The answer depends on how much and which data one consults
Media coverage of the 2015 influenza season in Australia depicted a severe influenza season, focusing on the record number of laboratory-confirmed influenza cases notified to health authorities.1,2 We used sentinel surveillance data and a weekly online symptoms survey to compare the magnitude of the 2015 influenza season in Australia with recent seasons.
Data were provided by the Australian Sentinel Practices Research Network (ASPREN), the Victorian Sentinel Practice Influenza Network (VicSPIN) and the Sentinel Practitioners Network of Western Australia (SPNWA). Together, these networks conduct Australia-wide surveillance of influenza-like illness (ILI; defined as cough, fever and fatigue). Participating general practitioners submit weekly reports on the number of patients presenting with ILI and the total number of consultations. Influenza polymerase chain reaction (PCR) test results of nose and throat swabs from ILI patients collated by ASPREN (a 20% systematic sample) and VicSPIN (selected at the discretion of the GP) were also available. Data were also provided by Flutracking, a national, weekly online survey of volunteers that can estimate the proportion of participants with ILI (defined as cough and fever, and/or the absence from normal duties). Notifications data are publicly available (http://www9.health.gov.au/cda/source/cda-index.cfm).
As shown in the Box, peak ILI rates in ASPREN, VicSPIN and Flutracking data during 2015 were not notably higher than during the preceding 5 years, and were similar to those of 2012. However, the percentage of positive PCR test results was lower in 2015 than in 2012. The peak ILI rate for SPNWA in 2015 was similar to the low peak of 2013. In contrast, cases of laboratory-confirmed influenza notified to the National Notifiable Diseases Surveillance System (NNDSS) increased by an average of 67% annually between 2010 and 2014, with a record 93 303 cases notified to 31 October 2015.
This discrepancy suggests that the increase in notified cases of influenza may be attributable to increased testing, rather than to increased morbidity. Medicare has reimbursed the costs of PCR testing since 2005, and public funding enabled the purchase of new PCR testing equipment after the 2009 influenza H1N1 pandemic; both developments facilitated increased routine influenza testing.3 A similar increase in notified pertussis cases was observed during 2008–2011.4 These data highlight the need for reporting negative laboratory results to calculate the proportion of positive influenza laboratory tests, and account for the effects of changing testing practices.5
Sentinel syndrome and laboratory surveillance data suggest that the magnitude of the 2015 influenza season was slightly higher than but nevertheless comparable with that of other post-2009 pandemic years. Increased media coverage that sensationalised the 2015 season, on the basis of notification data alone, was misleading. Interpretation of a season’s magnitude should draw on the multiple systems available that include data about community ILI, general practices, and emergency departments and hospitals. Selective use of data to motivate vaccination and other health-protecting behaviours in the population can mislead our health care professionals and compromise the community’s confidence in public health messages.
Box – Weekly influenza-like illness consultations per 1000 consultations by sentinel general practice networks (ASPREN, SPNWA, VicSpin)*; proportion of Flutracking participants reporting fever and cough; and notified cases of laboratory-confirmed influenza in Australia (January 2010 – October 2015)
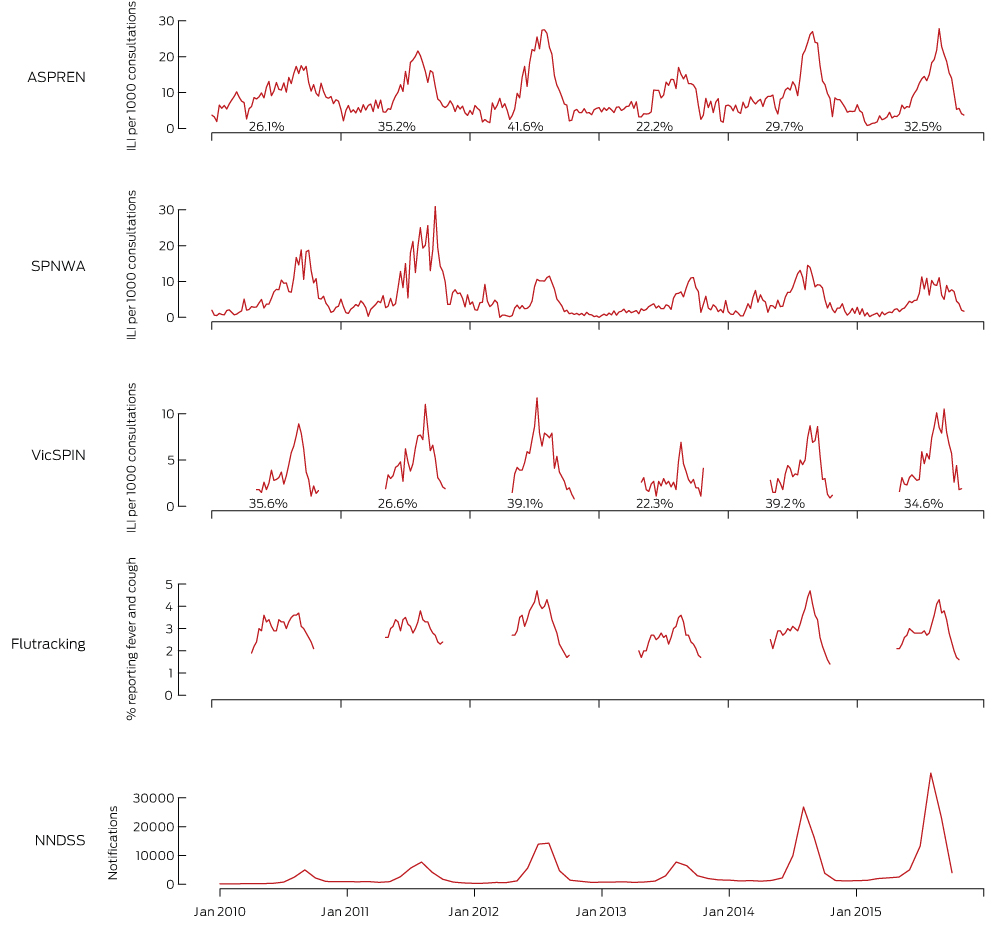
ASPREN = Australian Sentinel Practices Research Network; ILI = influenza-like illness; SPNWA = Sentinel Practitioners Network of Western Australia; VicSPIN = Victorian Sentinel Practice Influenza Network. * For ASPREN and VicSPIN: overall proportions of positive swabs collected during the influenza season (May–October).
Received 25 September 2015, accepted 18 November 2015
- 1. Scott S. Flu hits record number of Australian patients as doctors urge taking advantage of free vaccine. ABC News 2015; 8 Jul. http://www.abc.net.au/news/2015-07-08/flu-hits-record-number-of-australian-patients/6602706 (accessed Nov 2015).
- 2. Brennan R. Brisbane flu ‘not on the radar’ but try telling that to 13 000 victims. The Courier-Mail 2015; 2 Sep. http://www.couriermail.com.au/news/queensland/brisbane-flu-not-on-the-radar-but-try-telling-that-to-13000-victims/story-fnihsrf2-1227508437647 (accessed Nov 2015).
- 3. Australian Government Department of Health and Ageing. Review of Australia’s health sector response to pandemic (H1N1) 2009: lessons identified. Canberra: Commonwealth of Australia, 2011. http://www.health.gov.au/internet/publications/publishing.nsf/Content/review-2011-l/$File/lessons identified-oct11.pdf (accessed Nov 2015).
- 4. Kaczmarek MC, Valenti L, Kelly HA, et al. Sevenfold rise in likelihood of pertussis test requests in a stable set of Australian general practice encounters, 2000–2011. Med J Aust 2013; 198: 624-628. <MJA full text>
- 5. Lambert SB, Faux CE, Grant KA, et al. Influenza surveillance in Australia: we need to do more than count. Med J Aust 2010; 193: 43-45. <MJA full text>





We thank the general practitioners who contributed to ASPREN, VicSPIN and SPNWA during 2015. We also thank laboratory staff members from the following laboratories who undertook influenza testing and virus characterisation: SA Pathology, Adelaide, South Australia; PathWest Laboratory Medicine, Perth, Western Australia; the Victorian Infectious Diseases Reference Laboratory, Melbourne, Victoria; and the WHO Collaborating Centre for Reference and Research on Influenza, Melbourne, Victoria. Kristina Grant and Sandra Carlson collated the data for analysis. ASPREN and the WHO Collaborating Centre for Reference and Research on Influenza are funded by the Australian Government Department of Health. SPNWA and VicSPIN are funded by the Western Australian Department of Health and the Victorian Government Department of Health and Human Services respectively.
No relevant disclosures.