HIV diagnoses declined in Australia during the 1990s, only to increase again through the 2000s, with men who have sex with men (MSM) continuing to be the group at greatest risk. Increased rates of HIV diagnosis have been greater in Victoria than in other states.1,2 Multiple factors are thought to be contributing to this increase, including increased rates of unprotected anal intercourse among MSM,3 an increase in other sexually transmitted infections (STIs) that facilitate HIV transmission,4,5 and increased numbers of sexually active HIV-positive MSM since the introduction of highly active antiretroviral treatment (HAART).6
Over the years, there has been an increase in the age at HIV diagnosis among MSM in Victoria,7 as would be expected given reported similarities in age within MSM sexual networks.8 Despite this trend, there has been ongoing concern about the potential risk of acquiring and transmitting HIV among younger MSM because, compared with older MSM, they have less frequent testing for HIV and STIs9 and are less likely to know their HIV status and that of their partner.10,11
The VPCNSS is a network of clinical sites participating in the surveillance of HIV, syphilis, chlamydia and/or hepatitis C.12 The HIV network sites include sexual health and gay men’s health clinics with a high case load of MSM. These sites notified about 52% of all new HIV diagnoses in Victoria in 2008 (unpublished data, Burnet Institute, 2010). Demographic and risk behaviour information are collected from MSM undergoing routine testing for HIV and linked with their test result using a unique identifier.
Between 2000 and 2009, 1635 MSM were diagnosed with HIV in Victoria. The median age of MSM at HIV diagnosis increased steadily from 34.5 years (range, 19.1–64.5 years) in 2000 to 38.8 years (range, 19.2–70.5 years) in 2007 (P = 0.001), then declined significantly to 35.3 years in 2008 (range, 17.0–75.2 years) (P = 0.023) and remained at 35.9 years (range, 17.5–78.5 years) in 2009 (Box 1). Between 2007 and 2008, HIV notifications among MSM increased in all age groups under 35 years and decreased in all age groups between 35 and 49 years. In 2009, the number of HIV diagnoses among MSM aged 25–29 years was 62% higher than in 2007 (Box 2).
Between 2000 and 2009, 41% of the total HIV diagnoses among MSM were recently acquired infections. The annual median age of MSM diagnosed with recently acquired HIV ranged between 29.8 years (range, 19.1–57.0 years) in 2000 and 36.5 years (range, 18.6–62.8 years) in 2006. By 2009, the median age of MSM diagnosed with recently acquired HIV infections had declined to 31.6 years (range, 18.9–78.5 years) (P = 0.027 for difference between 2006 and 2009) (Box 1).
Based on recent HIV passive surveillance data showing that MSM diagnoses increased in all age groups under 35 years, we dichotomised VPCNSS patients into two age groups (< 35 years and ≥ 35 years) and compared behavioural data across the two groups. Compared with MSM aged 35 years and over, MSM aged under 35 years were more likely to have never previously been tested for HIV (relative risk [RR], 1.36 [95% CI, 1.30–1.41]); to report not knowing the HIV status of their regular partner (RR, 1.11 [95%CI, 1.01–1.21]); and to report inconsistent condom use with casual partners (RR, 1.07 [95% CI, 1.01–1.14]) and regular partners (RR, 1.07 [95% CI, 1.00–1.14]). Among sexually active MSM, those aged 35 years and over were less likely to report having more than five sexual partners in the previous 6 months (RR, 0.91 [95% CI, 0.85–0.97]) (Box 3).
Between 2004 and 2009, 1313 infectious syphilis cases were diagnosed among MSM in Victoria. The median age at diagnosis among MSM increased from 35.6 years (range, 20.9–70.0 years) in 2004 to 40.6 years (range, 18.6–83.6 years) in 2007 (P = 0.001), then declined to 36.0 years (range, 17.9–70.9 years) in 2008 (P < 0.001) and 37.1 years (range, 16.7–68.9 years) in 2009 (Box 1).
Between 2000 and 2009, 4744 gonorrhoea cases were diagnosed among MSM in Victoria. The median age at diagnosis among MSM increased from 32.9 years (range, 16.6–67.2 years) in 2000 to 33.9 years (range, 15.9–66.5) in 2005, then declined to 29.3 years (range, 15.9–68.6 years) in 2008 (P < 0.001) and 29.9 years (range, 17.6–60.7 years) in 2009 (Box 1).
In 2008, we observed a significant decline in the median age of MSM diagnosed with HIV in Victoria. This decline in age, which continued into 2009, is the first observed in Australia since the introduction of HAART. The decline in the median age of MSM recently acquiring HIV suggests recent increases in HIV transmissions (as distinct from diagnoses) and risky behaviour among younger MSM. Syphilis and gonorrhoea notification rates also increased among younger MSM. These STIs are considered markers of risky sexual behaviour,13 and may provide early indicators of HIV trends because they are more infectious14 and commonly symptomatic, thus encouraging testing.15
Examination of self-reported behavioural data from the VPCNSS showed little difference across age groups in the reported number of sexual partners. Younger gay men were slightly more likely to engage in risky sexual behaviour and to be unaware of their partner’s serostatus, and were more likely to have never previously been tested for HIV. These findings are consistent with other behavioural and epidemiological data relating to testing history and knowledge of partner serostatus.9-11
In addition, recent focus group data have shown that younger MSM are less likely to discuss HIV and other STIs with peers (Burnet Institute, unpublished data). It has also been suggested that younger gay men may be more susceptible to engaging in risky sexual behaviour because they are less aware of or less concerned about the implications of HIV since the introduction of HAART.16
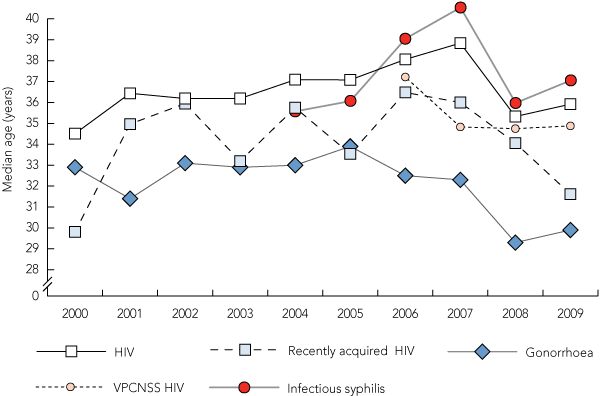
1 Median age of MSM at diagnosis of HIV, syphilis and gonorrhoea, Victoria, 2000–2009
 |
|
MSM = men who have sex with men. VPCNSS = Victorian Primary Care Network for Sentinel Surveillance. |
- Carol El-Hayek1
- Isabel Bergeri1
- Margaret E Hellard1
- Alisa E Pedrana1,2
- Nasra Higgins3
- Alan Breschkin4
- Mark Stoové1
- 1 Centre for Population Health, Burnet Institute, Melbourne, VIC.
- 2 Department of Epidemiology and Preventive Medicine, Monash University, Melbourne, VIC.
- 3 Communicable Disease Prevention and Control Unit, Victorian Government Department of Health, Melbourne, VIC.
- 4 Victorian Infectious Diseases Reference Laboratory, Melbourne, VIC.
We would like to acknowledge the ongoing contribution of the surveillance officers at the Burnet Institute and the notifying medical practitioners. Special thanks to the partner notification officers for their important role in the HIV/STI notification process, and to the sentinel sites and laboratories that undertake pathology services for the VCPNSS clinics. We are grateful for the financial support received from the Victorian Department of Health.
The Centre for Population Health at the Burnet Institute is contracted by the Victorian Department of Health to manage HIV passive surveillance (since 1991) and HIV, other STIs and hepatitis C sentinel surveillance (since 2006) in Victoria. Data from these surveillance systems form the basis of our article.
- 1. Guy R, McDonald AM, Bartlett MJ, et al. HIV diagnoses in Australia: diverging epidemics within a low-prevalence country. Med J Aust 2007; 187: 437-440. <MJA full text>
- 2. Guy RJ, McDonald AM, Bartlett MJ, et al. Characteristics of HIV diagnoses in Australia, 1993–2006. Sex Health 2008; 5: 91-96.
- 3. Frankland A, Zablotska I, Prestage G, et al. Gay community periodic survey: Melbourne 2008. Sydney: University of New South Wales, 2008. http://nchsr.arts.unsw.edu.au/media/File/Melbourne2008.pdf (accessed Oct 2010).
- 4. Middleton MG, Grulich AE, McDonald AM, et al. Could sexually transmissible infections be contributing to the increase in HIV infections among men who have sex with men in Australia? Sex Health 2008; 5: 131-140.
- 5. Wilson D, Hoare A, Regan D, et al. Mathematical models to investigate recent trends in HIV notifications among men who have sex with men in Australia. Sydney: University of New South Wales, 2008.
- 6. Ginige S, Chen MY, Hocking JS, et al. Rising HIV notifications in Australia: accounting for the increase in people living with HIV and implications for the HIV transmission rate. Sex Health 2007; 4: 31-33.
- 7. Murray JM, McDonald AM, Law MG. Rapidly ageing HIV epidemic among men who have sex with men in Australia. Sex Health 2009; 6: 83-86.
- 8. Garnett G, Hughes J, Anderson RM, et al. Sexual mixing patterns of patients attending sexually transmitted diseases clinics. Sex Transm Dis 1996; 23: 248-257.
- 9. Prestage G, Jin F, Zablotska I, et al. Trends in HIV testing among homosexual and bisexual men in eastern Australian states. Sex Health 2008; 5: 119-123.
- 10. Prestage G, Kippax S, Jin F, et al. Does age affect sexual behaviour among gay men in Sydney, Melbourne and Brisbane, Australia? AIDS Care 2009; 21: 1098-1105.
- 11. Pedrana A, Stoové M, Guy R, et al. “Suck it and see ...”: estimating HIV prevalence and unrecognised HIV infection among men who have sex with men in Victoria. Melbourne: Burnet Institute, 2009. http://www.burnet.edu.au/freestyler/gui/files//Prevalence%20Study-%20Final%20Report!%20Updated..pdf (accessed Oct 2010).
- 12. Goller J, Gold J, Lim MS, et al. HIV, syphilis and chlamydia in men who have sex with men in Victoria: testing, risk behaviour and prevalence. Victorian Infect Dis Bull 2008; 11: 5-9.
- 13. Wolitski R, Valdiserri R, Denning P, et al. Are we headed for a resurgence of the HIV epidemic among men who have sex with men? Am J Public Health 2001; 91: 883-888.
- 14. Sherrard J, Barlow D. Gonorrhoea in men: clinical and diagnostic aspects. Genitourin Med 1996; 72: 422-426.
- 15. Singh AE, Romanowski B. Syphilis: review with emphasis on clinical, epidemiologic, and some biologic features. Clin Microbiol Rev 1999; 12: 187-209.
- 16. Lightfoot M, Swendeman D, Rotheram-Borus MJ, et al. Risk behaviors of youth living with HIV: pre- and post-HAART. Am J Health Behav 2005; 29: 162-171.





Abstract
Objective: To describe recent trends among men who have sex with men (MSM) in age at diagnosis of HIV in Victoria.
Design and setting: Analysis of Victorian HIV surveillance data from (i) passive surveillance (2000–2009) and (ii) the Victorian Primary Care Network for Sentinel Surveillance (VPCNSS) (2006–2009). Age-trend comparisons were made using syphilis and gonorrhoea enhanced surveillance.
Main outcome measures: HIV diagnoses, HIV testing and behavioural indicators by year and age group among MSM.
Results: Following a period of sustained increase between 2000 and 2007, the median age at HIV diagnosis among MSM declined significantly, from 38.8 years in 2007 to 35.3 years in 2008 (P = 0.023), remaining at 35.9 years in 2009. Between 2007 and 2008, the median age of syphilis and gonorrhoea notifications also declined, from 40.6 to 36.0 years and from 32.3 to 29.3 years, respectively. The median age of HIV testing among MSM in the VPCNSS population remained constant between 2006 and 2009, at 33.0 years. Compared with older MSM, those aged less than 35 years were more likely to have never previously been tested for HIV (relative risk [RR], 1.36 [95% CI, 1.30–1.41]); to not know the HIV status of their regular partner (RR, 1.11 [95% CI, 1.01–1.21]); and to report inconsistent condom use with casual partners (RR, 1.07 [95% CI, 1.01–1.14]) and regular partners (RR, 1.07 [95% CI, 1.00–1.14]).
Conclusions: Younger MSM in Victoria may be at increasing risk of HIV infection. Enhanced methods of monitoring HIV and sexually transmitted infection transmission in younger MSM are needed, as well as prevention messages to target this group, who may not fully understand their HIV risk.