Since the ANZAC day weekend, when many Australians first learnt about a novel strain of influenza circulating in Mexico and the United States, there have been differing views among health professionals, politicians and the public about how we should have reacted to the influenza pandemic of 2009, officially known as pandemic (H1N1) 2009 influenza and still widely referred to as swine flu. Questions that arose related to the seriousness of pandemic (H1N1) 2009 influenza in comparison with other seasonal strains of influenza, and the best ways to manage the pandemic. One Victorian general practitioner wondered if we were lucky with our approach to the pandemic because the virus was relatively mild.1 As the pandemic wanes, we are in a position to explore some of these issues.
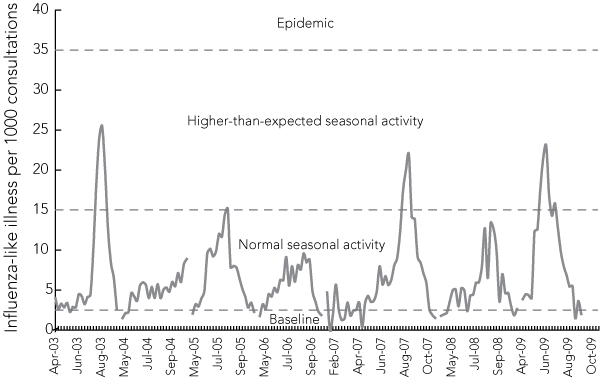
Unlike countries in the northern hemisphere, Australia experienced the swine flu outbreak when seasonal influenza circulation was expected. Victoria was the first Australian state to report a significant number of cases2 and the first Australian state to record the peak of the epidemic.3 This occurred around the end of June, as shown by the proportion of people presenting to sentinel GPs with an influenza-like illness (Box 1). The peak was similar to peaks recorded for seasonal influenza in 2003 and 2007, but the 2009 peak may have been inflated by an increased level of presentation to GPs. Worried about swine flu, people with an illness that they thought may have been influenza presented to their GP in 2009, when they might have stayed home in any other year. If this were the case, the proportion of influenza-like illness in sentinel patients may not be the most informative comparison.
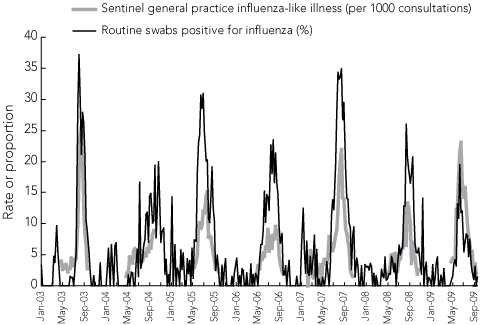
We, therefore, examined the proportion of requested laboratory tests that were positive for influenza between 2004 and 2009, a metric that corrects for increased testing associated with higher numbers of diagnostic requests for possible influenza, not necessarily associated with higher levels of influenza circulation. We compared influenza-like illness rates with the proportion of positive tests (Box 2). Confirming our previous surveillance findings that the rate of circulation of influenza virus was relatively high in 2003 and 2007,4,5 the proportion of positive tests was also highest in those 2 years. This is consistent with the positive predictive value of a test (the proportion of positive tests) increasing with the prevalence of disease (the influenza-like illness rate). However, the proportion of tests positive in 2009, when swine flu was the dominant circulating strain, was about the same as the proportions in 2004 and 2006, years known to be characterised by relatively low influenza activity (Box 2). Increased rates of presentation and testing may mean that this comparison is also biased.
The manifestation of swine flu infection, acknowledged to be most often mild, ranges from undiagnosed asymptomatic infection to serious illness and death. For seasonal influenza, the proportion of asymptomatic infection is between 25% and 33%,6,7 and 63% of people volunteering to be infected with seasonal H1N1 influenza experimentally do not have a fever.6 These proportions may also apply to pandemic (H1N1) 2009 influenza. Representatives from the World Health Organization now admit that we have no idea how many people have been, or will be, infected with swine flu.8 This estimate is as uncertain as is the estimate of the proportion of the world’s population affected in any influenza season.
On 3 June 2009, Victoria moved to a “Modified Sustain” phase of pandemic control,9 after which attempts to capture every case of pandemic (H1N1) 2009 influenza ceased. At this stage, 978 cases had been diagnosed in Victoria and individually followed up.10 However, sentinel surveillance indicated that the pandemic did not peak until more than 3 weeks later, so we have no estimate of the total number of cases that may have been diagnosed in Victoria if the approach to case ascertainment had not changed. Reported cases in Victoria by 23 September were 3052.9 This number does not include any asymptomatic cases or people who did not present for medical attention. Identification of asymptomatic cases requires well-designed serosurveys, and a number of these are planned.
The pandemic paradox is that, while disease in the community appears to be mild, and the risk of hospitalisation low (reported as 0.3% for the first 10 weeks of the pandemic in Victoria11), 20% of hospitalised patients required intensive care.11 People with underlying respiratory, cardiovascular and other chronic diseases are known to have worse outcomes from influenza infection, and this has been evident with confirmed swine flu infections.11 However, with swine flu we also see a high rate of serious disease among pregnant women2,11,12 and people who are very overweight.11,13 While there is continued discussion about whether obesity is an independent risk factor for severe outcome, or whether it is a feature of other known risk factors, such as type 2 diabetes, anecdotal reports indicate that obese patients are occupying a disproportionate amount of time in intensive care beds.14,15 There appears to be less doubt about the increased risk to pregnant women.
Up to 7 August 2009, 74 of the 2052 Australian patients hospitalised with confirmed pandemic (H1N1) 2009 influenza infection (4%) were pregnant.2 We used the approach of a United States study to estimate the number of pregnant women in Australia.12 Australia’s population in 2008 was estimated at 21 373 998, of whom 4 492 701 were women aged 15–44 years — the accepted reproductive age range.16 The number of live births in 2008 was 296 610,17 giving a fertility rate of 66.0 per 1000 women of reproductive age (296 610/4 492 701 × 1000). An abortion rate of about 20 per 1000 women of reproductive age has been reported for Australia in 2003 (admitted by the authors to be unreliable, but the best available estimate).18 Adding 9/12 of the fertility rate (a pregnancy resulting in a live birth lasts for an average of 9 months) to 2/12 of the abortion rate (a pregnancy resulting in an abortion lasts for an average of 2 months) gives an estimate of the pregnancy rate of 52.8 per 1000 women of reproductive age. Multiplying this rate by the number of women of reproductive age gives 237 215, an estimate of the number of pregnant women in Australia. This represents about 1.1% of the population, the same proportion as estimated for the US.12
Although case numbers are high, and there are problems in intensive care units, the number of deaths from swine flu may not be as high as the numbers modelled to die from seasonal influenza. In Victoria, as the pandemic appears to have waned, 24 deaths from pandemic (H1N1) 2009 influenza were recorded by 23 September 2009.9 We don’t know the numbers who die from seasonal influenza each year because we don’t test for seasonal influenza with the same enthusiasm that we have tested for swine flu. However, a comparison based on modelling estimates that about 3000 people aged at least 50 years will die from seasonal influenza each year in Australia.19 In Victoria, this might equate to 750 people — considerably higher than the number of swine flu deaths to date.
Complicating the comparison, however, is the observation that deaths from seasonal influenza and swine flu occur in different age groups. Modelling suggests that 85%–90% of deaths from seasonal influenza occur in people aged at least 65 years,19 while the median age of people who died from swine flu to 21 August 2009 in Australia is 54 years.2
What lessons can we learn from the pandemic experience? Although time consuming and expensive to collect, we could assemble quality data on the basic epidemiology of laboratory-confirmed influenza over sequential influenza seasons in different age and risk groups (Box 3). This is feasible with the advent of molecular diagnostic technology. Understanding the laboratory-confirmed burden of disease would also allow better understanding of the effectiveness and cost-effectiveness of interventions used to control influenza. If quality information about influenza disease burden had been available in 2009, we and others around Australia, and the world, may have been able to make sensible comparisons between seasonal and pandemic influenza. We may not then have needed a pandemic response to a disease that, although it has a different footprint, has been predominantly of seasonal intensity.
1 Proportion of influenza-like illness presentations per 1000 consultations in Victorian sentinel general practices, 2003–2009
2 Comparison of the rate of tests positive for influenza from routine diagnostic testing at the Victorian Infectious Diseases Reference Laboratory and the proportion of influenza-like illness per 1000 consultations in Victorian sentinel general practices, 2003–2009
3 Strategies for monitoring and studying influenza to assess laboratory-confirmed disease burden
Implement a representative national influenza-like illness surveillance network with laboratory support. Current networks are not representative and laboratory support is piecemeal. Such a network can be used to estimate vaccine effectiveness on an annual basis.20
Determine a reliable estimate of the annual community attack rate. Using the national influenza-like illness surveillance network, develop a national study protocol to determine the relationship between the proportion of patients with laboratory-confirmed influenza and the proportion of the community infected with influenza. The symptomatic attack rate for pandemic influenza in New Zealand has been estimated as 7.5%.21
Develop a routine surveillance network in sentinel paediatric and adult hospitals. This would involve routine sample collection to detect influenza and other respiratory viruses from children with any respiratory symptoms presenting to the emergency department or admitted to hospital. Sample collection from adult patients may need to include a wider range of illnesses, at least including presentations for respiratory and cardiovascular disease.
Develop a national protocol to confirm the risk of influenza infection in pregnant women and confirm that vaccination of pregnant women protects their newborn.22
- Heath A Kelly1
- Epidemiology Unit, Victorian Infectious Diseases Reference Laboratory, Melbourne, VIC.
I thank Kristina Grant for preparing the figures and helping with the manuscript, and Dr Geoff Mercer from the Australian National University for assistance with the calculation of the risk of hospitalisation in pregnancy.
None identified.
- 1. Eizenberg P. The general practice experience of the swine flu epidemic in Victoria — lessons from the front line. Med J Aust 2009; 191: 151-153. <MJA full text>
- 2. Australian Government Department of Health and Ageing. Australian influenza report 2009 — current report — 5 to 11 September 2009. http://www.health.gov.au/internet/main/publishing.nsf/Content/cda-surveil-ozflu-flucurr.htm (accessed Oct 2009).
- 3. Victorian Infectious Diseases References Laboratory. Sentinel influenza surveillance 2009. http://www.vidrl.org.au/surveillance/flu%20reports/flurpt09/flu09.html (accessed Oct 2009).
- 4. Turner J, Tran T, Birch C, et al. Higher than normal seasonal influenza activity in Victoria, 2003. Commun Dis Intell 2004; 28: 175-180.
- 5. Miller ER, Fielding JE, Grant KA, et al. Higher than expected seasonal influenza activity in Victoria, 2007. Commun Dis Intell 2008; 32: 63-70.
- 6. Carrat F, Vergu E, Ferguson NM, et al. Time lines of infection and disease in human influenza: a review of volunteer challenge studies. Am J Epidemiol 2008; 167: 775-785.
- 7. Cowling BJ, Fang VJ, Riley S, et al. Estimation of the serial interval of influenza. Epidemiology 2009; 20: 344-347.
- 8. World Health Organization. Changes in reporting requirements for pandemic (H1N1) 2009 virus infection. Pandemic (H1N1) 2009 briefing note 3 (revised). http://www.who.int/csr/disease/swineflu/notes/h1n1_surveillance_20090710/en/ (accessed Oct 2009).
- 9. Department of Health State Government of Victoria. H1N1 influenza 09 (human swine flu) http://humanswineflu.health.vic.gov.au/ (accessed Oct 2009).
- 10. Fielding JE, Higgins N, Gregory JE, et al. Pandemic H1N1 influenza surveillance in Victoria, Australia, April – September, 2009. Euro Surveill 2009; 14: pii=19368. http://www.eurosurveillance.org/ViewArticle.aspx?ArticleId=19368 (accessed Nov 2009).
- 11. Lum ME, McMillan AJ, Brook CW, et al. Impact of pandemic (H1N1) 2009 influenza on critical care capacity in Victoria. Med J Aust 2009; 191: 502-506. <MJA full text>
- 12. Jamieson DJ, Honein MA, Rasmussen SA, et al. H1N1 2009 influenza virus infection during pregnancy in the USA. Lancet 2009; 374: 451-458.
- 13. Hospitalized patients with novel influenza A (H1N1) virus infection — California, April–May, 2009. MMWR Morb Mortal Wkly Rep 2009; 58: 536-541.
- 14. Gale J. Swine flu packs bigger jolt for obese as “striking” link found. Bloomberg.com 2009; 10 Jul. http://www.bloomberg.com/apps/news?pid=newsarchive&sid=aPUbdh6sLlb0 (accessed Oct 2009).
- 15. Sweet M. Pandemic lessons from Australia. BMJ 2009; 339: b3317.
- 16. Australian Bureau of Statistics. Population by age and sex, Australian states and territories, Jun 2008. Data cube: population by age and sex (32010Do001_200806.xls). Canberra: ABS, 2008. (ABS Cat. No. 3201.0.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/3201.0Jun%202008?OpenDocument (accessed Oct 2009).
- 17. Australian Bureau of Statistics. Australian demographic statistics, Dec 2008. Data cube: Australian demographic statistics (31010Do001_200812.xls). Canberra: ABS, 2008. (ABS Cat. No. 3101.0.) http://www.abs. gov.au/AUSSTATS/abs@.nsf/DetailsPage/3101.0Dec%202008?OpenDocument (accessed Oct 2009).
- 18. Chan A, Sage LC. Estimating Australia’s abortion rates 1985–2003. Med J Aust 2005; 182: 447-452. <MJA full text>
- 19. Newall AT, Wood JG, Macintyre CR. Influenza-related hospitalisation and death in Australians aged 50 years and older. Vaccine 2008; 26: 2135-2141.
- 20. Kelly H, Carville K, Grant K, et al. Estimation of influenza vaccine effectiveness from routine surveillance data. PLoS One 2009; 4: e5079.
- 21. Baker MG, Wilson N, Huang QS, et al. Pandemic influenza A(H1N1)v in New Zealand: the experience from April to August 2009. Euro Surveill 2009; 14: pii 19319.
- 22. Zaman K, Roy E, Arifeen SE, et al. Effectiveness of maternal influenza immunization in mothers and infants. N Engl J Med 2008; 359: 1555-1564.





Abstract
The Victorian experience suggests that the circulation of pandemic (H1N1) 2009 influenza in the community was at most like influenza circulation in a season of moderate seasonal activity.
We have no estimate of the total case count, but we know most infections have been mild. However, while disease in the community appears mild, and the risk of hospitalisation is low, a high proportion of patients hospitalised with swine flu required intensive care.
Deaths from swine flu have not been as numerous as the modelled deaths from seasonal influenza, although people dying from swine flu are younger.
Because we do not understand the laboratory-confirmed burden of disease due to seasonal influenza (as opposed to the modelled burden of disease), we could not base our response to the pandemic on an informed comparison of seasonal and pandemic influenza.
We may not have needed a pandemic response to a disease that, although it has a different footprint, has been predominantly of seasonal intensity.
It is critical to accumulate quality evidence about laboratory-confirmed influenza to guide our intervention policies for both seasonal and pandemic influenza.