Australia is recognised internationally for an effective response to the HIV epidemic — a response that is evidence-based and conducted through a partnership involving government, non-government organisations, health professionals and the communities most affected, including people living with HIV infection. Regularly published analyses have shown that male-to-male sexual contact has been the major route of transmission of HIV in Australia and that transmission occurs less frequently by other routes.1,2 The incidence of HIV infection was at its highest in the early to mid 1980s,1 and both the prevalence and incidence of HIV infection in Australia are now very low compared with most other countries.3
Despite the apparent successes in Australia’s HIV response, concern has been raised over a recent increase in the annual number of people diagnosed with HIV, following more than a decade of decline. Surveillance reports indicate that there has also been a divergence between Australian states in the trends and patterns of diagnosis.2 These differences in trends have led to debate about the reasons for them, and whether they indicate inconsistencies in the level and effectiveness of response between jurisdictions.
Surveillance procedures for HIV infection in Australia have been described previously.1,2 Briefly, state and territory health authorities report newly diagnosed cases of infection to the National Centre in HIV Epidemiology and Clinical Research. Information sought on each case includes demographic and clinical characteristics (including CD4+ cell count), as well as information on the most likely route of exposure to HIV.
The classification of HIV exposure categories is based on patient self-report, and includes sexual exposure (male-to-male sex or heterosexual contact), history of injecting drug use, and the receipt of blood, blood products or tissue. People who report heterosexual contact are further classified according to whether they or their sexual partners were born in a country with high HIV prevalence (at least 1% in adults),3 or whether they report sexual partners in a behavioural category associated with increased HIV risk.
Per capita rates of HIV diagnosis per 100 000 population, directly standardised to the national population in 10-year age groups, were calculated by state/territory and year using Australian Bureau of Statistics mid-year population estimates.4,5 For diagnoses associated with male-to-male sex, rates per 100 000 male population were also calculated by state/territory. The proportions of the national population reported as Indigenous or overseas-born were obtained from 2001 census data.6,7 Cases newly diagnosed in Australia were analysed by Indigenous status for 1993–2006; in the Australian Capital Territory and Victoria, where routine reporting of Indigenous status at HIV diagnosis began in January 2005 and June 1998, respectively, cases diagnosed since these dates were included.2 Analyses by country of birth were limited to cases newly diagnosed in Australia from 2002, when reporting of country of birth was introduced nationally.
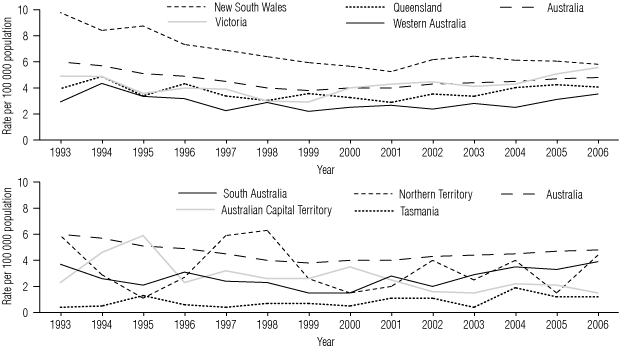
On a per capita basis (Box 1), there was a downward trend in HIV diagnoses in NSW, Victoria, Queensland, WA and SA until around 2000. There then appeared to be a divergence, with rates in NSW stabilising at 5.8 per 100 000 population in 2006, while the other four states increased with a significant trend. Victoria was the first state to show increased rates per 100 000 population, from 2.9 in 1999 to 4.5 in 2002, and by 2006 it had almost equalled NSW, with an annual rate of 5.6 diagnoses per 100 000 population.
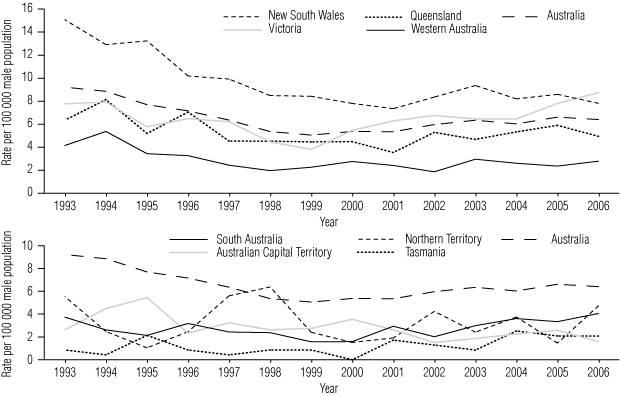
The per capita rate of diagnosis associated with male-to-male sex (per 100 000 male population) in 1993–2006 was 6.5, with the highest rate reported in NSW (9.6), followed by Victoria (6.5) and Queensland (5.3). Similar to the overall per capita rate, there was a significant downward trend in this rate until around 2000; rates then increased in Victoria, Queensland, WA and SA from 2001 onwards, but the trend was only significant in Victoria. By 2006, the rate in Victoria had surpassed NSW (8.7 v 7.8 per 100 000 male population; Box 2).
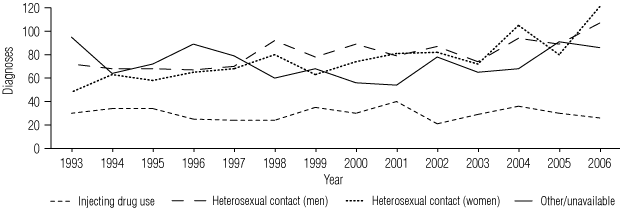
Among the 1134 cases in men reported as heterosexually acquired, 27% were in men born in a high-prevalence country and 26% in men who had a partner from a high-prevalence country. There were 1060 women with heterosexually acquired infection, including 39% from a high-prevalence country, 12% with a partner from a high-prevalence country, and a further 8% who reported a bisexual man as a partner (Box 3). Between 2004 and 2006, the average annual per capita rate of diagnosis associated with heterosexual contact was 0.97 per 100 000 population, with the highest per capita rates in the NT (2.42), followed by WA (1.45) and NSW (1.06). Lower per capita rates of HIV infection attributed to heterosexual contact were reported in Victoria (0.89), SA (0.88), Queensland (0.78), ACT (0.50) and Tasmania (0.21). Although the annual number of diagnoses associated with heterosexual contact increased steadily each year, the trend in the per capita rate of diagnosis was not statistically significant.
Time trends and geographic differences in the rate of reported HIV diagnosis may arise for several reasons. First, diagnosis is dependent on the uptake of testing for HIV infection. Regular surveys of men having male-to-male sex suggest that testing coverage among them is high, with between 50% and 70% of HIV-negative respondents saying that they are tested at least annually.8-10 There has been a small increase over the past few years in the proportion of respondents reporting annual HIV testing8-10 — a finding also seen in this analysis and corresponding to the increasing CD4+ cell counts seen at diagnosis — but these trends show little geographic variation and are therefore unlikely to explain the divergent diagnosis rates between jurisdictions.
Another factor may be the size of subgroups associated with increased risk of HIV transmission. In particular, variations in the population distribution of men having male-to-male sex would be likely to have a strong influence on these rates. Despite the ongoing concentration of gay men in Sydney,11 a national survey conducted in 2001–2002 found that the proportion of male respondents who had a male sex partner in the previous year did not vary considerably across the country.12 There is no information on the extent to which these proportions may vary over time, due to internal migration or other factors.
A third explanation for the geographic differences in HIV diagnosis trends may be divergent trends in sexual risk behaviour. Support for this possibility comes from the Gay Community Periodic Surveys, which recruit repeat cross-sectional samples in several Australian cities. When the surveys began in the late 1990s, participants from Sydney were the most likely to report having had unprotected anal intercourse with casual partners. The next few years saw a steady increase in all cities in the proportion of men reporting this practice, but the Sydney proportion reached a plateau around 2001, while in Brisbane and Melbourne this risk behaviour continued to rise.8-10 These behavioural trends in Australia’s three largest cities essentially match the corresponding state-specific trends in HIV diagnoses reported here.
Many other Western countries have reported recent increases in HIV diagnoses among men having male-to-male sex,13,14 and some have also reported increases in HIV-related risk behaviour in this population.14 These increases have been linked to changing perceptions about the seriousness of HIV infection due to the availability of effective treatments.15 Increases in sexually transmitted infections and the greater numbers of people living with HIV are also crucial determinants of new transmission,13,16 but we have no evidence that these factors are changing in a differential manner across jurisdictions.
Based on a much smaller number of cases, diagnoses related to heterosexual contact have also increased, but the per capita rate remains low and unchanged over time. The coverage of HIV testing among heterosexuals is quite low (about 25% reported a test in 2001–2002, compared with 56% of men with male sexual partners17), so there may be a greater degree of underdiagnosis than in the cases associated with male-to-male sex, but evidence from HIV screening of blood donors and testing in sexual health clinics would appear to confirm low and unchanging prevalence in this group. As in several European countries, many of the heterosexually acquired HIV cases in Australia are linked to countries of high HIV prevalence in Africa and Asia.13,18 Despite having a relatively comprehensive national system for HIV surveillance, Australia could improve the quality and validity of the information it produces. Serological assays are available that can distinguish between newly acquired and established HIV infections; these could be used more widely19-23 to provide a better indication of recent HIV transmission.24 New clinic-based sentinel surveillance systems have been developed in some parts of the country and could be used to provide more comprehensive information about HIV testing and prevalence. Surveillance to monitor the prevalence of drug-resistant strains among new infections could also be considered. Analysis of acute primary HIV infection cases diagnosed at St Vincent’s Hospital in Sydney indicated a substantial drop in the frequency of primary nucleoside analogue reverse transcriptase inhibitor resistance mutations from 29.3% before 1996 to 9.0% after 1996, following the introduction of highly active antiretroviral therapy into the transmitting community.25 Ongoing monitoring is required to detect changes in the prevalence and characteristics of transmitted resistance.
Received 6 June 2007, accepted 9 July 2007
- Rebecca J Guy1,2
- Ann M McDonald3
- Mark J Bartlett4
- Jo C Murray5
- Carolien M Giele6
- Therese M Davey7
- Ranil D Appuhamy8
- Peter Knibbs9
- David Coleman10
- Margaret E Hellard1
- Andrew E Grulich3
- John M Kaldor3
- 1 Centre for Epidemiology and Population Health Research, Burnet Institute, Melbourne, VIC.
- 2 Department of Epidemiology and Preventive Medicine, Monash University, Melbourne, VIC.
- 3 National Centre in HIV Epidemiology and Clinical Research, University of New South Wales, Sydney, NSW.
- 4 Communicable Diseases Branch, NSW Health Department, Sydney, NSW.
- 5 AIDS Medical Unit, Queensland Health, Brisbane, QLD.
- 6 Epidemiology and Surveillance Program, Communicable Disease Control Directorate, Department of Health, Perth, WA.
- 7 STD Services, Royal Adelaide Hospital, Adelaide, SA.
- 8 Health Protection Service, ACT Health, Canberra, ACT.
- 9 Sexual Health and Blood Borne Viruses Unit, Centre for Disease Control, Darwin, NT.
- 10 Communicable Diseases Prevention Unit, Department of Health and Human Services, Hobart, TAS.
The National Centre in HIV Epidemiology and Clinical Research (NCHECR) is funded by the Australian Government Department of Health and Ageing, and is affiliated with the Faculty of Medicine, University of New South Wales. The NCHECR Surveillance Program is a collaborating unit of the Australian Institute of Health and Welfare. Its work is overseen by the Ministerial Advisory Committee on AIDS, Sexual Health and Hepatitis.
None identified.
- 1. McDonald AM, Crofts N, Blumer CE, et al. The pattern of diagnosed HIV infection in Australia, 1984–1992. AIDS 1994; 8: 513-519.
- 2. National Centre in HIV Epidemiology and Clinical Research. HIV/AIDS, viral hepatitis and sexually transmissible infections in Australia. Annual Surveillance Report 2006. Sydney: NCHECR; Canberra: Australian Institute of Health and Welfare, 2006. http://web.med.unsw.edu.au/nchecr/Downloads/06_ansurvrp.pdf (accessed May 2007).
- 3. Joint United Nations Programme on HIV/AIDS (UNAIDS). 2006 Report on the global AIDS epidemic. Geneva: UNAIDS, 2006. http://www.unaids.org/en/HIV_data/2006GlobalReport/default.asp (accessed May 2007).
- 4. Australian Bureau of Statistics. Australian demographic statistics. Canberra: ABS, 2006 (ABS Cat. No. 3101.0.)
- 5. Australian Bureau of Statistics. Population by age and sex, Australian states and territories. Canberra: ABS, 2006. (ABS Cat. No. 3201.0.)
- 6. Australian Bureau of Statistics. Australian historical population statistics, 2001. Canberra: ABS, 2001. (ABS Cat. No. 3105.0.65.001.)
- 7. Australian Bureau of Statistics. Population characteristics, Aboriginal and Torres Strait Islander Australians, 2001. Canberra: ABS, 2001. (ABS Cat. No. 4713.0.)
- 8. Hull P, Prestage G, Zablotska I, et al. Gay Community Periodic Survey, Melbourne 2006. Sydney: National Centre in HIV Social Research, University of New South Wales, 2006. http://nchsr.arts.unsw.edu.au/pdf%20reports/Melbourne2006.pdf (accessed May 2007).
- 9. Zablotska I, Prestage G, Hull P, et al. Sydney Gay Community Periodic Survey 1996–2006. Sydney: National Centre in HIV Social Research, University of New South Wales, 2006. http://nchsr.arts.unsw.edu.au/pdf%20reports/sydney_gcps_feb2006.pdf (accessed May 2007).
- 10. Zablotska I, Prestage G, Imrie J, et al. Gay Community Periodic Survey, Queensland 2006. Sydney: National Centre in HIV Social Research, University of New South Wales, 2006. http://nchsr.arts.unsw.edu.au/pdf%20reports/QLD_GCPS_2006.pdf (accessed May 2007).
- 11. Madeddu D, Grulich A, Richters J, et al. Estimating population distribution and HIV prevalence among homosexual and bisexual men. Sex Health 2006; 3: 37-43.
- 12. Australian Research Centre in Sex, Health & Society, La Trobe University. Australian Study of Health and Relationships, 2001–2002 [computer file]. Canberra: Australian Social Science Data Archive, Australian National University, 2005.
- 13. Hamers FF, Downs AM. The changing face of the HIV epidemic in western Europe: what are the implications for public health policies? Lancet 2004; 364: 83-94.
- 14. Centers for Disease Control and Prevention (CDC). Trends in HIV/AIDS diagnoses — 33 states, 2001–2004. MMWR Morb Mortal Wkly Rep 2005; 54: 1149-1153.
- 15. Elford J, Bolding G, Maguire M, Sherr L. Combination therapies for HIV and sexual risk behavior among gay men. J Acquir Immune Defic Syndr 2000; 23: 266-271.
- 16. Ginige S, Chen MY, Hocking JS, et al. Rising HIV notifications in Australia: accounting for the increase in people living with HIV and implications for the HIV transmission rate. Sex Health 2007; 4: 31-33.
- 17. Grulich AE, de Visser RO, Smith AM, et al. Sex in Australia: sexually transmissible infection and blood-borne virus history in a representative sample of adults. Aust N Z J Public Health 2003; 27: 234-241.
- 18. Brown AE, Sadler KE, Tomkins SE, et al. Recent trends in HIV and other STIs in the United Kingdom: data to the end of 2002. Sex Transm Infect 2004; 80: 159-166.
- 19. Centers for Disease Control and Prevention (CDC). HIV incidence among young men who have sex with men — seven US cities, 1994–2000. MMWR Morb Mortal Wkly Rep 2001; 50: 440-444.
- 20. Guy RJ, Breschkin AM, Keenan CM, et al. Improving HIV surveillance in Victoria: the role of the “detuned” enzyme immunoassay. J Acquir Immune Defic Syndr 2005; 38: 495-499.
- 21. McDonald A, Cunningham P, Kelleher A, Kaldor J. Comparison of two assays for identifying incident infection among cases of newly diagnosed HIV infection. STARHS Symposium, 16th International Conference on AIDS; 2006 Aug 12; Toronto, Canada. http://www.ohtn.on.ca/pdf/starhs/Microsoft% 20PowerPoint%20-%20101%20detunevsbed.pdf (accessed May 2007).
- 22. Parekh BS, Hu DJ, Vanichseni S, et al. Evaluation of a sensitive/less-sensitive testing algorithm using the 3A11-LS assay for detecting recent HIV seroconversion among individuals with HIV-1 subtype B or E infection in Thailand. AIDS Res Hum Retroviruses 2001; 17: 453-458.
- 23. Rehle T, Shisana O, Pillay V, et al. National HIV incidence measures — new insights into the South African epidemic. S Afr Med J 2007; 97: 194-199.
- 24. Rutherford GW, Schwarcz SK, McFarland W. Surveillance for incident HIV infection: new technology and new opportunities. J Acquir Immune Defic Syndr 2000; 25 Suppl 2: S115-S119.
- 25. Ammaranond P, Cunningham P, Oelrichs R, et al. No increase in protease resistance and a decrease in reverse transcriptase resistance mutations in primary HIV-1 infection: 1992–2001. AIDS 2003; 17: 264-267.





Abstract
Objective:
Design and setting: Analysis of national surveillance system data for 1993–2006.
Main outcome measures: Number and population rate of new HIV diagnoses by year, exposure route and demographic characteristics.
Results: Between 1993 and 2006, 12 313 new diagnoses of HIV infection were reported in Australia. From 1993 to 1999, the annual number of diagnoses declined by 32% from 1056 to 718, and then increased by 31% from 763 in 2000 to 998 in 2006. Between 2000 and 2006, diagnosis rates significantly increased in Victoria, Queensland, South Australia and Western Australia. The most frequent route of HIV exposure was male-to-male sex, accounting for 70% of diagnoses. Heterosexual contact accounted for 18% of cases, with just over half of these people born in or having a sexual partner from a high-prevalence country. Exposure by injecting drug use remained infrequent.
Conclusions: The number of HIV diagnoses has risen in the past 7 years, but not in New South Wales, which has long had the highest rates. The differences in rates between states/territories are likely to be due to divergent trends in sexual risk behaviour in men having male-to-male sex, which remains the predominant route of HIV transmission in Australia. There is a need for effective, innovative and evidence-based programs for HIV prevention, particularly among men having male-to-male sex.