In April 2009, a novel influenza virus, currently termed pandemic (H1N1) 2009, was identified in the United States and Mexico.1,2 The situation evolved rapidly and, on 11 June 2009, the World Health Organization declared it to be a pandemic.3 Queensland implemented a graded response (Box 1) in line with the Australian Health Management Plan for Pandemic Influenza (AHMPPI).4
Here, we provide an overview of the public health actions undertaken in Queensland in the initial phases of the pandemic, and present the epidemiological findings up to the declaration of the “Protect” phase of the response5 on 22 June 2009.
The focus of the Delay phase was the early identification and management of cases and contacts. Clinicians were asked to strengthen infection control and notify suspected cases to population health units for follow-up and contact tracing. A suspected case was defined as someone with an acute febrile respiratory illness who had been to a country with sustained community transmission or had close contact with a confirmed or suspected case within the past 7 days.8 Patients with confirmed or suspected disease were treated with antiviral drugs and isolated for 7 days. Close contacts were given antiviral prophylaxis and quarantined for 7 days.4 If a patient with suspected disease tested negative, then antiviral therapy and isolation were ceased.
Border measures to identify potential cases included positive pratique (notification of the health status of passengers by pilots), self-declaration by passengers through health declaration cards, and thermal scanners at airports to identify those with high fevers.9,10 At Queensland airports, 780 travellers identified by these measures were screened by border nurses, and 52 who met the case definition were tested and referred to population health units for follow-up. Of these, four tested positive for pandemic (H1N1) 2009 infection.
A key public health measure in the Contain phase was school closures. Early reports from other countries and from Victoria showed that children and young adults were disproportionately affected, and that outbreaks had spread rapidly in schools.2,12-15 The closure of schools to reduce spread was also supported by modelling.4 Schools and childcare centres were closed if a person with confirmed disease had attended while infectious, for a week from their last attendance. Close contacts (including students and staff in the same class) were given antiviral prophylaxis and quarantined for 7 days. These measures continued until 26 June 2009, when school holidays started. A total of 48 schools (2.8% of all schools in Queensland) and five childcare centres were closed. Parents were also requested to keep their children away from school for 7 days if they had returned from an area of sustained community transmission.
In light of evidence showing that the disease was not as severe as initially thought, and to enable a response proportionate to the risk, a new phase — Protect — was introduced, and an annex was added to the AHMPPI.5 With the disease established in the community, the focus shifted to identifying and treating those who were most vulnerable to severe disease. Considerable resources were invested to prevent the spread of disease in Indigenous communities in remote areas of Far North Queensland, given concerns about the higher prevalence of medical risk factors and poorer access to medical services in these communities.16
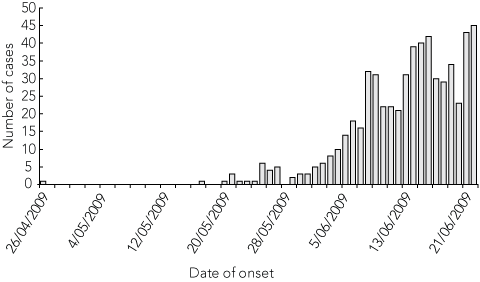
Population health units entered data on suspected and confirmed cases into a web-based, outbreak case-reporting tool (NetEpi), administered by the Australian Government Department of Health and Ageing. Five hundred and ninety-three laboratory-confirmed cases were notified in Queensland with onset of illness between 26 April and 22 June 2009 (Box 2). Sixteen patients were hospitalised, but no deaths were reported.
The use of personal protective equipment among health practitioners in the pandemic was not always ideal.17 Population health units reported several clinicians requiring prophylaxis and quarantine because of inadequate infection-control precautions. A cluster of six cases was also reported in a Queensland public hospital, linked to a health care worker.
Males and females were affected similarly (52% male). The mean and median ages of notified patients were 25 and 21 years, respectively (range, 0–76 years). The median age was similar in Queensland to that reported in Victoria (21 years) and Western Australia (22 years).18 Median ages reported by the WHO elsewhere were: 17 years in Canada, 12 years in the United Kingdom, 13 years in Chile, 24 years in the WHO European region, and 23 years in the WHO Western Pacific region.19
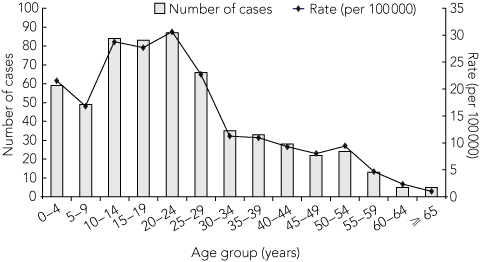
In Queensland, the highest rate of confirmed cases was in the 20–24-years age group (30.6 per 100 000). Age-specific rates are summarised in Box 3 and Box 4. Over-representation of younger age groups has been reported from other countries as well as Australia and may represent greater social mixing, increased susceptibility or biases towards testing these age groups.1,18,19
Border measures required the investment of significant clinical and public health resources and had only a low pick-up rate. The low sensitivity and usefulness of border measures were questioned after the 2003 outbreak of severe acute respiratory syndrome (SARS).21,22 We recommend that border screening should be formally evaluated in the context of the influenza pandemic and in reviews of pandemic plans.
As the pandemic progressed, the response shifted from predominantly public health to a clinical domain, with focus on preparing for the expected surge in admissions and requirement for intensive care services. Ongoing concerns are the potential for resistance to oseltamivir23,24 (the most widely used antiviral) to become more widespread, and the possibility of a second pandemic wave.25
The rollout of the pandemic vaccine, prioritised according to risk group, commenced nationally on 30 September 2009.26 Although this should have triggered a switch to the Control phase (according to the AHMPPI), the Protect phase will continue, with ongoing measures to reduce morbidity and mortality in vulnerable groups.27
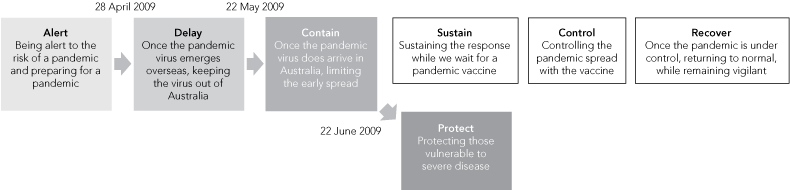
1 Pandemic phases according to the Australian Health Management Plan for Pandemic Influenza (AHMPPI)4,5
 | |||||||||||||||
|
Boxes represent the stages of the AHMPPI response, and arrows show the pathway followed by Queensland. Victoria commenced a “modified sustain” phase on 3 June 2009.6 | |||||||||||||||
2 Notifications of laboratory-confirmed cases of pandemic (H1N1) 2009 infection in Queensland by date of onset, 26 April – 22 June 2009
- Ranil D Appuhamy1
- Frank H Beard2
- Hai N Phung3
- Christine E Selvey3
- Frances A Birrell3
- Terry H Culleton3
- 1 Population Health, Queensland Health, Brisbane, QLD.
- 2 Communicable Diseases Branch, Queensland Health, Brisbane, QLD.
- 3 State Health Emergency Coordination Centre, Queensland Health, Brisbane, QLD.
None identified.
- 1. Dawood FS, Jain S, Finelli L, et al; Novel Swine-Origin Influenza A (H1N1) Virus Investigation Team. Emergence of a novel swine-origin influenza A (H1N1) virus in humans. N Engl J Med 2009; 360: 2605-2615.
- 2. New influenza A(H1N1) virus infections: global surveillance summary, May 2009. Wkly Epidemiol Rec 2009; 84 (20): 173-179.
- 3. World Health Organization. World now at the start of 2009 influenza pandemic. Statement to the press by WHO Director-General Dr Margaret Chan. 11 Jun 2009. http://www.who.int/mediacentre/news/statements/2009/h1n1_pandemic_phase6_20090611/en/index.html (accessed Jun 2009).
- 4. Australian Government Department of Health and Ageing. Australian Health Management Plan for Pandemic Influenza. http://www.flupandemic.gov.au/internet/panflu/publishing.nsf/Content/ahmppi (accessed Jun 2009).
- 5. Australian Government Department of Health and Ageing. Protect phase. Annex to the Australian Health Management Plan for Pandemic Influenza. 8 Jul 2009. http://www.healthemergency.gov.au/internet/healthemergency/publishing.nsf/Content/resources/$File/AHMPPI-PROTECTannex.pdf (accessed Jul 2009).
- 6. VIC Health. Victoria moves to modified sustain phase of flu plan [media release]. 3 Jun 2009. http://humanswineflu.health.vic.gov.au/downloads/media/media-release030609.pdf (accessed Jun 2009).
- 7. Australian Government Department of Health and Ageing. Australia upgrades its Australian pandemic phase. 28 Apr 2009. http://www.healthemergency.gov.au/internet/healthemergency/publishing.nsf/Content/news-002 (accessed Jul 2009).
- 8. Bishop J. Chief Medical Officer Update: 5 May 2009. http://www.healthemergency.gov.au/internet/healthemergency/publishing. nsf/Content/D20AB232CC89EC90CA25763C001A6F76/$File/090505%20Letter%20-%20CMO%20update%206%20-%20SIGNED.pdf (accessed Nov 2009).
- 9. Australian Government Department of Health and Ageing. Positive pratique for all flights. 29 Apr 2009. http://www.healthemergency.gov.au/internet/healthemergency/publishing.nsf/Content/news-006 (accessed Jul 2009).
- 10. Australian Government Department of Health and Ageing. Government activates thermal scanners and health declaration cards at airports. 30 Apr 2009. http://www.healthemergency.gov.au/internet/healthemergency/publishing.nsf/Content/news-008 (accessed Sep 2009).
- 11. Australian Government Department of Health and Ageing, Minister for Health and Ageing. Alert level raised to ‘contain’ [media release]. 22 May 2009. http://www.healthemergency.gov.au/internet/healthemergency/publishing.nsf/Content/news-022 (accessed Jul 2009).
- 12. Swine-origin influenza A (H1N1) virus infections in a school — New York City April 2009. MMWR Morb Mortal Wkly Rep 2009; 58: 470-472.
- 13. Health Protection Agency, Health Protection Scotland new influenza A(H1N1) investigation teams. Epidemiology of new influenza A(H1N1) in the United Kingdom, April–May 2009. Euro Surveill 2009; 14 (19): pii=19213. http://www.eurosurveillance.org/ViewArticle.aspx?ArticleId=19213 (accessed Jul 2009) .
- 14. World Health Organization Regional Office for Europe. Update on influenza A(H1N1), European Region of the World Health Organization. April–May 2009. http://www.euro.who.int/influenza/AH1N1/20090523_1 (accessed Jun 2009).
- 15. State Government of Victoria, Minister for Health. Six more schools close due to H1N1 human swine flu [media release]. 31 May 2009. http://humanswineflu.health.vic.gov.au/downloads/media/media-release310509.pdf (accessed Jul 2009).
- 16. Australian Institute of Health and Welfare. Australia’s health 2008. Canberra: AIHW, 2008. (AIHW Cat. No. AUS 99.)
- 17. Novel influenza A (H1N1) virus infections among health-care personnel — United States, April–May 2009. MMWR Morb Mortal Wkly Rep 2009; 58: 641-645.
- 18. Kelly HA, Grant KA, Williams S, et al. Epidemiological characteristics of pandemic influenza H1N1 2009 and seasonal influenza infection. Med J Aust 2009; 191: 146-149. <MJA full text>
- 19. New influenza A (H1N1) virus infections: global epidemiological situation, June 2009. Wkly Epidemiol Rec 2009; 84 (25): 249-257.
- 20. Australian Bureau of Statistics. Population by age and sex, Australia 2007. Canberra: ABS, 2008. (ABS Cat. No. 3235.0.)
- 21. Pitman RJ, Cooper BS, Trotter CL, et al. Entry screening for severe acute respiratory syndrome (SARS) or influenza: policy evaluation. BMJ 2005; 331: 1242-1243.
- 22. Samaan G, Patel M, Spencer J, Roberts L. Border screening for SARS in Australia: what has been learnt? Med J Aust 2004; 180: 220-223. <MJA full text>
- 23. Health Protection Agency (UK). Swine flu sample resistant to antiviral oseltamivir [media release]. 30 Jun 2009. http://www.hpa.org.uk/servlet/Satellite?c=HPAweb_C&cid=1246345135429&pagename=HPAweb%2FHPAwebStandard (accessed Jul 2009).
- 24. World Health Organization. Viruses resistant to oseltamivir (Tamiflu) identified. Pandemic (H1N1) 2009 briefing note 1. 8 Jul 2009. http://www.who.int/csr/disease/swineflu/notes/h1n1_antiviral_resistance_20090708/en/index.html (accessed Jul 2009).
- 25. World Health Organization. Pandemic (H1N1) 2009 briefing note 9. Preparing for the second wave: lessons from current outbreaks. 28 Aug 2009 http://www.who.int/csr/disease/swineflu/notes/h1n1_second_wave_20090828/en/index.html (accessed Nov 2009).
- 26. Australian Government Department of Health and Ageing. Pandemic (H1N1) 2009 vaccine. http://www.healthemergency.gov.au/internet/healthemergency/publishing.nsf/Content/vaccine (accessed Sep 2009).
- 27. Australian Government Department of Health and Ageing. Current status. Pandemic phases. http://www.healthemergency.gov.au/internet/healthemergency/publishing.nsf/Content/phases (accessed Sep 2009).





Abstract
A graded public health response was implemented to control the pandemic (H1N1) 2009 outbreak in Queensland.
Public health measures to contain the outbreak included border control, enhanced surveillance, management of cases and contacts with isolation or quarantine and antivirals, school closures and public education messages.
The first confirmed case in Australia was notified on 8 May 2009, in a traveller returning to Queensland from the United States.
In Queensland, 593 laboratory-confirmed cases were notified with a date of onset between 26 April and 22 June 2009, when the Protect phase of the Australian Health Management Plan for Pandemic Influenza was implemented; 16 hospitalisations and no deaths were reported during this time.
The largest number of confirmed cases was reported in the 10–19-years age group (167, 28% of cases), followed by the 20–29-years age group (153, 26% of cases).
With ongoing community transmission, the focus has shifted from public health to the clinical domain, with an emphasis on protecting vulnerable groups.
Considerable resources have been invested to prevent and control the spread of disease in Indigenous communities in Far North Queensland.
The capacity of clinical services to cope with increased admissions, the potential for widespread antiviral resistance, and rollout of mass vaccination campaigns remain future challenges.