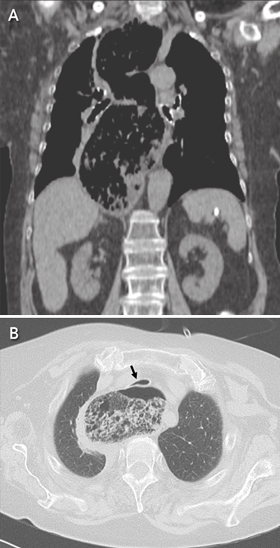
A 79-year-old woman was admitted with shortness of breath that had worsened over the previous week. Two months earlier, she had developed dysphagia with nocturnal regurgitation, cough and occasional stridor. Physical examination showed no abnormalities apart from an oxygen saturation level of 85% on room air. The patient had a history of achalasia, which had been treated 5 years earlier with pneumatic dilation.
A chest computed tomography scan showed a severely dilated and tortuous oesophagus with retained food (Figure, A) causing compression of the trachea (Figure, B). The woman was successfully treated with laparoscopic Heller myotomy and discharged.
- Nicola Mumoli1
- Department of Internal Medicine, Livorno Hospital, Livorno, Italy.
Correspondence: nimumoli@tiscali.it
Online responses are no longer available. Please refer to our instructions for authors page for more information.