Syphilis is a sexually transmissible infection (STI) caused by Treponema pallidum. It is treatable with standard antibiotics,1 but in the absence of therapy, gives rise to sequential clinical stages. In the initial stages, the infection is highly transmissible and often presents as ulcerative genital lesions or a rash. Infectiousness diminishes through a long latency period, which may be followed by serious complications including cardiovascular and neurological disease.1 Syphilis can be passed on during pregnancy to the developing fetus and frequently causes miscarriage, stillbirth, neonatal death or serious consequences such as deafness, blindness and mental retardation.2
Syphilis is a legally notifiable infection in all states and territories. Since 2004, new diagnoses that are determined on the basis of laboratory and clinical information to be in the early, infectious stage (less than 2 years’ duration)3 have been reported by all Australian states and territories to the National Notifiable Diseases Surveillance System, with information on patient demographics.4
Historically, the reported rates of infectious syphilis have been much higher among Aboriginal and Torres Strait Islander (Indigenous) people than in non-Indigenous Australians. Indigenous Australians residing in remote communities are particularly affected.4 There have been sustained efforts to control syphilis in this population using clinical strategies based on population screening, in combination with preventive strategies. These measures have had some success;5-7 however, there remains considerable disparity between Indigenous and non-Indigenous Australians.
We first conducted a descriptive analysis of infectious syphilis cases notified in 2009 by Indigenous status, jurisdiction, sex, age group and area of residence (based on Australian Standard Geographical Classification Accessibility/Remoteness Index of Australia Plus scores).8
We calculated crude and age-standardised infectious syphilis notification rates per 100 000 population based on the Australian Bureau of Statistics census.9 Age-standardised population rates by Indigenous status, jurisdiction and sex in 2009 were calculated using the direct method, taking the 2006 population as the standard.9
The summary rate ratio for Indigenous v non-Indigenous people was 7.91 (P < 0.001) (Box 1).
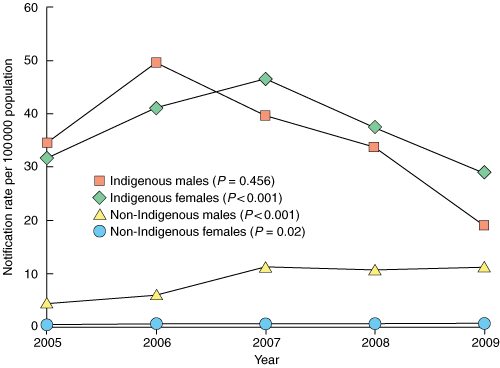
Among Indigenous females, there was a downward trend in notification rates per 100 000 population, dropping from 35 in 2005 to 19 in 2009 (P < 0.001). There was no significant trend for Indigenous males (P = 0.456) (Box 2).
In the non-Indigenous population, there was a significant increasing trend in the crude infectious syphilis notification rate in both sexes. The rate increased from 4.5 in 2005 to 11.1 in 2009 for males (P < 0.001); and from 0.40 in 2005 to 0.64 in 2009 for females (P = 0.02) (Box 2).
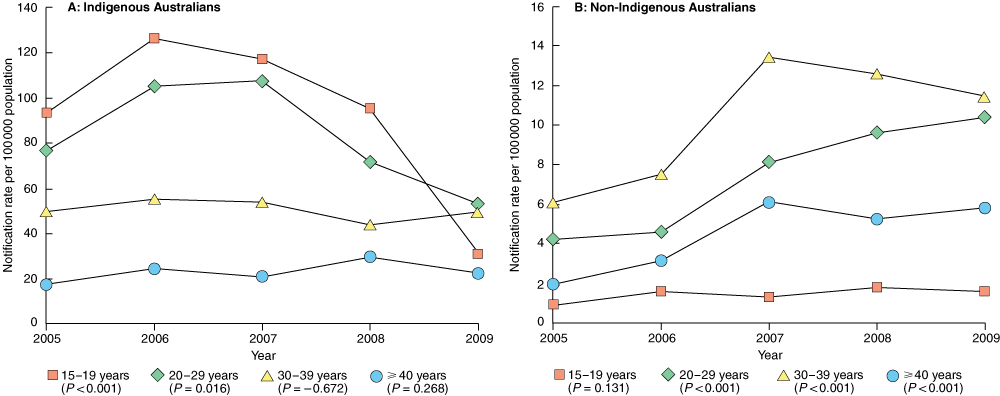
In the Indigenous population, the highest crude infectious syphilis notification rates occurred in people aged 15–19 years and 20–29 years in all years except 2009. A significant downward trend was observed in both age groups (Box 3).
In the non-Indigenous population, the crude infectious syphilis notification rate increased significantly for all age groups (P < 0.001) except 15–19 year olds (Box 3).
The summary rate ratio for Indigenous v non-Indigenous people was highest in 15–19 year olds (64.65) (Box 1).
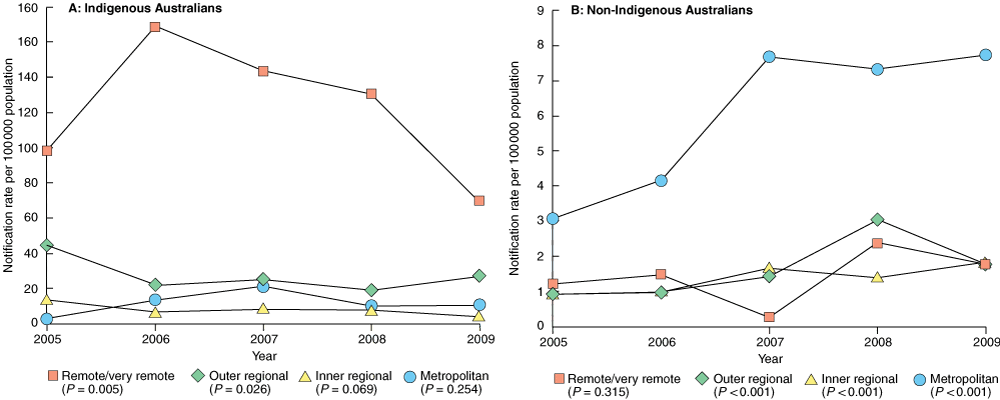
The highest notification rate in the Indigenous population occurred in remote/very remote areas, where a significant downward trend was observed between 2005 and 2009 (from 99 down to 70; P = 0.005) (Box 4).
In contrast, for the non-Indigenous population, the highest rate was observed in metropolitan areas, with a significant upward trend between 2005 and 2009 (from 3.1 to 7.7; P < 0.001) (Box 4). The Indigenous v non-Indigenous summary rate ratio was highest in remote/very remote areas (86.33) (Box 1).
In 2009, most notifications (84%) among Indigenous people came from Northern Territory, Western Australia and Queensland, whereas 90% of notifications among non-Indigenous people came from New South Wales, Queensland and Victoria. Trends over the study period in the Indigenous population varied across jurisdiction, with a statistically significant downward trend in the NT and Queensland (P < 0.001), and a significant upward trend in WA (P < 0.001). There was no significant trend in other jurisdictions (Box 1).
For the non-Indigenous population, there was a significant upward trend in the infectious syphilis notification rate in all five of the largest jurisdictions (P < 0.001). The Indigenous v non-Indigenous summary rate ratio was highest in WA (23.89), followed by Queensland (6.71) (Box 1).
Australia has two distinct patterns of infectious syphilis.
In the non-Indigenous population, the notification rate is highest in males aged 20 years and older (particularly those who live in metropolitan centres) and has increased significantly over the past 5 years.
Among Indigenous people, the notification rate is highest in young people aged 15–29 years (particularly those who live in remote and very remote locations) and has decreased significantly over the past 5 years.
The increasing rates in the non-Indigenous population occur mostly (but not exclusively) in males and are predominantly reported among men who have sex with men (MSM).10-14 Due to the absence of a reliable denominator, it is not possible to calculate the population rates for this population. However, given that 90% of male non-Indigenous cases occur among MSM, and that MSM are estimated to make up about 2% of the total male population,15 the crude rate among MSM would match the highest rates seen in young Indigenous people in remote settings.
The downward trend in infectious syphilis rates seen in Indigenous people commenced in 2006. Only in WA was there an upward trend. This could be due to a change of reporting procedures in June 2006, whereby notifications of syphilis cases from laboratories became mandatory rather than voluntary, or to a well defined outbreak of syphilis infection identified in a remote region of WA in 2008.16
By 2009, notification rates in Indigenous people aged 15–19 years were at a level below all other age groups, excluding the ≥ 40 years group. This may be a consequence of people aged over 40 years missing out on the benefit of annual screening rounds, which generally target people aged 15–35 years.17
The significant decrease in notifications of infectious syphilis seen in Indigenous people between 2005 and 2009 might be attributable to a decline in testing and case finding. However, available testing data suggest the opposite. For example, in far north Queensland, the number of syphilis tests increased from 4054 tests in 2004 to 6199 in 2005,18 and the implementation of a Young Persons Check in remote communities since early 2009 has increased levels of syphilis testing in target age groups. In central Australia and cross-border regions of WA, NT and South Australia, high rates of testing achieved through annual community STI screening programs have been sustained during the study period.6,17 Nationally, antenatal screening is seen as an important contributor to reductions in infectious syphilis notifications, with fewer than 10 cases of congenital syphilis diagnosed annually since 2007.19
An alternative explanation for the observed decreasing trend in infectious syphilis notification rates in the Indigenous population is a real decrease in incidence achieved through population screening and case management. Centrally based state-wide syphilis registers, staffed by specialists and specifically trained nurse consultants, have improved case management by providing testing, treatment and management advice to clinicians for infectious and congenital syphilis.17
Other factors possibly contributing to the observed decrease in infectious syphilis include incidental treatment of early syphilis due to increasing use of antibiotics, such as azithromycin, for treatment of other common infections, including bacterial STIs. While single doses of oral azithromycin or amoxicillin plus probenecid are not recommended as treatment for syphilis, both are recommended as second-line treatments for syphilis in people with penicillin allergies.20,21 The reduction in the absolute numbers of infectious syphilis cases from 233 in 2006 to 123 in 2009, combined with the relative geographical concentration of cases in remote communities, provides the opportunity to consider whether a renewed and strengthened emphasis on intervention may actually eliminate infectious syphilis from this population.
In Australia, a recently endorsed national strategy22 recognises this potential. At the community level, the goal of elimination has already been shown to be feasible. For example, the STI program in the Anangu Pitjantjatjara Yankunytjatjara Lands of SA, coordinated by Nganampa Health Council, has achieved a significant reduction in infectious syphilis prevalence over the past 11 years using the Eight Way Model.6,23 This model incorporates clinical activities, such as screening and opportunistic testing and treatment, combined with project planning and management, staff training, community-based education and health promotion, health hardware (including condom provision), research, surveillance, and monitoring and evaluation.
A factor that gives cause for optimism in contemplating the elimination of infectious syphilis from remote communities is that those communities appear to have sexual networks that are relatively separate from non-Indigenous populations. Notably, antibiotic resistance in Neisseria gonorrhoeae is only just emerging in remote communities, even though it has been widespread in non-Indigenous people for over 25 years.24 However, it is recognised that cases associated with male-to-male sex do occur among men who also have sex with women, highlighting the potential for onward transmission in Indigenous communities.
The central Australian donovanosis project of 1997 and the National Donovanosis Eradication Project implemented in 2000 further support the notion that elimination of syphilis is achievable within Indigenous remote communities. The Donovanosis Eradication Project employed four project officers in northern Australia who provided health services with support, including education and centralised coordination to assist case-finding and management.25 This led to significant decreases in donovanosis diagnoses, from 121 cases in 1994 to 32 cases in 2001; in 2009, only one case was identified in Australia.3,25,26 However, T. pallidum is an extremely infectious organism that can be transmitted without symptoms; it may therefore be more difficult to eliminate than donovanosis.1
- James S Ward1
- Rebecca J Guy1
- Snehal P Akre1
- Melanie G Middleton1
- Carolien M Giele2
- Jiunn Y Su3
- Craig A Davis4
- Handan Wand1
- Janet B Knox1
- Patricia S Fagan5
- Basil Donovan1
- John M Kaldor1
- Darren B Russell6,7
- 1 Kirby Institute (formerly National Centre in HIV Epidemiology and Clinical Research), University of New South Wales, Sydney, NSW.
- 2 Communicable Disease Control Directorate, Public Health Division, WA Department of Health, Perth, WA.
- 3 Centre for Disease Control, Department of Health and Families, Darwin, NT.
- 4 Health Protection Directorate, Division of the Chief Health Officer, Queensland Health, Brisbane, QLD.
- 5 Tropical Regional Services, Queensland Health, Cairns, QLD.
- 6 James Cook University, Townsville, QLD.
- 7 Cairns Sexual Health Centre, Queensland Health, Cairns, QLD.
None identified.
- 1. Donovan B, Dayan L. Syphilis. In: Warrell DA, Cox TM, Firth JD, editors. Oxford textbook of medicine. Oxford: Oxford University Press, 2010: 885-896.
- 2. Schmid GP, Stoner BP, Hawkes S, et al. The need and plan for global elimination of congenital syphilis. Sex Transm Dis 2007; 34: S5-S10.
- 3. Australian Government Department of Health and Ageing. Australian national notifiable diseases case definitions. Syphilis — infectious (primary, secondary and early latent), less than 2 years duration case definition. http://www.health.gov.au/internet/main/publishing.nsf/Content/cda-surveil-nndss-casedefs-cd_syphl2.htm (accessed Oct 2010).
- 4. National Centre in HIV Epidemiology and Clinical Research. Bloodborne viral and sexually transmitted infections in Aboriginal and Torres Strait Islander people. Surveillance and evaluation report 2009. Sydney: University of New South Wales, 2009.
- 5. Miller PJ, Torzillo P, Tizard J, et al. Interventions to reduce the interval to treatment in syphilis: central case management and encrypted email. Venereology 1998; 11: 26-29.
- 6. Mak D, Johnson G, Plant A. A syphilis outbreak in remote Australia: epidemiology and strategies for control. Epidemiol Infect 2004; 132: 805-812.
- 7. Huang R-L, Torzillo PJ, Hammond VA, et al. Epidemiology of sexually transmitted infections on the Anangu Pitjantjatjara Yankunytjatjara Lands: results of a comprehensive control program. Med J Aust 2008; 189: 442-445. <MJA full text>
- 8. McGrail MR, Humphreys JS. Geographical classifications to guide rural health policy in Australia. Aust N Z Health Policy 2009; 6: 28.
- 9. Australian Bureau of Statistics. Experimental estimates and projections, Aboriginal and Torres Strait Islander Australians, 1991 to 2021. Canberra: ABS, 2009. (ABS Cat. No. 3238.0.)
- 10. Jin F, Prestage GP, Zablotska I, et al. High incidence of syphilis in HIV-positive homosexual men: data from two community-based cohort studies. Sex Health 2009; 6: 281-284.
- 11. National Centre in HIV Epidemiology and Clinical Research. HIV, viral hepatitis and sexually transmissible infections in Australia. Annual surveillance report 2010. Sydney: University of New South Wales, 2010.
- 12. Allen K, Guy R, Leslie D, et al. The rise of infectious syphilis in Victoria and the impact of enhanced clinical testing. Aust N Z J Public Health 2008; 32: 39-42.
- 13. Guy RJ, Leslie DE, Simpson K, et al. Sustained increase in infectious syphilis notifications in Victoria. Med J Aust 2005; 183: 218. <MJA full text>
- 14. Jin F, Prestage GP, Kippax SC, et al. Epidemic syphilis among homosexually active men in Sydney. Med J Aust 2005; 183: 179-183. <MJA full text>
- 15. Prestage GP, Ferris J, Grierson J, et al. Homosexual men in Australia: population, distribution and HIV prevalence. Sex Health 2008; 5: 97-102.
- 16. Government of Western Australia Department of Health. Disease Watch: the Western Australian Communicable Diseases Bulletin 2010; 14(2). http://www.public.health.wa.gov.au/cproot/3156/2/DW_14_no_2_Jun_2010_web.pdf (accessed Apr 2011).
- 17. Smith K, Fethers K, Tangey A, et al. Sexually transmitted infections (STIs) in Central Australia — time for concerted action. Proceedings of the Australasian Sexual Health Conference; 2006 Oct 9-11; Melbourne, Australia.
- 18. Fagan PS, Cannon FM. Syphilis in remote north Queensland. Commun Dis Intell 2007; 31: 125-127.
- 19. NNDSS Annual Report Writing Group. Australia’s notifiable status, 2007. Annual report of the National Notifiable Diseases Surveillance System. Commun Dis Intell 2009; 33: 89-154.
- 20. Workowski KA, Berman S; Centers for Disease Control and Prevention. Sexually transmitted diseases treatment guidelines, 2010. MMWR Recomm Rep 2010; 59 (RR-12): 1-110.
- 21. Klausner JD, Kohn RP, Kent CK. Azithromycin versus penicillin for early syphilis. N Engl J Med 2006; 354: 204.
- 22. Australian Government Department of Health and Ageing. Third National Aboriginal and Torres Strait Islander Blood Borne Viruses and Sexually Transmissible Infections Strategy 2010–2013. Canberra: Commonwealth of Australia, 2010. http://www.health.gov.au/internet/main/publishing.nsf/Content/ohp-national-strategies-2010-atsi-bbv/$File/atsi.pdf (accessed Apr 2010).
- 23. Sexual Health and Blood-borne Virus Program. Western Australian Aboriginal Sexual Health Strategy 2005–2008. Perth: WA Department of Health, 2005.
- 24. Australian Gonococcal Surveillance Programme. Annual report 2009. Commun Dis Intell 2010; 34: 89-95.
- 25. Australian Government Department of Health and Ageing. National Notifiable Diseases Surveillance System. Number of notifications of donovanosis, Australia, 1991 to present. http://www9.health.gov.au/cda/Source/CDA-index.cfm (accessed Oct 2010).
- 26. Bowden F, on behalf of the National Donovanosis Eradication Advisory Committee. Donovanosis in Australia: going, going... Sex Transm Infect 2004; 81: 365-366.





Abstract
Objective: To describe the epidemiology of infectious syphilis among Aboriginal and Torres Strait Islander (Indigenous) people in Australia.
Design and setting: We assessed trends in national infectious syphilis notification rates from 2005 to 2009 using Poisson regression, with a focus on geographic and demographic differences by Indigenous status. We compared Indigenous and non-Indigenous rate ratios over the study period and summarised the annual changes (summary rate ratio).
Main outcome measures: Crude notification rates and summary rate ratios by Indigenous status, jurisdiction, sex, age group and area of residence.
Results: From 2005 to 2009, in the Indigenous population, there was a substantial decline in the notification rate for infectious syphilis nationally; as well as in the following subgroups: females, 15–29 year olds, and people living in outer regional and remote areas in the Northern Territory and Queensland. In contrast, there was a significant (P < 0.001) upward trend in the notification rate in the non-Indigenous population nationally; as well as in males, in people aged 20 years and over, and in residents of metropolitan and regional areas, New South Wales, Queensland, South Australia, Victoria and Western Australia. The highest summary rate ratios were seen in remote/very remote areas (86.33; 95% CI, 57.45–129.74), in 15–19 year olds (64.65; 95% CI, 51.12–81.78), in females (24.59; 95% CI, 19.73–30.65), and in Western Australia (23.89; 95% CI, 19.82–28.82).
Conclusion: These data demonstrate that Australia has two distinct patterns of infectious syphilis: a substantially declining occurrence in Indigenous remote communities and an increasing incidence in males residing in urban and regional areas. Given the decline in notification rates in Indigenous remote communities, now might be the right time to move toward eliminating infectious syphilis from Indigenous communities.