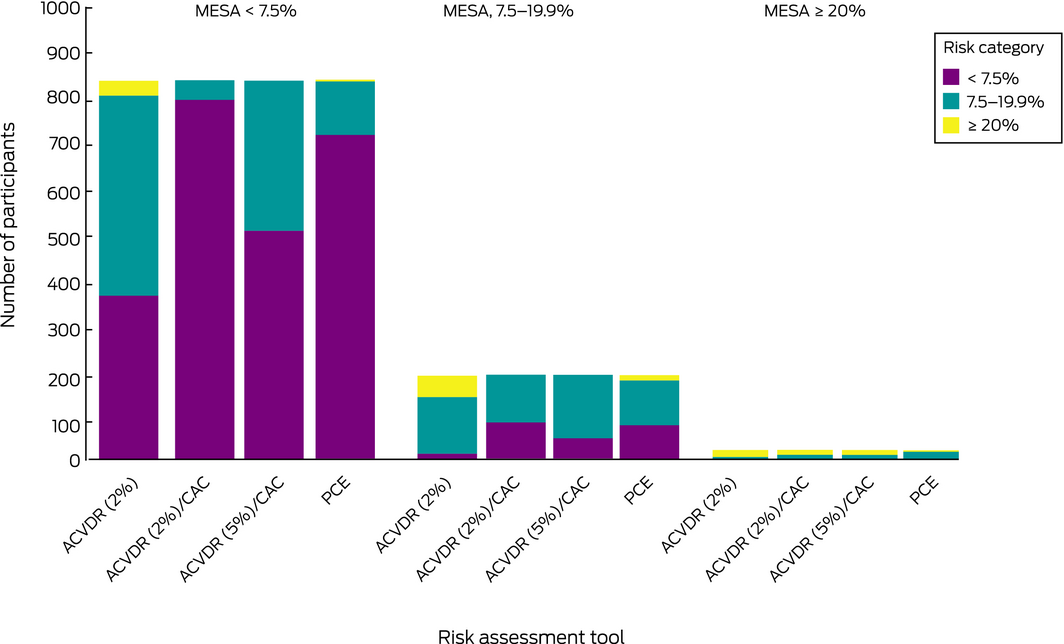
CAC = coronary artery calcium scoring. * The results of two inclusion ACVDR risk level thresholds for scanning are shown: 2% (with and without calcium scoring) and 5% (with calcium scoring). Numbers of participants by MESA risk group: < 7.5%: 851; 7.5–19.9%, 188; ≥ 20%, 20.
Received 2 October 2019, accepted 26 March 2020
- Prasanna Venkataraman1
- Tony Stanton2
- Danny Liew3
- Quan Huynh4
- Stephen J Nicholls3,5
- Geoffrey K Mitchell2
- Gerald F Watts6
- Andrew Maxwell Tonkin3
- Thomas H Marwick1
- 1 Baker IDI Heart and Diabetes Institute, Melbourne, VIC
- 2 University of Queensland, Brisbane, QLD
- 3 Monash University, Melbourne, VIC
- 4 Menzies Institute for Medical Research, University of Tasmania, Hobart, TAS
- 5 Monash Medical Centre, Melbourne, VIC
- 6 University of Western Australia, Perth, WA
This study was supported by a project grant (GRT1080582) and Postgraduate Scholarship for Prasanna Venkataraman from the National Health and Medical Research Council, and by the Wishlist Sunshine Coast Health Foundation. We acknowledge the commitment of our volunteers and the tireless work of the study coordinators, Kristyn Whitmore (Hobart), Jackie Ryan (Perth), Jasmine Pritchard, Joanne Harris and Louise Brown (Melbourne), Sara McLennan (Brisbane), and Jessica Phillips and Kristen Fragnito (Adelaide).
No relevant disclosures.
- 1. Banks E, Crouch SR, Korda RJ, et al. Absolute risk of cardiovascular disease events, and blood pressure‐ and lipid‐lowering therapy in Australia. Med J Aust 2016; 204: 320. https://www.mja.com.au/journal/2016/204/8/absolute-risk-cardiovascular-disease-events-and-blood-pressure-and-lipid
- 2. Australian Department of Health. New MBS items for heart health check. Updated Mar 2019. http://www.mbsonline.gov.au/internet/mbsonline/publishing.nsf/Content/Factsheet-HeartHealthCheck (viewed Jan 2020).
- 3. National Vascular Disease Prevention Alliance. Guidelines for the management of absolute cardiovascular disease risk. 2012. http://www.cvdcheck.org.au/pdf/Absolute_CVD_Risk_Full_Guidelines.pdf (viewed Jan 2020).
- 4. Piepoli MF, Hoes AW, Agewall S, et al; ESC Scientific Document Group. 2016 European guidelines on cardiovascular disease prevention in clinical practice. Eur Heart J 2016; 37: 2315–2381.
- 5. National Vascular Disease Prevention Alliance. Australian absolute cardiovascular risk calculator. 2012. http://cvdcheck.org.au (viewed Jan 2020).
- 6. Arnett DK, Blumenthal RS, Albert MA, et al. 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol 2019; 74: e177–e232.
- 7. Kral BG, Becker LC, Vaidya D, et al. Noncalcified coronary plaque volumes in healthy people with a family history of early onset coronary artery disease. Circ Cardiovasc Imaging 2014; 7: 446–453.
- 8. Nasir K, Bittencourt MS, Blaha MJ, et al. Implications of coronary artery calcium testing among statin candidates according to American College of Cardiology/American Heart Association cholesterol management guidelines: MESA (Multi‐Ethnic Study of Atherosclerosis). J Am Coll Cardiol 2015; 66: 1657–1668.
- 9. Paixao AR, Berry JD, Neeland IJ, et al. Coronary artery calcification and family history of myocardial infarction in the Dallas Heart Study. JACC Cardiovasc Imaging 2014; 7: 679–686.
- 10. Mitchell JD, Fergestrom N, Gage BF, et al. Impact of statins on cardiovascular outcomes following coronary artery calcium scoring. J Am Coll Cardiol 2018; 72: 3233–3242.
- 11. Baigent C, Keech A, Kearney PM, et al; Cholesterol Treatment Trialists’ Collaborators. Efficacy and safety of cholesterol‐lowering treatment: prospective meta‐analysis of data from 90 056 participants in 14 randomised trials of statins. Lancet 2005; 366: 1267–1278.
- 12. Marwick TH, Whitmore K, Nicholls SJ, et al. Rationale and design of a trial to personalize risk assessment in familial coronary artery disease. Am Heart J 2018; 199: 22–30.
- 13. Deakin University Centre for Population Health Research, Health Technology Assessment Team. Ezetimibe review: review of clinical guidelines (appendix G to Post‐market review of ezetimibe: final report to the Pharmaceutical Benefits Advisory Committee). 24 Nov 2016. http://www.pbs.gov.au/reviews/ezetimibe-review-files/appendix-g-review-of-clinical-guidelines.pdf (viewed June 2020).
- 14. Woodward M, Brindle P, Tunstall‐Pedoe H; SIGN group on risk estimation. Adding social deprivation and family history to cardiovascular risk assessment: the ASSIGN score from the Scottish Heart Health Extended Cohort (SHHEC). Heart 2007; 93: 172–176.
- 15. National Prescribing Service. Australian absolute cardiovascular disease risk calculator functional specifications. Sydney: NPL, 2009.
- 16. Pylypchuk R, Wells S, Kerr A, et al. Cardiovascular disease risk prediction equations in 400 000 primary care patients in New Zealand: a derivation and validation study. Lancet 2018; 391: 1897–1907.
- 17. Conroy RM, Pyorala K, Fitzgerald AP, et al; SCORE project group. Estimation of ten‐year risk of fatal cardiovascular disease in Europe: the SCORE project. Eur Heart J 2003; 24: 987–1003.
- 18. McClelland RL, Jorgensen NW, Budoff M, et al. 10‐year coronary heart disease risk prediction using coronary artery calcium and traditional risk factors: derivation in the MESA (Multi‐Ethnic Study of Atherosclerosis) with validation in the HNR (Heinz Nixdorf Recall) study and the DHS (Dallas Heart Study). J Am Coll Cardiol 2015; 66: 1643–1653.
- 19. Goff DC, Lloyd‐Jones DM, Bennett G, et al; American College of Cardiology/American Heart Association Task Force on Practice Guidelines. 2013 ACC/AHA guideline on the assessment of cardiovascular risk: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation 2014; 129 (25 Suppl 2): S49–S73.
- 20. D'Agostino RB, Vasan RS, Pencina MJ, et al. General cardiovascular risk profile for use in primary care: the Framingham Heart Study. Circulation 2008; 117: 743–753.
- 21. Giampaoli S, Palmieri L, Donfrancesco C, et al. Cardiovascular risk assessment in Italy: the CUORE Project risk score and risk chart. Ital J Public Health 2007; 4: 102–109.
- 22. National Cholesterol Education Program (NCEP) Expert Panel. Detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III): third (final) report. Circulation 2002; 106: 3143–3421.
- 23. Scottish Intercollegiate Guideline Network. Risk estimation and prevention of cardiovascular disease: a national clinical guideline (SIGN 149). Edinburgh: Healthcare Improvement Scotland, 2017. https://www.sign.ac.uk/assets/sign149.pdf (viewed Jan 2020).
- 24. Ministry of Health (New Zealand). Cardiovascular disease risk assessment and management for primary care (HP 6747). Wellington: Ministry of Health, 2018. https://www.health.govt.nz/publication/cardiovascular-disease-risk-assessment-and-management-primary-care (viewed Jan 2020).
- 25. Palmieri L, Rielli R, Demattè L, et al. CUORE project: implementation of the 10‐year risk score. Eur J Cardiovasc Prev Rehabil 2011; 18: 642–649.
- 26. Australian Bureau of Statistics. 2033.0.55.001. Census of population and housing: Socio‐Economic Indexes for Areas (SEIFA), Australia, 2016. Mar 2018. https://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/2033.0.55.0012016?OpenDocument#Publications (viewed Jan 2020).
- 27. Hanley JA, McNeil BJ. A method of comparing the areas under receiver operating characteristic curves derived from the same cases. Radiology 1983; 148: 839–843.
- 28. Youden WJ. Index for rating diagnostic tests. Cancer 1950; 3: 32–35.
- 29. Dragano N, Hoffmann B, Stang A, et al; Heinz Nixdorf Recall Study Investigative Group. Subclinical coronary atherosclerosis and neighbourhood deprivation in an urban region. Eur J Epidemiol 2009; 24: 25–35.
- 30. Hippisley‐Cox J, Coupland C, Vinogradova Y, et al. Performance of the QRISK cardiovascular risk prediction algorithm in an independent UK sample of patients from general practice: a validation study. Heart 2008; 94: 34–39.
- 31. Greenland P, Blaha MJ, Budoff MJ, et al. Coronary calcium score and cardiovascular risk. J Am Coll Cardiol 2018; 72: 434–447.
- 32. Hamilton‐Craig CR, Chow CK, Younger JF, et al. Cardiac Society of Australia and New Zealand position statement executive summary: coronary artery calcium scoring. Med J Aust 2017; 207: 357–361. https://www.mja.com.au/journal/2017/207/8/cardiac-society-australia-and-new-zealand-position-statement-executive-summary
- 33. Albarqouni L, Doust JA, Magliano D, et al. External validation and comparison of four cardiovascular risk prediction models with data from the Australian Diabetes, Obesity and Lifestyle study. Med J Aust 2019; 220: 161–167. https://www.mja.com.au/journal/2019/210/4/external-validation-and-comparison-four-cardiovascular-risk-prediction-models





Abstract
Objectives: To assess the predictive value of the Australian absolute cardiovascular disease risk (ACVDR) calculator and other assessment tools for identifying Australians with family histories of early onset coronary artery disease (CAD) who have coronary artery calcification.
Design, setting, participants: People without known CAD were recruited at seven Australian hospitals, October 2016 – January 2019. Participants were aged 40–70 years, had a family history of early onset CAD, and a 5‐year ACVDR of 2–15%.
Main outcome measures: CT coronary artery calcium score greater than zero (any coronary calcification) or greater than 100 (calcification warranting lipid therapy).
Results: 1059 participants were recruited; 477 (45%) had non‐zero coronary artery calcium scores (median 5‐year ACVDR, 4.8% [IQR, 2.9–7.6%]; median coronary artery calcium score, 41.7 [IQR, 8–124]); 582 (55%) did not (median 5‐year ACVDR, 3.2% [IQR, 2.0–4.6%]). Of 151 participants with calcium scores of 100 or more, 116 (77%) were deemed to be at low cardiovascular risk by Australian guidelines, while 14 of 75 participants at intermediate risk (19%) had zero calcium scores. The sensitivity of the ACVDR calculator for identifying people with non‐zero calcium scores (area under receiver operator curve [AUC], 0.674) was lower than that of the pooled cohort equation (AUC, 0.711; P < 0.001). ACVDR (10‐year)‐ and Multi‐Ethnic Study of Atherosclerosis (MESA)‐predicted risk categories concurred for 511 participants (48%); classifications were concordant for 925 participants (87%) when the ACVDR was supplemented by calcium scores.
Conclusions: Coronary artery calcium scoring should be considered as part of the heart health check for patients at intermediate ACVDR risk and with family histories of early onset CAD. Alternative risk calculators may better select such patients for further diagnostic testing and primary prevention therapy.
Trial registration: Australian New Zealand Clinical Trials Registry, ACTRN 12614001294640; 11 December 2014 (prospective).