The roles of clinician, educator and researcher have traditionally been central pillars of the discipline of medicine. The synergy created by combining these roles adds value to all three, facilitating high-quality teaching, clinically relevant research and evidence-based practice.1-3 However, current trends in Australia are placing pressure on the sustainability of academic medicine, and on the traditional ways of delivering medical education and undertaking medical research.
Demand for medical educators is increasing because of both rising numbers of medical students and changed models of education. Between 2005 and 2012, the number of graduates from Australian medical schools will grow by 81%, with 12 new medical programs commencing since 2000.4 Although there is neither evidence nor consensus about how to estimate the size of the academic medical workforce that will be needed,5 it is clear that increased medical school intakes will necessitate more medical academics. In the United Kingdom, data on medical academic staff have been collected annually since 2000 by the Medical Schools Council6 (the UK equivalent of Medical Deans Australia and New Zealand). The Association of American Medical Colleges maintains a similar collection for the United States.7 In Australia, a standardised national dataset for education and research capacity would provide clearer guidance on academic workforce needs.
In 2006 (latest available data), there were 650 Australian medical practitioners whose primary role was medical educator, representing around 1% of the total medical workforce.8 This represents an increase of 222 (52%) since 2000.9 During the same period, the total medical workforce grew by 22%, while the number of enrolled medical students increased by 40%.8-10 With seven new medical programs commencing in 2007 and 2008, creating increases in the order of 20% on 2006 student numbers, we expect a continued need for growth of the medical education workforce.
Most of the newer medical schools use a problem-based learning approach, and many existing medical schools have also shifted to this model. Based on small-group teaching and adult learning theory,11 it is a resource-intensive method, requiring higher staff–student ratios than traditional lecture-based methods, further increasing academic medical workforce requirements.
The need for greater resources to meet student demand extends beyond universities. Medical practitioners whose primary role is clinical have always played a significant part in teaching and research. In 2006, 20% of medical practitioners with a primary clinical occupation reported providing some medical education.12 Over a third of specialists were involved in education (36%), along with 18% of specialists-in-training, 10% of primary care clinicians and 8% of hospital non-specialists. For clinicians who provided medical education, the average time spent was 4.7 hours per week.8
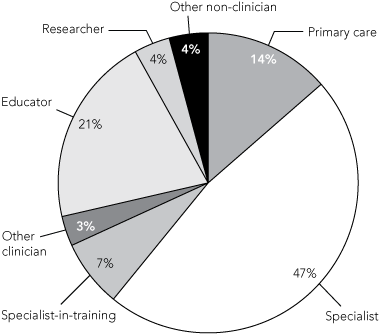
Because the clinical medical workforce is much larger than the medical education workforce, the contribution of clinicians to medical education in terms of total time spent is substantial. In 2006, clinicians provided almost three-quarters of total medical teaching hours — specialists provided almost half (47%), and primary care clinicians provided 14% (Box 1). Available data do not indicate the stage of education provided (student, intern or registrar), but this probably varies between specific clinical and non-clinical medical occupations. Many clinicians involved in education have honorary appointments. Yet, the system of adjunct or honorary appointments, which has been an important contributor to university medical programs, is highly variable and often lacks transparency and clear expectations.13
However, with greater numbers of students needing clinical placements, clinicians are struggling to cope. Furthermore, many sectors of the Australian medical workforce, such as general practice, are currently experiencing workforce shortages, which are expected to continue.14,15 These shortages strain the capacity of clinicians to meet the demand — pressured clinicians are likely to prioritise provision of clinical services over the less urgent demands of teaching and, particularly, research.16
Training no longer takes place exclusively, or even predominantly, in the public hospital sector. This shift is a result of both lack of capacity within traditional settings and changing patterns of clinical service delivery. As the burden of disease shifts to chronic conditions,17 and length of stay in acute settings decreases,18 primary care and ambulatory settings become increasingly prominent. Private-sector settings are being used more for training, but the mechanisms to support and recognise teaching by clinicians vary significantly across these settings.
Teaching functions in public hospitals are funded by a complex mix of sources, including general state government hospital funding, state and federal government funding for vocational trainee positions, and specific funding agreements with individual universities for medical students. General practitioners are eligible for teaching activity payments through the Practice Incentives Program, and about one in five Australian general practices currently claim this incentive.19 Medical specialists have no equivalent program to support teaching activities within their own private practices. The interim report of the National Health and Hospitals Reform Commission (NHHRC) noted that many contributions to medical education receive little explicit resourcing or acknowledgement.16
Support for research is even more limited, and medical research is more divorced from clinical settings than medical education. The core medical research workforce, which in 2006 comprised 1149 medical practitioners,8 was responsible for just over half of all estimated research time in that year.12 Only 7% of clinicians reported undertaking research in 2006.12 Specialists had the highest proportion involved (15%), compared with 8% of specialists-in-training, and negligible numbers of primary care clinicians (1%) and hospital non-specialists (2%). The average time spent in medical research by clinicians who undertook this work was 6.6 hours per week in 2006.
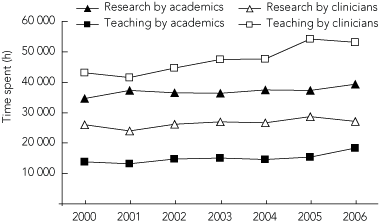
The demands of service delivery and changed funding models in public hospitals are straining the capacity of clinicians to undertake education and research.20 Data from the Australian Institute of Health and Welfare suggest that both the teaching hours and research hours of clinicians are decreasing. Total teaching hours for clinicians, which increased between 2000 and 2005 due to increased numbers of clinicians and slight increases in average hours per week, dropped in 2006, when lower proportions of all clinical occupations reported involvement in education compared with 2005 (Box 2). Total research hours for clinicians changed little between 2000 and 2005, and then decreased slightly in 2006, again attributable to lower proportions of clinicians involved. Although these data raise the possibility of a downward trend in the amount of academic work being done by clinicians, more detailed data collection and analysis are warranted.
The changes described above are putting pressure on the traditional model for educating successive generations of doctors and the sustainability of academic medicine. Although the consequences of deteriorating academic capacity within the medical workforce may be less immediately obvious than deficits in clinical capacity, they are still important. Ongoing programs of clinically relevant research are essential for continued improvements in the quality, efficacy and efficiency of health service delivery.16,20 More broadly, a strong and productive academic sector is at the core of maintaining and developing all disciplines in medicine.
We have identified a range of strategies that could be implemented by universities, health providers and governments to ensure an adequate medical academic workforce and a sustainable, quality medical education system (Box 3). The importance of a coordinated approach cannot be overemphasised, given the current lack of integration between stages of medical education; the multiplicity of funding sources, accreditation authorities, and individual arrangements within and between institutions such as universities and hospitals; and the lack of career pathways for medical researchers and educators.13,27
Unless medical education and research work are perceived as being valued, they are at risk of erosion. Recognition can be achieved by quarantined time, or through payment structures at all levels — from individual payment mechanisms for private providers through to funding agreements for hospitals — that recognise and reward education and research work. In light of recent observations that financial incentives can engender more business-style relationships in medicine,28 it is important that arrangements support, rather than undermine, traditional professional values and roles. The NHHRC interim report presents specific proposals to improve and embed supports for research and teaching by clinicians, including activity-based payments, research networks, health service reporting on research activity, and enhancement of existing programs, such as clinical research fellowships. A UK academic described recent developments in the UK to improve translational clinical research capacity, noting that Australia currently lacks a strategic approach.29
Targeted support for academic departments of general practice has been proposed as an important strategy to ensure future sustainability and relevance of academic medicine,30 and the NHHRC interim report proposes specific support for clinical education in underdeveloped settings,16 which, on the basis of our data, would include general practice. The Primary Health Care Research, Evaluation and Development Strategy has succeeded in increasing the publication output of general practice, but it remains a fraction (2%–5%) of the publication output of specialist medicine.31 The presence of general practice within the academic medical workforce and the capacity of primary care clinicians to contribute to research and education should be further strengthened as a key strategy to sustain the academic workforce.
1 Proportion of total time spent on medical education in Australia, by main occupation, 2006*
 | |||||||||||||||
|
* Total time spent on medical education was calculated from national medical labour force survey data as follows: the average number of hours per week spent in medical education (stratified by main occupation)8 was multiplied by the estimated number of medical practitioners in each occupation group who provided at least 1 hour per week of education (the latter calculated from the proportion in each occupation who reported undertaking medical education12 and the benchmark medical workforce numbers for 20068). | |||||||||||||||
2 Total time spent on medical teaching and research by academics (medical educators and researchers) and clinicians in Australia, 2000–2006*
 | |||||||||||||||
|
* Data were derived from references 8, 12 and 21–25. See also footnote to Box 1. | |||||||||||||||
3 Strategies to support and enhance medical education and research
Clinical academic workforce “thinktank”: As part of the new national health workforce agency,26 convene a working group to ensure a coordinated, systematic approach to development and enhancement of the academic medical workforce, with the establishment of monitoring systems for the clinical academic workforce as a first task.
Capital support: Provide funding support for capital or infrastructure developments as required to ensure there are adequate teaching facilities in both major clinical teaching sites and private clinics.
- Catherine M Joyce1
- Leon Piterman2
- Steven L Wesselingh3
- Monash University, Melbourne, VIC.
None identified.
- 1. Wilkinson D, Ward RL. International Campaign to Revitalise Academic Medicine (ICRAM): what does it mean for Australia? Med J Aust 2004; 181: 658-659. <MJA full text>
- 2. DeAngelis CD. Professors not professing. JAMA 2004; 292: 1060-1061.
- 3. International Working Party to Promote and Revitalise Academic Medicine. ICRAM (the International Campaign to Revitalise Academic Medicine): agenda setting. BMJ 2004; 329: 787-789.
- 4. Joyce CM, Stoelwinder JU, McNeil JJ, Piterman L. Riding the wave: current and emerging trends in graduates from Australian university medical schools. Med J Aust 2007; 186: 309-312. <MJA full text>
- 5. International Working Party to Promote and Revitalise Academic Medicine. Academic medicine: the evidence base. BMJ 2004; 329: 789-792.
- 6. Aldridge J, Fitzpatrick S. Clinical academic staffing levels in UK medical schools as at 31 July 2007. London: Medical Schools Council (UK), 2008.
- 7. Association of American Medical Colleges. Diversity in medical education: facts and figures 2008. Washington, DC: AAMC, 2008.
- 8. Australian Institute of Health and Welfare. Medical labour force 2006. Canberra: AIHW, 2008. (AIHW Cat. No. HWL 42.)
- 9. Australian Institute of Health and Welfare. Medical labour force 2000. Bulletin no. 5. Canberra: AIHW, 2003. (AIHW Cat. No. AUS 33.)
- 10. Medical Training Review Panel. Eleventh report. Canberra: Australian Government Department of Health and Ageing, 2007.
- 11. Wood DF. Problem based learning [editorial]. BMJ 2008; 336: 971.
- 12. Australian Institute of Health and Welfare. Number of employed medical practitioners by main occupation and medical role (for practitioners reporting at least 1 hour per week in the medical role), 2000–2006 [custom dataset extracted from national medical labour force surveys]. Canberra: AIHW, 2008.
- 13. Rane A, de Costa C. Why would anyone be an academic [letter]? Med J Aust 2007; 187: 374-375. <MJA full text>
- 14. Brooks PM, Lapsley HM, Butt DB. Medical workforce issues in Australia: “tomorrow’s doctors — too few, too far”. Med J Aust 2003; 179: 206-208. <MJA full text>
- 15. Joyce CM, McNeil JJ, Stoelwinder JU. More doctors, but not enough: Australian medical workforce supply 2001–2012. Med J Aust 2006; 184: 441-446. <MJA full text>
- 16. National Health and Hospitals Reform Commission. A healthier future for all Australians. Interim report. Canberra: Commonwealth of Australia, 2008.
- 17. Australian Institute of Health and Welfare. The burden of disease and injury in Australia 2003. Canberra: AIHW, 2007. (AIHW Cat. No. PHE 82.)
- 18. Australian Institute of Health and Welfare. Australian hospital statistics 2006–07. Canberra: AIHW, 2008. (AIHW Cat. No. HSE 55.)
- 19. Medicare Australia. Practice Incentives Program statistics reports. https://www.medicareaustralia.gov.au/statistics/div_gen_prac.shtml (accessed Dec 2008).
- 20. Penington DG. Rediscovering university teaching hospitals for Australia. Med J Aust 2008; 189: 332-335. <MJA full text>
- 21. Australian Institute of Health and Welfare. Medical labour force 2005. Canberra: AIHW, 2008. (AIHW Cat. No. HWL 41.)
- 22. Australian Institute of Health and Welfare. Medical labour force 2004. Canberra: AIHW, 2006. (AIHW Cat. No. HWL 39.)
- 23. Australian Institute of Health and Welfare. Medical labour force 2003. Canberra: AIHW, 2005. (AIHW Cat. No. HWL 32.)
- 24. Australian Institute of Health and Welfare. Medical labour force 2002. Canberra: AIHW, 2004. (AIHW Cat. No. HWL 30.)
- 25. Australian Institute of Health and Welfare. Medical labour force 2001. Canberra: AIHW, 2003. (AIHW Cat. No. HWL 28.)
- 26. Council of Australian Governments’ meeting 29 November 2008. http://www.coag.gov.au/coag_meeting_outcomes/2008-11-29/index.cfm (accessed May 2009).
- 27. McGrath BP, Graham IS, Crotty BJ, Jolly BC. Lack of integration of medical education in Australia: the need for change. Med J Aust 2006; 184: 346-348. <MJA full text>
- 28. Hartzband P, Groopman J. Money and the changing culture of medicine. N Engl J Med 2009; 360: 101-103.
- 29. Byrne E. Clinical research in the United Kingdom: a new era [editorial]. Med J Aust 2009; 190: 172-173. <MJA full text>
- 30. Newton WP, DuBard CA. Shaping the future of academic health centers: the potential contribution of departments of family medicine. Ann Fam Med 2006; 4 Suppl 1: S2-S11.
- 31. Askew DA, Schluter PJ, Gunn JM. Research productivity in Australian general practice: what has changed since the 1990s? Med J Aust 2008; 189: 103-104. <MJA full text>





Abstract
Demand for medical education is increasing, and clinicians are struggling to maintain involvement in teaching and research activities.
The settings of clinical training are changing and diversifying.
The traditional model of medical education and the sustainability of academic medicine are under strain.
Better support is required to ensure continued integration of research and education with clinical activities.
Better coordination is required to overcome fragmentation within the medical education system, to ensure appropriate recognition for teaching and research across all clinical settings.