The known Privately insured patients often undertake inpatient rehabilitation after total knee arthroplasty, but there is no evidence that it improves recovery after surgery.
The new Rehabilitation pathways incorporating inpatient rehabilitation were significantly more expensive, but did not achieve patient-reported recovery superior to that of pathways not including inpatient rehabilitation.
The implications Given the substantial difference in costs, better value alternatives than inpatient rehabilitation should be considered for patients who have not experienced a major complication or progressed slowly after total knee arthroplasty.
Annual rates of total knee arthroplasty (TKA) have been increasing in Australia since 2003; 50 623 primary TKA procedures were undertaken in 2015, 6.1% higher than in 2014.1 This trend is consistent with those in other countries.2,3 The procedure reduces pain, improves function, and enhances health-related quality of life, but is expensive;4 TKA is often cited as a major driver of increases in private health insurance premiums.5,6
An important but underappreciated contributor to the overall cost of TKA is post-operative care in an inpatient rehabilitation facility. Two large private insurers in Australia indicated that the average rebate per overnight stay in 2015 was $700 (personal communication); as the average length of stay is 12 days, the average total rebated cost is $8400. Inpatient rehabilitation is more common in the private sector because privately insured health care consumers have ready access to (private) rehabilitation beds, but public health care patients do not; about 40% of TKA patients with private insurance reportedly undergo inpatient rehabilitation, compared with 5–10% of those not privately insured.7
It is unknown whether inequity in access undermines recovery from surgery, as little research has been undertaken in this area.8,9 Because privately insured patients are reluctant to be randomised to a therapy other than the one to which they feel entitled, it is difficult to conduct a randomised controlled trial (RCT) that compares the most resource-intensive pathway (inpatient rehabilitation) with less resource-intensive alternatives. The preferences of orthopaedic surgeons and carers, the preferences of patients about being discharged directly home, and the relationships between treatment centres and rehabilitation facilities are other factors that make RCTs difficult.
In an attempt to redress the lack of research in this area, we conducted a propensity score-matched cohort study of privately insured TKA patients, in which we compared the effectiveness of a rehabilitation pathway including inpatient rehabilitation with one that did not. A propensity score is the conditional probability of treatment assignment according to observed baseline characteristics.10,11 We matched people on their propensity scores to minimise bias associated with being allocated to a particular treatment (in this case, inpatient therapy) on the basis of baseline patient characteristics.10-13 This approach is superior to traditional multiple regression techniques because treatment effects are reported in the same manner as if an RCT had been undertaken, facilitating interpretation.10,11 We hypothesised that the more expensive inpatient rehabilitation pathway would yield better joint-specific and general health outcomes in the short and longer term than a pathway not including inpatient rehabilitation. We also estimated rehabilitation provider charges for the two pathways.
Method
This study was nested in a national, prospective observational investigation of the relationships between care received and outcomes after knee or hip arthroplasty (ClinicalTrials.gov identifier: NCT01899443).
Sampling and hospital recruitment
In the larger study, public and private hospitals performing more than 275 TKA or total hip arthroplasty procedures during 2012 were eligible to participate. Eligible hospitals were identified by their listing in the Australian Orthopaedic Association National Joint Replacement Registry.1 The sampling procedure has been described in detail elsewhere.14 The original sample included ten public and nine private hospitals from five Australian states (all except Western Australia).
Patient enrolment and eligibility
During August 2013 – December 2014, people awaiting arthroplasty secondary to osteoarthritis were screened by site coordinators during their pre-admission review. Patients were eligible for the larger study if the arthroplasty was the primary surgery and undertaken no later than January 2015; no further arthroplasty within 3 months of the first was planned; and the patient was able to understand the protocol, and could be followed up by telephone for 12 months. An additional inclusion criterion for this nested study was that the patient had private insurance cover for the surgery. To eliminate treatment selection bias and to improve generalisability to uncomplicated TKA, we excluded patients referred to inpatient rehabilitation because of slow progress, and those who had conditions that would alter their typical recovery and rehabilitation pathway, such as simultaneous bilateral surgeries, as well as those who experienced a significant complication within 90 days of surgery. We therefore only included patients for whom the rehabilitation pathway was not dictated by a medical or physical indication and the decision for inpatient therapy was probably made prior to surgery.
Data collection
The following baseline data were collected at the time of patient consent: weight and height; insurance status; comorbid conditions, including requirement for daily medication; education level; presence of other lower limb or back conditions that impair mobility; and the patient-reported outcomes measures described below. Site coordinators provided additional patient-specific data in forms completed by clinicians, including American Society of Anesthesiologists (ASA) scores, complications, hospital length of stay (LOS), and discharge destination, with reason for the specific destination. Thirty-five day, 90-day, and 365-day outcomes, and data on time off work (for patient and carer) were obtained in telephone follow-up interviews. For quality control, clinician-reported data were re-abstracted from medical records, and significant complications reported by patients during follow-up were verified by treating hospitals, general practitioners, or orthopaedic surgeons.
Complications
Acute complications were coded according to the Clavien–Dindo classification,15 based on the type of care deviation necessitated by the complication. Patients experiencing a complication during their acute admission (typically grade 3 or higher) that probably required referral to inpatient rehabilitation were flagged. Complications graded as less severe, but which would probably undermine rehabilitation (such as footdrop or knee instability requiring bracing), were also flagged. Complications and unrelated health events manifested after discharge (including re-admission within 90 days) were also captured, as they potentially affect the continuity of rehabilitation.
Outcomes
Primary patient-reported outcomes included the Oxford Knee Score (OKS; at 90 and 365 days)16 and the EuroQol Visual Analogue Scale for “today” health (EQ-VAS; at 35, 90 and 365 days).17 The OKS comprises 12 joint-specific Likert-style questions about pain and functional impairment during the previous month; responses are scored from 0 (maximal discomfort/pain or maximal impairment) to 4 (no pain/discomfort or impairment), providing a total score out of 48; higher scores indicate better joint status. EQ-VAS is a scaled measure of how the respondent perceives their own overall health on the day, from 0 (worst health imaginable) to 100 (best health imaginable). Baseline scores were based on responses by patients to the printed survey, while follow-up scores were collected by telephone interview; the two approaches have been shown to be equivalent.17
Rehabilitation charges were determined from the perspective of the provider. Adjustments for inflation were made if the source document for costs was published before 2015.18 Overall provider charges for each participant were based on the types of therapy received up to ten weeks after surgery. The unit costs applied and the associated justification are provided in online Appendix 1.
Statistical analysis
The sample size for this nested study was dictated by the projected sample size for the main study (n = 2000). Given the sample size required to detect a conventionally defined moderate treatment effect19 (half the standard deviation of the baseline mean) for a continuous outcome is 128, we conservatively anticipated we would have sufficient power (at a = 0.05) to detect a moderate effect.
Normality of data was assessed prior to analysis. Descriptive statistics were used to characterise the cohorts. The covariates of the unmatched cohorts were assessed in independent t and ?2 tests; outcomes data were analysed in paired t tests, Wilcoxon signed rank tests, and McNemar tests, as were the covariates in the matched cohorts.
Propensity scores (PSs) for the prediction of referral to inpatient rehabilitation were estimated for all eligible patients and used to match each patient who received inpatient rehabilitation with one who did not (1:1). PSs were determined by unconditional logistic regression, with the outcome being treatment group; the predictors (covariates) were variables known or thought to influence either treatment allocation prior to surgery or the primary outcomes.10-13 Covariates included in the model were the continuous variables baseline OKS and EQ-VAS scores, age and body mass index, and the categorical or ordinal variables sex, ASA scores, comorbidity, other lower limb or back problems limiting mobility, and education level.
We applied caliper matching without replacement to determine the matched pairs.10,11 An absolute difference in PS of 0.05 was initially trialled; a caliper distance of 0.03 (equivalent to one-fifth of the pooled standard deviation of the PS) improved matching.11 Successful matching was primarily deemed to be indicated by a standardised difference between the groups of less than 0.10 for a variable;11,13 a marginally greater difference was tolerated if the variable was not significantly different in both the pre- and post-matched cohorts. We did not rely upon changes in significance alone (from significance to non-significance), given the reduction in sample size that inevitably accompanies matching and the consequently increased likelihood of type II errors.13 Variables not included in the matching were interaction terms, employment status (presumed not to influence treatment allocation or primary outcomes), and “surgeon” and “hospital” (their inclusion caused non-convergence of the estimate in the PS calculation, a consequence of the high correlation between surgeon or hospital and treatment). In response to this last problem, we performed multiple linear regression analyses that incorporated “hospital” for the entire eligible cohort (online Appendix 2).
Several patients had a second arthroplasty (different joint) or experienced a major health event, such as hip surgery, between 90 and 365 days after surgery. We conducted sensitivity analyses of the 365-day outcomes that excluded these patients, as these events could have affected the primary outcomes and were deemed to be unrelated to the mode of rehabilitation provided.
Ethics approval
Ethics approval for the main study was provided by nine human research ethics committees (HRECs): the Hunter New England HREC (New South Wales; reference, LNR/12/HNE/390); St Vincent’s Health and Aged Care HREC (Queensland; reference, HREC #13/10); Austin Health HREC (Victoria; reference, LNR/14/Austin/208 LNRR MAP); Barwon Health HREC (Victoria; reference, 13/82); Epworth HREC (Victoria; reference, LR138-13); Calvary Health Care Clinical and Research Ethics Committee (Tasmania; references, 2:05:13 and 5:13:12), and Calvary Healthcare Adelaide HREC (South Australia; reference, 13-CHREC-E007). Each participating patient provided written informed consent before their operation.
Results
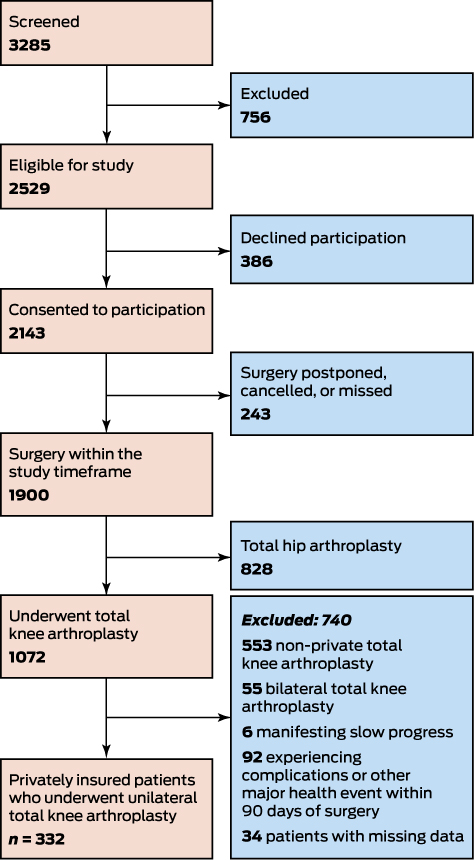
Cohort ascertainment is summarised in Box 1. A total of 129 pairs were matched from an eligible sample of 332 privately insured patients from 12 hospitals; 98% of patients had had their operations in private hospitals.
In the unmatched cohort, the group of patients discharged to inpatient rehabilitation had a lower mean “today” health score (P = 0.08), included more patients with lower ASA scores, and a higher proportion of men (P = 0.009), and had longer mean acute care LOS (P = 0.009) (Box 2). Matching reduced the standardised difference for 12 covariates included in the matching; the largest remaining mean difference in this group of covariates was 0.12 (Box 3). For the remaining covariates (including three of the four education categories), between-treatment group differences were not statistically significant in either the pre- or post-matched comparisons.
Matched cohort
Outcomes for the inpatient rehabilitation group were not superior at any time point (Box 4), and their “today” health ratings were significantly worse than those of the comparison group on Day 35 (P = 0.01). Median rehabilitation provider costs were 26 times as high for the inpatient group as for the comparison group (P < 0.001). After excluding inpatient rehabilitation charges, provider charges for the inpatient rehabilitation group were still three times as high because of the greater number of community physiotherapy visits (median, 8 visits; interquartile range [IQR], 5–11; for non-inpatients: median, 5 visits; IQR, 0–9; P < 0.001). The patients in this group also preferred comparatively expensive day hospital rehabilitation to other community-based alternatives (online Appendix 3). Time off work for patients and carers was not statistically significantly lower for the inpatient group (Box 4).
Sensitivity analysis of 365-day outcomes yielded similar results (online Appendix 4).
Discussion
The authors of a Canadian RCT of knee and hip arthroplasty recipients reported that 18 days’ inpatient rehabilitation was not associated with better outcomes than an average of eight domiciliary physiotherapy sessions.9 Our own group recently completed the only RCT to have compared the efficacy of inpatient rehabilitation with that of a simple home program after TKA for public patients;8 we found that recovery of mobility and patient-reported outcomes were not superior for patients receiving inpatient therapy. The results of our current study of privately insured patients reinforce these findings. Further, the results for patients undergoing inpatient rehabilitation were not superior despite the fact that they received more community-based therapy.
Our study has several strengths. Propensity-based scoring helps reduce the bias inherent to observational studies, permitting researchers to more reliably estimate treatment effects.10-13 We used a national cohort from hospitals with high volumes of arthroplasty procedures, and the characteristics of the unmatched cohort were typical for patients who undergo TKA in Australia.4,8,17,20,21 Our matched cohort should therefore be a representative sample of such patients. Our PS strategy achieved acceptable matching between the cohorts on many variables purported to influence treatment allocation and outcomes. In addition to matching, our comprehensive screening and sensitivity analysis excluded patients with conditions that predisposed them to either requiring inpatient rehabilitation or a worse outcome, thereby eliminating these sources of confounding and bias.
A limitation of propensity-based scoring is that the extent to which bias is reduced depends on the degree to which covariates are matched.10-13 While the PSs and exclusion criteria accounted for many factors, unrecognised covariates may have remained unbalanced. Most notably, we could not account for the effects of “surgeon” or “hospital” because most surgeons and hospitals almost routinely referred patients to one pathway or the other. Our supplementary regression analysis (online Appendix 2) indicated that adding “hospital” (“hospital” and “surgeon” are highly correlated) did not influence the OKS outcome, but did affect EQ-VAS health scores, with a negative effect on the scores of those in the inpatient group. Prosthesis type was also not included in the matching, but patient-reported recovery in the short term appears not to be influenced by this factor.22,23
Recall bias may be a limitation of a study with respect to data on return to work and community-based therapy visits (and by extension, provider charges), but we have no reason to assume that this bias would have been more prominent in either treatment group. A larger sample size may have clarified the trends in time off work. The lack of objective markers of recovery might also be considered a limitation, although earlier research has not detected differences in such outcomes.8,9 Perhaps the most important limitation is that our results cannot be extrapolated to patients who experience significant complications, nor to those who are referred to inpatient rehabilitation because of poor progress. We therefore acknowledge that inpatient rehabilitation may be more beneficial for some subgroups of patients, and thus remains a valid treatment option.
In conclusion, our study provides new observations on the comparative effectiveness and costs of rehabilitation pathways for privately insured patients after uncomplicated TKA. Pathways involving inpatient rehabilitation are more expensive because of the costs of both the inpatient treatment and subsequent community-based therapy, but were not found to be associated with improved patient-reported outcomes. Alternatives to inpatient rehabilitation after uncomplicated TKA should therefore be considered first.
Box 2 – Characteristics of patients undergoing total knee arthroplasty, August 2013 – January 2015: before matching
|
|
Inpatient rehabilitation |
No inpatient rehabilitation |
Standardised mean difference* |
P |
|||||||||||
|
|
|||||||||||||||
|
Number of patients |
185 |
147 |
|
|
|||||||||||
|
Variables included in matching |
|
|
|
|
|||||||||||
|
Age (years), mean (SD) |
68.9 (8.9) |
67.2 (7.3) |
0.21 |
0.06 |
|||||||||||
|
Sex (men) |
117 (63%) |
72 (49%) |
0.29 |
0.009 |
|||||||||||
|
Body mass index (kg/m2), mean (SD) |
31.0 (6.0) |
30.4 (5.0) |
0.10 |
0.36 |
|||||||||||
|
Highest level of education |
|
|
|
|
|||||||||||
|
1 (no formal education) |
3 (2%) |
1 (1%) |
0.09 |
0.43 |
|||||||||||
|
2 (year 10 or less) |
43 (23%) |
35 (24%) |
0.00 |
1.0 |
|||||||||||
|
3 (year 11 or 12) |
100 (54%) |
86 (59%) |
0.09 |
0.42 |
|||||||||||
|
4 (tertiary degree) |
38 (21%) |
17.0 (25) |
0.09 |
0.41 |
|||||||||||
|
American Society of Anesthesiologists (ASA) score |
|
|
|
|
|||||||||||
|
1 (healthy) |
11 (6%) |
19 (13%) |
0.24 |
0.03 |
|||||||||||
|
2 (mild systemic disease) |
90 (49%) |
82 (56%) |
0.14 |
0.21 |
|||||||||||
|
3 (severe systemic disease) |
81 (44%) |
46 (31%) |
0.27 |
0.02 |
|||||||||||
|
4 (life-threatening severe systemic disease) |
2 (1%) |
0 |
0.15 |
0.20 |
|||||||||||
|
Comorbidity |
|
|
|
|
|||||||||||
|
None |
13 (7%) |
18 (12%) |
0.18 |
0.10 |
|||||||||||
|
Yes, but no daily medication |
10 (6%) |
8 (5%) |
0.02 |
0.84 |
|||||||||||
|
Yes, with daily medication |
181 (87%) |
121 (82%) |
0.13 |
0.23 |
|||||||||||
|
Oxford Knee Score, mean (SD) |
23.6 (8.7) |
25.2 (7.2) |
0.20 |
0.02 |
|||||||||||
|
EQ-VAS, mean (SD) |
71.8 (18.9) |
76.3 (14.4) |
0.27 |
0.08 |
|||||||||||
|
Other lower limb or back problems limiting mobility |
81 (44%) |
47.6 (70) |
0.08 |
0.49 |
|||||||||||
|
Variables not included in matching |
|
|
|
|
|||||||||||
|
Paid employment |
43 (23%) |
43 (29%) |
0.14 |
0.31 |
|||||||||||
|
Length of acute hospital stay (days), mean (SD) |
6.8 (2.2) |
6.2 (2.2) |
0.29 |
0.009 |
|||||||||||
|
|
|||||||||||||||
|
EQ-VAS = EuroQol Visual Analogue Scale. SD = standard deviation. For the Oxford Knee Score and EQ-VAS, higher scores indicate lesser joint impairment and better health respectively. 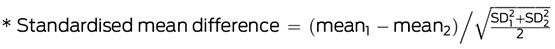 |
|||||||||||||||
Box 3 – Characteristics of patients undergoing total knee arthroplasty, August 2013 – January 2015: after matching
|
|
Inpatient rehabilitation group |
No inpatient rehabilitation group |
Standardised mean difference* |
P |
|||||||||||
|
|
|||||||||||||||
|
Number of patients |
129 |
129 |
|
|
|||||||||||
|
Propensity score, mean (SD) |
0.55 (0.13) |
0.53 (0.13) |
|
|
|||||||||||
|
Variables included in matching |
|
|
|
|
|||||||||||
|
Age (years), mean (SD) |
68.6 (9.2) |
67.6 (7.3) |
0.12 |
0.34 |
|||||||||||
|
Sex (men) |
75 (58%) |
69 (54%) |
0.09 |
0.45 |
|||||||||||
|
Body mass index (kg/m2), mean (SD) |
30.6 (5.9) |
30.7 (5.1) |
0.03 |
0.82 |
|||||||||||
|
Highest level of education |
|
|
|
|
|||||||||||
|
1 (no formal education) |
3 (2%) |
1 (1%) |
0.13 |
0.31 |
|||||||||||
|
2 (Year 10 or lower) |
28 (22%) |
34 (26%) |
0.11 |
0.38 |
|||||||||||
|
3 (Year 11 or 12) |
68 (53%) |
73 (57%) |
0.08 |
0.53 |
|||||||||||
|
4 (tertiary degree) |
30 (23%) |
21 (16%) |
0.18 |
0.16 |
|||||||||||
|
American Society of Anaesthesiologists (ASA) score |
|
|
|
|
|||||||||||
|
1 (healthy) |
10 (8%) |
10 (8%) |
0.00 |
1 |
|||||||||||
|
2 (mild systemic disease) |
70 (54%) |
74 (57%) |
0.06 |
0.62 |
|||||||||||
|
3 (severe systemic disease) |
49 (38%) |
45 (35%) |
0.06 |
0.60 |
|||||||||||
|
4 (life-threatening severe systemic disease) |
0 |
0 |
NA |
NA |
|||||||||||
|
Comorbidity |
|
|
|
|
|||||||||||
|
None |
7.8 (10) |
12 (9%) |
0.06 |
0.66 |
|||||||||||
|
Yes, but no daily medication |
3.1 (4) |
6 (5%) |
0.08 |
0.52 |
|||||||||||
|
Yes, with daily medication |
89.2 (115) |
111 (86%) |
0.09 |
0.45 |
|||||||||||
|
Oxford Knee Score, mean (SD) |
24.6 (8.4) |
24.7 (7.0) |
0.01 |
0.92 |
|||||||||||
|
EQ-VAS, mean (SD) |
74.9 (16.2) |
75.3 (14.8) |
0.02 |
0.84 |
|||||||||||
|
Other lower limb or back problems limiting mobility |
49.6 (64) |
48.1 (62) |
0.03 |
0.90 |
|||||||||||
|
Variables not included in matching |
|
|
|
|
|||||||||||
|
Paid employment |
28 (22%) |
34 (26%) |
0.11 |
0.67 |
|||||||||||
|
Length of acute hospital stay (days), mean (SD) |
6.5 (1.9) |
6.3 (2.8) |
0.12 |
0.60 |
|||||||||||
|
|
|||||||||||||||
|
EQ-VAS = EuroQol Visual Analogue Scale. NA = not applicable. SD = standard deviation. |
|||||||||||||||
Box 4 – Outcomes 35, 90 and 365 days after surgery for the matched cohort of patients receiving or not receiving inpatient rehabilitation (n = 129 per group)
|
Time |
Oxford Knee Score: median (IQR) |
EQ-VAS score: median (IQR) |
Rehabilitation costs: median (IQR) |
Rehabilitation costs, excluding inpatient rehabilitation: median (IQR) |
Patients with time off work (> 6 weeks): proportion (95% CI) |
Carers with time off work (any): proportion (95% CI) |
|||||||||
|
|
|||||||||||||||
|
35 days |
|
|
|
|
|
|
|||||||||
|
Inpatient rehabilitation |
— |
80 (70–87) |
— |
— |
— |
14.4% (8.9–22.3%) |
|||||||||
|
No inpatient rehabilitation |
— |
80 (75–90) |
— |
— |
— |
18.6% (12.3–27.1%) |
|||||||||
|
Median difference* |
— |
–5 (–19 to 10) |
— |
— |
— |
–4.2% (–12.8% to 4.4%) |
|||||||||
|
P |
— |
0.01 |
— |
— |
— |
0.34 |
|||||||||
|
90 days |
|
|
|
|
|
|
|||||||||
|
Inpatient rehabilitation |
40 (34–43) |
85 (75–90) |
$9978 ($7599–11 841) |
$1123 ($510–2296) |
16.1% (10.2–24.3%) |
— |
|||||||||
|
No inpatient rehabilitation |
40 (34–43) |
90 (80–91) |
$374 ($0–722) |
$374 ($0–722) |
18.6% (12.3–27.1%) |
— |
|||||||||
|
Median difference* |
0 (–6 to 5) |
–2.5 (–15 to 10) |
$9500 ($7000–11 497) |
$749 ($0–1980) |
–2.5% (–12.6% to 7.6%) |
— |
|||||||||
|
P |
0.54 |
0.09 |
< 0.001 |
< 0.001 |
0.62 |
— |
|||||||||
|
365 days |
|
|
|
|
|
|
|||||||||
|
Inpatient rehabilitation |
44 (42–45) |
85 (75–90) |
— |
— |
— |
— |
|||||||||
|
No inpatient rehabilitation |
44 (42–46) |
85 (80–90) |
— |
— |
— |
— |
|||||||||
|
Median difference* |
0 (–4 to 3) |
0 (–10 to 6) |
— |
— |
— |
— |
|||||||||
|
P |
0.40 |
0.32 |
— |
— |
— |
— |
|||||||||
|
|
|||||||||||||||
|
CI = confidence interval. EQ-VAS = EuroQol Visual Analogue Scale. IQR = interquartile range. * Inpatient rehabilitation group v no inpatient rehabilitation group. |
|||||||||||||||
Received 28 November 2016, accepted 21 March 2017
- Justine Maree Naylor1,2,3
- Andrew Hart1
- Rajat Mittal1
- Ian Harris1,2,3
- Wei Xuan1,2
- 1 South Western Sydney Clinical School, University of New South Wales, Sydney, NSW
- 2 Ingham Institute of Applied Medical Research, Sydney, NSW
- 3 South Western Sydney Local Health District, Sydney, NSW
This study was partially supported by a grant from the HCF Research Foundation to Justine Naylor, Ian Harris and Wei Xuan. We acknowledge the contribution made by Helen Badge, project manager of the larger investigation in which this study was nested.
This study was partially funded by a grant awarded by the HCF Research Foundation, but the funder had no influence on the study design or the research plan.
- 1. Australian Orthopaedic Association. National Joint Replacement Registry: hip, knee and shoulder arthroplasty annual report 2016. Adelaide: AOA, 2016. https://aoanjrr.sahmri.com/documents/10180/275066/Hip%2C%20Knee%20%26%20Shoulder%20Arthroplasty (accessed June 2017).
- 2. Hart A, Bergeron SG, Epure L, et al. Comparison of US and Canadian perioperative outcomes and hospital efficiency after total hip and knee arthroplasty. JAMA Surg 2015; 150: 990-998.
- 3. Briggs T. A national review of adult elective orthopaedic services in England: getting it right first time. London: British Orthopaedic Association, 2015. https://www.boa.ac.uk/wp-content/uploads/2015/03/GIRFT-National-Report-MarN.pdf (accessed Mar 2017).
- 4. Peel TN, Cheng AC, Liew D, et al. Direct hospital cost determinants following hip and knee arthroplasty. Arthritis Care Res 2015; 67: 782-790.
- 5. Health Insurance Consultants Australia. The growing cost of hip and knee replacements [media release]. 13 Feb 2014. http://www.hica.com.au/health-insurance-news/the-growing-cost-of-hip-and-knee-replacements (accessed Mar 2017).
- 6. Health Insurance Consultants Australia. New prostheses list advisory committee could reduce private insurance costs [media release]. 12 Sept 2016. http://www.hica.com.au/health-insurance-news/new-prostheses-list-advisory-committee-could-reduce-private-insurance-costs (accessed Mar 2017).
- 7. Buhagiar, MA, Naylor JM, Harris IA, et al. Hospital Inpatient versus HOme-based rehabilitation after knee arthroplasty (the HIHO study): study protocol for a randomized controlled trial. Trials 2013; 14: 432.
- 8. Buhagiar, MA, Naylor JM, Harris IA, et al. Effect of inpatient rehabilitation vs a monitored home program on mobility in patients with total knee arthroplasty: the HIHO randomized clinical trial. JAMA 2017; 317: 1037-1046.
- 9. Mahomed NN, Davis AM, Hawker G, et al. Inpatient compared with home-based rehabilitation following primary unilateral total hip or knee replacement: a randomized controlled trial. J Bone Joint Surg Am 2008; 90: 1673-1680.
- 10. Rosenbaum PR, Rubin DB. The central role of the propensity score in observational studies for causal effects. Biometrika 1983; 70: 41-55.
- 11. Austin PC. An introduction to propensity score methods for reducing the effects of confounding in observational studies. Multivariate Behav Res 2011; 46: 399-424.
- 12. D’Agostino RB. Tutorial in biostatistics. Propensity score methods for bias reduction in the comparison of a treatment to a non-randomized control group. Stat Med 1998; 17: 2265-2281.
- 13. Austin PC. Balance diagnostics for comparing the distribution of baseline covariates between treatment groups in propensity-score matched samples. Stat Med 2009; 28: 3083-3107.
- 14. Naylor JM, Descallar J, Grootemaat M, et al. Is satisfaction with the acute-care experience higher amongst consumers treated in the private sector? A survey of public and private sector arthroplasty recipients. PLoS One 2016; 11: e0159799.
- 15. Clavien PA, Barkun J, de Oliveira ML, et al. The Clavien-Dindo classification of surgical complications. Ann Surg 2009; 250; 187-196.
- 16. Murray DW, Fitzpatrick R, Rogers K, et al. The use of the Oxford hip and knee scores. J Bone Joint Surg Br 2007; 89-B: 1010-1014.
- 17. Chatterji R, Naylor JM, Harris IA, Descallar J. An equivalence study: are patient-completed and telephone interview equivalent modes of administration for the EuroQol survey? Health Qual Life Outcomes 2017; 15: 18.
- 18. Australian Bureau of Statistics. 6401.0. Consumer price index inflation calculator 2015. http://www.abs.gov.au/websitedbs/d3310114.nsf/home/Consumer+Price+Index+Inflation+Calculator (accessed Mar 2017).
- 19. Norman GR, Sloan JA, Wyrwich KW. Interpretation of changes in health-related quality of life: the remarkable universality of half a standard deviation. Med Care 2003; 41: 582-592.
- 20. Ko V, Naylor J, Harris I, et al. One-to-one therapy is not superior to group or home-based therapy after total knee arthroplasty: a randomized, superiority trial. J Bone Joint Surg Am 2013; 95: 1942-1949.
- 21. Christells N, Wallace S, Sage CE, et al. An enhanced recovery after surgery program for hip and knee arthroplasty. Med J Aust 2015; 202: 363-369. <MJA full text>
- 22. Hofstede SN, Nouta KA, Jacobs W, et al. Mobile bearing vs fixed bearing prostheses for posterior cruciate retaining total knee arthroplasty for postoperative functional status in patients with osteoarthritis and rheumatoid arthritis. Cochrane Database Syst Rev 2015; (2): CD003130.
- 23. Verra WC, van den Boom LGH, Jacobs W, et al. Retention versus sacrifice of the posterior cruciate ligament in total knee arthroplasty for treating osteoarthritis. Cochrane Database Syst Rev 2013; (10): CD004803.





Abstract
Objective: To compare the effectiveness of rehabilitation after total knee arthroplasty (TKA) in models with or without an inpatient rehabilitation component.
Design, setting and participants: A propensity score-matched cohort of privately insured patients with osteoarthritis who underwent primary, unilateral TKA in one of 12 Australian hospitals between August 2013 and January 2015 were included. Those discharged to an inpatient facility because of poor progress or who experienced significant complications within 90 days of surgery were excluded.
Intervention: Discharge after surgery to an inpatient rehabilitation facility or home.
Main outcome measures: Patient-reported knee pain and function (Oxford Knee Score; at 90 and 365 days after surgery) and health rating (EuroQol “today” health scale; at 35, 90 and 365 days). Inpatient and community-based rehabilitation provider charges were also assessed.
Results: 258 patients (129 pairs) from a sample of 332 were matched according to their propensity scores for receiving inpatient rehabilitation; covariates used in the matching included age, sex, body mass index, and markers of health and impairment. The only significant difference in outcomes was that EuroQol health scores were better on Day 35 for patients not undergoing inpatient rehabilitation (median difference, 5; IQR, –10 to 19; P = 0.01). Median rehabilitation provider charges were significantly higher for those discharged to inpatient therapy (total costs: median difference, $9500; IQR, $7000–11 497; P < 0.001; community therapy costs: median difference, $749; IQR, $0–1980; P < 0.001).
Conclusions: Rehabilitation pathways incorporating inpatient rehabilitation did not achieve better joint-specific outcomes or health scores than alternatives not including inpatient rehabilitation. Given the substantial cost differences, better value alternatives should be considered for patients after uncomplicated TKA.