During the global outbreak of severe acute respiratory syndrome (SARS), border screening programs were instigated to detect SARS among travellers and thus limit the spread of the disease.1-3 Although the World Health Organization (WHO) recommended exit screening only,4 many countries such as Canada, New Zealand, Hong Kong and Australia also had entry screening to identify ill travellers and to assess them for SARS. Some of the screening measures used at border points included visual or clinical screening of travellers by medical personnel, and health declaration cards that documented travel history, the presence of SARS-like symptoms and a history of contact with SARS patients.
SARS posed a challenge to traditional disease-control measures, as information about the emerging infection was scant and public concern was high. Rapid consideration had to be given to the sensitivity and specificity of border screening criteria, the personnel and logistics needed, and the possible impact of screening on international traffic and trade. Most countries recognised the need to use border screening in conjunction with other disease-control measures, but emphasised its role in preserving public confidence and limiting negative economic consequences.5
To prepare for future outbreaks of SARS or similar emerging infections, it is necessary to assess the effectiveness of Australia’s border entry program. Publications from three countries have alluded to their experience with border screening, and all revealed extremely low detection rates of SARS. 1-3 Hong Kong screened 35.6 million people at its borders and, based on the use of health declaration cards, identified two people with SARS; Canada screened 6.5 million people and Singapore screened 0.4 million people, but neither country identified any SARS cases at the border.
We report here the effectiveness of the Australian border screening program, and the lessons learnt for future application — for SARS and other emerging diseases.
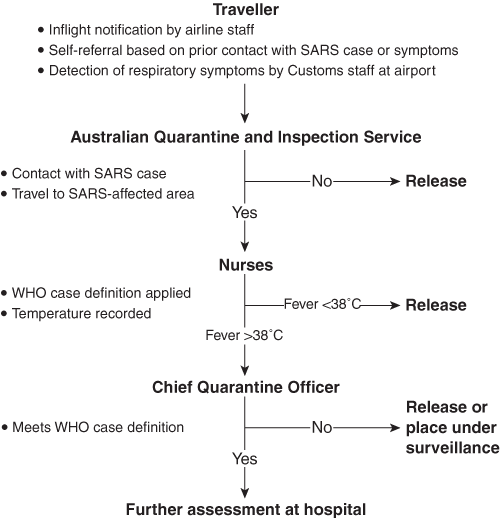
Three levels of border screening for SARS were introduced at Australian international airports on 5 April 2003 (Box 1). Based on the presence of respiratory symptoms, such as cough, shortness of breath and difficulty breathing, arriving travellers were referred by flight or airport staff for an initial screening by the staff of the Australian Quarantine and Inspection Service (AQIS). Travellers considered likely to have SARS on the basis of their travel history and symptoms were referred by AQIS staff to nurses stationed at the airports. The nurses assessed clinical symptoms, measured body temperature using an ear thermometer, and determined possible exposure to SARS based on the WHO case definition.6 At this stage, the traveller was either considered not to have SARS and released, or was referred to the Chief Quarantine Officer (CQO) of the respective state or territory for further assessment. The nurse telephoned the CQO, who then assessed the traveller in a room fitted with appropriate infection control measures.7 If the CQO concurred that SARS was a likely explanation for the illness, the traveller was then referred to a designated state or territory hospital for further assessment and management.
A two-level program was instigated at Australia’s seaports, where AQIS staff directly contacted the CQO to inform him or her of ill passengers.
The effectiveness of the border entry screening program was assessed for arrivals between 5 April and 16 June 2003. This 72-day period was a peak period in the global outbreak, during which 6044 of the total 8422 cases were reported.8 During this period, people arriving at airports and seaports received health-alert notices from Customs staff to inform them of SARS, and of ways to seek medical assistance if symptoms developed. During the study period, the screening program did not include completion of written health declaration cards or mass temperature screening for all arrivals.
There were 1.84 million arrivals into Australia during the 72-day study period. Of these, 241 491 (13.1%) arrived from countries with local transmission of SARS (ie, Vietnam, Taiwan, Singapore, Hong Kong, Canada, China and the Philippines). Of all arrivals, AQIS staff assessed 794 travellers. Of these, 734 (92.4%) were referred by AQIS staff to the nurses at airports; this number constituted 3.1 travellers referred per 1000 arrivals from SARS-affected areas, and 0.4 travellers per 1000 arrivals from all ports of origin. Nineteen people (2.4%) were then referred to the CQO.
Of the 19 travellers referred to the CQO, four were referred to hospital for further investigations (Box 2). Two additional travellers, who were asymptomatic, were placed under home surveillance, as they had been in recent close contact with SARS patients.
Based on the Australian SARS Case Register, 13 people were initially assessed as probable SARS cases and 64 as suspected SARS cases. Of these, five people from the former group and 24 from the latter group acknowledged being symptomatic on arrival (Box 3). However, border screening had detected only 4 (13.8%) of these 29 symptomatic travellers, although none of these people were later classified as probable SARS cases. Of the 25 people with symptoms who had been missed by border screening, one person was finally reported as a probable SARS case, but without local transmission of the disease. The remaining 24 did not have SARS, as an alternative diagnosis fully explained their illnesses, or they did not have a convincing exposure to the disease.
Australia’s border entry screening program had a low identification rate of travellers symptomatic on arrival and later investigated for SARS. Possible reasons for this low rate included exit screening procedures in countries affected by SARS, the low prevalence of the disease (pre-test probability), and the use at Australian ports of screening procedures with a low sensitivity for detecting SARS cases. Although the screening program was based on WHO’s sensitive case definition of SARS, the screening procedures relied on subjective observations through self-report of symptoms or ad-hoc visual screening by flight crews and Customs staff at airports. Based on advice given through inflight announcements, passengers were expected to report symptoms of SARS, or previous contact with people with SARS. They may not have reported these to evade screening, or may not have heard or understood the inflight announcements. A study of international arrivals at Darwin airport 3 months into the SARS outbreak revealed that, of the 384 people interviewed who arrived from either Singapore, Denpasar or Brunei, 16% did not hear the announcements and a further 7% did not speak or understand English.9
The border screening procedures to identify SARS cases were strengthened in mid-June through the introduction of health declaration cards for all arrivals, and standardised procedures and algorithms for screening by nursing staff.10,11 However, screening may still have been ineffective, as it was possible for passengers to make false declarations, deny contact with people with SARS, or take antipyretic drugs to conceal fever. There have also been concerns about the utility of screening, as symptoms of SARS are vague and difficult to detect.12
Considering these limitations, is it still worth using a labour- and cost-intensive screening program for SARS or for other, similar transmissible diseases in the future? Although Singapore used health declaration cards and measured the temperature of each arriving passenger, only 136 (0.03% of all arrivals) were referred for further investigations, and none had SARS. Nonetheless, the authors reporting this considered this form of screening essential because of the high medical, social, economic and international impact of even one imported case of SARS.3 Similarly, the detection rates of people with SARS were extremely low in Hong Kong and Canada: Hong Kong referred 171 people for further investigation (0.001% of all arrivals) and identified two SARS cases, while Canada followed up 9100 people (0.001% of all arrivals) and did not identify any cases. Canada’s health authorities concluded that, unless the disease is present in the general population and can be detected by screening, screening is an expensive and potentially highly intrusive measure.1
Testing the temperature of departing passengers (exit screening) is important to prevent exporting SARS.13 By contrast, the role of testing the temperature of arrivals (entry screening) is less clear, and has not been recommended by WHO. However, this is probably an important component of the overall strategy for repeatedly emphasising to communities the determination of each country to control introduction of SARS.
The important lesson from the SARS experience is that transmission of the disease occurs, typically in the healthcare setting, from patients who are severely ill about 5 or more days after the onset of symptoms, and when infection control measures are lacking or inadequate.14 The other groups of people likely to be part of superspreading events are the elderly and those with chronic underlying diseases.13 These groups and their healthcare providers need to be particularly targeted when health messages concerning international travel are produced.
While border screening is one strategy to detect SARS, informing travellers about the risks of SARS and what to do if symptoms start after arrival in a country is of greater importance in containing the disease. As an example, a traveller who entered Canada symptom-free followed the instructions of the health notice closely when he subsequently developed symptoms consistent with SARS.1 He was reported as a probable case of SARS, but without secondary transmission of the disease.
The key lesson is that every country in this age of jet travel must be prepared to respond to the perpetual risk of emerging infections that will initially have an unknown potential for transmission. For new diseases, we need to be prepared to invest in objective screening measures, be capable of prompt implementation, and have the capacity to review the utility of the measures when knowledge about the disease develops.
For SARS, we have learnt that transmission of the disease occurs during the symptomatic phase of the illness, and that specific groups — including the elderly and those with underlying chronic diseases — are at high risk of transmitting disease. This knowledge empowers us to develop border programs that best manage the risk of disease spread.
1: Entry screening protocol to detect severe acute respiratory syndrome (SARS) at Australian airports, 5 April – 16 June 2003
2: Number and characteristics of travellers screened at Australian ports and referred to the Chief Quarantine Officer (CQO), by action taken, 5 April – 16 June 2003
Action taken by CQO |
No. of people |
History of previous exposure to SARS |
Fever on arrival |
Consistent with WHO case definition |
Outcome |
||||||
Hospitalised |
4 |
4 |
4 |
Suspected SARS case |
Alternative diagnosis (2); diagnosis undetermined, but not SARS (2) |
||||||
Placed under surveillance |
2 |
2 |
0 |
Not SARS |
No illness |
||||||
Released |
13 |
3 |
10 |
Not SARS |
Diagnosis undetermined, but not SARS |
||||||
SARS = severe acute respiratory syndrome. WHO = World Health Organization. |
|||||||||||
3: Number of travellers symptomatic on arrival and subsequently investigated for SARS, Australian SARS Case Register, 5 April – 16 June 2003
People investigated for SARS |
No. of people |
No. symptomatic on arrival in Australia |
No. detected by airport screening |
No. missed by airport screening |
|||||||
Investigated as probable SARS case |
13 |
5 |
0 |
5 |
|||||||
Investigated as suspected SARS case |
64 |
24 |
4 |
20 |
|||||||
Total |
77 |
29 |
4 |
25 |
|||||||
SARS = severe acute respiratory syndrome. |
|||||||||||
- Gina Samaan1
- Jenean Spencer2
- Leslee Roberts3
- Mahomed Patel4
- 1 Australian Department of Health and Ageing, Canberra, ACT.
- 2 National Centre for Epidemiology and Population Health, Australian National University, Canberra, ACT.
This research was supported by the Masters of Applied Epidemiology Program at the Australian National University and funded by the Australian Department of Health and Ageing.
None identified.
- 1. Health Canada. Learning from SARS: renewal of public health in Canada, October 2003. Available at: www.hc-sc.gc.ca/english/protection/warnings/sars/learning.html (accessed Nov 2003).
- 2. Hong Kong Department of Health. SARS in Hong Kong: from experience to action, October 2003. Available at: www.sars-expertcom.gov.hk/english/reports/reports.html (accessed Nov 2003).
- 3. Wilder-Smith A, Goh KT, Paton NI. Experience of severe acute respiratory syndrome in Singapore: importation of cases and defense strategies at the airport. J Travel Med 2003; 10: 259-262.
- 4. World Health Organization. WHO recommends new measures to prevent travel-related spread of SARS. Available at: www.who.int/csr/sars/archive/2003_03_27/en/ (accessed Dec 2003).
- 5. World Health Organization. WHO Global Conference on SARS, June 2003. Available at www.who.int/csr/sars/conference/june_2003/materials/report/en/ (accessed Nov 2003).
- 6. World Health Organization. Case definitions for surveillance of severe acute respiratory syndrome (SARS). Available at: www.who.int/csr/sars/casedefinition/en/ (accessed Nov 2003).
- 7. Australian Department of Health and Ageing. Interim Australian Infection Control Guidelines for SARS, May 2003. Available at: www.health.gov.au/sars/pdf/1_icg.pdf (accessed Dec 2003).
- 8. World Health Organization. Cumulative number of reported probable cases of SARS. Available at www.who.int/csr/sars/country/en/ (accessed Dec 2003).
- 9. Webby R, Krause V. Evaluation of SARS audit at Darwin International Airport. Northern Territory Disease Control Bulletin 2003; 10: 8-10.
- 10. Australian Department of Health and Ageing. New information cards introduced to safeguard Australia from SARS, June 2003. Available at: www.health.gov.au/mediarel/yr2003/kp/kp03090.htm (accessed Dec 2003).
- 11. Australian Department of Health and Ageing. International airport procedures for public health nurse referrals, June 2003. Available at: www.health.gov.au/sars/pdf/nurse.pdf (accessed Nov 2003).
- 12. Cameron PA, Rainer TH, De Villiers Smit P. The SARS epidemic: lessons for Australia. Med J Aust 2003; 178: 478-479. <MJA full text>
- 13. Peiris JSM, Yuen KY, Osterhaus AD, Stohr K. The severe acute respiratory syndrome. N Engl J Med 2003; 349: 2431-2441.
- 14. World Health Organization. Department of Communicable Disease Surveillance and Response. Consensus document on the epidemiology of severe acute respiratory syndrome (SARS). Geneva: WHO, 2003. (WHO/CDS/CSR/GAR/2003.11.) Available at: www.who.int/csr/sars/en/WHOconsensus.pdf (accessed Dec 2003).





Abstract
Objective: To assess the effectiveness of the Australian border entry screening program to detect arriving travellers with symptoms of severe acute respiratory syndrome (SARS).
Design and setting: Descriptive study of outcomes of screening at Australian airports and seaports between 5 April 2003 and 16 June 2003. To determine the number of international travellers who were symptomatic on arrival in Australia but missed by screening, data were obtained on the number of arrivals screened and the number with symptoms (from the Australian Quarantine and Inspection Service [AQIS]), as well as the number of people investigated for SARS (from the Australian SARS Case Register).
Results: There were 1.84 million arrivals into Australia during the study period, and 794 were referred for screening to AQIS staff. Of these, the findings in four travellers were consistent with the World Health Organization case definition for SARS, and they were referred by the Chief Quarantine Officers to designated hospitals for further investigation. None of these people was confirmed to have SARS. One person reported as a probable SARS case acknowledged being symptomatic on arrival, but had been missed by border screening.
Conclusions: The low identification rate was attributed to the low prevalence of SARS, the use of exit screening by affected countries, and the subjective measures used in the screening process. With current knowledge about SARS, border screening should focus on educating incoming travellers, especially groups at high risk of transmitting the disease (the elderly and those with underlying chronic illnesses). Objective screening measures should be used during SARS outbreaks to prevent importation of the disease.