In 1994, it was reported that the risk of mother-to-child transmission of HIV is substantially reduced by treating the mother during pregnancy and delivery, and the infant after birth, with zidovudine.1 The use of highly active antiretroviral therapy (HAART) during pregnancy has reduced the risk even further.2 Delivery by elective caesarean section is also associated with lower transmission risk than vaginal delivery.3 Observational studies indicate that a mother-to-child transmission rate of less than 0.5% can be achieved for non-breastfed children whose mothers have an undetectable viral load at term through use of HAART during pregnancy and delivery.4-8
Previous reports of the pattern of perinatal exposure to HIV in Australia indicate increasing use of antiretroviral therapy during pregnancy and avoidance of breastfeeding by women diagnosed with HIV infection before delivery.9-11 Here, we describe the pattern and outcome of perinatal HIV exposure in children born in Australia, including those born during the HAART era.
Children born to women with diagnosed HIV infection were notified from 1982 to a national registry of perinatal exposure to HIV through an informal network of clinicians coordinated by the Sydney Children’s Hospital, and, from May 1993, by paediatricians through the Australian Paediatric Surveillance Unit (APSU), using previously described methods.12 Cases were also notified after retrospective assessment of perinatal HIV exposure among children born to women with new diagnoses of HIV infection from July 1995.9,10
the child was diagnosed with HIV infection;
the mother was documented as having acquired HIV infection on a specified date before 1985 following receipt of HIV-infected blood or tissue;
the mother’s HIV infection was diagnosed in an antenatal specimen or dried blood spots collected through newborn screening programs; or
the mother had a documented history of exposure on a specified date, either before the birth or while breastfeeding.
Newly diagnosed HIV infections, including diagnoses of mother-to-child transmission and AIDS in children, are notifiable in Australia.13 Diagnoses are based on standardised laboratory tests and procedures.14 An exposed child was confirmed to be without infection if HIV antibody testing of a specimen from the child at age 18 months or older gave a negative result. From 1998, the absence of HIV infection was also diagnosed using polymerase chain reaction (PCR) testing for detection of HIV RNA.
before 1994, avoidance of breastfeeding alone;4
from 1994, avoidance of breastfeeding plus antiretroviral therapy during pregnancy and delivery, and treatment of the newborn;1,2 and
from 1999, delivery by elective caesarean section in addition to other interventions, if appropriate.3
Rates of perinatal HIV exposure by state/territory and year of the child’s birth were age-standardised, using the Australian population of women aged 15–49 years who delivered a live baby in 2001 as the standard.15 Rates of perinatal HIV exposure were also age-standardised by the mother’s region of birth using the population of Australian-born women in 2001 as the standard.16 The pattern of perinatal HIV exposure was assessed by year of the child’s birth, timing of the mother’s HIV diagnosis with respect to the child’s birth, and use of interventions by women diagnosed antenatally.
The age-standardised rate of perinatal HIV exposure in Australia increased from 2.3 per 100 000 live births in 1982–1986 to 8.3 per 100 000 live births in 2003–2006 (Box 1). Between 1995 and 2006, the exposure rate was stable for children of Australian-born women (0.2 per 100 000 live births). However, it increased for children of women born elsewhere in Oceania and in high-prevalence countries in South-East Asia (to 1.1 and 1.3 per 100 000 live births, respectively, in 2003–2006), and particularly for children of women born in high-prevalence countries in sub-Saharan Africa (to 9.3 per 100 000 in 1999–2002, dropping slightly to 7.4 per 100 000 in 2003–2006).
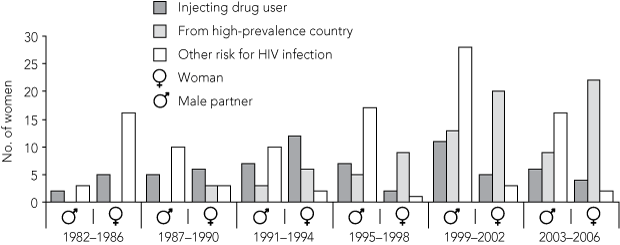
Sources of maternal HIV exposure are shown in Box 2. For women whose first exposed child was born in Australia in 1982–1986, the predominant source of exposure was receipt of HIV-infected blood or tissue before 1985 (16 of 26 women). In contrast, for those whose first exposed child was born in 2003–2006, heterosexual contact — in Australia or overseas — was the most frequent source (31 of 59 women). This included nine women who reported having a partner from a high-prevalence country, mostly in sub-Saharan Africa), and an increasing number who reported heterosexual contact in Australia with a partner with an HIV risk factor other than coming from a high-prevalence country or injecting drug use. Twenty-two women came from a high-prevalence country (12 from sub-Saharan Africa and seven from South-East Asia). Among 19 Aboriginal and Torres Strait Islander women, HIV exposure was attributed to heterosexual contact (17) or injecting drug use (2).
The mother had an antenatal HIV diagnosis in 75% of reported cases of perinatal exposure in children born in Australia 1982–2006, including 21 of the 25 children (84%) born to Indigenous mothers. The percentage of mother–child pairs with an antenatal diagnosis increased significantly over time (P < 0.001), from 11% in 1982–1986, to 66% in 1991–1998, and 98% in 2003–2006 (Box 3).
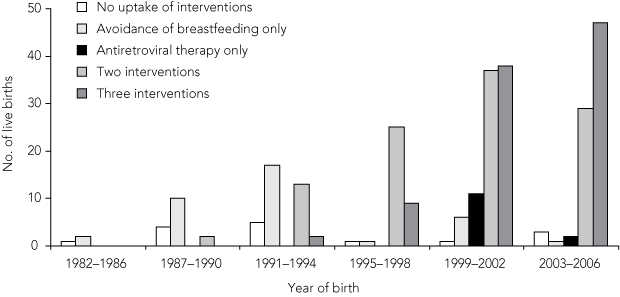
Uptake of interventions by women with an antenatal diagnosis is shown in Box 4. Avoidance of breastfeeding was the only intervention used by 52% of women (29/56) whose child was born in 1982–1994. Use of antiretroviral therapy during pregnancy plus avoidance of breastfeeding more than doubled, from 30% (11/37) in 1991–1994 to 69% (25/36) in 1995–1998, and then declined, as the use of three interventions steadily increased — from 5% (2/37) in 1991–1994, to 57% (47/82) in 2003–2006.
Mother-to-child transmission rates for women with an antenatal diagnosis, by uptake of interventions to minimise transmission are shown in Box 5. Transmission occurred in 47% of children (7/15) born to women who reported using no interventions, and 24% (9/37) whose mothers reported avoiding breastfeeding alone. Rates were much lower in children of women who used two interventions (4%; 4/106) or all three interventions (2%; 2/96). In the six cases where transmission occurred despite use of two or three interventions, the duration of antiretroviral therapy during pregnancy was 3 months or less. No cases of mother-to-child transmission occurred among 21 children born to Indigenous women diagnosed antenatally, including 15 whose mother used at least two interventions.
Among children born to women with a postnatal HIV diagnosis, the mother-to-child transmission rate remained high over the period 1982–2006, in comparison with the rate among women diagnosed antenatally (Box 3). Most of these women reported breastfeeding (62/72; 86%). Most were born in Australia (57; 66%), with smaller numbers born in high-prevalence countries (13; 15%) or another country (16; 19%).
Cases of perinatal HIV exposure were initially reported through a network of HIV specialists. In 1993, reporting was expanded to include a national network of paediatricians, coordinated by the APSU. Because only a small number of specialists manage pregnancy in women diagnosed with HIV infection in Australia, or refer exposed children to paediatricians, APSU reporting is thought to be a reliable indicator of trends in perinatal HIV exposure among women with an antenatal HIV diagnosis. Among women with a postnatal diagnosis, the increasing rate of mother-to-child transmission over time suggests underreporting or underdiagnosis of perinatal exposure that does not result in infection. If mother-to-child transmission occurs in 16% of exposed children who are breastfed,17 and 39 cases of infection have been diagnosed among 86 exposed children of mothers with a postnatal diagnosis, then an estimated 160 additional children have been exposed but not infected, bringing the total number of exposed children born in Australia by December 2006 to around 515.
The substantial increase in the population rate of perinatal HIV exposure from 1999 coincided with increases in the population of women of childbearing age from countries with high HIV prevalence in sub-Saharan Africa and South-East Asia. The percentage of the Australian population of women of childbearing age who were born in countries in sub-Saharan Africa and South-East Asia increased from 0.6% and 2.9%, respectively, in 1996, to 1.0% and 3.3%, respectively, in 2006.16 The substantially higher population rate of perinatal HIV exposure among women from high-prevalence countries compared with Australian-born women may reflect differences in HIV prevalence among women of childbearing age by country of birth. The stable rate of perinatal exposure to HIV among Australian-born women suggests that HIV prevalence in this group changed little between 1982 and 2006.
The increase in the population rate of perinatal HIV exposure in Australia in 1999–2002 coincided with the availability of HAART for minimising the risk of mother-to-child transmission. Use of HAART has been associated with a decrease in AIDS diagnoses and death following AIDS among children with perinatal infection in both Australia and in other developed countries.18-20 Since the development of HAART, women diagnosed with HIV infection may be electing to have children because of the possibility of substantially reducing the risk of transmission and adverse outcomes after perinatal HIV infection.
Use of all three interventions — antiretroviral therapy during pregnancy, elective caesarean section and avoidance of breastfeeding — was associated with a substantially reduced mother-to-child transmission rate in Australia, comparable with rates reported from large international studies.5-8 In the six Australian cases of mother-to-child transmission that occurred despite the reported use of antiretroviral therapy during pregnancy, the duration of therapy was 3 months or less before delivery, also consistent with results of international studies. Short duration of antenatal antiretroviral therapy has been identified as a risk factor for mother-to-child transmission among women with an undetectable viral load at term.5-7
The use of antenatal HIV antibody testing has steadily increased in Australia, to around 60% of pregnant women seen by Fellows of the Royal Australian and New Zealand College of Obstetricians and Gynaecologists in 2004,21-23 suggesting increasing acceptance of testing among women of childbearing age. However, HIV infection remained undiagnosed during pregnancy for a substantial number of Australian-born women and women from high-prevalence countries. The national policy on antenatal HIV testing was revised in 2006 and recommends that it be offered to all women.24 The impact of this policy on perinatal HIV exposure and its outcome in Australia is awaited.
1 Age-standardised rate of perinatal HIV exposure among Australia-born children, by place of mother’s birth
3 Number of Australian-born children reported with perinatal HIV exposure and number infected, by timing of the mother’s HIV diagnosis with respect to the child’s birth
* Includes one mother whose date of HIV diagnosis was not reported. |
|||||||||||||||
4 Uptake of interventions by women with an antenatal HIV diagnosis, by year of birth of the exposed child
Received 31 July 2008, accepted 9 December 2008
- Ann M McDonald1
- Yvonne A Zurynski2
- Handan C Wand1
- Michelle L Giles3,4
- Elizabeth J Elliott2,5
- John B Ziegler6,7
- John M Kaldor1
- 1 National Centre in HIV Epidemiology and Clinical Research, Sydney, NSW.
- 2 Australian Paediatric Surveillance Unit, Children’s Hospital at Westmead, Sydney, NSW.
- 3 Infectious Diseases Unit, Alfred Hospital, Melbourne, VIC.
- 4 Department of Medicine, University of Melbourne, Melbourne, VIC.
- 5 Children’s Hospital at Westmead Clinical School, University of Sydney, Sydney NSW.
- 6 Sydney Children’s Hospital, Sydney, NSW.
- 7 School of Women’s and Children’s Health, University of New South Wales, Sydney, NSW.
The National Centre in HIV Epidemiology and Clinical Research (NCHECR) is funded by the Australian Government Department of Health and Ageing, and is affiliated with the Faculty of Medicine, University of NSW. Its work is overseen by the Ministerial Advisory Committee on AIDS, Sexual Health and Hepatitis. The NCHECR Surveillance Program is a collaborating unit of the Australian Institute of Health and Welfare. The APSU is supported by the Australian Government Department of Health and Ageing, the National Health and Medical Research Council (Enabling Grant No. 402784 and Practitioner Fellowship No. 457084: Elizabeth Elliott), Discipline of Paediatrics and Child Health and Faculty of Medicine at the University of Sydney, the Children’s Hospital at Westmead, and the Division of Paediatrics and Child Health, Royal Australasian College of Physicians. We thank all reporting clinicians who participate in monthly surveillance and reported cases to this study.
None identified.
- 1. Connor EM, Sperling RS, Gelber R, et al. Reduction of maternal–infant transmission of human immunodeficiency virus type 1 with zidovudine treatment. N Engl J Med 1994; 331: 1173-1180.
- 2. Cooper ER, Charurat M, Mofenson L, et al. Combination antiretroviral strategies for the treatment of pregnant HIV-1 infected women and prevention of perinatal HIV-1 transmission. J Acquir Immune Defic Syndr 2002; 29: 484-494.
- 3. European Mode of Delivery Collaboration. Elective caesarean-section versus vaginal delivery in prevention of vertical HIV-1 transmission: a randomised clinical trial. Lancet 1999; 353: 1035-1039.
- 4. Ziegler JB, Cooper DA, Johnson RO, Gold J; Sydney AIDS Study Group. Postnatal transmission of AIDS-associated retrovirus from mother to infant. Lancet 1985; 1: 896-897.
- 5. European Collaborative Study. Mother-to-child transmission of HIV infection in the era of highly active antiretroviral therapy. Clin Infect Dis 2005; 40: 458-465.
- 6. Warszawski J, Tubiana R, le Chenadec J, et al; ANRS French Perinatal Cohort. Mother-to-child HIV transmission despite antiretroviral therapy in the ANRS French Perinatal Cohort. AIDS 2008; 22: 289-299.
- 7. Townsend CL, Cortina-Borja M, Peckham CS, et al. Low rates of mother-to-child transmission of HIV following effective pregnancy interventions in the United Kingdom and Ireland, 2000–2006. AIDS 2008; 22: 973-981.
- 8. Townsend CL, Cortina-Borja M, Peckham CS, Tookey PA. Trends in management and outcome of pregnancies in HIV-infected women in the UK and Ireland, 1990–2006. BJOG 2008; 115: 1078-1086.
- 9. McDonald AM, Cruickshank M, Ziegler JB, et al. Perinatal exposure to HIV in Australia, 1982–1994. Med J Aust 1997; 166: 77-80.
- 10. McDonald AM, Li Y, Cruickshank MA, et al. Use of interventions for reducing mother-to-child transmission of HIV in Australia. Med J Aust 2001; 174: 449-452.
- 11. Giles ML, McDonald AM, Elliot EJ, et al. Variable uptake of recommended interventions to reduce mother-to-child transmission of HIV in Australia, 1982–2005. Med J Aust 2008; 189: 151-154. <MJA full text>
- 12. Zurynski YA, Peadon E, Bower C, Elliott EJ. Impacts of national surveillance for uncommon conditions in childhood. J Paediatr Child Health 2007; 43: 724-731.
- 13. Guy RJ, McDonald AM, Bartlett MJ, et al. HIV diagnoses in Australia: diverging epidemics within a low-prevalence country. Med J Aust 2007; 187: 437-440. <MJA full text>
- 14. Communicable Diseases Network Australia. Interim surveillance case definitions for the Australian national notifiable diseases surveillance system. Canberra: CDNA, Australian Government Department of Health and Ageing, 2004. http://www.health.gov.au/internet/main/publishing.nsf/content/cdna-casedefini tions.htm (accessed Mar 2009).
- 15. Australian Bureau of Statistics. Births Australia. Canberra: ABS, 2007. (ABS Cat. No. 3301.0.)
- 16. Australian Bureau of Statistics. Migration, Australia, 2006–07. Canberra: ABS, 2008. (ABS Cat. No. 3412.0.)
- 17. Nduati R, John G, Mbori-Ngacha D, et al. Effect of breastfeeding and formula feeding on transmission of HIV-1: a randomized clinical trial. JAMA 2000; 283: 1167-1174.
- 18. Lindegren ML, Byers RH, Thomas P, et al. Trends in perinatal transmission of HIV/AIDS in the United States. JAMA 1999; 282: 531-538.
- 19. Doerholt K, Duong T, Tookey P, et al, and the Collaborative HIV Paediatric Study (CHIPS). Outcomes for human immunodeficiency virus-1 infected infants in the United Kingdom and Republic of Ireland in the era of effective antiretroviral therapy. Pediatr Infect Dis J 2006; 25: 420-426.
- 20. Gibb DM, Duong T, Tookey PA, et al; National Study of HIV in Pregnancy and Childhood Collaborative HIV Paediatric Study. Decline in mortality, AIDS and hospital admissions in perinatally HIV-1 infected children in the United Kingdom and Ireland. BMJ 2003; 327: 1019.
- 21. Elford J, MacDonald MA, Gabb RG, et al. Antenatal HIV antibody testing in Australia. Med J Aust 1995; 163: 183-185.
- 22. Spencer JD, Tibbits D, Tippet C, et al. Review of antenatal testing policies and practice for HIV and hepatitis C infection. Aust N Z J Public Health 2003; 27: 614-619.
- 23. Giles ML, Garland SM, Grover SR, et al. Impact of an education campaign on management in pregnancy of women infected with a blood-borne virus. Med J Aust 2006; 184: 389-392. <MJA full text>
- 24. National HIV Testing Policy 2006. Canberra: Ministerial Advisory Committee on AIDS, Sexual Health and Hepatitis, and Department of Health and Ageing, 2006. http://www.health. sa.gov.au/PEHS/PDF-files/hiv-testing-policy-2006.pdf (accessed Jul 2008).





Abstract
Objective: To describe the pattern of perinatal HIV exposure and outcomes among children born in Australia, 1982–2006.
Design and setting: National surveillance for perinatal HIV exposure.
Participants: Women with HIV infection and their perinatally exposed children.
Main outcome measures: Trends in the age-standardised rate of perinatal exposure, uptake of interventions by women with an antenatal HIV diagnosis, and rate of mother-to-child transmission.
Results: Between 1982 and 2006, there were 354 reported cases of perinatal HIV exposure among children born in Australia. The age-standardised rate of perinatal exposure per 100 000 live births increased from 2.3 (1982–1986) to 5.1 (1991–1998), 9.9 (1999–2002) and 8.3 (2003–2006). Among children whose mother was diagnosed antenatally, the mother-to-child transmission rate declined significantly, from 25% (4/16; 95% CI, 7%–52%) in 1987–1990 to 5% (4/82; 95% CI, 1%–12%) in 2003–2006 (P < 0.001). The rate declined from 8% (4/51; 95% CI, 2%–19%) in 1987–1998 to 1% (2/151; 95% CI, 0.2%–5%) in 1999–2006 among children whose mother used at least two interventions. Mother-to-child transmission remained high among children born to women diagnosed postnatally (39/87, 45%; 95% CI, 34%–56%) and to women diagnosed antenatally who used no interventions (7/15, 47%; 95% CI, 21%–73%).
Conclusion: The increasing rate of perinatal exposure and the decreasing rate of mother-to-child transmission among children whose mothers’ HIV infection was diagnosed antenatally were temporally associated with use of interventions for minimising mother-to-child transmission. Mother-to-child transmission remained high when the mother’s HIV infection was not known during pregnancy.