- The introduction of casemix funding systems has focused attention
on the reliability and validity of coded health data.
- Defining and classifying medical and health related terms are the
core activities of the National Centre for Classification in Health
(NCCH), which has recently published the Australian modification of
the International statistical classification of diseases and
health related problems, 10th revision (ICD-10-AM). An
important feature is a classification of procedures (MBS-E) based on
the Commonwealth Medical Benefits Schedule.
- Clinicians have made major contributions to the new classification
through a network of 21 Clinical Coding and Classification Groups,
which advise the NCCH.
- Major advantages of ICD-10-AM for clinicians include the ability to
update the classification within Australia with continued clinical
consultation, the familiarity of the procedure codes based on MBS,
and the possibility of having one classification for use in public and
private healthcare facilities.
Introduction Codes for diseases and procedures are the basic ingredients of the casemix recipe. However, the coding function was not invented for casemix. The need to classify and measure has been around for centuries (Box 1). Allied to this need to impose order by classifying is the need to define the elements of a disease or procedure so that the meaning is clear and classification can take place. O'Rourke highlighted the importance of the meaning of medical terms in the context of doctor-patient communication in cardiology.3 Using codes to describe concepts is a shorthand way of ensuring a common understanding of the definition of that concept.
The introduction of casemix funding systems based on the classification of diseases and procedures has meant that disciplined attention has been paid to the reliability and validity of coded health data. The connection between the codes and the health dollar has turned the spotlight on coding previously used only to identify groups of similar patients for research, utilisation studies or quality assurance.
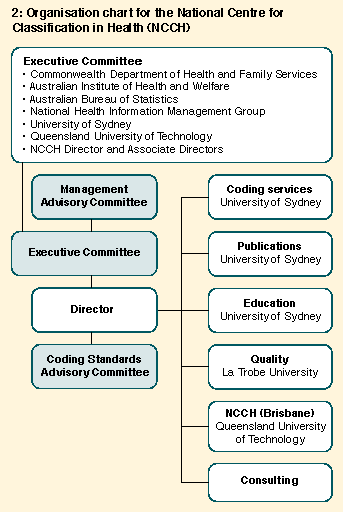
National Centre for Classification in Health The twin functions of defining and classifying medical and health related terms are the core activities of the National Centre for Classification in Health (NCCH), located at the University of Sydney, and Queensland University of Technology (Box 2). The Quality Division at La Trobe University, Melbourne, examines issues relating to coding and data quality. The NCCH develops codes and coding standards for use in Australian health services, publishes in hard copy and electronically, and educates clinical coders and clinicians in the application of codes. It also publishes methods of measuring coding quality and assists the Australian Institute of Health and Welfare in its role as WHO Collaborating Centre for Classification of Diseases. The Brisbane site supports the Australian Bureau of Statistics (ABS) in relation to its classification of causes of death.
The ABS has been recording cause of death using the classification system International classification of diseases (ICD) and its predecessors since 1907 (Box 1). Australian hospitals and health services have collected ICD data on diagnoses and procedures since 1968. Before 1968, the Standard Nomenclature of Diseases and Operations,4 and sometimes the ICD, were used in hospitals to capture disease and procedure information, mainly for research purposes.
The use of codes for casemix classification led to the need for Australian national standards in the application of codes, and eventually to the formation of specific Australian codes and classifications. These Australian Coding Standards have been developed by the NCCH.5
ICD-10-AM The NCCH has recently published the International statistical classification of diseases and related health problems, 10th revision, Australian modification (ICD-10-AM),5 which includes Australian extensions of the WHO codes in ICD-10 and some specific Australian disease codes. An important feature is the addition of a classification of procedures based on the Commonwealth Medicare Benefits Schedule (MBS) of fees for health services. It was a deliberate decision of the Casemix Implementation Project Board in 1995 to create this Australian procedure classification based on the fee schedule so that the classification of procedures in the public and private sectors, as well as in ambulatory situations, would be more consistent. The Australian procedure classification, known as the Medicare Benefits Schedule, Extended (MBS-E), is more specific than MBS, and is organised logically according to body system and site and includes a detailed index. Codes have been added for procedures not currently eligible for benefits, such as cosmetic surgery, obstetrics and allied health procedures.
ICD-10-AM was introduced in July 1998 in hospitals and other healthcare agencies in New South Wales, the Australian Capital Territory, Victoria and the Northern Territory. It will be introduced in the remaining States from July 1999. The ABS, because of its commitment to report mortality data to the WHO, will continue to use the WHO version of the ICD classification. It is planned to implement ICD-10 for mortality coding in the year 1999 or 2000; the decision will depend on the availability of the Automated Cause of Death coding software from the United States.
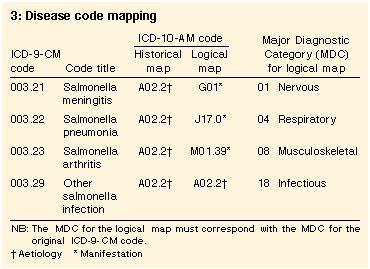
Casemix classification and mapping Construction of casemix classifications requires data expressed in the source coding systems. Because the national casemix classification system, AN-DRG, has until now been based on the previous standard classification in Australia, ICD-9-CM, the changeover to ICD-10-AM will require mapping between the classifications so that a version of AN-DRG based on ICD-10-AM can be built. Until data are available in ICD-10-AM from Australian hospitals and health services, AN-DRG allocation must rely on mappings between ICD-9-CM and ICD-10-AM. Mappings for grouping purposes are known as "logical" mappings, while those for longitudinal epidemiological studies are called "historical" mappings. The slight differences between these mappings arise because of differences in specificity of the classifications, especially in situations where one code in the new classification maps to many codes in the previous classification, and the many codes are spread over many DRGs (Box 3).
Interaction between clinicians and clinical coders
Clinicans have made major contributions to the structure and content of the new Australian disease and procedure classifications through a network of 21 Clinical Coding and Classification Groups (CCCG), which advise both the NCCH and the Australian Casemix Clinical Committee (ACCC) on issues relating to coding and casemix refinement. Many additions to the WHO ICD-10 were made as a result of mapping between ICD-9-CM and ICD-10 to ensure that specificity and new Australian codes introduced to ICD-9-CM were replicated in ICD-10-AM. Examples of notable improvements in ICD-10-AM compared with ICD-9-CM are listed in Box 4.
To promote clinician-coder communication, the NCCH has been funded by the ACCC to publish a series of specialty booklets on coding and casemix. A series of 21 booklets on different clinical topics is planned, of which a third is already available. Detailed information of interest to clinicians and epidemiologists about changes in ICD-10-AM is currently being prepared by the NCCH and will be available on the NCCH internet homepage.6 The NCCH also has an education function in keeping clinical coders abreast of annual updates to the coding system and the Australian Coding Standards.5 It will play a major role in educating clinical coders in ICD-10-AM. The NCCH's homepage6 is regularly updated and has links to relevant Australian and overseas organisations.
Impact of ICD-10-AM
Clinicians: Australian clinicians will benefit greatly from the new Australian classification. Firstly, it makes current the description and classification of diseases, and reinforces the Australian clinical contribution to updating the underlying WHO classification. The mechanism of clinical consultation used in constructing the classification will be continued in the updating process so that the classification remains clinically coherent and relevant. Secondly, by using the Medicare Benefits Schedule as the foundation of the procedure classification, the concepts and labels of the procedure codes will be familiar to clinicians, and the update of MBS-E will proceed in tandem with the update of MBS. Having one Australian procedure classification for use in public and private healthcare facilities, inpatient and ambulatory situations will be more efficient than the existing system (ICD-9-CM in the public sector and MBS in the private sector) and will do away with the need for mapping between MBS and ICD.
Clinical coder workforce: Introduction of the new classification will have major implications for the clinical coder workforce. They will not only need to become familiar with ICD-10-AM coding, but will also need an understanding of anatomy and the surgical procedures required by the specificity of the MBS-E. ICD-10-AM coding is expected to take longer initially,7 although no allowances have been made in the deadlines for reporting hospital morbidity data in the States and Territories adopting the new classification in 1998. Health facility managers are becoming more aware of the need for resources for clinical coders to reflect the complexity of casemix through accurate and timely clinical coding.
Updating the classification: A major benefit is the ability to regularly update the classification within Australia. We intend to maintain close connections with international disease classification systems so that statistics on causes of death and morbidity are comparable. However, having an Australian centre for health classification develops local expertise and fosters robustness of the Australian classification itself, data quality and efficiency of data collection, as well as a clearer understanding of the meaning of clinical terms and their place in classification hierarchies.
Synchronising coding systems: Introduction of ICD-10-AM also provides an opportunity for synchronising coding systems with software designed to support electronic patient records. Without appropriate coding standards, data from these systems cannot be extracted, analysed and stored so that it is retrievable and capable of integration with other related modules and functions (eg, pharmacy and laboratory data). Modifications to health service software systems will be required to accommodate the new composition of the codes. The ICD-10-AM disease codes are alpha-numeric (3-5 characters; eg, Ross River disease [B33.1]) and the procedure codes are numeric (7 characters; eg, endoluminal repair of aneurysm [90228-00]).
Analysis of longitudinal data: The change in classifications will affect analysis of longitudinal data by epidemiologists and public health practitioners. They will have the option of mapping forwards from the old to the new classification, or backwards from the new to the old classification. In either case, meaning will be lost when the codes of one classification are more precise or less precise than those of the other. However, there will be benefits in the introduction of appropriate new codes and terminology, particularly for infectious diseases, neoplasms, obstetrics and mental health.
Conclusion Considerable effort has always been devoted to coding diseases and procedures in hospitals. Casemix funding systems with their reliance on accurate classification of diseases and procedures provide a major incentive to getting the data right. Systems are in place through the ICD-10-AM codes, the Australian Coding Standards, the clinical coder workforce, and through input from clinicians to ensure that coding is clinically appropriate, efficient, accurate and timely.
References
- Lyons AS, Petrucelli RJ. Medicine: An illustrated history. New York: Harry N Abrams, 1987.
- History of the development of the ICD. In: World Health Organization. International statistical classification of diseases and related health problems. 10th revision. Vol 2, Ch 6. Geneva: WHO, 1993.
- O'Rourke MF. What's in a name? Med J Aust 1997; 166: 372-373.
- Thompson ET, Hayden AC. Standard nomenclature of diseases and operations. 5th ed. New York: McGraw-Hill, American Medical Association; 1961.
- National Centre for Classification in Health. The international statistical classification of diseases and related health problems, 10th revision, Australian modification (ICD-10-AM). Sydney: National Centre for Classification in Health, Faculty of Health Sciences, University of Sydney, 1998.
- National Centre for Classification in Health. World Wide Web homepage: http://www.cchs.usyd.edu.au/NCCH/ncch.html
- Department of Health and Family Services. ICD-10-AM impact assessment project. Final report. Adelaide: Coopers & Lybrand Consultants, November 1997: 30.
Authors' details National Centre for Classification in Health, University of Sydney, Sydney, NSW; and Queensland University of Technology, Brisbane, QLD.
Rosemary F Roberts, MPH, MBA, Director, National Centre for Classification in Health, Sydney.
Kerry C Innes, AssocDip(MRA), Associate Director, National Centre for Classification in Health, Sydney.
Susan M Walker, BAppSc(MRA), Associate Director, National Centre for Classification in Health, Brisbane.
Reprints will not be available from the authors.
Correspondence:
Associate Professor R F Roberts, National Centre for Classification
in Health, University of Sydney, PO Box 170, Lidcombe, NSW 1825.
E-mail: R.RobertsATcchs.usyd.edu.au




