Timely primary percutaneous coronary intervention (PCI) has proven mortality benefits over thrombolysis for treating ST-elevation myocardial infarction (STEMI).1 These benefits are time dependent with longer door-to-balloon (DTB) times associated with higher mortality.2-6 Every 30-minute delay in PCI increases the absolute risk of the patient dying in hospital by 1%.6 Guidelines recommend DTB times < 90 minutes in 75% of cases presenting to institutions providing primary PCI.7,8 Australian registry data suggest these targets are rarely achieved, with median DTB times of 102 minutes and only 35% of cases performed in < 90 minutes.9
The importance of reducing DTB times was noted in a recent position statement by the Australian Acute Coronary Syndromes (ACS) Implementation and Advocacy Working Group, which recommends that the cardiac catheterisation laboratory (CCL) be activated by a single call by the first health care professional qualified to recognise a STEMI.10 Traditionally, evaluation by the cardiology team is required for activation of the CCL. However, emergency physicians usually see patients with STEMI first and many initiated thrombolysis before PCI was introduced.11
System changes enabling emergency department (ED) activation of the CCL and immediate patient transfer have reduced DTB times in the United States and Canada.12-14 Barriers to implementing ED activation of the CCL are concerns about handing over diagnostic responsibility;15 potential adverse outcomes from misdiagnosis; overcalling; and increased resource use. Current Australian practice is variable and individualised by hospital or health service. We understand that many Australian hospitals continue to use cardiology activation of the CCL by the cardiology team.
Our hospital’s audit data suggested that we were not achieving target DTB times despite many practice changes. Therefore, we changed CCL activation criteria and practices, with close collaboration between the emergency and cardiology departments. The aim of our study was to determine if ED activation of the CCL and immediate patient transfer to the CCL (the “Code STEMI” protocol [Box 1]) reduces overall DTB times and increases the proportion of patients for whom the recommended DTB time of < 90 minutes is achieved.
We conducted an observational study of patients presenting consecutively to Sir Charles Gairdner Hospital, Perth, Western Australia, from January 2007 to October 2009, who underwent emergency coronary angiography for suspected STEMI. We included patients of all ages; those who had suffered a cardiac arrest outside the hospital; were in cardiogenic shock; were undergoing imaging to exclude aortic dissection; had non-diagnostic first electrocardiography; and those who presented more than 12 hours after the onset of pain and underwent primary PCI for ongoing pain or cardiac conduction instability. Patients transferred from other hospitals and those having “rescue” PCI for unsuccessful thrombolysis were excluded, as the ED was not involved in their care. Median DTB times before and after implementation of the Code STEMI protocol were compared.
The traditional protocol involved the cardiology team activating the CCL and routine transfer of the patient to the CCL (Box 2). A collaborative root-cause analysis of the protocol was undertaken in November 2008 to decide how to improve the system of care. Two main reasons for prolonged DTB times were identified: lengthy and complicated decision-making processes and delays in patient transfers to the CCL.
Code STEMI was introduced in February 2009 and involved four main changes: emergency physician CCL activation; ED single-call CCL activation; immediate patient transfer to the CCL by ED staff; and early feedback of results to all staff involved.
During office hours (8 am to 5 pm, Monday to Friday), patient transfers to the CCL occurred as soon as possible using a “pack up and go” approach. Any unnecessary procedures, such as chest x-rays, and heparin and nitrate infusions, were avoided. For patients who arrived after hours, we aimed for a 20-minute period from activation to their arrival in the CCL to give CCL staff enough time to arrive at the hospital. After-hours patients who were in cardiogenic shock, intubated or had cardiac conduction instability often required cardiologist assessment before transfer. Emergency staff were encouraged to assist with CCL patient care and observe procedures for educational purposes.
Results including median DTB time, door-to-activation (DTA) time, activation-to-balloon (ATB) time, coronary anatomy and procedural success were emailed to ED and cardiology staff within 48 hours. Electrocardiograms (ECGs), DTB times and coronary angiograms of interesting cases were posted on an ED noticeboard. Results were presented quarterly at departmental meetings. The protocol was dynamic, with ongoing minor changes (eg, ensuring coronary-care staff turned CCL lights on for after-hours patients).
Throughout the study, staff recorded the door, activation and balloon times in the CCL database at the time of coronary angiography. After reviewing their medical records, we classified the patients into four subgroups: those who underwent PCI; false positives; those whose acute coronary syndromes were managed medically; and those whose acute coronary syndromes were managed with coronary artery bypass graft surgery. Based on prespecified criteria (Box 1) and with blinding to DTB times, we classified those undergoing PCI as suitable for ED activation either with or without cardiologist consultation. Post-PCI charts were reviewed for clinical and outcome data not recorded in the CCL database. All data were entered into a version of the existing CCL Excel database with added data fields. To assess inter-rater reliability, a second reviewer (D M) checked 28 randomly selected medical records.
The primary outcome measures were median DTB time and the percentage of patients with a DTB time < 90 minutes. Secondary outcomes were DTA time, ATB time and false-positive rates. DTA time is a direct marker of the time taken to record an ECG, take a directed history and decide about further investigation and care. ATB time measures the transfer process and procedural times. False positives were defined as coronary artery luminal narrowing < 50%, without a visible culprit lesion and no wall-motion abnormality in the distribution of ECG changes.16 Subgroup analysis was performed for after-hours presentations, ambulance presentations and those meeting immediate ED activation criteria.
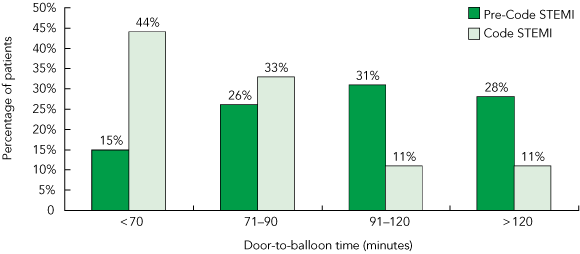
Two hundred and thirty-four ED patients were transferred to the CCL for suspected STEMI, of whom 188 (80%) underwent primary PCI (118 before, and 70 after Code STEMI implementation); 15 (6%) were managed medically; 27 (12%) were false-positive activations of the CCL; and 4 (2%) had emergency coronary artery bypass graft surgery. There were no significant differences between the demographic or clinical features of the cohorts undergoing PCI before and after Code STEMI implementation (Box 3). After implementation of Code STEMI, the median DTB time was reduced by 20 minutes (97 to 77 min; P < 0.001) (Box 4) and the proportion of DTB times < 90 min increased from 41% to 77% (P < 0.001) (Box 5). Improvements were seen early in the study and were maintained throughout the implementation period: the median DTB time during the first 3 months was 79 min (n = 24); from 4 to 9 months, it was 77 min (n = 46) (P = 0.496). There was no difference in false positive CCL activation rates (12% before v 11% after code STEMI; P = 0.38).
For subjects who met immediate ED activation criteria, the median DTB time was reduced from 88 to 63 min (P < 0.001) and the proportion of DTB times < 90 min increased from 53% (38/72) to 93% (42/45; P < 0.001). There were significant improvements in median DTA times (11 v 22 min; P < 0.001) and median ATB times (55 v 64 min; P = 0.03). The shortest times occurred during office hours for patients who met criteria for immediate ED activation (median DTB time, 54 min; n = 15).
For subjects requiring cardiology consultation, the median DTB time was reduced from 139 to 94 min (P < 0.006). Also for this group, improvement was seen in both median DTA (57 v 43 min; P = 0.220) and median ATB times (69 v 50 min; P = 0.006).
After-hours DTB times were longer in both cohorts (Box 6). DTA times pre-Code STEMI were twice as long after hours as during office hours (41 v 21 min; P < 0.001), whereas Code STEMI DTA times were similar regardless of presentation time (19 v 15 min; P = 0.24).
There were insignificant differences in DTB times for ambulance arrivals compared with self-presenters (88 v 91 min; P = 0.40) or between sexes (89 min for men v 86 for women; P = 0.61).
Assessment of inter-rater reliability showed agreement on 271 of the 315 collected data points. The κ coefficient (Cohen’s method) was 0.72 (95% CI, 0.64–0.79), suggesting substantial agreement.
This is the first published report of an Australian experience of a system change involving ED activation of the CCL and immediate patient transfer. We showed that this simple, cost-effective approach resulted in immediate and sustained improvements with a highly significant 20-minute reduction in median DTB time and a marked increase in the proportion of patients with < 90 minute DTB times. Fears concerning overcalling or misdiagnoses were not confirmed, with no change in false-positive rates. These rates are comparable to other centres.16 Two important steps of the primary angioplasty pathway were improved: the decision-making process and transfer of the patient to the CCL.
ED activation of the CCL reduces DTA times and was particularly beneficial for after-hours presentations. With traditional activation by a cardiologist, whereby the emergency doctor involves the cardiology registrar who then involves the cardiology consultant, after-hours DTA times were twice as long. With ED activation, DTA times were shorter and independent of the time of presentation.
The impact of immediate patient transfer to the CCL was as important in reducing DTB times as ED activation. Early in the implementation process, ED and CCL staff were concerned about after-hours patients arriving at the CCL before CCL staff. This was addressed by setting a target time of 20 minutes for after-hours activation to CCL reception of the patient. Additionally, after-hours patients in cardiogenic shock or with cardiac conduction instability were transferred with cardiology and ED staff support. During office hours, there were minimal staffing problems preventing immediate patient transfer.
It is important to appreciate that the clinical variability among patients undergoing primary angioplasty is great and decision-making is often difficult. In our study, patients with prolonged DTA times included older people or those with significant comorbidities, borderline first ECGs, out-of-hospital cardiac arrests, left bundle branch block, chest pain for longer than 12 hours, atypical pain or pain suggesting acute aortic dissection. For these patients, DTB times are appropriately longer, allowing for correct management decisions and essential cardiology team collaboration.
In patients who meet ED activation criteria, the decision-making process is straightforward, which is reflected in shorter DTB times. For this subgroup, in which most people with STEMI belong (about two-thirds of our cases), it is realistic to expect DTB times of < 90 minutes in 90% and to aim for 60-minute DTB times, particularly during office hours.
Despite these improvements, ATB times remain longer after hours, indicating that the time taken by CCL staff to arrive at the hospital is a limiting factor. Prehospital activation of the CCL based on ambulance-performed ECGs, sent digitally to the ED, may reduce this discrepancy.
Accessibility to Australian data on DTB times for patients with STEMI and relevant hospital programs is limited to article abstracts and conference presentations. We strongly support the National Heart Foundation ACS Implementation and Advocacy Working Group’s recommendations of “improved STEMI data collection” at a health-department level and development of a “national web-based portal to enable health services and clinical networks to access and share locally developed evidence based clinical pathways and educational tools”.10,16 A successful United States program called the “D2B: an alliance for quality” is a useful model.17-19
Considerable delays remain for patients with STEMI presenting to hospital, with one-third arriving more than 2 hours into their acute myocardial infarction. Decreasing DTB times, although proven to reduce mortality, should be seen as complementary to increasing use of, and earlier contact with, ambulance services by patients with chest pain. Success of mass media campaigns to reduce patient delay in calling ambulances has been short-lived.20 The National Heart Foundation’s “Chest pain — every minute counts working group” has developed an action plan to induce people to respond promptly to warning signs of heart attack.20,21
In assessing our DTB times, we attempted to limit bias by including all patients requiring primary PCI regardless of their clinical presentation. For example, we included those requiring exclusion of aortic dissection (two in the Code STEMI cohort, both with DTB times > 180 minutes) and patients whose first ECG was non-diagnostic. The increased frequency of patient transfer to the CCL for suspected STEMI after Code STEMI implementation follows a trend at our centre since 2004. It may represent a lower threshold for ordering emergency coronary angiography and a change in the referral pattern, with a tendency for ambulances to divert patients with a potential STEMI to primary PCI-capable centres.
A limitation of this study is that it did not include patients transferred from secondary hospitals for primary PCI. DTB times for these patients are longer and outcomes may be worse. Planned implementation of prehospital diagnosis with ambulance diversion to dedicated 24-hour primary PCI centres may help solve this problem. Another limitation is potential measurement error in allocating ED activation criteria. We reviewed charts retrospectively for data that met prespecified inclusion–exclusion criteria for independent ED activation (Box 1). Despite this, reduction in times was achieved in both ED and cardiology activation groups, showing that the protocol is applicable to all patients requiring primary PCI. Some improvements may be due to the “Hawthorn effect” (that is, subjects improve an aspect of their performance simply as a result of being studied).22 Countering this was an intense focus on DTB times by our centre over the previous 2 years; during that time, we achieved some improvement but it had plateaued before we introduced Code STEMI. We assume that reduced ATB times resulted from earlier patient arrival at the CCL and that procedural times remained constant. Mortality rates of our study are lower than those reported in most studies but this may be an effect of our small sample.
Some Australian centres are implementing earlier CCL activation through ambulance officers recording 12-lead ECGs and digitally conveying them to a referral centre.23 This approach may be ideal,24,25 but requires considerable resources and coordination of many stakeholders, expensive initial equipment and ambulance personnel training. Other deficiencies of prehospital activation of the CCL include: at some centres, 50% or more of patients with STEMIs self-present;14 not all ambulances will have the necessary equipment or personnel; and the clinical profile of about 30% of patients may make prehospital activation inappropriate. Therefore, a system involving the ED activating the CCL and immediate patient transfer should be seen as a complementary process because it is simple, cost-effective, applicable to all patients and has immediate and sustained results.
A collaborative approach between the ED and the cardiology team, based on agreed criteria for independent ED activation of the CCL and immediate patient transfer, has shown dramatic improvements in median DTB time and allowed us to meet current Australasian standards. This study strongly supports the recent position statement of the National Heart Foundation ACS Implementation and Advocacy Working Group on delivering best practice for patients with ACS. Widespread implementation of the Code STEMI protocol should significantly improve the clinical outcome for patients with STEMI undergoing primary PCI.
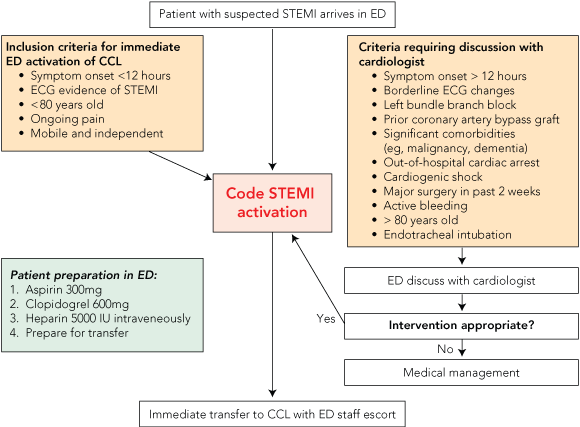
1 Code STEMI* pathway
 | |||||||||||||||
|
CCL = cardiac catheterisation laboratory. ECG = electrocardiogram. ED = emergency department. | |||||||||||||||
2 Management pathway of ST-elevation myocardial infarction (STEMI) before implementation of Code STEMI* (January 2007 to January 2009) and after implementation of Code STEMI (February 2009 to October 2009)
 |
|
CABG = coronary artery bypass graft. CCL = cardiac catheterisation laboratory. |
3 Demographic and clinical features of patients with ST-elevation myocardial infarction (STEMI) undergoing primary PCI before implementation of Code STEMI* (January 2007 to January 2009) and after implementation of Code STEMI (February 2009 to October 2009)
Pre-Code STEMI† (n = 118) |
Code STEMI* (n = 70) |
P |
|||||||||||||
Age (SD) [range] |
61 (± 12) [35–89] |
63 (± 12) [41–91] |
0.33 |
||||||||||||
Age > 80 years |
8 (7%) |
7 (10%) |
0.43 |
||||||||||||
Male |
96 (81%) |
53 (76%) |
0.44 |
||||||||||||
Ambulance arrival |
91 (77%) |
49 (70%) |
0.28 |
||||||||||||
After-hours presentation |
67 (57%) |
42 (60%) |
0.66 |
||||||||||||
Pain-to-door time |
|
|
0.29 |
||||||||||||
≤ 1 hour |
30 (25%) |
18 (26%) |
|
||||||||||||
> 1–2 hours |
41 (35%) |
29 (41%) |
|
||||||||||||
> 2–6 hours |
34 (29%) |
15 (22%) |
|
||||||||||||
> 6–12 hours |
5 (4%) |
4 (6%) |
|
||||||||||||
≥ 12 hours |
1 (1%) |
3 (4%) |
|
||||||||||||
Missing values |
7 (6%) |
1 (1%) |
|
||||||||||||
Prehospital activation of CCL |
0 |
0 |
|
||||||||||||
Criteria met for immediate ED activation of CCL |
72 (61%) |
45 (64%) |
0.74 |
||||||||||||
Drug-eluting stent(s) |
61 (52%) |
36 (51%) |
0.50 |
||||||||||||
Peak creatine kinase serum level (mean U/L) |
1943 |
1964 |
0.94 |
||||||||||||
Median length of stay (days) |
3 |
3 |
0.94 |
||||||||||||
In-hospital mortality (%) |
2 (2%) |
0 |
0.27 |
||||||||||||
Site of culprit lesion |
|
|
0.47 |
||||||||||||
Left main coronary artery |
2 (2%) |
0 |
|
||||||||||||
Left anterior descending coronary artery |
46 (39%) |
32 (46%) |
|
||||||||||||
Circumflex coronary artery |
15 (13%) |
5 (7%) |
|
||||||||||||
Right coronary artery |
54 (46%) |
33 (47%) |
|
||||||||||||
Coronary artery bypass graft |
1 (1%) |
0 |
|
||||||||||||
Mean emergency CCL transfers per month |
6 |
9 |
0.08 |
||||||||||||
CCL = cardiac catheterisation laboratory. ED = emergency department. PCI = percutaneous coronary intervention. * Protocol involving activation of CCL by cardiology team and routine patient transfer to CCL. |
|||||||||||||||
4 Median door-to-balloon, door-to-activation, activation-to-balloon and pain-to-door times before implementation of Code STEMI* (January 2007 to January 2009) and after implementation of Code STEMI (February 2009 to October 2009)
|
Pre-Code STEMI† (n = 118) |
Code STEMI* (n = 70) |
P |
||||||||||||
Door-to-balloon time‡ (IQR) |
97 (79–123) |
77 (60–89) |
< 0.001 |
||||||||||||
Door-to-activation time‡ (IQR) |
28 (16–47) |
15 (8–340) |
0.002 |
||||||||||||
Activation-to-balloon time‡ (IQR) |
66 (52–75) |
53 (45–63) |
< 0.001 |
||||||||||||
Pain-to-door time‡ (IQR) |
89 (58–186) |
92 (60–169) |
0.926 |
||||||||||||
IQR = interquartile range. STEMI = ST-elevation myocardial infarction. * Protocol involving activation of cardiac catheterisation laboratory (CCL) by emergency department and immediate transfer of patient with STEMI to CCL. † Protocol involving activation of CCL by cardiology team and routine patient transfer to CCL. ‡ Median times in minutes. |
|||||||||||||||
5 Percentage of patients with suspected ST-elevation myocardial infarction (STEMI) achieving various door-to-balloon times before implementation of Code STEMI* (January 2007 to January 2009) and after implementation of Code STEMI (February 2009 to October 2009)
 |
|
* Protocol involving emergency physician activation of the cardiac catheterisation laboratory (CCL) and immediate transfer of patients with suspected STEMI to the CCL. |
6 Impact of the time when the patient presents to hospital on median door-to-balloon, door-to-activation and activation-to-balloon times before implementation of Code STEMI* (January 2007 to January 2009) and after implementation of Code STEMI (February 2009 to October 2009)
|
Office hours† |
After hours |
|||||||||||||
|
Pre-Code STEMI‡ (n = 51) |
Code STEMI (n = 28) |
P |
Pre-Code STEMI (n = 67) |
Code STEMI (n = 42) |
P |
|||||||||
Door-to-activation time (IQR)§ |
21 (9–32) |
19 (11–44) |
0.521 |
41 (20–78) |
15 (8–32) |
< 0.001 |
|||||||||
Activation-to-balloon time (IQR)§ |
54 (45–66) |
43 (38–50) |
< 0.001 |
69 (63–79) |
60 (53–70) |
< 0.001 |
|||||||||
Door-to-balloon time (IQR)§ |
83 (71–96) |
61 (54–87) |
< 0.001 |
113 (93–158) |
81 (66–95) |
< 0.001 |
|||||||||
IQR = interquartile range. STEMI = ST-elevation myocardial infarction. * Protocol involving activation of cardiac catheterisation laboratory (CCL) by emergency department and immediate patient transfer to CCL. † 8 am–5 pm, Monday to Friday. ‡ Protocol involving activation of CCL by cardiology team and routine patient transfer to CCL. § Median times in minutes. |
|||||||||||||||
Received 7 March 2010, accepted 24 June 2010
- Alexander B Willson1
- David Mountain2,3
- Joanne M Jeffers2
- Cheryl G Blanton1
- Brendan M McQuillan4
- Joseph Hung4
- Michael H Muhlmann1
- Michael C Nguyen1
- 1 Cardiovascular Medicine Department, Sir Charles Gairdner Hospital, Perth, WA.
- 2 Emergency Medicine Department, Sir Charles Gairdner Hospital, Perth, WA.
- 3 Academic Department of Emergency Medicine, University of Western Australia, Perth, WA.
- 4 Sir Charles Gairdner Hospital Unit, School of Medicine and Pharmacology, University of Western Australia, Perth, WA.
We wish to acknowledge and thank for their valuable contributions to this study Dr Michelle Ammerer, Dr Devind Bhullar, Dr Donald Latchem, Dr Eric Yamen, Dr Phil Cooke, Dr Paul Stobie, Dr Debra O’Brien, the staff of the Cardiovascular Invasive Laboratory, the staff of the Coronary Care Unit, the doctors and staff of the Emergency Department and the switchboard staff at Sir Charles Gairdner Hospital.
David Mountain received an unrestricted grant of $50 000 a year for 3 years from Roche Pharmaceuticals to collect national thrombolysis data 1998–2000. The National Heart Foundation paid his travel and accommodation expenses to attend steering group meetings for the national guideline development committee.
- 1. Keeley EC, Boura JA, Grines CL. Primary angioplasty versus intravenous thrombolytic therapy for acute myocardial infarction: a quantitative review of 23 randomised trials. Lancet 2003; 361: 13-20.
- 2. Keeley EC, Hillis LD. Primary PCI for myocardial infarction with ST segment elevation. N Engl J Med 2007; 356: 47-54.
- 3. Brodie BR, Hansen MA, Stuckey TD, et al. Door to balloon time with primary percutaneous coronary intervention for acute myocardial infarction impacts late cardiac mortality in high-risk patients and patients presenting early after the onset of symptoms. J Am Coll Cardiol 2006; 47: 289-295.
- 4. McNamara RL, Wang Y, Herrin J, et al. Effect of door-to-balloon time on mortality in patients with ST-segment elevation myocardial infarction. J Am Coll Cardiol 2006; 47: 2180-2186.
- 5. De Luca G, Suryapranata H, Ottervanger JP, et al. Time delay to treatment and mortality in primary angioplasty for acute myocardial infarction: every minute of delay counts. Circulation 2004; 109: 1223-1225.
- 6. Rathore SS, Curtis JP, Chen J, et al. Association of door to balloon time and mortality in patients admitted to hospital with ST elevation myocardial infarction: national cohort study. BMJ 2009; 338: b1807.
- 7. Acute Coronary Syndrome Guidelines Working Group. Guidelines for the management of acute coronary syndromes 2006. Med J Aust 2006; 184 (8 Suppl): S1-S32. <MJA full text>
- 8. Antman EM, Hand M, Armstrong PW, et al. 2007 focused update of the ACC/AHA 2004 guidelines for the management of patients with ST elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 2008; 51: 210-247.
- 9. Erikson M, Rankin J, Amerena J, et al. Reperfusion therapy in STEMI: ACACIA registry contemporary Australian data [abstract]. Heart Lung Circ 2007; 16 Suppl 2: S124.
- 10. Brieger D, Kelly A-M, Aroney C, et al. ACS Implementation and Advocacy Working Group. Acute coronary syndromes: consensus recommendations for translating knowledge into action. Med J Aust 2009; 191: 334-338. <MJA full text>
- 11. Hourigan CT, Mountain D, Langton PE, et al. Changing the site of delivery of thrombolytic treatment for ST elevation myocardial infarction from the coronary care unit to the emergency department greatly reduces door to needle time. Heart 2000; 84: 157-156.
- 12. Bradley EH, Curry LA, Webster TR, et al. Achieving rapid door to balloon times: how top hospitals improve complex clinical systems. Circulation 2006; 113: 1079-1085.
- 13. Bradley EH, Herrin J, Winy Y, et al. Strategies for reducing the door to balloon time in acute myocardial infarction. N Engl J Med 2006; 355: 2308-2320.
- 14. Khot UN, Johnson ML, Ramsey C, et al. Emergency department physician activation of the catheterization laboratory and immediate transfer to an immediately available catheterization laboratory reduce door-to-balloon time in ST elevation myocardial infarction. Circulation 2007; 116: 67-76.
- 15. Bradley EH, Roumains S, Radford M, et al. Achieving door to balloon times that meet quality guidelines. How do the successful hospitals do it? J Am Coll Cardiol 2005; 46: 1236-1241.
- 16. Larson DM, Menssen KM, Sharkey SW, et al. “False positive” cardiac catheterization laboratory activation among patients with suspected ST segment elevation myocardial infarction. J Am Coll Cardiol 2007; 198: 2754-2760.
- 17. Scott I. Why we need a national registry in interventional cardiology. Med J Aust 2008; 189: 223-227. <MJA full text>
- 18. American College of Cardiology. D2B: an alliance for quality. http://www.d2balliance.org (accessed Jul 2010).
- 19. Krumholz HM, Bradley EH, Nallamothu BK, et al. A campaign to improve the timeliness of primary percutaneous coronary intervention: door to balloon time: an alliance for quality. J ACC Cardiovasc Interv 2008; 1: 97-104.
- 20. Finn JC, Nick Bett JH, Shilton TR, et al. Patient delay in responding to symptoms of possible heart attack: can we reduce time to care? Med J Aust 2007; 187: 293-298. <MJA full text>
- 21. Heart Foundation. Warning signs of heart attack campaign. http://www.heartfoundation.org.au/Professional_Information/Warning_Signs_of_Heart_Attack/Pages/default.aspx (accessed Jul 2010).
- 22. McCarney R, Warner J, Iliffe S, et al. The Hawthorne effect: a randomised, controlled trial. BMC Med Res Methodol 2007; 7: 30.
- 23. Hutchinson A, Malaiapan Y, Barger B, et al. Field 12 lead ECG and ED activation of the infarct team in STEMI improves door to balloon times: an update on the Monash heart acute myocardial infarction (Mon-AMI) 12 lead project [abstract] Heart Lung Circ 2009; 18: S1-S286.
- 24. Dorsch M, Greenwood J, Priestley C, et al. Direct ambulance admission to the cardiac catheterisation laboratory significantly reduces door to balloon times in primary percutaneous coronary intervention. Am Heart J 2008; 155: 1054-1058.
- 25. Brown J, Mahmud E, Dunford J, Ben-Yehuda O. Effect of prehospital 12 lead electrocardiogram on activation of the cardiac catheterisation laboratory and door to balloon time in ST elevation myocardial infarction. Am J Cardiol 2008; 101: 158-161.





Abstract
Objectives: To assess whether a collaborative interdepartmental pathway involving emergency department (ED) physicians activating the cardiac catheterisation laboratory (CCL) with immediate patient transfer to the CCL reduces door-to-balloon (DTB) times for patients with suspected ST-elevation myocardial infarction (STEMI).
Design, setting and participants: A quasi-experimental before-and-after observational study using a prospective database, supplemented by chart review, of consecutive patients transferred from the ED to the CCL for suspected STEMI, from January 2007 to October 2009, at Sir Charles Gairdner Hospital, an adult tertiary-care hospital, Western Australia.
Main outcomes measures: Median DTB time and proportion of patients with DTB time of < 90 minutes. Secondary outcomes, based on analysis of predefined subgroups, included door-to-activation time, activation-to-balloon time and false-positive activations of the CCL.
Results: Two hundred and thirty-four patients underwent emergency coronary angiography for suspected STEMI, with 188 (80%) undergoing percutaneous coronary intervention (118 before and 70 after implementation of the new pathway). Following implementation of the new pathway, median DTB time reduced from 97 to 77 minutes (P < 0.001), median door-to-activation time from 28 to 15 minutes (P = 0.002) and median activation-to-balloon time from 66 to 53 minutes (P < 0.001). The proportion of patients with recommended DTB time of < 90 minutes increased from 41% to 77% (P < 0.001) with no change in false positive CCL activation rates (12% v 11%; P = 0.38).
Conclusion: ED physician activation of CCL with immediate patient transfer is associated with highly significant improvements in DTB time without increased false positive rates.