Following the emergence of the novel H1N1 influenza 09 (human swine flu), global surveillance of the spread and epidemiology of this virus has been high. The establishment of local infection was recognised in Victoria in late May, which coincided with the beginning of the winter seasonal influenza period, and prompted the shift in Australian pandemic phases from the “Delay” Phase to the “Contain” Phase on 22 May 2009.1 Intensive public health measures to identify and confirm all cases of pandemic (H1N1) 2009 influenza during this phase provided baseline data to inform the ongoing assessment of the impact of the pandemic on the acute care health system.
A review of available data sources for influenza surveillance in Victoria had previously identified that existing mechanisms for surveillance through hospitals would not be sufficiently timely for operational purposes during a pandemic.2 Before the commencement of the Contain Phase, three parameters were identified for daily reporting by hospitals to the Victorian Health Emergency Coordination (VHEC) of the Victorian Department of Human Services (DHS). These were: (i) the number of emergency department presentations compared with usual daily demand; (ii) hospitalisation of patients with laboratory-confirmed H1N1 infection; and (iii) transfer to an intensive care unit (ICU) of patients with confirmed H1N1 infection. A secure website was established for daily hospital reporting. These data were used for prospective forecasting and assessment of the impact of the H1N1 pandemic on hospitals using modelling tools.
On 3 June 2009, the pandemic phase was changed to “Modified Sustain”, with the recognition that sustained community transmission was occurring in Victoria.3 Community diversion influenza clinics were established to mitigate high volumes of presentations to emergency departments and hospitals. The World Health Organization declared a global pandemic on 11 June 2009, and Australia moved to a “Protect” Phase on 23 June, which shifted the focus to testing, treatment and prophylaxis for vulnerable groups.4 This phase reduced the requirements for laboratory testing at the community level, but hospitalised patients continued to receive intensive surveillance.
Forecasting and assessment of the impact of the H1N1 influenza 2009 pandemic on hospitals was achieved through use of the two modelling tools; FluSurge 2.0 and FluAid 2.0, developed by the United States Centers for Disease Control and Prevention (CDC).5 FluSurge estimates the surge in demand over time for hospital-based services, whereas FluAid provides a range of estimates of impact in terms of deaths, hospital admissions, and outpatient presentations due to pandemic influenza. As inputs into the FluAid 2.0 model, we used the default FluAid 2.0 estimates of outpatient presentations per 1000 population. These were US national estimates of outpatient presentation rates from influenza per 1000 population by age and risk group, based on the definition of groups at high risk for complications of influenza infection as determined by the CDC’s Advisory Committee on Immunization Practices (ACIP).6,7 These high-risk groups are:
People aged 65 years or older;
Residents of nursing homes or other chronic care facilities that house people with chronic medical conditions;
Adults and children who have chronic disorders of the pulmonary or cardiovascular systems, including those with asthma;
Adults and children who require regular medical follow-up or hospital admission because of chronic metabolic diseases (including diabetes mellitus), renal dysfunction, haemoglobinopathies, or immunosuppression (including immunosuppression caused by medications);
Children and teenagers (aged 6 months to 18 years) receiving long-term aspirin therapy, and who might therefore be at risk of Reye syndrome after influenza infection; and
Women who will be in the second or third trimester of pregnancy during the influenza season.
5% for minimum (or “best-case” scenario), which estimates the fewest possible number of outpatient presentations;
10% for mean (or “most likely” scenario), which estimates the number of outpatient presentations most likely to occur; and
20% for maximum (or “worst-case” scenario), which estimates the largest number of outpatient presentations.
Hospital admission numbers were modelled over 12 weeks as being between 0.1% and 0.5% (in 0.1% increments) of estimated outpatient presentations during this period. Transfers to ICUs were modelled as 20% of hospital admissions (Box 1). Data from daily hospital reports were applied to the model to assist with health service planning by the VHEC. Estimated hospital presentations from the FluAid 2.0 model, using 5%, 10% and 20% clinical attack rates, were compared with the observed hospital presentations. Additional data from specially established community diversion influenza clinics contributed to monitoring and modelling of the hospital impact.
Although the clinical attack rate was unknown at the outset of the pandemic, the Contain Phase provided comprehensive data for hospital presentations and laboratory confirmed cases of pandemic (H1N1) 2009 influenza. The observed number of hospital admissions for H1N1 infection (433 on 31 July 2009) was broadly consistent with the estimate from the FluAid 2.0 model for a 5% gross clinical attack rate, with an estimated 143 740 outpatient presentations, and 0.3% of these being hospitalised (410 on 31 July 2009) (Box 2).
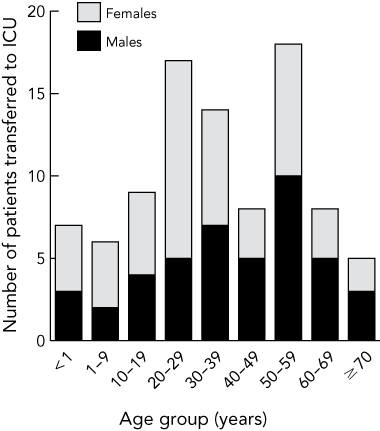
While the epidemiological profile of community infection in Victoria describes a relatively young age group susceptible to H1N1 infection (median age, 21 years),8 the 92 patients with severe disease and who were admitted to an ICU were older (median age, 37 years). These patients reflected the vulnerable population with pre-existing medical conditions and risk factors (Box 3). Due to the elevated risk of serious infection during pregnancy, a bimodal age distribution was observed, with peak incidence occurring in the 20–29-years and 50–59-years age groups (Box 4). Sex differences were only apparent in the 20–29-years age group where the excess proportion of women was the result of the pregnant cohort.
The 10th week of the pandemic in Victoria (FluAid 2.0 model, week ending 29 July) showed a postpeak decline in presentations. The cumulative total for hospital admissions numbered 433 patients, of whom 92 (21%) had been treated in an ICU. This rate of hospital-based care was consistent with the modelled 5% clinical attack rate among the general population, suggesting a stable and relatively mild virulence. Notwithstanding that H1N1 influenza was a mild disease for most of the community, severe disease among vulnerable populations confirmed the early initial observations highlighting the risk of life-threatening respiratory failure.9 Fewer than 10% of patients requiring intensive care management had no identified risk factor (Box 3).
The clinical attack rate refers to the number of people infected with pandemic (H1N1) 2009 influenza who needed any form of clinical assessment or care. The 5% clinical attack rate observed in Victoria is well below the level assumed in the Australian Health Management Plan for Pandemic Influenza.10 This reflects the mild nature of the disease at present. The community attack rate is likely to have been much higher, with most cases being subclinical or minimally symptomatic. Evidence from a serological survey to determine the community attack rates will be needed as soon as is practicable. The estimates of the number of cases presenting for care are broadly consistent with the experience of general practitioners and influenza clinics, but the lack of clinical reporting from primary care, beyond sentinel surveillance in Australia, is an obstacle that needs to be removed to improve health intelligence objectives. Epidemiology of the outbreak in the community from the sentinel surveillance scheme and other sources will be described elsewhere.
Implementation of community-based diversion clinics for influenza was consistent with the observed low clinical attack rate and moderate virulence. Detailed analysis of influenza clinic performance will also be described elsewhere. Peak demand in emergency department presentations was relatively brief in areas where diversion clinics were operating. These clinics progressively closed once demand declined, and were no longer required by the end of the 6th week (week ending 3 July). Monitoring of ICU demand through the VHEC function of the DHS provided the capacity for system-wide response and rational distribution of resources, and helped critical care clinicians communicate and share experiences as the pandemic unfolded.11
1 Observed weekly numbers of pandemic (H1N1) 2009 influenza-related hospital admissions and intensive care unit (ICU) transfers in Victoria, compared with estimated weekly numbers based on a 5% clinical attack rate, and a 0.3% hospital admission rate
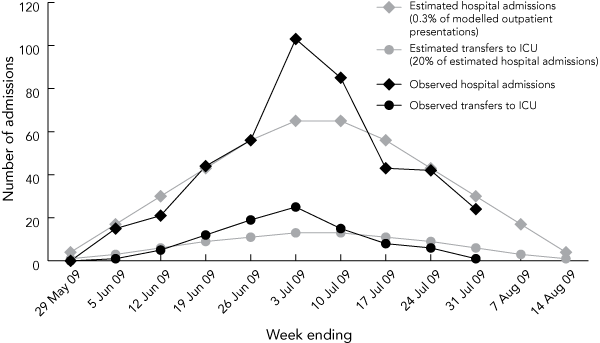
2 Observed cumulative number of hospital admissions, compared with projected admission numbers based on 0.2%, 0.3% and 0.4% of estimated outpatient presentations
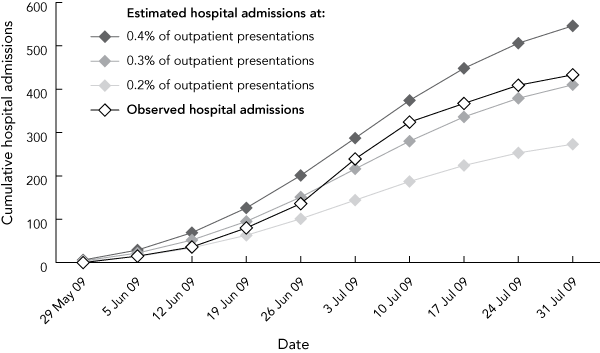
- Martin E Lum1
- Alison J McMillan2
- Chris W Brook3
- Rosemary Lester4
- Leonard S Piers5
- State Government of Victoria, Department of Health, Melbourne, VIC.
We thank the following State Government of Victoria, Department of Human Services staff: Zoe Theodore, Funding and Health Information Policy Branch, and Catherine Lineham, Access and Metropolitan Performance Branch for collating daily hospital demand reports; James Fielding and Joy Gregory, Communicable Disease Prevention and Control Unit for assisting with verification of cases of notified disease; and Alison Markwick, Health Intelligence Unit, for help with epidemiological modelling.
None identified.
- 1. State Government of Victoria, Department of Human Services. Victorian health management plan for pandemic influenza. July 2007. Melbourne: DHS, 2007. http://www.health.vic.gov. au/__data/assets/pdf_file/0017/54503/Victorian_health_management_plan_for_pandemic_influenza.pdf (accessed Aug 2009).
- 2. Clothier HJ, Atkin L, Turner J, et al. A comparison of data sources for the surveillance of seasonal and pandemic influenza in Victoria. Commun Dis Intell 2006; 30: 345-349.
- 3. State Government of Victoria, Department of Human Services. Victoria moves to modified sustain phase of flu plan [media release]. Melbourne: DHS, 2009; 3 Jun. http://humanswineflu.health.vic.gov.au/downloads/media/media-release030609.pdf (accessed Sep 2009).
- 4. Australian Government Department of Health and Ageing. Protect phase. Annex to the Australian Health Management Plan For Pandemic Influenza. Version 2.0. Canberra: DoHA, 2009; 8 Jul. http://www.healthemergency.gov.au/internet/healthemergency/publishing.nsf/Content/resources/$File/AHMPPI-PROTECTannex.pdf (accessed Sep 2009).
- 5. United States Government Department of Health and Human Services, Centers for Disease Control and Prevention. Pandemic influenza resources. Pandemic influenza preparedness tools for professionals. http://www.cdc.gov/flu/pandemic/preparednesstools.htm (accessed Sep 2009).
- 6. Meltzer MI, Cox NJ, Fukuda K. The economic impact of pandemic influenza in the United States: implications for setting priorities for intervention. Emerg Infect Dis 1999; 5: 659-671.
- 7. Meltzer MI, Cox NJ, Fukuda K. Modeling the economic impact of pandemic influenza in the United States: Implications for setting priorities for intervention. Atlanta, Ga: Centers for Disease Control and Prevention, 1999; 30 Apr. http://www.cdc.gov/ncidod/eid/vol5no5/melt_back.htm (accessed Sep 2009).
- 8. Kelly HA, Grant KA, Williams S, et al. Epidemiological characteristics of pandemic influenza H1N1 2009 and seasonal influenza infection. Med J Aust 2009; 191: 146-149. <MJA full text>
- 9. Kaufman MA, Duke GJ, McGain F, et al. Life-threatening respiratory failure from H1N1 influenza 09 (human swine influenza). Med J Aust 2009; 191: 154-156. <MJA full text>
- 10. Australian Government Department of Health and Ageing. Pandemic influenza. Australian Health Management Plan for Pandemic Influenza 2008. http://www.flupandemic.gov.au/internet/panflu/publishing.nsf/Content/ahmppi (accessed Sep 2009).
- 11. State Government of Victoria, Department of Human Services. Victorian health emergency coordination. Information for health services. Melbourne: DHS, 2008; 11 Apr. http://www.dhs.vic.gov.au/__data/assets/pdf_file/0011/191684/vhec_info_for_health_services_april_2008V3.pdf (accessed Sep 2009).





Abstract
Objective:
Design and setting: Prospective modelling with the tools FluSurge 2.0 and FluAid 2.0 (developed by the United States Centers for Disease Control and Prevention) over 12 weeks from when the pandemic “Contain” Phase was declared on 22 May 2009, compared with data obtained from daily hospital reports of pandemic (H1N1) 2009 influenza-related admissions and transfers to intensive care units (ICUs).
Main outcome measures: The effect on hospitals as projected by the FluAid 2.0 model compared with observed hospital admissions and ICU admissions.
Results: Prospective use of the FluAid 2.0 model provided valuable health intelligence for assessment and projection of hospitalisation and critical care demand through the first 10 weeks of the pandemic in Victoria. The observed rate of hospital admissions for pandemic (H1N1) 2009 was broadly consistent with a 5% gross clinical attack rate, with 0.3% of infected patients being hospitalised. Transfers to ICUs occurred at a rate of 20% of hospital admissions, and were associated with vulnerable patient groups, and severe respiratory failure in 82% of patients admitted to ICUs. Most patients treated in ICUs (85%) survived after an average ICU length of stay of 9 days (SD, 6.5 days). Mechanical ventilation was required by 72% of patients admitted to ICUs, and extracorporeal membrane oxygenation (ECMO) was used for 7%. Pre-existing haematological malignancy accounted for half of all the deaths in patients admitted to ICUs with pandemic (H1N1) 2009 influenza.
Conclusions: Prospective use of modelling tools informed critical decisions in the planning and management of the pandemic. Early estimation of the clinical attack rate, hospitalisation rates, and demand for ICU beds guided implementation of surge capacity. ECMO emerged as an important treatment modality for pandemic (H1N1) 2009 influenza, and will be an important consideration for future pandemic planning.