Rates of mortality from cancer are markedly higher for Indigenous compared with non-Indigenous Australians,1-4 even after adjustment for stage at diagnosis, cancer treatment and comorbidities.5 Treatment disparity accounts for most of the survival deficit.6
Effective doctor–patient communication, particularly crucial in cancer care,7 positively correlates with the development of a strong therapeutic bond, adherence to therapy, understanding of treatment risks, reduced patient anxiety, patient satisfaction and reduced risk of medical mishaps or malpractice claims.8-10 Miscommunication can have adverse consequences, including misdiagnosis, procedures being carried out without informed consent, poor adherence to treatment and persistent health-damaging behaviours.11
Communication can be adversely affected by people’s socioeconomic, historical and cultural backgrounds. Culture is a complex phenomenon encompassing knowledge, folklore, language, rules, rituals, habits, lifestyles, attitudes, beliefs and customs that link and give a common identity to a particular group of people at a specific point in time,12 and doctor–patient communication can occur in a context where there is interplay between cultures. Concerns about communication between Indigenous patients and health professionals have been previously identified.13-15 Physicians have been found to deliver less information and less supportive talk to patients of black and Hispanic background and of lower socioeconomic class, and to be less proficient in their clinical performance with such patients.16 A study with Native Canadians identified history, trust and concept of time as influencing communication between them and physicians,15 while physicians have documented the significant role of non-verbal communication in interaction with patients of native and First Nations (original inhabitants of Canada and their descendants) ethnicity.17 If unaccustomed to these non-verbal signals, clinicians could easily misinterpret patient behaviour.
In Australia, few studies have looked at the extent, nature and consequences of (mis)communication between Aboriginal patients and service providers.11,13 A 2002 study identified sources of miscommunication such as lack of patient control over language, timing, content and circumstances of interactions, differing modes of discourse, dominance of biomedical knowledge, cultural and linguistic distance, and lack of resources including trained interpreters.13 In this research, we explored Aboriginal people’s views and experiences of cancer-related services in WA and their impact on decisions about uptake of cancer treatment.
In light of Aboriginal Australians’ previous negative experiences with research,18 relationship building was prioritised and interviews were conducted in a setting of the participants’ choice. On rural visits, a respected appropriate local person nominated by the health service introduced the interviewer, and often remained throughout the interview.
Interviews were audio-recorded, transcribed verbatim and coded independently by two researchers. The interviewer maintained a reflective journal throughout. NVivo 7 (QSR International, Melbourne, Vic) software was used to assist data management and analysis. Participants’ narratives were divided into broad categories to allow identification of key themes. Feedback sessions with available participants clarified whether emerging themes were an accurate reflection of participants’ experiences. A social-ecological and holistic approach was considered for interpreting data.19,20 Social-ecological epistemology considers the interrelatedness of several social elements21 and looks at effects and relationships at multiple levels.19,22 The holistic approach considers overall wellbeing in terms of physical, mental, emotional and spiritual aspects of healing and wellness.20
Thirty interviews were conducted with 14 Aboriginal patients with cancer and 16 family members. Demographic characteristics of the 30 interviewees are shown in Box 1.
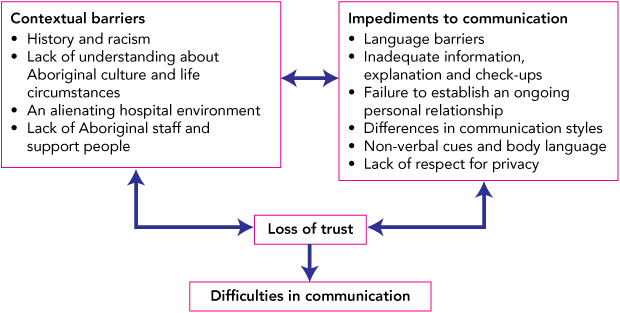
Thematic analysis identified many concerns relating to hospital treatment. Communication issues with service providers were a salient concern, with subthemes of contextual barriers, impediments to communication and loss of trust (Box 2). These themes were often coded concurrently, highlighting the connection between them. These results align with the social-ecological model, highlighting the complex interplay between factors at different levels (individual, family, community, societal) and their impact on patient–provider communication. Although many of the issues identified are applicable to non-Aboriginal people when accessing treatment, their severity and impact on Aboriginal people is compounded by an aggregation of factors including their collective historical experience, cultural background and preferences, and poorer socioeconomic circumstances.
Racism doesn’t help the process of getting better; it delays it. A lot of our people know. They don’t have to hear it; they can see it in the person’s actions. — Urban female patient
Aboriginal women from remote communities make decisions not to come to Perth for treatment because of the way they are treated here — Urban female family member
— or to delay their attendance. Racism and discrimination are frequently experienced by Aboriginal people in contemporary Australia.23 Participants spoke about discomforting experiences with doctors’ behaviour and feeling discriminated against (Box 3, A).
Participants reported that many providers lacked understanding about Aboriginal culture, and the socioeconomic conditions and life circumstances of Aboriginal families. The importance of extended family and of country was often ignored in the hospital system. Some health professionals were seen as not wanting to deal with attending family members at all. Aboriginal patients’ wishes to be at home for as much time as possible and to die in their country were underappreciated. Doctors had failed to inform some families that a relative had cancer or was gravely ill until days before death. A view reiterated was that terminally ill patients should be informed and offered the opportunity to return home as soon as possible (Box 3, B). Furthermore, suggestions by service providers about managing cancer, including taking liquid or “right diet” foods, and refrigeration of medications were sometimes unrealistic, confusing and frustrating.
Putting Aboriginal men and women together, mixing family groups inappropriately, male doctors attending female patients and vice versa, and young(er) providers advising older Aboriginal patients were also culturally inappropriate and problematic (Box 3, B).
Participants viewed the medical system as cold, indifferent, and inflexible. They felt their needs and preferences were not considered important within mainstream service provision (Box 3, C). Many commented on the need for Aboriginal support people to help patients and their families negotiate the hospital system, and to play a significant role in ensuring that patients understood treatment plans, possible outcomes and responsibilities. Just “having an Aboriginal face around” would help people settle better in the hospitals (Box 3, C).
English is not the language of choice for some Aboriginal people, particularly those from remote communities, yet there are no Aboriginal language interpreter services available in Perth tertiary hospitals. Family or community members may assist, but they may be stressed or lack adequate knowledge to provide informed support for the patient. Some Aboriginal patients lacked any support (Box 4, A).
Some participants had encountered medical staff who failed to explain treatment side effects and the purpose of medications, or who were not forthcoming about the severity and prognosis of their illness. This angered patients and their families. Physicians’ use of jargon and technical terms also caused frustration24 (Box 4, B), as did perceived avoidance of talking with the patient.
Staff turnover in hospitals affected continuity of care, impeded development of good doctor–patient relationships and quality of treatment and follow-up services, and disappointed patients. This contributed to patient uncertainty about engagement in treatment and follow-up. Patients felt that the way they were treated during hospital appointments reflected doctors’ lack of real care for them (Box 4, C); this is an issue likely to have a particular impact on Aboriginal people because of the importance placed upon relationship within their culture.25
Participants reported that Aboriginal people are “cluey”, “intuitive”, “can read minds”, and have an ability to pick up whether a provider is genuinely interested in them as soon as they meet. Many physicians were felt to lack compassion or warmth in interpersonal interactions, whereas participants expected them to be “understanding”, “compassionate”, “concerned” and “empathetic” (Box 4, D). Many Aboriginal people are “reserved” during their visits to doctors, and are reluctant to admit difficulties with understanding (Box 4, D). This reticence could stem from believing that “the doctors know everything”, lack of confidence to ask questions, silence as part of their culture or a learned behaviour from previous encounters within mainstream institutions. Such silence could be easily misinterpreted by health care providers.
Conspicuous distrust of hospital services was noticeable. This distrust stemmed from Aboriginal patients’ negative encounters and experiences within the health system (Box 5). Trust develops as a result of broad-level social interaction, and requires reliability of the other within a given context. The absence of manifest respect for the culture of a particular group, together with repeated betrayal of trust, can create further distrust. Once distrust develops, all forms of involvement are undermined. People feel alienated from the system.26
Our study findings indicated that the tools needed to facilitate the entry of Aboriginal people into the medical system and to manage effective treatment are culturally sensitive and empathetic personal contact, acknowledgement and respect for Aboriginal family structures, culture and life circumstances, and the importance of land and community. Although Aboriginal peoples’ experiences with cancer are not unique, they are overlaid by a collective experience of systemic racism within a public health care system.27 There was considerable commonality in the reports of participants, irrespective of whether they were patients or family members, and despite variation in their demographic backgrounds.
Effective communication between patients and health care providers is essential for quality health care delivery,16 and is inevitably affected by the culture(s) of those involved.12 The dissimilarities between Aboriginal beliefs and cultural considerations and the approach of the Western medical system help explain Aboriginal people’s underuse of health services.28,29 Typically, health professionals focus on educating Aboriginal people to increase their biomedical understanding of disease processes. However, if health service providers are to be really effective as “healers”, there are strong arguments for their making efforts to understand a patient’s culture and social circumstances.
Sensitivity in patient care requires attention to the patient as a person, and this requires focus on patient–provider communication, understanding and relationship. Minorities around the world report less involvement in medical decisions, less partnership, and lower levels of satisfaction with their care providers.15,16,30
Limitations of our study include the under-representation of male participants. Possible reasons for this include: the main interviewer being female; women predominating as health care professionals and carers; there being a differential cancer survival according to sex; and higher use of health services by women.31,32 The larger number of selected quotations from family members suggests that the family members were able to frame the experience of Aboriginal people better, and were more coherent and succinct in reporting.
Participants wanted an ongoing, trusting relationship with a provider who genuinely cared about them, but Aboriginal people often felt their wishes were not heeded and that their trust was betrayed. Good care must acknowledge that people care about relational issues such as being treated with dignity and respect and being heard.33 Trust is crucial for patients in accepting difficult diagnoses, following complex treatment plans,34 and for being satisfied with their medical care and having positive clinical outcomes.35 The system appears to focus too much on clinical competence and too little on other psychosocial characteristics that encourage patient trust — equality, benevolence, integrity, respect, and honesty.36 If treatment outcomes are to improve, the health system must become responsive to Aboriginal needs and heed their suggestions (Box 6). Participation and representation of Aboriginal people at a decision-making level in hospitals will help ensure these issues are addressed; such inclusion will, in itself, be an important symbol of progress. Increasing Aboriginal health literacy requires access to appropriate information and dedicated employment of Aboriginal staff.24
Culturally appropriate, integrated and sustainable care for Aboriginal people with cancer requires a coordinated person-centred approach, involving patients, family members, Aboriginal health staff, and clinicians. Relationships developed through such networks are likely to help Aboriginal patients cope with the hospital settings, and ultimately enhance their confidence in communicating with the doctors. Many of the issues raised here are again identified in current national review processes, emphasising that the needs of Aboriginal people are indicative of the need for a broader health care reform process.37
2 Barriers to effective communication between Aboriginal patients and health service providers in the hospital setting
3 Family members’ responses illustrating contextual barriers to effective communication between Aboriginal patients and health service providers in hospitals
B. Lack of understanding about Aboriginal culture and life circumstances
C. An alienating hospital environment and lack of Aboriginal support people
4 Interviewees’ responses illustrating impediments to communication in hospitals
B. Inadequate information, explanation and check-ups
C. Failure to establish an ongoing personal relationship
D. Different communication styles and non-verbal communication
6 Suggestions and recommendations based on the study findings
At the hospital and system level
Recruit Aboriginal people onto hospital decision-making committees
Recruit Aboriginal support people and increase the number of Aboriginal staff in hospitals
Make the hospital environment more welcoming to Aboriginal people
Use interpreters or relevant support people to understand patients’ concerns and needs
Improve continuity of care by allowing more time to build rapport, and to know the person
Provide care and follow-up closer to home where possible
Increase linkages between the hospital and primary and community-based care
Make available cultural safety training and encourage all staff, particularly doctors, to attend
Improve communication skills in oncology staff through training in communication skills and Aboriginal cultural safety
Rethink how patients are approached for consent around medical and other students
Mandate participation in cultural safety training so health staff understand and consider Aboriginal cultural needs (behaviours, preferences, importance of family, bond with the land, traditional practice)
Understand and consider Aboriginal life circumstances such as rural or remote background, food, lifestyle, bond with the land, and the colonial past and its impact, and make realistic suggestions
Show empathy, kindness and understanding for the person affected by cancer
Use clear, plain language to communicate with Aboriginal patients and their families
Explain options clearly and listen to patients’ choices
Make sure that Aboriginal patients and their families have understood what has been prescribed or recommended in regard to cancer treatment, follow-ups and management
- Shaouli Shahid1
- Lizzie D Finn2
- Sandra C Thompson3
- Centre for International Health, Curtin University of Technology, Perth, WA.
This research was supported by a grant from the Cancer Council of Western Australia. Shaouli Shahid was supported by Curtin University and an Australian Postgraduate Award. We thank all of the people interviewed for their frankness and for sharing their experiences, and the many health service providers who assisted in the process of data collection. We acknowledge the invaluable contribution of the Aboriginal Reference Group and other investigators for their contributions: Peter Howat, Brian Bishop, Timothy Threlfall, Katie Thomas, Moyez Jiwa, John Mallard, Terry Slevin, Leanne Pilkington, Francine Eades, Dot Henry, Gwen Rakabula, Dawn Bessarab, Jude Comfort and Kim Worthington.
None identified.
- 1. Calver J, Wiltshire A, Holman CD, et al. Does health assessment improve health outcomes in indigenous people? An RCT with 13 years of follow-up. Aust N Z J Public Health 2005; 29: 107-111.
- 2. Condon JR, Armstrong BK, Barnes A, Cunningham J. Cancer in Indigenous Australians: a review. Cancer Causes Control 2003; 14: 109-121.
- 3. Condon JR, Barnes T, Armstrong BK, et al. Stage at diagnosis and cancer survival for Indigenous Australians in the Northern Territory. Med J Aust 2005; 182: 277-280. <MJA full text>
- 4. Roder D. Comparative cancer incidence mortality and survival in Indigenous and non-Indigenous residents of South Australia and the Northern Territory. Can Forum 2005; 29: 7-9.
- 5. Valery PC, Coory M, Stirling J, et al. Cancer diagnosis, treatment, and survival in Indigenous and non-Indigenous Australians: a matched cohort study. Lancet 2006; 367: 1842-1848.
- 6. Coory MD, Green AC, Stirling J, Valery PC. Survival of Indigenous and non-Indigenous Queenslanders after a diagnosis of lung cancer: a matched cohort study. Med J Aust 2008; 188: 562-566. <MJA full text>
- 7. Butow PN, Tattersall MHN, Goldstein D. Communication with cancer patients in culturally diverse societies. Ann N Y Acad Sci 1997; 809: 317-329.
- 8. Ong LML, de Haes JCJM, Hoos AM, Lammes FB. Doctor–patient communication: a review of the literature. Soc Sci Med 1995; 40: 903-918.
- 9. Travaline JM, Ruchinskas R, D’Alonzo GE. Patient–physician communication: why and how. J Am Osteopath Assoc 2005; 105: 13-18.
- 10. Wenrich MD, Curtis JR, Shannon SE, et al. Communicating with dying patients within the spectrum of medical care from terminal diagnosis to death. Arch Intern Med 2001; 161: 868-874.
- 11. Lowell A. Communication and cultural knowledge in Aboriginal health care. A review of two subprograms of the Cooperative Research Centre for Aboriginal and Tropical Health’s Indigenous Health and Education. Research program. October 1998. 1. Communication in Aboriginal health care: an overview. Darwin: Cooperative Research Centre for Aboriginal and Tropical Health, 2001: 3-18. http://www.crcah.org.au/publications/downloads/Communication_and_Cultural.pdf (accessed Mar 2009).
- 12. Airhihenbuwa CO. Health and culture: beyond the Western paradigm. London: Sage Publications, 1995.
- 13. Cass A, Lowell A, Christie M, et al. Sharing the true stories: improving communication between Aboriginal patients and healthcare workers. Med J Aust 2002; 176: 466-470. <MJA full text>
- 14. Kaufert JM, Putsch RW, Lavallee M. End-of-life decision making among Aboriginal Canadians: Interpretation, mediation, and discord in the communication of “bad news”. J Palliat Care 1999; 15: 31-38.
- 15. Towle A, Godolphin W, Alexander T. Doctor–patient communications in the Aboriginal community: towards the development of educational programs. Patient Educ Couns 2006; 62: 340-346.
- 16. Cooper LA, Roter DL. Patient–provider communication: the effect of race and ethnicity on process and outcomes of healthcare. In: Smedley BD, Stith AY, Nelson AR, editors. Unequal treatment: confronting racial and ethnic disparities in health care. Washington, DC: National Academy Press, 2003: 552-593.
- 17. Kelly L, Brown JB. Listening to native patients. Changes in physicians’ understanding and behaviour. Can Fam Physician 2002; 48: 1645-1652.
- 18. Larson A, Gillies M, Howard PJ, et al. It’s enough to make you sick: the impact of racism on the health of Aboriginal Australians. Aust N Z J Public Health 2007; 31: 322-329.
- 19. Fondacaro MR, Weinberg D. Concepts of social justice in community psychology: toward a social ecological epistemology. Am J Community Psychol 2002; 30: 473-492.
- 20. Aboriginal Cancer Care Unit, Cancer Care Ontario. “It’s our responsibility”. Report of the Aboriginal cancer care needs assessment. Toronto: Cancer Care Ontario, Nov 2002. http://www.cancercare.on.ca/common/pages/UserFile.aspx?fileId=13836 (accessed Mar 2009).
- 21. Oetzel JG, Ting-Toomey S, Rinderle S. Conflict communication in contexts: a social ecological perspective. In: Oetzel JG, Ting-Toomey S, editors. The SAGE handbook of conflict communication. Thousand Oaks, Calif: Sage, 2006.
- 22. Prilleltensky I, Nelson G. Doing psychology critically: making a difference in diverse settings. London: Palgrave Macmillan, 2002.
- 23. McDonald H. Culture in health research and practice. In: Anderson I, Baum F, Bentley M, et al, editors. Beyond bandaids: exploring the underlying social determinants of Aboriginal health. Papers from the Social Determinants of Aboriginal Health Workshop, Adelaide, July 2004. Darwin: Cooperative Research Centre for Aboriginal Health, 2007: 255-280. http://www.crcah.org.au/publications/downloads/BeyondBandaidsText.pdf (accessed Mar 2009).
- 24. Anderson K, Devitt J, Cunningham J, et al. “All they said was my kidneys were dead”: Indigenous Australian patients’ understanding of their chronic kidney disease. Med J Aust 2008; 189: 499-503. <MJA full text>
- 25. Smith LT. Decolonizing methodologies: research and Indigenous peoples. London: Zed Books, 1999.
- 26. Thiede M. Information and access to health care: is there a role for trust? Soc Sci Med 2005; 61: 1452-1462.
- 27. National Breast Cancer Centre and National Cancer Control Initiative. Clinical practice guidelines for the psychosocial care of adults with cancer. Sydney: NBCC, 2003.
- 28. Cunningham J. Diagnostic and therapeutic procedures among Australian hospital patients identified as Indigenous. Med J Aust 2002; 176: 58-62. <MJA full text>
- 29. Fisher DA, Weeramanthri TS. Hospital care for Aboriginals and Torres Strait Islanders: appropriateness and decision making. Med J Aust 2002; 176: 49-51. <MJA full text>
- 30. Cooper-Patrick L, Gallo JJ, Gonzales JJ, et al. Race, gender, and partnership in the patient-physician relationship. JAMA 1999; 282: 583-589.
- 31. Courtenay WH. Constructions of masculinity and their influence on men’s well-being: a theory of gender and health. Soc Sci Med 2000; 50: 1385-1401.
- 32. Bertakis KD, Azari R, Helms LJ, et al. Gender differences in the utilisation of health care services. J Fam Pract 2000; 49: 147-152.
- 33. Tyler TR. Psychological models of the justice motive: antecedents of distributive and procedural justice. J Pers Soc Psychol 1994; 67: 850-863.
- 34. Tarn DM, Meredeth LS, Kagawa-Singer M, et al. Trust in one’s physician: the role of ethnic match, autonomy, acculturation, and religiosity among Japanese and Japanese Americans. Ann Fam Med 2005; 3: 339-347.
- 35. Thom DH, Kravitz RL, Bell RA, et al. Patient trust in the physician: relationship to patient requests. Fam Pract Manag 2002; 19: 476-483.
- 36. Wright EB, Holcombe C, Salmon P. Doctors’ communication of trust, care, and respect in breast cancer: qualitative study. BMJ 2004; 328: 864-867.
- 37. National Health and Hospitals Reform Commission. A healthier future for all Australians — interim report December 2008. Canberra: NHHRC, 2009. http://www.nhhrc.org.au/internet/nhhrc/publishing.nsf/Content/BA7 D3EF4EC7A1F2BCA25755B001817EC/$File/NHHRC.pdf (accessed Mar 2009).





Abstract
Objective: To report Aboriginal patients’ views about effective communication between Aboriginal people and health service providers in Western Australian hospital settings.
Design, setting and participants: Qualitative study involving indepth interviews between 1 March 2006 and 30 September 2007 with 30 Aboriginal people affected by cancer from across WA.
Main outcome measures: Aboriginal patients’ views about the quality of communication within the hospitals, factors impairing communication and suggestions for improvement.
Results: Factors crucial to effective patient–provider communication such as language, shared understanding, knowledge and use of medical terminology require attention. Additionally, communication between Aboriginal people and health care professionals needs to be understood within a broader sociocultural and political context. Fear of the medical system and of being disempowered; mistrust; collective memories of the experience of colonisation and its aftermath; lack of understanding of Aboriginal customs, values, lifestyle and the importance of family and land; and experiences of racism were key issues impairing communication. Health service providers’ inability to interpret non-verbal communication and the symbolism of hospital environments also posed problems.
Conclusion: Key areas for the attention of health service providers in communicating and caring for Aboriginal people in the hospital setting include culturally sensitive and empathetic personal contact, acknowledgement and respect for Aboriginal family structures, culture and life circumstances, an understanding of the significant role of non-verbal communication, and the importance of history, land and community. Employing more Aboriginal health workers in hospitals, and allowing Aboriginal people to participate at a decision-making level in hospitals is likely to improve Aboriginal people’s access to cancer treatment, and would be important symbols of progress in this area.