Although some improvements, arising out of the recommendations of the 1998 Ministerial Review of General Practice Training,1 have been made, there are still ongoing challenges that will test the sustainability of the current regionalised business model of general practice training.
The changing governance of general practice education and training from the 1970s to present is illustrated in Box 1, which summarises the key organisations involved, the changing focus of training and the decision-making model used by the key organisations involved. There has been an increase from two key organisations in the 1970s to six in 2011, with the training focus expanding from a national to a regionalised perspective and incorporating vertical integration of medical training.
From the 1970s through the 1990s, all decision-making responsibility rested with the federal government (ie, the previous incarnations of the Australian Government Department of Health and Ageing) and the Royal Australian College of General Practitioners (RACGP).2 They exercised direct decision-making powers over funding and training delivery, respectively — the federal government provided funding and the RACGP managed funds, delivered training and developed the curriculum. During this period, the federal government extended its role when it linked training with quality by making changes to sections 19AA and 19AB of the Health Insurance Act 1973 (Cwlth) and by establishing vocational registration.
A third player entered the general practice education and training environment in 1997 with the establishment of the Australian College of Rural and Remote Medicine (ACRRM). The ACRRM arose from a belief by some that rural and remote medicine was a broad but discrete form of general practice,3 and from a dissatisfaction with the way the RACGP related to its Rural Faculty members. The ACRRM adopted a similar governance and direct decision-making role to the RACGP, but without the legislative recognition as a training program that is required for granting independent vocational registration status as a general practitioner.3
The 1998 review of general practice training led to the introduction of a regionalised model of general practice education and training using regional training providers (RTPs). In 2001, the Commonwealth Department of Health and Aged Care established a Commonwealth-owned company, General Practice Education and Training (GPET), to establish the new training environment for general practice vocational training.4
In 2002, the newly established GPET and the RTPs significantly changed the business model of general practice vocational training. The regionalised model now included additional organisations in the governance of general practice education and training, and shifted decision-making responsibilities so that they involved direct, delegated and consultative processes (Box 2). For example, funds management, as a key decision-making responsibility, was delegated to GPET, which in turn delegated aspects of this role to the RTPs. This new model also shifted decision making related to education and training development and delivery — previously held predominantly by the RACGP — to the RTPs.
During the establishment phase of the new model, there was confusion and mistrust regarding the demarcation and devolution of governance and decision-making roles for both new and old organisations, but most notably the colleges, GPET and RTPs. The roles of the new organisations (GPET and RTPs) were evolving and the roles of the old organisations (RACGP and ACRRM) were in a state of flux. With the establishment of the AGPT program, the RACGP vocational training program that had been in place for nearly 30 years was deemed to be at risk, particularly by those who perceived they were losing governance and decision-making roles and responsibilities to new players.5 However, nearly 10 years on, each organisation’s role is becoming better defined and delineated. Box 2 provides a matrix of the current integrated distribution of governance and decision-making roles across the key organisations — from an RTP perspective.
The current regionalised model for general practice education and training has achieved a number of successes. These include regionalisation of training,6,7 general practice exposure during hospital training years,8 increased rural training,9 the formal inclusion of Aboriginal and Torres Strait Islander health training in education and training syllabi,10 and, most recently, the introduction of a streamlined training post/supervisor accreditation process.
The decision to regionalise the general practice vocational training program in 2002 resulted in the creation of 22 RTPs, which were charged with delivering general practice training throughout Australia. In 2011, the number of RTPs was reduced to 17 but still had the same coverage responsibility. Recent reviews indicated that the current training model provides optimal benefits to the Australian community and demonstrated that the current distribution of registrar training is a good match to the distribution of the population (in contrast to the distribution of GPs).6,7
Since 2005, there have been expanded opportunities for junior doctors to be exposed to general practice during their hospital years of general training, through the introduction of the Prevocational General Practice Placements Program (PGPPP). This has built on its much smaller but successful predecessor program, the ACRRM’s Rural and Remote Area Placement Program. As an example, in South Australia, the PGPPP annually allows over 110 interns and residents to undertake at least one of their junior rotations in general practice.11,12 The intern component equates to at least a third of the intern cohort in SA. A study conducted in 2007 confirmed that the inclusion of general practice as a junior doctor rotation was perceived positively by trainees and deemed to be of equal value to hospital-based rotations.8 Further, supervision and teaching in general practice rotations were deemed to be of superior quality.8 In 2010, the opportunities through PGPPP were expanding significantly across the nation, at equivalent and higher levels than those in SA.13
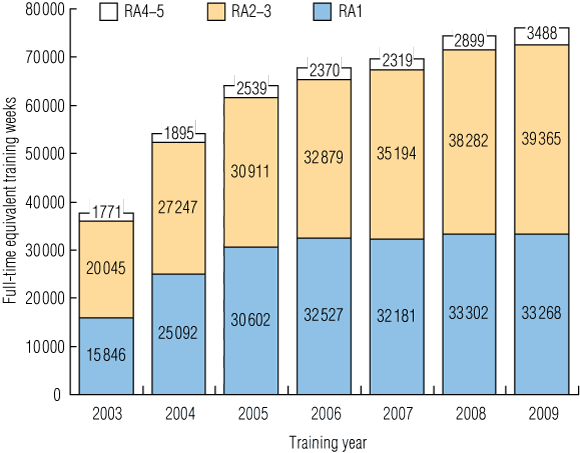
Available data indicate that the current training model has increased the number of registrars training in rural regions (Box 3).9 The rural pathway is now a distinct path that registrars can select from entry, regardless of their fellowship intent, and is available through most RTPs. In 2006, the ACRRM successfully gained recognition of its fellowship as a legislative end point for independent status as a specialist GP. At the same time, the RACGP strengthened its approach and support of rural-oriented registrars.
The formal inclusion of Aboriginal and Torres Strait Islander Health training in RTP education and training syllabi continues to be a work in progress, but some achievements have occurred as part of the new regionalised model. During this period, GPET developed a Framework for general practice training in Aboriginal and Torres Strait Islander health10 and, more recently, a draft guide to general practice training in Aboriginal and Torres Strait Islander health, which will act as a regional component to the framework. GPET also established the Aboriginal and Torres Strait Islander Health Training Advisory Group14 as a subcommittee to its Board, and, in 2008, created an ongoing professional support network for Aboriginal and Torres Strait Islander GP registrars. Additionally, the number of registrars undertaking training in accredited Aboriginal and Torres Strait Islander medical services has increased from 65 in 2003 to 141 in 2009.9
the outcomes of the primary care reforms, which may see changes in GPs’ roles and an emphasis on team care;
the role of generalism within medicine and how training supports this;
the competition for clinical training places for health students and the impact this will have on teaching practices and access to hospital training positions for GP registrars;
the issue of the cost of general practice vocational training and the link between funding with outcomes; and
the expansion of the type and level of training and primary health education that is expected to occur within general practice in the near future.
For example, as shown in Box 1, the future is likely to include more organisations across a broader range of health disciplines that will need to be part of the governance and decision-making framework. Necessarily, the model will need to expand its focus to include vertically and horizontally integrated education and training.
Regardless of the type and level of education and training required in general practice, decision-making responsibilities will continue across fund management, curriculum development, training standards development, education development and delivery, trainee examinations, RTP accreditation, training post/supervisor accreditation, workforce distribution and strategic training policy. Over the past decade, some lessons have been learned about how to more effectively allocate these responsibilities across all parties involved in education and training in general practice. In a more complex environment with more organisations involved, the most significant challenge remains to continuously improve this governance and decision-making framework so that it remains integrated, and strengthens the regionalised model of education and training in general practice.15
If we are able to demonstrate a collective level of maturity that allows for this genuine and respectful collaborative approach, then this model will not only be sustainable, but grow in status as a best-practice regionalised training provider model. It will allow for the development of interdisciplinary teaching, interprofessional education and most importantly collaborative practice that will benefit local patients in local communities. We are of the strong view that this outcome is worthy of pursuit — a sentiment that is being increasingly echoed by international colleagues.15
- Caroline O Laurence1,2
- Linda E Black2
- Mark Rowe3
- Rod Pearce4
- 1 Discipline of General Practice, University of Adelaide, Adelaide, SA.
- 2 Adelaide to Outback GP Training Program, Adelaide, SA.
- 3 Victorian Metropolitan Alliance General Practice Training, Melbourne, VIC.
- 4 Beulah Park Medical Practice, Adelaide, SA.
None identified.
- 1. General practice education: the way forward. Final report of the Ministerial Review of General Practice Training. Canberra: Commonwealth Department of Health and Family Services, Mar 1998.
- 2. Royal Australian College of General Practitioners. Australian general practice — a celebration. http://www.racgp.org.au/history/celebration (accessed Jun 2010).
- 3. Australian College of Rural and Remote Medicine. History. http://www.acrrm.org.au/history (accessed Jun 2010).
- 4. Commonwealth Department of Health and Aged Care. 2000–01 annual report for the Department of Health and Aged Care. Canberra: Department of Health and Aged Care, 2001.
- 5. Kidd MR. Is general practice vocational training at risk [editorial]? Med J Aust 2003; 179: 16-17. <MJA full text>
- 6. ACIL Tasman. Evaluation of regionalisation of general practice vocational training. Report prepared for Department of Health and Ageing. Canberra: ACIL Tasman, Oct 2005.
- 7. Access Economics. GPET’s funding model for RTPs: an update. Canberra: GPET, 2010.
- 8. Martin AA, Laurence CO, Black LE, Mugford BV. General practice placements for pre-registration junior doctors: adding value to intern education and training. Med J Aust 2007; 186: 346-349. <MJA full text>
- 9. Australian General Practice Training. Annual report to 30th June 2010. Canberra: GPET, 2010.
- 10. Australian General Practice Training. A framework for general practice training in Aboriginal and Torres Strait Islander health. Canberra: GPET, 2004. http://www.agpt.com.au/IndigenousHealthTraining/PublicationsandResources (accessed Apr 2011).
- 11. Sturt Fleurieu GP Education and Training. Prevocational General Practice Placement Program (PGPPP). http://www.sfgpet.com.au/GPTraining/PrevocationalTrainingPGPPP/tabid/176/Default.aspx (accessed Nov 2010).
- 12. Adelaide to Outback GP Training Program. Prevocational Placements (PGPPP). http://adelaidetooutback.com.au/TrainingOpportunities/Prevocational-Placements--PGPPP- (accessed May 2011).
- 13. Australian Government. Australian Government 2010–11 Health and Ageing Portfolio Budget statements: outcome 5. Primary care. http://www.health.gov.au/budget2010 (accessed Jun 2010).
- 14. General Practice Education and Training. Aboriginal and Torres Strait Islander Health Training Advisory Group. http://www.agpt.com.au/IndigenousHealthTraining/GeneralInformation3/#advisory (accessed May 2011).
- 15. Health Professions Network Nursing and Midwifery Human Resources for Health. Framework for Action on Interprofessional education and collaborative practice. Geneva: World Health Organization, 2010.





Abstract
The 1998 Ministerial Review of General Practice Training identified several areas for improvement that led to major changes in the provision of general practice training, including the establishment of General Practice Education and Training (GPET) and the regionalisation of training.
The regionalised training business model has been in place for nearly 10 years, and several key organisations have been involved in its evolution, including the Australian Government, speciality colleges, GPET and regionalised training providers.
Both the college-focused and regionalised-focused models have had some successes. These include recognition and support of general practice as a vocational specialty, increased numbers of junior doctors undertaking placements in general practice, and increased numbers of registrars training in rural areas.
This period has also seen changes in the governance and decision-making processes with creation of a new framework that is inclusive of all the key players in the new regionalised training system.
The future holds challenges for the regionalised training business model as the general practice education and training landscape becomes more complex. The framework in the current model will provide a base to help meet these challenges and allow for further sustainable expansion.