Compared with adult mothers, teenage mothers are more likely to originate from economically disadvantaged families1 and live in areas of socioeconomic disadvantage.2 Rapid-repeat pregnancy (RRP), defined as pregnancy within 2 years of a first teenage birth,3 compounds this social inequality, as participation in education and work or training is repeatedly delayed and less likely to ever be attained.4
Teenage mothers who experience RRP are more likely than those who do not to have had an intended first pregnancy,3 have more positive attitudes to childbearing5 and engage in drug or alcohol use.5,6 They are also more likely to be older (18–19 years old)7 and have a partner who wants a pregnancy.3,7,8 The rate of RRP has been found to be between 35% and 42%.7,8
Despite most teenage mothers having access to contraception postpartum,9,10 contraceptive use is inconsistent.10 Those who live with their partners resume sex earlier than their peers and are less likely to use contraception when they do.10 Positive attitudes towards contraception5 and the use of long-acting contraceptives8,11 have been found to reduce RRP.
The aim of this study was to prospectively evaluate the predictors of a return to sexual intercourse and the incidence of RRP in a population of teenage mothers followed at 3-monthly intervals for 2 years. We hypothesised that pregnancy intentions and the use of a long-acting contraceptive would be independently associated with RRP.
Questionnaires were completed at recruitment (either before the birth or within 6 days after the birth), 6 weeks postpartum and then at 3-monthly intervals (alternating between a self-administered questionnaire completed during a home visit and a phone-call questionnaire) for a 2-year follow-up period. Participants were lost to follow-up if they could not be contacted between visits up to the next scheduled visit. Pregnancy was defined as a positive pregnancy test, termination, spontaneous miscarriage or live birth and was assessed at each follow-up after the birth.
Psychometric measures of health and social and emotional functioning previously found to be valid and reliable in teenage populations were used.12 Pregnancy planning, self-esteem, self-efficacy, mental health and family function were assessed using the London Measure of Unplanned Pregnancy,13 the Rosenberg Self-Esteem Scale,14 the Perceived Self-Efficacy Scale,15 the Depression Anxiety Stress Scales,16 and the McMaster Family Assessment Device.17 Social disadvantage was assessed using the Australian Bureau of Statistics Index of Relative Socioeconomic Disadvantage, with the lowest quintile representing the most disadvantaged group.18
At recruitment and each follow-up after the birth, teenagers’ living arrangements, social supports, relationship with the birth father and whether sexual intercourse had occurred were documented. Participants were also asked which contraceptive methods they had used, being grouped according to the contraceptives they had used most: long-acting contraceptives (etonogestrel implant or depot medroxyprogesterone acetate not requiring daily administration; oral contraceptives requiring daily administration; and barrier methods (which are coital dependent) or no contraception. Those using two forms of contraception were classified according to the most effective form (ie, the long-acting contraceptive where both it and condoms were used).
Participants were asked if they were attending school and, if not attending, when they had dropped out. Those who were one school year or more behind in relation to their age were classified as having an age-inappropriate education. Participants were also asked if they had used alcohol, cigarettes or marijuana, and if they were employed.
It was estimated that a sample size of 160 teenagers was sufficient to attain 80% power to detect odds ratios (ORs) of 3.0 in a two-group comparison of exposure prevalence between those with and without the outcome, assuming an outcome prevalence of 33% and an exposure prevalence of 25% for those without the outcome.19 This estimation allowed for 10% loss to follow-up.19
Medians, interquartile ranges and ranges were used to summarise continuous data, and frequency distributions were used to summarise categorical data. χ2 and Fisher exact tests were used to assess univariate associations of the categorical explanatory variables with the outcome of RRP. Univariate logistic regression analysis was used to identify significant candidate predictors associated with sexual intercourse or RRP. Multivariable logistic regression was used to identify factors simultaneously associated with sexual intercourse and RRP until 24 months postpartum, with the covariate effects summarised using ORs and 95% confidence intervals. Sexual intercourse and RRP were both considered at 3-monthly follow-up periods, and logistic regression modelling was implemented using generalised estimating equations, with the individual teenagers modelled as random effects. SPSS statistical software, version 15 (SPSS Inc, Chicago, Ill, USA) was used for data analysis.
Of the 560 teenagers who gave birth to their first baby during the study period at KEMH, 289 (52%) were invited to participate; of these, 189 (65%) agreed to participate. Eight were ineligible because they did not complete the recruitment questionnaire; 27 declined postpartum follow-up; and a further seven were withdrawn for reasons including stillbirth, removal of their child by child protection services, and loss of contact. Of the remaining 147 (78%) who were followed up, 109 (74%) continued with the study until 24 months postpartum. Within 2 years of their first birth, 49 (33%; 95% CI, 26%–41%) became pregnant, two of these before 6 weeks postpartum.
The majority of teenagers (65%) had age-inappropriate education. However, almost a third (27%) returned to school for at least 3 months in the first 12 months postpartum. Teenagers who had an RRP were more likely to be unemployed at 12 months than those who did not (96% v 82%, P = 0.029) (Box 1).
Teenagers who had an RRP were less likely to have low self-esteem than those who did not (35% v 59%; P = 0.002) (Box 1).
At recruitment, most participants (66%) were in a relationship with the birth father, and 44% lived with the birth father. Teenagers who had an RRP were more likely to be living with the birth father at 12 months than those who did not (50% v 31%; P = 0.033) (Box 1).
Participants reported frequent drug and alcohol use before their first pregnancy: 69% used alcohol, 44% used marijuana, and 62% smoked tobacco. During their first pregnancy, 45% continued to smoke tobacco. Rates of smoking tobacco and alcohol use were similar among those who had an RRP and those who did not, and increased with time postpartum (Box 1).
Most participants (76%) had not intended to conceive their first child, and 48% were not using contraception when they conceived. Teenagers who did not have an RRP were more likely to have continued using the same contraceptive method (no switches) than those who did (57% v 14%; P < 0.001) (Box 1).
The proportion of teenagers intending to become pregnant fluctuated postpartum. Teenagers who had an RRP were more likely to intend to become pregnant than those who did not at 9 months (38% v 18%; P = 0.025), 12 months (42% v 9%; P < 0.001), 15 months (47% v 23%; P = 0.017), and 21 months (46% v 22%; P = 0.019) (data not shown).
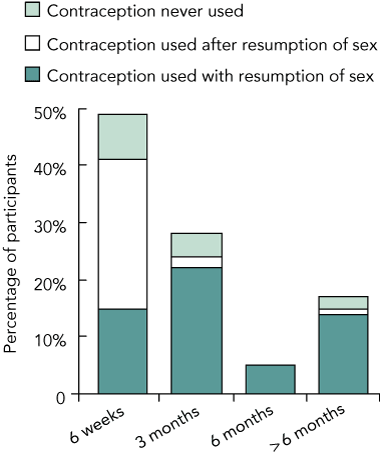
Within 24 months postpartum, 138 participants (94% of the initial 147 participants) had resumed sex. Of these, 41 (30%) did so without using contraception. Most (106; 77%) had resumed sex by 3 months postpartum, with 55 of these participants (52%) initially having no contraceptive cover (Box 2).
Simultaneous analysis of the factors associated with sexual intercourse (Box 3) highlighted that teenagers using an oral contraceptive were more likely to be sexually active than other teenagers (OR, 2.83; 95% CI, 1.38–5.82; P = 0.005).
Relative to participants at 12–24 months postpartum, participants were less likely to be sexually active before 6 weeks postpartum (OR, 0.10; 95% CI, 0.05–0.21; P < 0.001) and from 6 weeks up to 12 months postpartum (OR, 0.57; 95% CI, 0.38–0.85; P = 0.006). Sexual intercourse was linked to: living with the birth father (OR, 8.43; 95% CI, 5.12–13.86; P < 0.001); intending to become pregnant (OR, 3.20; 95% CI, 1.53–6.65; P = 0.002); smoking marijuana (OR, 2.60; 95% CI, 1.38–4.79; P = 0.003); and using alcohol (OR, 1.93; 95% CI, 1.17–3.20; P = 0.011).
Analysis of factors associated with RRP (Box 3) showed current use of long-acting contraceptives was associated with a reduced incidence of RRP (OR, 0.27; 95% CI, 0.12–0.62; P = 0.002). Teenagers using an oral contraceptive had a similar risk of RRP to those using barrier methods or no contraception. Other factors associated with RRP were: being sexually active for more than 3 months (OR, 8.96; 95% CI, 1.97–40.74; P = 0.005); intending to become pregnant (OR, 2.39; 95% CI, 1.62–4.93; P = 0.018); and being an Indigenous Australian (OR, 2.38; 95% CI, 1.38–4.11; P = 0.002).
This is the first Australian study to prospectively study the predictors of RRP in an unselected population of teenage mothers. The incidence of RRP of 33% is consistent with findings in the existing literature,3,7 as is our finding that use of long-acting contraceptives reduces the incidence of RRP.7,8
Most teenagers resumed sex within 3 months of giving birth. Contraceptive counselling and free access to contraception postpartum did not guarantee contraceptive use. Early resumption of sexual intercourse without contraception was common. Two teenagers were already pregnant by 6 weeks postpartum, highlighting that the 6-week check may be too late for providing contraceptive counselling and reviewing contraceptive options. Our finding that 94% of teenagers had resumed sex by 24 months postpartum reinforces the need for ongoing contraceptive support and follow-up in this population, to encourage long-term use.
A surprising finding in our study was that teenagers using an oral contraceptive were as likely as those using barrier methods or no contraception to experience RRP. Teenagers can be poor users of oral contraceptives,11 and condom use in this population is often inconsistent.20 Long-acting contraceptives appear to be the only means by which RRP is effectively reduced in this population.8,11
Our observation that intention with regard to a second pregnancy predicted both resumption of sexual intercourse and RRP suggests that clinicians should enquire directly about teenagers’ intention with regard to further pregnancy. For teenagers planning an RRP, counselling may be helpful for conveying the likely advantages of delaying another pregnancy for at least 2 years.3 Alternatively, the clinical focus could shift to preconception planning, and social and educational support to avoid adverse outcomes.
Cigarette, alcohol and marijuana use are high in teenage mothers.6 Consistent with other studies, we found that alcohol and marijuana use dropped during pregnancy,21 but rates of cigarette smoking remained high.22 The use of cigarettes and alcohol postpartum increased with time.23 This is the first study to prospectively follow marijuana and alcohol use postpartum and to show a link between these activities and sexual intercourse. Clinicians should ask teenage mothers about alcohol and drug use as it may provide an opportunity for health promotion.23 However, as effective cessation strategies have not been established for this group, this is an important area for future health promotion research.
It has been shown that Indigenous Australian teenagers are more likely to experience teenage pregnancy than non-Indigenous Australian teenagers.24 Our study is the first to demonstrate that Indigenous teenagers are at increased risk of RRP compared with non-Indigenous teenagers. Providing Indigenous teenagers with culturally appropriate advice and accessible contraception will reduce their exposure to the increased social inequality associated with RRP.
There were limitations to the design of our study. After the birth, we answered all questions from the teenagers about contraception and provided referrals. These factors would have affected the findings. As teenagers could attend other KEMH antenatal clinics and also give birth at KEMH without attending for antenatal care, we were only able to approach 52% of teenagers giving birth to their first baby at KEMH.
Our data have shown that there are two options available for reducing the rate of RRP. The first is to provide teenage mothers with ready access to long-acting contraceptives and provide ongoing contraceptive support to encourage their long-term use. The second is for health care providers to gain a clear understanding of teenage mothers’ intention with regard to repeat pregnancy so appropriate advice and support can be given.
1 Characteristics of participants recorded at recruitment and follow-up visits, by rapid repeat pregnancy (RRP) or no RRP*
Variable |
All† |
RRP‡ |
No RRP§ |
P |
|||||||||||
Age in years at initial conception, median (IQR) [range] |
17 (16–17) |
16 (16–17) |
17 (16–17) |
0.623 |
|||||||||||
Age in years at first sex, median (IQR) [range] |
15 (14–16 |
15 (14–16) |
15 (14–16) |
0.667 |
|||||||||||
Indigenous Australian |
26 (18%) |
11(22%) |
15 (15%) |
0.311 |
|||||||||||
Low SES |
52 (35%) |
14 (29%) |
38 (39%) |
0.223 |
|||||||||||
Age-inappropriate education |
95 (65%) |
32 (65%) |
63 (64%) |
0.973 |
|||||||||||
Returned to school within 12 m |
34 (27%) |
10 (22%) |
24 (31%) |
0.276 |
|||||||||||
Unemployed at 12 m |
108 (87%) |
44 (96%) |
64 (82%) |
0.029 |
|||||||||||
Unemployed at 21 m |
74 (67%) |
33 (79%) |
41 (60%) |
0.057 |
|||||||||||
Low self-esteem¶ |
75 (51%) |
17 (35%) |
58 (59%) |
0.002 |
|||||||||||
Low self-efficacy** |
97 (66%) |
35 (71%) |
62 (63%) |
0.919 |
|||||||||||
Depression†† |
38 (26%) |
9 (18%) |
29 (30%) |
0.419 |
|||||||||||
Anxiety†† |
56 (38%) |
20 (41%) |
36 (37%) |
0.778 |
|||||||||||
Stress†† |
46 (31%) |
15 (31%) |
31 (32%) |
0.861 |
|||||||||||
Abnormal family function‡‡ |
40 (27%) |
14 (29%) |
26 (27%) |
0.850 |
|||||||||||
Relationship with birth father |
97 (66%) |
35 (71%) |
62 (63%) |
0.461 |
|||||||||||
Living with birth father |
64 (44%) |
19 (39%) |
45 (46%) |
0.911 |
|||||||||||
Living with birth father at 12 m |
47 (38%) |
23 (50%) |
24 (31%) |
0.033 |
|||||||||||
Never used contraception |
19 (13%) |
5 (10%) |
14 (14%) |
0.448 |
|||||||||||
Not using contraception at first conception |
71 (48%) |
22 (45%) |
49 (50%) |
0.419 |
|||||||||||
Did not intend to get pregnant§§ |
112 (76%) |
33 (67%) |
79 (81%) |
0.094 |
|||||||||||
Pregnancy intentions kept changing§§ |
23 (16%) |
12 (24%) |
11 (11%) |
— |
|||||||||||
Intended to get pregnant§§ |
12 (8%) |
5 (10%) |
7 (7%) |
— |
|||||||||||
No contraceptive switches within 24 m |
44 (40%) |
6 (14%) |
38 (57%) |
<0.001 |
|||||||||||
Smoker before first pregnancy |
91 (62%) |
32 (65%) |
59 (60%) |
0.707 |
|||||||||||
Smoked during first pregnancy |
66 (45%) |
23 (47%) |
43 (44%) |
0.806 |
|||||||||||
Smoking at 3 m |
68 (50%) |
24 (50%) |
44 (49%) |
0.950 |
|||||||||||
Smoking at 15 m |
77 (66%) |
26 (59%) |
51 (70%) |
0.234 |
|||||||||||
Alcohol before first pregnancy |
101 (69%) |
38 (78%) |
63 (64%) |
0.131 |
|||||||||||
Alcohol at 3 m |
68 (50%) |
21 (44%) |
47 (53%) |
0.349 |
|||||||||||
Alcohol at 15 m |
77 (66%) |
26 (59%) |
51 (70%) |
0.234 |
|||||||||||
Marijuana before first pregnancy |
64 (44%) |
20 (41%) |
44 (45%) |
0.362 |
|||||||||||
Marijuana at 3 m |
30 (22%) |
11 (23%) |
19 (21%) |
0.832 |
|||||||||||
Marijuana at 15 m |
22 (19%) |
8 (18%) |
14 (19%) |
0.894 |
|||||||||||
SES = socioeconomic status. m = months postpartum. * Percentages may not add up to 100% due to missing values for some variables. Proportions are expressed as number (%) unless specified as medians, interquartile ranges (IQR) and ranges. Unless stated otherwise, variables are based on numbers recorded at recruitment. † Baseline population: n = 147 at 6 weeks; n = 137 at 3 m; n = 124 at 12 m; n = 117 at 15 m; n = 110 at 21 m; and n = 109 at 24 m. ‡ Baseline population: n = 49 at 6 weeks; n = 48 at 3 m; n = 46 at 12 m; n = 44 at 15 m; n = 42 at 21 m; and n = 42 at 24 m. § Baseline population: n = 98 at 6 weeks; n = 89 at 3 m; n = 78 at 12 m; n = 73 at 15 m; n = 68 at 21 m; and n = 67 at 24 m. ¶ Measured using the Rosenberg Self-Esteem Scale. ** Measured using the Perceived Self Efficacy Index. †† Measured using the Depression Anxiety and Stress Scales. ‡‡ Measured using the McMaster Family Assessment Device. §§ Measure derived from London Measure of Unplanned Pregnancy. |
|||||||||||||||
3 Factors simultaneously associated with sexual intercourse and rapid-repeat pregnancy (RRP) until 24 months postpartum, identified by multivariable logistic regression
Outcome |
No. (%) |
Odds ratio (95% CI) |
P |
||||||||||||
Sexual intercourse* |
|
|
|
||||||||||||
Contraception |
|
|
|
||||||||||||
Barrier methods or no contraception |
299 (33%) |
1.00 |
|
||||||||||||
Oral contraceptive use |
144 (16%) |
2.83 (1.38–5.82) |
0.005 |
||||||||||||
Long-acting contraceptive use |
453 (51%) |
1.59 (0.92–2.75) |
0.095 |
||||||||||||
Resumption of sex |
|
|
|
||||||||||||
12 months to 24 months postpartum |
447 (50%) |
1.00 |
|
||||||||||||
Before 6 weeks postpartum |
114 (13%) |
0.10 (0.05–0.21) |
<0.001 |
||||||||||||
6 weeks to 12 months postpartum |
335 (37%) |
0.57 (0.38–0.85) |
0.006 |
||||||||||||
Living with birth father |
317 (35%) |
8.43 (5.12–13.86) |
<0.001 |
||||||||||||
Intends to become pregnant |
158 (18%) |
3.20 (1.53–6.65) |
0.002 |
||||||||||||
Marijuana use |
206 (23%) |
2.60 (1.38–4.79) |
0.003 |
||||||||||||
Alcohol use |
549 (61%) |
1.93 (1.17–3.20) |
0.011 |
||||||||||||
RRP† |
|
|
|
||||||||||||
Contraception |
|
|
|
||||||||||||
Barrier methods or no contraception |
238 (32%) |
1.00 |
|
||||||||||||
Oral contraceptive use |
137 (18%) |
0.91 (0.39–2.12) |
0.832 |
||||||||||||
Long-acting contraceptive use |
375 (50%) |
0.27 (0.12–0.62) |
0.002 |
||||||||||||
Ongoing sexual intercourse over > 3 months |
120 (16%) |
8.96 (1.97–40.74) |
0.005 |
||||||||||||
Intends to become pregnant |
170 (23%) |
2.39 (1.62–4.93) |
0.018 |
||||||||||||
Indigenous Australian |
94 (13%) |
2.38 (1.38–4.11) |
0.002 |
||||||||||||
* Predictors of sexual intercourse, for all teenagers for each 3-month period, with 896 “teenager-months” analysed. † Predictors of RRP, only for sexually active teenagers for each 3-month period, with 750 “teenager-months” analysed. |
|||||||||||||||
- Lucy N Lewis1
- Dorota A Doherty1
- Martha Hickey2
- S Rachel Skinner3
- 1 University of Western Australia, Perth, WA.
- 2 University of Melbourne, Melbourne, VIC.
- 3 Discipline of Paediatrics and Child Health, University of Sydney, Sydney, NSW.
This study was supported by a Princess Margaret Hospital for Children Clinical Research Scholarship, WA; the Women and Infants Research Foundation, WA; and a Raine Medical Research Foundation Priming Grant, University of WA. We are grateful for the database construction, maintenance and biostatistical support provided by James Humphreys and Angela Jacques.
None identified.
- 1. Coory M. Trends in birth rates for teenagers in Queensland, 1988 to 1997: an analysis by economic disadvantage and geographic remoteness. Aust N Z J Public Health 2000; 24: 316-319.
- 2. van der Klis KA, Westenberg L, Chan A, et al. Teenage pregnancy: trends, characteristics and outcomes in South Australia and Australia. Aust N Z J Public Health 2002; 26: 125-131.
- 3. Boardman LA, Allsworth J, Phipps MG, Lappane KL. Risk factors for unintended versus intended rapid repeat pregnancies among adolescents. J Adolesc Health 2006; 39: 597.e1-597.e8.
- 4. Jumping-Eagle S, Sheeder J, Kelly L, Stevens-Simon C. Association of conventional goals and perceptions of pregnancy with female teenagers’ pregnancy avoidance behavior and attitudes. Perspect Sex Reprod Health 2008; 40: 74-80.
- 5. Stevens-Simon C, Kelly L, Singer D. Absence of negative attitudes toward childbearing among pregnant teenagers. A risk factor for a rapid repeat pregnancy? Arch Pediatr Adolesc Med 1996; 150: 1037-1043.
- 6. Quinlivan JA, Petersen RW, Gurrin LC. Adolescent pregnancy: psychopathology missed. Aust N Z J Psychiatry 1999; 33: 864-868.
- 7. Raneri LG, Wiemann CM. Social ecological predictors of repeat adolescent pregnancy. Perspect Sex Reprod Health 2007; 39: 39-47.
- 8. Stevens-Simon C, Kelly L, Kulick R. A village would be nice but it takes a long-acting contraceptive to prevent repeat adolescent pregnancies. Am J Prev Med 2001; 21: 60-65.
- 9. Kershaw TS, Niccolai LM, Ickovics JR, et al. Short and long-term impact of adolescent pregnancy on postpartum contraceptive use: implications for prevention of repeat pregnancy. J Adolesc Health 2003; 33: 359-368.
- 10. Kelly LS, Sheeder J, Stevens-Simon C. Why lightning strikes twice: postpartum resumption of sexual activity during adolescence. J Pediatr Adolesc Gynecol 2005; 18: 327-335.
- 11. Templeman CL, Cook V, Goldsmith LJ, et al. Postpartum contraceptive use among adolescent mothers. Obstet Gynecol 2000; 95: 770-776.
- 12. Zubrick SR, Lawrence DM, Silburn SR, et al. The Western Australian Aboriginal Child Health Survey (volume 1): the health of Aboriginal children and young people. Perth: Telethon Institute for Child Health Research, 2004. Available at: http://www.ichr.uwa.edu.au/waachs (accessed Oct 2009).
- 13. Barrett G, Smith SC, Wellings K. Conceptualisation, development, and evaluation of a measure of unplanned pregnancy. J Epidemiol Community Health 2004; 58: 426-433.
- 14. Rosenberg M. Society and the adolescent self image. Princeton, NJ: Princeton University Press, 1965.
- 15. Cowen EL, Work WC, Hightower PA, et al. Toward the development of a measure of perceived self-efficacy in children. J Clin Child Psychol 1991; 20: 169-178.
- 16. Lovibond PF, Lovibond SH. The structure of negative emotional states: comparison of the Depression Anxiety Stress Scales (DASS) with the Beck Depression and Anxiety Inventories. Behav Res Ther 1995; 33: 335-343.
- 17. Epstein NB, Baldwin LM, Bishop DS. The McMaster Family Assessment Device. J Marital Fam Ther 1983; 9: 171-180.
- 18. Australian Bureau of Statistics. Information paper: an introduction to Socio-Economic Indexes for Areas (SEIFA), 2006. (ABS Cat No. 2039.0.)
- 19. Hintzte J. PASS user’s guide: PASS 2000 power analysis and sample size for windows. Kaysville, Utah: NCSS, 2000.
- 20. Meade CS, Ickovics JR. Systematic review of sexual risk among pregnant and mothering teens in the USA: pregnancy as an opportunity for integrated prevention of STD and repeat pregnancy. Soc Sci Med 2005; 60: 661-678.
- 21. Crome IB, Kumar MT. Epidemiology of drug and alcohol use in young women. Semin Fetal Neonatal Med 2007; 12: 98-105.
- 22. Chan DL, Sullivan EA. Teenage smoking in pregnancy and birthweight: a population study, 2001-2004. Med J Aust 2008; 188: 392-396. <MJA full text>
- 23. Gillmore MR, Gilchrist L, Lee J, Oxford ML. Women who gave birth as unmarried adolescents: trends in substance use from adolescence to adulthood. J Adolesc Health 2006; 39: 237-243.
- 24. Lewis LN, Hickey M, Doherty DA, Skinner SR. How do pregnancy outcomes differ in teenage mothers? A Western Australian Study. Med J Aust 2009; 190: 537-541. <MJA full text>





Abstract
Objectives: To examine the determinants of pregnancy within 2 years of a teenager giving birth for the first time (rapid-repeat pregnancy [RRP]) and resumption of sexual intercourse after the birth.
Design, setting and participants: Prospective cohort study between June 2004 and September 2006 at the sole tertiary obstetric hospital in Western Australia involving teenagers who gave birth for the first time. Data were collected using questionnaires at recruitment, 6 weeks and 3-monthly intervals for up to 2 years postpartum.
Main outcome measures: RRP and time to a return to sexual intercourse after giving birth.
Results: Of the 147 participants, 49 (33%) experienced an RRP. Sexual intercourse was independently significantly associated with using an oral contraceptive (odds ratio [OR], 2.83; 95% CI, 1.38–5.82); living with the birth father (OR, 8.43; 95% CI, 5.12–13.86); intending to become pregnant (OR, 3.20; 95% CI, 1.53–6.65); smoking marijuana (OR, 2.60; 95% CI, 1.38–4.79); and using alcohol (OR, 1.93; 95% CI, 1.17–3.20). Use of long-acting contraceptives was associated with reduced odds of RRP (OR, 0.27; 95% CI, 0.12–0.62), while teenagers who used an oral contraceptive had a similar risk of RRP compared with those using barrier methods or no contraception. Other factors predicting RRP were: being sexually active for more than 3 months (OR, 8.96; 95% CI, 1.97–40.74); intending to become pregnant (OR, 2.39; 95% CI, 1.62–4.93); and being an Indigenous Australian (OR, 2.38; 95% CI, 1.38–4.11).
Conclusion: There are two options available to health care providers for reducing the rate of RRP: to facilitate teenage mothers’ access to long-acting contraceptives; and to gain clear understanding of their intention with regard to repeat pregnancy and to provide appropriate support.