In Australia, each year from 1999 until 2006 inclusive, at least 6000 people were detained in immigration detention centres under the Migration Act 1958 (Cwlth).1 Most were held in detention centres across Australia, and a small number were in offshore detention centres (Christmas Island, Manus Island [Papua New Guinea] and Nauru). All these centres, and the health services provided by them, were managed by private organisations under contract. They employed general practitioners, medical specialists, and nursing and allied health staff, who performed routine screening on arrival and departure, and provided primary health care services.
The health of people in immigration detention has attracted considerable attention, both in the popular press2 and in academic publications.3-6 In particular, there is almost universal criticism of the policy of detaining asylum seekers, particularly in terms of the mental health implications, with studies reporting a link between detention and mental illness.7-11
The 2005 Palmer Inquiry12 found serious flaws in the culture and processes of the now Department of Immigration and Citizenship (DIAC) and in the organisation of health services for people in detention. In response to this criticism, the Australian Government established a Detention Health Advisory Group (DeHAG) in early 2006, consisting of representatives from key clinical associations.13 DeHAG recommended that independent research be undertaken on the health of people in detention, and here we summarise the key findings of that analysis.
The study and sample populations, by category and length of stay in detention, are shown in Box 1. Within each of the cohorts, people were selected at random for the sample. The sample represented 10% of people in detention and nearly 28% of days spent in detention during 2005–06 (Box 1).
Each encounter was coded according to its primary reason. The International Classification of Primary Care, version 2 PLUS (ICPC-2 PLUS)14 was used to code complaints, symptoms and interventions, and the International Classification of Diseases, 10th revision, Australian modification (ICD-10-AM)15 was used to code causes of injury. The ICPC-2 PLUS codes enabled a distinction to be made between encounters at which a definitive medical diagnosis was made (“Diagnosis”) and encounters at which health problems were recorded but there was no definitive diagnosis (“Complaints and symptoms”).16 For example, “depressive disorder” and “migraine” were coded as diagnoses, whereas “feeling depressed” and “headache” were coded as complaints and symptoms. We use the term “health problems” collectively to include diagnoses and complaints or symptoms.
The age and estimated sex profiles of the study population are given in Box 2. Age was calculated as at the date the detainee first entered detention. During 2005–06, children were in detention centres (this no longer occurs); there were 346 children aged < 17 years, 46 of whom were in the sample.
Between them, the 7375 people in the study population spent 298 536 days in detention in 2005–06, during which time they had an estimated 52 192 (95% CI, 50 238–54 145) health encounters (Box 3). This was equivalent to 1.2 (95% CI, 1.18–1.27) health encounters per person-week. A new health problem was recorded at an estimated 16% of encounters, and 29% of encounters were for routine screening or assessment. Nearly half (44%) were for follow-up of a health problem recorded at an earlier encounter.
An estimated 37.5% (95% CI, 31.5%–43.5%) of detainees had at least one new health problem in 2005–06; the estimated proportion varied from 66.8% (95% CI, 66.7%–66.9%) of “Unauthorised boat arrivals” to 20.8% (95% CI, 19.6%–22.1%) of “Unauthorised air arrivals”. Box 4 lists the estimated number of new health problems. The most common types of problems included dental and respiratory problems, and lacerations. Among those detained for more than a year, mental health, social and musculoskeletal problems were common.
Incidence rates of new health problems in the study period by cohort are shown in Box 5, A. “Unauthorised boat arrival” asylum seekers detained for > 24 months had the most new health problems, with an average of 6.47 recorded for every 100 person-days in detention. These problems were in addition to any diagnosed before the study period.
Box 5, B shows that mental health was a significant health issue for people in detention. The reason for detention was found to have a significant additional effect on the rate of new mental health problems after allowing for time spent in detention (P < 0.001). The rate for those designated “Unauthorised boat arrivals” was significantly higher than that for other groups (a multiplicative factor of 2.0 [95% CI, 1.6–3.3] compared with “Visa breach”; 3.8 [95% CI, 2.0–7.2] compared with “Visa overstay”; and 11.9 [95% CI, 2.8–50.4] compared with “Illegal foreign fisher”). Similarly, time in detention was found to have a significant additional effect after allowing for the reason for detention (P = 0.018). People detained for > 24 months had rates of new mental illness 3.6 (95% CI, 1.1–11.0) times higher than for those who were released within 3 months.
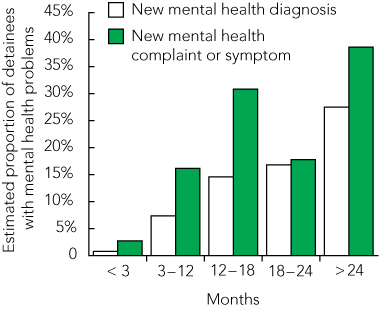
As shown in Box 6, the proportion of people with at least one mental health diagnosis was related to time spent in detention. The estimated proportion of those with a new mental health diagnosis during the year varied from < 1% (95% CI, 0–2.0%) in the group detained for < 3 months, to > 27% (95% CI, 27.3%–27.7%) for those in detention for > 24 months. Likewise, for mental health complaints or symptoms, the estimated percentage varied from 3% (95% CI, 0.5%–5.0%) to 39% (95% CI, 38.4%–38.9%). The 12–18-months cohort, largely people detained for “Visa overstay”, had a lower rate of new mental health problems.
Injury rates (Box 7) (adjusted for time in detention) were highest for “Unauthorised air arrivals” and “Visa breach” at about 0.3 per 100 person-days. The “Illegal foreign fishers” had the lowest injury rate at almost 0.1 per 100 person-days. People seeking asylum had proportionally fewer injuries due to assault, but proportionally more due to self-harm, in comparison with the other cohorts.
Other studies have also found an association between time in detention and mental health. Among a non-random sample of asylum seekers in detention centres or gaols (n = 70) in three US states, 70% reported that their mental health had worsened substantially while in detention, and there was a relationship between length of time in detention and levels of anxiety, depression and post-traumatic stress disorder.7 Another study (n = 55) compared the mental health of detained and not detained Afghan asylum seekers in Japan and found that detention was associated with a worsening of mental health.8
A large retrospective review of referral records (n = 4516) of asylum seekers in centres run by the Danish Red Cross “found an increase in referrals for mental disorders with increased length of stay in asylum centres in a large, multiethnic population of asylum seekers”.9 Two Australian studies investigated mental health issues in previously detained refugees from different communities. In a Mandaean community (n = 241), longer detention was associated with more severe mental disturbance, an effect that persisted for an average of 3 years after release.10 A study in a Persian-speaking community (n = 116) identified the detention experience as a cause of serious or very serious stress.11
1 Study and sample populations by category and length of stay in detention, 2005–06
3 Reason for health encounter, by cohort, 2005–06
Estimated proportion of health encounters involving definitive treatment |
|||||||||||||||
4 New health conditions recorded in detainees, 2005–06, by ICPC-2 PLUS chapter
Estimated no. of new health problems (95% CI) and % of total |
|||||||||||||||
ICPC-2 PLUS = International Classification of Primary Care, version 2 PLUS.14 * Including non-compliance with treatment and/or medication. |
|||||||||||||||
5 New health (A) and mental health (B) problems (diagnoses and complaints or symptoms), 2005–06
Estimated rate of new health problems per 100 person-days (95% CI) |
|||||||||||||||
Diagnoses as a percentage of estimated number of new health problems |
|||||||||||||||
Estimated rate of new mental health problems per 100 person-days (95% CI) |
|||||||||||||||
Diagnoses as a percentage of estimated number of new mental health problems |
|||||||||||||||
na = not applicable (see Box 1). * Actual population rate. † Too few occurrences in sample to calculate CI. |
|||||||||||||||
Received 16 August 2008, accepted 30 August 2009
- Janette P Green1
- Kathy Eagar2
- Centre for Health Service Development, University of Wollongong, Wollongong, NSW.
The study was funded by the Australian Department of Immigration and Citizenship, who had no role in the analysis or interpretation of data, the writing of the report or the decision to publish. We acknowledge the contributions of the Detention Health Advisory Group; as well as Kerry Innes, Lauren Jones, Carmel Cheney-Fielding, Peter Samsa, Peter Eklund and Pam Grootemaat; and the helpful advice of Elmer V Villanueva.
None identified.
- 1. Australian Government Department of Immigration and Citizenship. Media Fact Sheet 82 — Immigration detention. http://www.immi. gov.au/media/fact-sheets/82detention.htm (accessed Nov 2009).
- 2. Immigration feature. The Age (Melbourne) 2005; 25 Aug – 24 Oct. http://www.the age.com.au/issues/immigration (accessed Nov 2009).
- 3. Steel Z, Silove DM. The mental health implications of detaining asylum seekers. Med J Aust 2001; 175: 596-599. <MJA full text>
- 4. Smith MM. Asylum seekers in Australia. Med J Aust 2001; 175: 587-589. <MJA full text>
- 5. Swan N. Concern grows over health of Australia’s refugee population. BMJ 2001; 323: 529.
- 6. Fazel M, Silove D. Detention of refugees. BMJ 2006; 332: 251-252.
- 7. Keller AS, Rosenfeld B, Trinh-Shevrin C, et al. Mental health of detained asylum seekers. Lancet 2003; 362: 1721-1723.
- 8. Ichikawa M, Nakahara S, Wakai S. Effect of post-migration detention on mental health among Afghan asylum seekers in Japan. Aust N Z J Psychiatry 2006; 40: 341-346.
- 9. Hallas P, Hansen AR, Staehr MA, et al. Length of stay in asylum centres and mental health in asylum seekers: a retrospective study from Denmark. BMC Public Health 2007; 7: 288.
- 10. Steel Z, Silove D, Brooks R, et al. Impact of immigration detention and temporary protection on the mental health of refugees. Br J Psychiatry 2006; 188: 58-64.
- 11. Momartin S, Steel Z, Coello M, et al. A comparison of the mental health of refugees with temporary versus permanent protection visas. Med J Aust 2006; 185: 357-361. <MJA full text>
- 12. Palmer MJ. Inquiry into the circumstances of the immigration detention of Cornelia Rau. Report. Canberra: Commonwealth of Australia, July 2005. http://www.immi.gov.au/media/publications/pdf/palmer-report.pdf (accessed Nov 2009).
- 13. Detention Health Advisory Group. Report against 2006-2007 work programme. A report to the Department of Immigration and Citizenship. March 2007: 2. http://www.immi.gov.au/managing-australias-borders/detention/_pdf/dehag.pdf (accessed Nov 2009).
- 14. Family Medicine Research Centre, University of Sydney. ICPC-2 PLUS User’s Guide 1998. http://www.fmrc.org.au/Download/PC_UserGuide_Web2007.pdf (accessed Nov 2009).
- 15. Roberts RF, Innes KC, Walker SM. Introducing ICD-10-AM in Australian hospitals. Med J Aust 1998; 169 (8 Suppl): S32-S35. <MJA full text>
- 16. International Classification Committee of WONCA. ICPC-2 International classification of primary care, 2nd ed. Oxford: Oxford Medical Publications, 1998.





Abstract
Objective:
Design, setting and subjects: An analysis of the health records of 720 of the 7375 people in detention in the financial year 1 July 2005 – 30 June 2006, with oversampling of those detained for > 3 months.
Main outcome measures: Health encounters and health condition categories; estimated incidence rates of new health conditions, new mental health conditions, and new injuries for each cohort (defined by time in, and reason for, detention).
Results: People in detention had an estimated 1.2 (95% CI, 1.18–1.27) health encounters per person-week. Those detained for > 24 months had particularly poor health, both mental and physical. Asylum seekers had more health problems than other people in detention. The main health problems varied depending on the length of time in detention, but included dental, mental health, and musculoskeletal problems, and lacerations. Both time in, and reason for, detention were significantly related to the rate of new mental health problems (P = 0.018 and P < 0.001, respectively). The relationship between these variables and the incidence rates of physical health problems was more complex.
Conclusion: People in immigration detention are frequent users of health services, and there is a clear association between time in detention and rates of mental illness. Government policies internationally should be informed by evidence from studies of the health of this marginalised and often traumatised group.