The 10–12-year gap in life expectancy between Indigenous and non-Indigenous Australians1 remains a cause of ongoing grief for Aboriginal and Torres Strait Islander peoples, and a source of shame for all Australians. This gap in life expectancy has prompted government action through the Council of Australian Governments’ (COAG) agreement to “Close the Gap”.2 Strategies proposed include addressing size and quality of the health workforce through providing
an adequate workforce to meet Aboriginal and Torres Strait Islander health needs by increasing the recruitment, retention, effectiveness [and] training of health practitioners working within Aboriginal and Torres Strait Islander health settings
and increasing the number of health professionals who are themselves Aboriginal or Torres Strait Islander.3
The first call for improved training of health professionals in Aboriginal and Torres Strait Islander health came from the National Aboriginal Health Strategy (NAHS) in 1989.4 This was echoed in subsequent reports.5,6 The organisations and processes involved in development of general practice curricula in Aboriginal and Torres Strait Islander health training are described in Box 1.
The colleges’ curricula9,11 were developed in partnership with the National Aboriginal Community Controlled Health Organisation (NACCHO). For the Royal Australian College of General Practitioners (RACGP), this partnership was enacted through a Joint Consultative Committee between the RACGP and NACCHO.
In 1997, the RACGP became the first Australian medical college to mandate training in Aboriginal health. By 2001, the RACGP curriculum was being implemented in every state and territory except Tasmania.12 In 2007, when the Australian College of Rural and Remote Medicine (ACRRM) was accredited by the Australian Medical Council, Aboriginal and Torres Strait Islander health training was also mandated for registrars training for the ACRRM Fellowship.
In 2001, responsibility for delivery of general practice vocational training moved from the RACGP to General Practice Education and Training (GPET), which contracts with regional training providers (RTPs) to deliver training. Cultural and medical educators delivering the RACGP Aboriginal health curriculum were concerned that gains made might be lost as new RTPs struggled to deliver an all-encompassing general practice curriculum. GPET responded by establishing an Aboriginal and Torres Strait Islander Health Training Reference Group to oversee development and implementation of a Framework for General Practice Training in Aboriginal and Torres Strait Islander Health.13 Following endorsement of the Framework by the GPET Board in 2003, RTPs were required to deliver training in accordance with the GPET Framework.
In parallel with the development of the GPET Framework, the Committee of Deans of Australian Medical Schools (now part of Medical Deans Australia and New Zealand) developed a framework requiring inclusion of Aboriginal and Torres Strait Islander health in medical curricula.14 Also at this time, the Australian Government Department of Health and Ageing formalised a previous agreement with the RACGP, allowing health services employing GP registrars in Aboriginal and Torres Strait Islander health training positions to obtain reimbursement of their salaries while also billing Medicare for registrar-incurred general practice items. This addressed NACCHO’s concerns about the financial viability of general practice training in ACCHSs.
Thus, RTPs were required and supported to deliver training in accordance with the GPET Framework, in conformity with the RACGP and ACRRM curricula.9,11 This training would build on learning required in Australian medical schools, and be developed and delivered in partnership with Aboriginal and Torres Strait Islander people and organisations. Critically, Aboriginal and Torres Strait Islander health training posts (84% of these in ACCHSs by 2005)15 were supported financially to provide training.
The GPET Framework was based on best evidence available at the time and informed by consultations with a wide range of stakeholders. Evaluations of the implementation of the GPET Framework in 200516 and 200815 reported an increase in Aboriginal and Torres Strait Islander training placements undertaken since the Framework was introduced, although variation was noted in RTP implementation of the Framework. The later evaluation noted that not only was the consultation informing its development of value, but the very existence of such a Framework was of benefit.15 Both reports recommended enhanced recruitment and support of Aboriginal and Torres Strait Islander educators and mentors and improved processes for tracking training and related outcomes.15,16 The Framework is currently being updated.17
appointment of a NACCHO representative to the Board of Directors and provision of cultural awareness training for the Board and executive;
increased staff allocation to Aboriginal and Torres Strait Islander health training including the establishment of a full-time Aboriginal- and/or Torres Strait Islander-identified position;
revision of terms of reference and representative structure of the (now) GPET Aboriginal and Torres Strait Islander Health Training Advisory Group;
continuation of the Aboriginal and Torres Strait Islander salary reimbursement program with trial of a regionalised model of re-imbursement; and
improvement of data collection systems to enable GPET to track progress in Aboriginal and Torres Strait Islander health training.
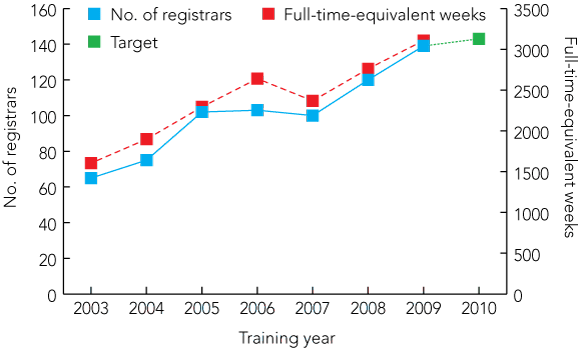
RTPs have worked with NACCHO affiliate-based training advisors to recruit and support new Aboriginal and Torres Strait Islander training posts. The number of registrars undertaking training in these posts continues to increase (Box 2). Funding through the COAG “Close the Gap” agreement will provide additional Aboriginal and Torres Strait Islander health training positions.
GP registrars have led two key recent initiatives. With Aboriginal and Torres Strait Islander health addressed in the core curriculum of both the RACGP and ACRRM, registrars demanded that assessment reflect this. Both colleges now regularly include assessment of Aboriginal and Torres Strait Islander health learning outcomes in their Fellowship examinations. More recently, GPET has supported Aboriginal and Torres Strait Islander registrars to meet regularly. In response to their recommendations, an Indigenous registrar liaison officer position is to be established.17
GPET, RTPs and the Aboriginal and Torres Strait Islander educators, organisations and communities with whom they work have achieved many targets of the original Framework. Others remain to be substantially addressed.15 It is timely to review the literature to determine what new evidence has emerged for approaches taken to date, and what new approaches may be relevant in the future.
A recent review of cultural competency training highlighted the need for:
organisational commitment, including development of a cultural competence training policy;
maintenance of partnerships to enable development, implementation and evaluation of training;
clear description of the purpose, goals and learning objectives for training;
needs assessment before training and ongoing evaluation; and
use of self-directed learning resources, workshops, field visits and cultural immersion, and mentoring and follow-up activities.19
Organisational approaches highlighted in the review are similar to those being implemented in accordance with the GPET Framework. The colleges’ curricula provide descriptions of the purpose, goals and learning objectives for training.9,11 The development of resources and learning approaches specific to general practice vocational training has been addressed to varying extents across RTPs. National resource development, such as a learning guide that is adaptable to different local contexts, would help RTPs deliver the colleges’ curricula.
Content areas for such a guide could include those identified for orientation of GP registrars working in remote Aboriginal communities,20 such as communication skills and cultural safety training, population health, personal and professional role delineation and self-care, and consideration of organisational issues.
The need for recognition and support of the role played by Aboriginal health workers in mentoring non-Indigenous health workers has been highlighted by those engaged in general practice training.21 A study identified barriers and facilitators for Aboriginal and Torres Strait Islander community members in taking on roles as educators and mentors.22 Community members reported being motivated by a desire to “break down the barriers between Indigenous and non-Indigenous people” and to provide a role model for young people.22 Teaching was noted to be difficult in the context of a lack of training, personal illness, family and community responsibilities, and the confronting nature of the subject matter. Learner ignorance and lack of interest were also noted as barriers. Community members were reported to prefer small group informal teaching approaches. Provision of teaching resources and training, as well as recognition and remuneration for teaching, were recommended.22
Evaluations of general practice vocational training indicate that Aboriginal and Torres Strait Islander health training posts provide this learning environment.15,16 However, with training numbers expected to increase, these services, like other general practice training posts, will need to expand their capacity. This will require development and resourcing of innovative teaching approaches such as vertical integration of training, if the increased numbers are not to be achieved at the cost of compromising quality of that training.23,24
In rural and remote areas, international medical graduates, who often provide medical services in Aboriginal and Torres Strait Islander communities with minimal orientation or training, could also benefit from these teaching approaches.25
Both the NAHS4 and the Close the Gap targets3 highlight the importance of training Aboriginal and Torres Strait Islander health professionals and this is also recognised in the GPET Framework.13 Ongoing close partnership with the Australian Indigenous Doctors’ Association (AIDA) in engaging with Aboriginal and Torres Strait Islander medical students and providing support throughout their training will be critical in recruiting these doctors to general practice. Both colleges will similarly need to work with AIDA to support their retention in the workforce.
- Mary E Martin1
- Jennifer S Reath2
- 1 Queensland Aboriginal and Islander Health Council, Brisbane, QLD.
- 2 Department of General Practice, University of Western Sydney, Sydney, NSW.
Queensland Aboriginal and Islander Health Council receives funding from GPET for Mary Martin’s employment. Jennifer Reath worked as a consultant to GPET from 2002 to 2008.
- 1. Australian Bureau of Statistics. Experimental estimates and projections, Aboriginal and Torres Strait Islander Australians, 1991 to 2021. Canberra: ABS, 2009. (ABS Cat. No. 3238.0.)
- 2. Council of Australian Governments. National partnership agreement on closing the gap in Indigenous health outcomes. http://www.coag.gov.au/intergov_agreements/federal_financial_relations/docs/national_partnership/NP_closing_the_Gap_indigenous_health_outcomes.pdf (accessed Apr 2010).
- 3. Australian Human Rights Commission. Close the gap — part 2 outcomes from the National Indigenous Health Equality Summit. http://www.hreoc.gov.au/social_justice/health/targets/closethegap/part2_3.html (accessed May 2010).
- 4. National Aboriginal Health Strategy Working Party. A National Aboriginal Health Strategy. Canberra: NAHSWP, 1989.
- 5. House of Representatives Standing Committee on Family and Community Affairs. Health is life: report on the inquiry into Indigenous health. Canberra: the Committee, 2000.
- 6. Royal Commission into Aboriginal Deaths in Custody. National report: overview and recommendations by Commissioner Elliott Johnston QC. Canberra: AGPS, 1991.
- 7. Collins L, Beaton N. Aboriginal and Torres Strait Islander Health Curriculum Design Project: Steering Committee summary. In: 3rd National Rural Health Conference Proceedings; 1995 Feb 3-5; Mt Beauty, Vic. Canberra: National Rural Health Alliance, 1995: 345-350.
- 8. Royal Australian College of General Practitioners Faculty of Rural Medicine and the National Aboriginal Community Controlled Health Organisation. Final Position Paper of the Aboriginal and Torres Strait Islander Health Curriculum Design Project. Melbourne: RACGP, 1994.
- 9. Royal Australian College of General Practitioners. Draft RACGP Curriculum Project. Aboriginal and Torres Strait Islander health. http://www.racgp.org.au/scriptcontent/curriculum/pdfdraft/DRAFT_Aboriginal_and_Torres_Strait_Islander_health_curriculum_statement.pdf (accessed May 2010).
- 10. Prideaux D, Smith J. Aboriginal health training module. Melbourne: Royal Australian College of General Practitioners Training Program, 1998.
- 11. Doolan T, editor. Primary curriculum. 3rd ed. Brisbane: Australian College of Rural and Remote Medicine, 2009.
- 12. Royal Australian College of General Practitioners Quality Improvement Unit. Aboriginal health: an evaluation of the implementation of the curriculum. Melbourne: RACGP, 2001.
- 13. General Practice Education and Training Aboriginal and Torres Strait Islander Health Training Reference Group. A Framework for General Practice Training in Aboriginal and Torres Strait Islander Health. Canberra: GPET, 2003.
- 14. Philips G. CDAMS Indigenous Health Curriculum Framework. Melbourne: Committee of Deans of Australian Medical Schools, 2004.
- 15. Urbis. Evaluation of GPET’s Aboriginal and Torres Strait Islander Health Training Framework. Sydney: Urbis, 2008. http://www.agpt.com.au/view/document.shtml?y74348-bifoiwk.pdf (accessed Feb 2010).
- 16. Reath J, Doolan G. Progress in Aboriginal and Torres Strait Islander health training — an evaluation of the implementation of the GPET framework. Aust Fam Physician 2005; 34 Suppl 1: 23-26.
- 17. Hunter J, editor. December 2010 [newsletter issue]. Ngaaminya: the GPET Aboriginal and Torres Strait Islander Health Training Newsletter. Canberra: Australian General Practice Training, Dec 2010. http://ngaaminyanewsletter.cmail1.com/t/ViewEmail/r/9DC6C3141FEEBBC2 (accessed Feb 2010).
- 18. General Practice Education and Training. Indigenous health training report 2003–2009. Canberra: GPET, 2010.
- 19. Farrelly T, Lumby B. A best practice approach to cultural competence training. Aborig Isl Health Work J 2009; 13 (5): 14-22.
- 20. Morgan S. Orientation for general practice in remote Aboriginal communities: a program for registrars in the Northern Territory. Aust J Rural Health 2006; 14: 202-208.
- 21. Abbott P, Gordon E, Davison J. Expanding roles of Aboriginal health workers in the primary care setting: seeking recognition. Contemp Nurse 2008; 27: 157-164.
- 22. Nguyen HT, Gardiner A. Indigenous community members as teachers of Indigenous health. Aust Fam Physician 2008; 37: 1019-1021.
- 23. Van Der Weyden MB. Expanding primary care based medical education: a renaissance of general practice [editorial]? Med J Aust 2007; 187: 66-67. <MJA full text>
- 24. Dick MLB, King DB, Mitchell GK, et al. Vertical Integration in Teaching And Learning (VITAL): an approach to medical education in general practice. Med J Aust 2007; 187: 133-135. <MJA full text>
- 25. Gilles MT, Wakerman J, Durey A. “If it wasn’t for OTDs, there would be no AMS”: overseas-trained doctors working in rural and remote Aboriginal health settings. Aust Health Rev 2008; 32: 655-663.





Abstract
This article reviews the history of general practice vocational training in Aboriginal and Torres Strait Islander health, identifies current initiatives and recommends future approaches based on recent evidence.
General practice vocational training in Aboriginal and Torres Strait Islander health requires ongoing support and investment from governments and training and general practice organisations if the gains made to date are to be consolidated and health outcomes are to improve.
In particular, investment in sustained and respectful partnerships with Aboriginal and Torres Strait Islander peoples and organisations will continue to provide the groundwork for effective training of general practitioners in this critical health area, and will also play an important role in capacity-building in Aboriginal and Torres Strait Islander communities.