Northern Queensland has been in the vanguard of trends to regionally based medical education in Australia. The first new Australian medical school in over 20 years was established at James Cook University (JCU) in 2000, producing its first graduates in 2005.1 JCU’s 6-year undergraduate program is entirely regional, involves at least 20 weeks of clinical placement per student in small communities, and has an emphasis on rural, remote, Indigenous and tropical health.2,3 With medical student numbers doubling nationally, and many new medical schools having been established since 2000, educators are looking to develop new clinical teaching sites and opportunities.4,5 Evidence supports the success of the “rural pipeline”, recruiting rural students through rurally based education into postgraduate training.6 Academic performance of rurally based students remains strong, and interest in rural careers and regional internships is rising.7,8 However, increased demand for rural teaching placements has not yet been accompanied by increases in the rural workforce and the capacity to train students.
Before the establishment of the JCU medical school, northern Queensland had an existing vertically integrated training system for general practice and rural medicine, and an established network of teaching practices.9 Since 2000, the region has had to rapidly accommodate increasing numbers of medical students in a health system simultaneously facing the challenges of meeting the clinical demands of a growing population in the context of a national health workforce shortage.
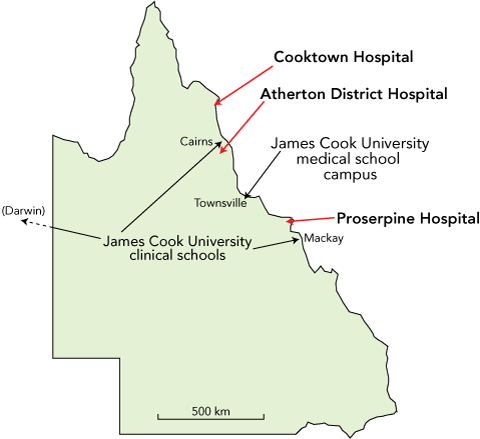
Two rural hospitals, in Atherton and Proserpine, have provided notable leadership in meeting the challenges of increasing teaching capacity. Other hospitals, such as Cooktown Hospital, are developing similar models. The locations of the three hospitals (Atherton, Proserpine and Cooktown) are shown in Box 1, and a comparison of their features is shown in Box 2. We believe the local experiences of the health care providers at these rural hospitals in evolving their clinical services into a “teaching health care system” are instructive. In this article, we describe the development of these services, their impact on capacity to teach and deliver health care services, and the long-term implications for workforce, planning and policy at these sites and elsewhere.
Medical students at JCU are predominantly school-leavers, and most are from non-metropolitan backgrounds. In their early years, they are based in Townsville, but in Years 5 and 6, they attend clinical schools in Mackay, Townsville, Cairns and Darwin (in the Northern Territory). All students are given early clinical exposure and undertake 20 weeks of rural placements.10 The three rural placements during the course offer a broad choice of locations and different sequenced learning objectives, including experiencing rural health care (Year 2), clinical skills and pathology (Year 4), and taking more responsibility for clinical care in the Year 6 rural internship.3,10
On the basis of previous experience, and of formal evaluations performed for the Rural Undergraduate Support and Coordination (RUSC) program,11 JCU medical school identified three key elements of successful rural clinical placements: student accommodation and teaching space, committed clinical teachers, and an appropriate caseload. Each leg of this “three-legged stool” is considered critical — if any one is missing, the placement will “fall over”. As student placements were developed, infrastructure was progressively secured while academic staff provided preceptor support.
The rural hospitals in Atherton and Proserpine have successfully implemented models allowing them to increase their teaching capacity, and case studies of these two hospitals are provided. A glimpse of Cooktown Hospital’s journey toward becoming a rural teaching facility is described in a brief personal perspective by its Medical Superintendent (Box 3).
The Atherton District Hospital has a long history of having skilled, enthusiastic rural doctors committed to the community and to teaching. More recently, excellent clinical care, medical leadership and coordination of local resources enabled the development of a functional generalist rural hospital with quality staff focused on collaborative education, audit and excellence in clinical care within the local community.13 This led a transition to a stable workforce with high rates of staff retention.
During the 1990s, the reform of general practice training and establishment of new Australian Government rural health programs, including RUSC and Rural Health Support, Education and Training,5 enabled the development of local practical relationships between key organisations, including Queensland Health, the regional general practice training provider (Tropical Medical Training), JCU, the local Division of General Practice, local government, and practising rural doctors. The provision of administrative support, together with clinical backfill (external funds provided to cover the clinical duties of the Medical Superintendent while he undertook teaching and administrative roles) facilitated development of Atherton Hospital’s teaching capacity. A practical, apprenticeship-style vertical teaching cascade was gradually developed. This evolved to include:
high school mentoring;
placements for JCU students in multiple years;
placements for students from other medical schools (includes elective, John Flynn Placement Program, and bonded students);
interns, general practice registrars and rural generalist (ie, vocationally trained doctors skilled in primary care, procedural and extended skills, emergency medicine and public health) trainees;
overseas-trained doctors; and
rotating medical registrars.
1 Locations of the three rural hospitals, and the James Cook University medical school campus and clinical schools
2 Comparison of three rural hospitals that are or are becoming teaching health services
- Tarun K Sen Gupta1
- Richard B Murray1
- Neil S Beaton2
- David J Farlow3
- Clare B Jukka1,2
- Natasha L Coventry4
- 1 School of Medicine and Dentistry, James Cook University, Townsville, QLD.
- 2 Atherton District Hospital, Atherton, QLD.
- 3 Whitsunday Health Service, Proserpine, QLD.
- 4 Cooktown Multipurpose Health Service, Cooktown, QLD.
None identified.
- 1. Hays RB, Wronski I, Veitch J, McCloskey T. Intern choices for the first graduates of the James Cook University [letter]. Med J Aust 2006; 184: 94. <MJA full text>
- 2. Hays RB. Rural initiatives at the James Cook University School of Medicine: a vertically integrated regional/rural/remote medical education provider. Aust J Rural Health 2001; 9 Suppl 1: S2-S5.
- 3. Sen Gupta TK, Murray RB, McDonell A, et al. Rural internships for final year students: clinical experience, education and workforce. Rural Remote Health [Internet] 2008; 8: 827. Epub 2008 Feb 13.
- 4. Eley DS, Baker PG. Will the Australian rural clinical schools be an effective workforce strategy? Early indications of their positive impact on intern choice and rural career interest. Med J Aust 2007; 187: 166-167. <MJA full text>
- 5. Eley DS, Young L, Wilkinson D, et al. Coping with increasing numbers of medical students in rural clinical schools: options and opportunities. Med J Aust 2008; 188: 669-671. <MJA full text>
- 6. Murray RB, Wronski I. When the tide goes out: health workforce in rural, remote and Indigenous communities. Med J Aust 2006; 185: 37-38. <MJA full text>
- 7. Worley P, Strasser R, Prideaux D. Can medical students learn specialist disciplines based in rural practice: lessons from students’ self-reported experience and competence. Rural Remote Health [Internet] 2004; 4: 338. Epub 2004 Nov 23.
- 8. Eley D, Baker P. Does recruitment lead to retention? — Rural Clinical School training experiences and subsequent intern choices. Rural Remote Health [Internet] 2006; 6: 511. Epub 2006 Feb 3.
- 9. Hays RB, Sen Gupta T, Arlett K. Integrating general practice medical education — the North Queensland model. Med J Aust 1994; 160: 388-389.
- 10. James Cook University Australia. Faculty of Medicine, Health and Molecular Sciences. Our programs. http://www.jcu.edu.au/medicine/programs/index.htm (accessed Jun 2009).
- 11. Sen Gupta TK, Gupta S, Jukka C, et al. Going bush — a chance of a lifetime. Key factors in ensuring the quality of 4- and 8-week rural placements for medical students. Report to the Rural Undergraduate Support and Co-ordination Program. Canberra: Australian Government Department of Health and Ageing, 2004.
- 12. Queensland Health. Physician’s Assistant Pilot Program in Queensland. http://www.health.qld.gov.au/pa/ (accessed Jun 2009).
- 13. Beaton NS, Nichols A, McLellan T, et al. Regionalisation of rural medical training in Far North Queensland: a learning experience for medical educators and managers. Aust J Rural Health 2001; 9 Suppl 1: S32-38.






Abstract
Major developments in medical education in Australia include increasing the numbers of students and educating more students within the community and in regional, rural and remote settings.
Rapid growth of student numbers and the rural orientation of the James Cook University medical school course has meant that northern Queensland had to deal with these issues earlier than other regions.
One solution has been to transform some rural hospitals into teaching health services.
Two hospitals that have successfully made this transformation, and another on its way, suggest that important factors include local commitment to quality clinical services, medical and academic leadership, coordination of local resources, community support, and strategic links between key organisations.
Transformation to a teaching health service involves senior doctors functioning as true consultants with cascading supervision as in the traditional consultant–registrar–resident model. As both clinical and teaching capacity develops, the workforce may stabilise, infrastructure and teaching culture are established, and long-term recruitment and retention strategies emerge.
Applying these models in other rural and community settings may make it possible to manage the increased training capacity and address workforce needs without compromising the educational experience — indeed, it may be enhanced.