Cardiovascular disease is more prevalent among Indigenous Australians than non-Indigenous Australians, and Indigenous Australians present for cardiac surgery about 20 years earlier, on average. This is likely to be due both to higher rates of traditional cardiovascular risk factors and to persistence of rheumatic heart disease.1-4 In addition to differences between Indigenous and non-Indigenous Australians in disease prevalence, there is evidence of disparity in outcomes after acute cardiovascular events such as myocardial infarction.5,6 While cardiac surgery is highly effective, outcomes for Indigenous patients may be less favourable, owing to more extensive disease at the time of presentation, a higher prevalence of cardiovascular risk factors, difficulty accessing ongoing medical care, and higher mortality from non-cardiovascular causes.
Diabetes was defined by a previous physician diagnosis or treatment with hypoglycaemic medication.
The European System for Cardiac Operative Risk Evaluation (euroSCORE) is a widely used model for predicting 30-day mortality in patients undergoing cardiac surgery7 (the higher the euroSCORE, the higher the predicted operative mortality). It was developed from outcomes in 128 European centres and has been validated in European, Japanese, and North American populations.8-12 Although the euroSCORE model has previously been shown to overestimate operative mortality in an Australian population, it does provide sufficient discrimination between strata of risk.13,14 Using standard component definitions, we calculated the logistic euroSCORE for all patients preoperatively (Box 1).7
Preoperative renal dysfunction was defined by a serum creatinine level > 200 μmol/L.
Baseline clinical and procedural variables were stratified by Indigenous status. To control for confounding by preoperative clinical parameters, we used the euroSCORE to model preoperative risk.7 Calibration and discrimination of the euroSCORE in our population were first examined using the c statistic (a measure of concordance) and the Hosmer–Lemeshow goodness-of-fit test. Operative mortality was stratified by Indigenous status in quintiles of the euroSCORE.
Non-Indigenous patients were more likely to have the cardiovascular risk factors of hypertension and hypercholesterolaemia, whereas Indigenous patients were more likely to have diabetes and renal dysfunction and to be current smokers (Box 2). Indigenous patients were also more likely to present with moderate or severe left ventricular dysfunction, active endocarditis and pulmonary hypertension. The median euroSCORE was lower for Indigenous patients than non-Indigenous patients (2.08 [IQR, 1.49–3.92] v 2.49 [IQR, 1.51–5.13]; P < 0.001), owing to the inclusion of age in this score.
Indigenous patients were more likely to undergo either single or double valve surgery. In patients undergoing mitral valve replacement, Indigenous patients were less likely to undergo implantation of a mechanical prosthesis (Box 2).
Forty-two patients (1.6%) died either within 30 days of cardiac surgery or during the same admission (Box 3). In the overall cohort, euroSCORE was able to discriminate risk of operative mortality (c statistic, 0.75), but overestimated events in all strata (Hosmer–Lemeshow goodness-of-fit, P < 0.001). The increasing frequency of operative mortality associated with increasing euroSCORE is evident from the graph in Box 4. There was a non-significant trend towards higher operative mortality in Indigenous patients than non-Indigenous patients (2.5% v 1.5%), whether unadjusted or adjusted for euroSCORE (Box 3).
At a median follow-up of 45 months (IQR, 25–60 months), there were 293 deaths (11.1%) (Box 3). Indigenous status was associated with a borderline-significant excess in late mortality (Indigenous patients, 12.7% v non-Indigenous patients, 10.9%; HR, 1.4 [95% CI, 0.99–2.0]) that became significant when adjusted for euroSCORE (HR, 1.5 [95% CI, 1.03–2.1]).
Survival at 1 and 5 years was 94.0% and 80.6%, respectively, for Indigenous patients compared with 96.7% and 87.7%, respectively, for non-Indigenous patients (Box 5).
The mean age of Indigenous patients was substantially lower than the mean age of non-Indigenous patients. When the analysis was restricted to patients aged < 55 years, there was a significant excess in operative mortality among Indigenous patients (Box 6). The difference persisted when adjusted for euroSCORE (Box 3). The operative mortality of Indigenous patients aged < 55 years (3.5%) was in fact higher than that for non-Indigenous patients aged ≥ 55 years (1.7%).
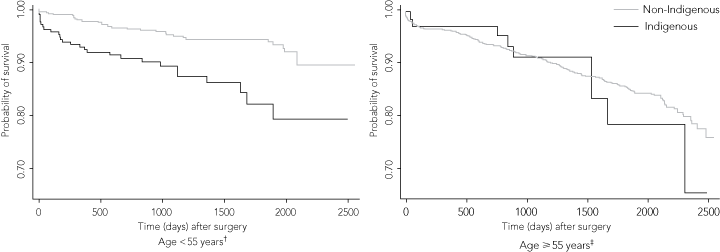
In patients aged < 55 years, at a median follow-up of 45 months, death occurred in 27/202 Indigenous patients (13.4%) and 26/458 non-Indigenous patients (5.7%) (Box 6). Unadjusted survival curves of patients in the two age groups (< 55 years and ≥ 55 years) (Box 7) showed excess late mortality among Indigenous patients compared with non-Indigenous patients in the younger cohort (HR, 3.0 [95% CI, 1.8–5.3]), which persisted despite adjustment for euroSCORE (HR, 6.9 [95% CI, 1.4–33.5]). By contrast, differences in survival between Indigenous and non-Indigenous patients were not significant in the older cohort, whether unadjusted (HR, 1.2 [95% CI, 0.6–2.3]) or adjusted (HR, 0.9 [95% CI, 0.5–1.8) for euroSCORE. This was primarily due to a low number of Indigenous patients (and hence events) in the older age group (interaction P value for age < 55 years, Indigenous status and mortality, 0.005).
The influence of ethnic status on outcomes of cardiac surgery has been described in international settings. In North America, both African-American and South-East Asian populations have been shown to have increased operative mortality after risk adjustment.15-17
Previous studies of Indigenous Australians have focused on the management of valvular disease rather than cardiac surgery overall. They have revealed high rates of morbidity and mortality following valve surgery, particularly after the implantation of mechanical prostheses.18-20 In addition, an excess in age-adjusted mortality after percutaneous mitral commissurotomy has been found in an Indigenous cohort compared with a non-Indigenous control group.20 But, to our knowledge, ours is the first analysis of cardiac surgical outcomes in Indigenous people compared with non-Indigenous people.
Consistent with previous analyses are the differences in baseline characteristics of Indigenous patients presenting with symptomatic cardiovascular disease.18-20 Not only are there significant age differences, but the severity of heart disease appears different. Rheumatic valvular disease and premature coronary atherosclerosis are both major health problems in Indigenous populations and are responsible for the marked age discrepancy in our cohort presenting for cardiac surgery. However, the younger age of onset and severity of heart disease do not completely explain the adverse outcomes, as disparity in outcomes persisted after risk adjustment. Differences in late mortality must also take into account the known higher rate of non-cardiovascular mortality in Indigenous populations.1
A strength of our study was the standardised collection of data and analysis of in-hospital outcomes from a large single-centre registry. A limitation was that, after discharge, the assessment of late outcome was based on total mortality rather than repeated cardiovascular events or need for re-operation. There is some evidence to suggest that differences in the timing of mortality reporting in Indigenous populations have the potential to cause underestimation of mortality at the time of follow-up.1 In addition, we recorded all-cause late mortality rather than death from cardiovascular causes. A larger sample size would allow a more detailed analysis of the mechanisms of adverse outcomes and, potentially, the development of a more accurate operative risk prediction model for Indigenous patients. Future studies should aim at increasing the sample size of Indigenous patients through national collaboration, while maintaining standardised definitions and data collection methods. Although we used the euroSCORE to adjust for surgical risk, the score has not been validated in the Indigenous population. We acknowledge the limitations of using this measure for risk stratification in the Indigenous population, but it is widely used throughout Australia and we believe it to be the best currently available tool for such a purpose.
1 Components of the logistic euroSCORE (European System for Cardiac Operative Risk Evaluation)7
4 Operative mortality of Indigenous and non-Indigenous patients, divided into quintiles of baseline euroSCORE*
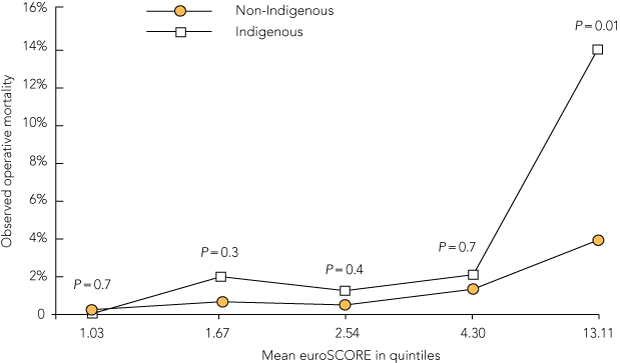 | |||||||||||||||
5 Survival (proportion of patients alive at 1- to 5-year follow-up after surgery), by Indigenous status and type of surgery
- Sam J Lehman1
- Robert A Baker2
- Philip E Aylward3
- John L Knight4
- Derek P Chew5
- Department of Cardiology, Flinders University, Adelaide, SA.
Sam Lehman is supported by grants from the National Heart Foundation of Australia, the Cardiac Society of Australia and New Zealand, and the Royal Australian and New Zealand College of Physicians.
None identified.
- 1. Australian Bureau of Statistics and Australian Institute of Health and Welfare. The health and welfare of Aboriginal and Torres Straight Islander peoples 2008. Canberra: ABS and AIHW, 2008. (ABS Cat. No. 4704.0; AIHW Cat. No. IHW 21.)
- 2. Walsh WF. Cardiovascular health in Indigenous Australians: a call for action. Med J Aust 2001; 175: 351-352. <MJA full text>
- 3. Australian Bureau of Statistics. National Aboriginal and Torres Straight Islander Health Survey, 2004–05. Canberra: ABS, 2006. (ABS Cat. No. 4715.0.)
- 4. Thompson PL, Bradshaw PJ, Veroni M, et al. Cardiovascular risk among urban Aboriginal people. Med J Aust 2003; 179: 143-146. <MJA full text>
- 5. Mathur S, Moon L, Leigh S. Aboriginal and Torres Straight Islander people with coronary heart disease: further perspectives on health status and treatment. Canberra: AIHW, 2006. (AIHW Cat. No. CVD 33.)
- 6. Coory MD, Walsh WF. Rates of percutaneous coronary interventions and bypass surgery after acute myocardial infarction in Indigenous patients. Med J Aust 2005; 182: 507-512. <MJA full text>
- 7. Roques F, Nashef SA, Michel P, et al. Risk factors and outcome in European cardiac surgery: analysis of the EuroSCORE multinational database of 19030 patients. Eur J Cardiothorac Surg 1999; 15: 816-822.
- 8. Nashef SA, Roques F, Hammill BG, et al. Validation of European System for Cardiac Operative Risk Evaluation (EuroSCORE) in North American cardiac surgery. Eur J Cardiothorac Surg 2002; 22: 101-105.
- 9. Michel P, Roques F, Nashef SA; EuroSCORE Project Group. Logistic or additive EuroSCORE for high-risk patients? Eur J Cardiothorac Surg 2003; 23: 684-687.
- 10. Geissler HJ, Hölzl P, Marohl S, et al. Risk stratification in heart surgery: comparison of six score systems. Eur J Cardiothorac Surg 2000; 17: 400-406.
- 11. Kawachi Y, Nakashima A, Toshima Y, et al. Risk stratification analysis of operative mortality in heart and thoracic aorta surgery: comparison between Parsonnet and EuroSCORE additive model. Eur J Cardiothorac Surg 2001; 20: 961-966.
- 12. Gogbashian A, Sedrakyan A, Treasure T. EuroSCORE: a systematic review of international performance. Eur J Cardiothorac Surg 2004; 25: 695-700.
- 13. Yap CH, Mohajeri M, Ihle BU, et al. Validation of Euroscore model in an Australian patient population. ANZ J Surg 2005; 75: 508-512.
- 14. Yap CH, Reid C, Yii M, et al. Validation of the EuroSCORE model in Australia. Eur J Cardiothorac Surg 2006; 29: 441-446.
- 15. Taylor NE, O’Brien S, Edwards FH, et al. Relationship between race and mortality and morbidity after valve replacement surgery. Circulation 2005; 111: 1305-1312.
- 16. Bridges CR, Edwards FH, Peterson ED, Coombs LP. The effect of race on coronary bypass operative mortality. J Am Coll Cardiol 2000; 36: 1870-1876.
- 17. Brister SJ, Hamdulay Z, Verma S, et al. Ethnic diversity: South Asian ethnicity is associated with increased coronary artery bypass grafting mortality. J Thorac Cardiovasc Surg 2007; 133: 150-154.
- 18. Carapetis JR, Powers JR, Currie BJ, et al. Outcomes of cardiac valve replacement for rheumatic heart disease in aboriginal Australians. Asia Pac Heart J 1999; 8: 138-147.
- 19. McLean A, Waters M, Spencer E, Hadfield C. Experience with cardiac valve operations in Cape York Peninsula and the Torres Strait Islands, Australia. Med J Aust 2007; 186: 560-563. <MJA full text>
- 20. McCann AB, Walters DL, Aroney CN. Percutaneous balloon mitral commissurotomy in Indigenous versus non-Indigenous Australians. Heart Lung Circ 2008; 17: 200-205.





Abstract
Objective: To describe baseline characteristics, operative events and late mortality among Indigenous Australians undergoing cardiac surgery.
Design, setting and participants: Prospective study of consecutive patients undergoing cardiac surgery at Flinders Medical Centre in Adelaide between January 2000 and December 2005.
Main outcome measures: Operative (30-day) mortality and late mortality after cardiac surgery.
Results: Of 2635 patients undergoing cardiac surgery, 283 (10.7%) were Indigenous. Indigenous patients were substantially younger than non-Indigenous patients (mean, 47 [SD, 14] years v 65 [SD, 12] years; P = 0.001) and were more likely to have diabetes (39.6% v 27.3%; P = 0.001), renal dysfunction (3.2% v 1.2%; P = 0.009), and valvular surgery (53.0% v 23.1%; P < 0.001). There was a non-significant trend toward excess operative mortality in Indigenous patients (Indigenous 2.5% v non-Indigenous 1.3%; hazard ratio [HR], 1.67 [95% CI, 0.74–3.75]). But in the under-55-years age cohort, the difference between the two groups was highly significant (Indigenous 3.3% v non-Indigenous 0.4%; HR, 7.99 [95% CI, 1.66–38.50]), even after adjustment for euroSCORE (the European System for Cardiac Operative Risk Evaluation). Survival at 1 and 5 years was 94.0% and 80.6%, respectively, for Indigenous patients compared with 96.7% and 87.7%, respectively, for non-Indigenous patients. There was an excess in euroSCORE-adjusted mortality in the Indigenous cohort overall (HR, 1.46 [95% CI, 1.03–2.07]) that strengthened when restricted to the under-55-years cohort (HR, 6.9 [95% CI, 1.42–33.5]).
Conclusion: Indigenous Australians present for cardiac surgery nearly 20 years earlier than non-Indigenous Australians and experience excess age-stratified operative and late mortality.