Rural clinical schools are now established through federal funding in most medical schools in Australia,1 and are required to provide 25% of medical students with at least 50% of their clinical training. A major expectation is that this will encourage rural medical workforce recruitment and retention.1
The rural clinical school at the University of Queensland (UQRCS), established in 2002, is part of the School of Medicine’s 4-year graduate MB BS program. Year 4 students may elect to train in the Central or Southern (capital city) Divisions, or the Rural Division, comprising teaching sites throughout regional and rural central and south-west Queensland. This report presents an update on how the UQRCS is addressing the need to prepare and encourage its students to enter rural medical practice.
University of Queensland Year 4 MB BS students undertook their entire fourth year (2006) of clinical training in the UQRCS. Two questionnaires, the entry survey (administered at the start of Year 4) and exit survey (end of Year 4) were developed or modified (2003–2005) to capture the most important variables related to choosing rural medicine as a career.2
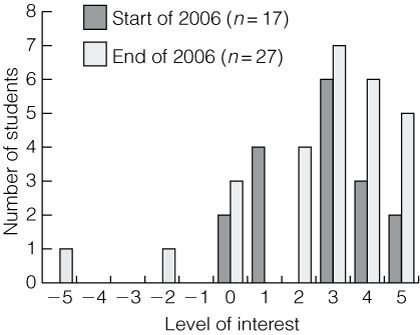
Likewise, the exit survey asked, How did your year at the UQRCS alter your interest in pursuing a rural medicine career? Using a similar 11-point scale of − 5 to − 1 (discouraged my interest) to +1 to +5 (encouraged my interest) with a midpoint of no change, only two students registered discouragement. Twenty-two were encouraged and three reported no change. Box 1 shows the trend toward a positive effect of the UQRCS on interest in a future rural medicine career.
On exit, the most important factors related to choosing to study at the UQRCS were the quality of teaching, level of student–teacher contact, and high patient access (Box 2). Availability of free accommodation also ranked highly, as did rurality (location) of the UQRCS.
Evidence is mounting in support of a strong relationship between rural educational exposure and an increased interest in pursuing a rural career or selecting a rural internship.4 Students’ choice of internship location (urban hospital versus regional or rural hospital) is an important indication of their desire to pursue rural medicine.
Most of our cohort was of urban origin, a feature noted in other rural clinical schools or programs with a rural focus.2 There is strong evidence for a relationship between geographical background and predictors of practice locality,5,6 but studies have identified that up to 74% of rural doctors have an urban background.6 This illustrates the important role that rural clinical schools play in developing and encouraging an interest in rural medicine among students of both urban and rural backgrounds.
1 Effect of the University of Queensland rural clinical school over the year on Year 4 students’ interest in pursuing a career in rural medicine
 | |||||||||||||||
2 Important factors in choosing to study at the University of Queensland rural clinical school (UQRCS)
How important were the following factors in your decision to study at the UQRCS? |
Frequency distribution of student responses |
||||||||||||||
- Diann S Eley1
- Peter G Baker2
- School of Medicine Rural Clinical Division, University of Queensland, Toowoomba, QLD.
None identified.
- 1. Australian Government Department of Health and Ageing. Rural clinical schools program. http://health.gov.au/clinicalschools (accessed Jun 2007).
- 2. Eley D, Baker P. Does recruitment lead to retention? Rural clinical school training experiences and subsequent intern choices. Rural Remote Health [Internet] 2006; 6: 511. http://www.rrh.org.au/articles/defaultnew.asp?Issue No=6x (accessed Jun 2007).
- 3. Australian Rural and Remote Workforce Agencies Group. Review of the Rural and Remote Metropolitan Areas Classification System. A submission to the Department of Health and Ageing. Melbourne: ARRWAG, 2005. http://www.arrwag.com.au/client_images/84169.pdf (accessed Mar 2007).
- 4. Tolhurst HM, Adams J, Stewart SM. An exploration of when urban background medical students become interested in rural practice. Rural Remote Health [Internet] 2006; 6: 452. http://www.rrh.org.au/articles/defaultnew.asp?Issue No=6x (accessed Jun 2007).
- 5. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Aust J Rural Health 2003; 11: 277-284.
- 6. Wilkinson D, Laven G, Pratt N, Beilby J. Impact of undergraduate and postgraduate rural training, and medical school entry criteria on rural practice among Australian general practitioners: a national study of 2414 doctors. Med Educ 2003; 37: 809-814.





Abstract
Objective: To use short-term indicators (hospital internship choice, and interest in a future rural career) to assess how the University of Queensland rural clinical school is meeting its program objectives.
Design: Cross-sectional quantitative data collected through self-report questionnaires.
Setting: University of Queensland rural clinical school (UQRCS).
Participants: Year 4 students who attended the UQRCS for their entire clinical year in 2006.
Results: Most students were from an urban background. Over the year, interest in a future rural medical career increased measurably across the cohort. The most important factors in choosing to study at the UQRCS were the quality of teaching, level of student contact with clinical teachers, increased patient access, and accommodation facilities. Comparison of graduates’ choice of internship location for 2006 compared with 2005 showed a trend away from urban or metropolitan toward regional or rural hospitals.
Conclusions: Our results suggest that the primary attraction of UQRCS is the quality of education, and rural undergraduate training is a popular choice for urban students. Although the long-term effect on rural medical workforce remains to be determined, the trend at UQRCS of new graduates choosing non-urban internships is encouraging.