Several studies in other countries have shown that some groups of hospital patients, such as African-Americans and women, are less likely than white male patients to receive a variety of diagnostic and therapeutic procedures.1-12 Disparities have been found for procedures for treating heart disease,1-5 for organ transplantation,6-7 and for orthopaedic8-11 and gastrointestinal procedures.8,12
Little research in this area has been done in Australia, and the extent to which such disparities exist for Indigenous patients compared with non-Indigenous patients is unknown, in part because of incomplete identification of Indigenous patients in hospitals in most jurisdictions.13 However, a recently published national report on hospital separations for the financial year 1997–98 (for which I was a co-author) noted that patients identified as Indigenous were less likely than other admitted patients to have a principal procedure recorded (45% v 75%, after excluding admissions for routine dialysis treatment).14 This finding was not the focus of the report, and we did not consider more than one patient characteristic at a time or look at more specific illnesses and conditions. Moreover, no information was available about hospital type and size.
Data were obtained from the National Hospital Morbidity Database (NHMD), which is managed by the Australian Institute of Health and Welfare (AIHW) and includes information on characteristics, diagnoses and care of admitted patients in almost all public and private hospitals in Australia. NHMD records are based on separations (episodes of care) rather than individual patients; a given patient may have multiple separations within the same year.15
Data for this analysis relate to hospital separations between 1 July 1997 and 30 June 1998. All data on diagnoses and procedures for that year were coded using the coding scheme of the ninth revision of the International classification of diseases, clinical modification (ICD-9-CM).16 Data for 1998–99 were not used, as two different versions, ICD-9 and ICD-10, were in use in Australia in that year.17 ICD-9-CM coding was used rather than Australian national diagnosis-related groups (AN-DRGs), because AN-DRGs are determined in part by whether a procedure has been performed.18
Permission to access, analyse and publish data was sought and received from all States and the Northern Territory. The Australian Capital Territory (ACT) denied permission, but this jurisdiction accounted for only 0.4% of separations of patients identified as Indigenous (and 1.3% of all separations) in 1997–98.15
Public and private hospitals were considered separately because of large differences in apparent use of private hospitals by Indigenous and non-Indigenous people, as well as differences in the levels of recorded procedures for all patients. Analysis of private hospitals was limited to New South Wales, Queensland, South Australia and Western Australia, as only these jurisdictions had recorded any acute, non-dialysis separations of patients identified as Indigenous. No information on Indigenous status of patients was available for 1997–98 for private hospitals in Victoria, and no data were available for the single private hospital in the Northern Territory.
The outcome of interest was any recorded principal procedure. According to the National health data dictionary, the principal procedure is the most significant procedure performed for treatment of the principal diagnosis (Box 1).19 If no procedure is performed for treatment of the principal diagnosis, then a principal procedure should be selected according to a hierarchy based on type of procedure (therapeutic or diagnostic/exploratory) and whether the procedure is related to the principal diagnosis.19 Thus, if any procedures are recorded for a given episode of care, a principal procedure should be included in the NHMD, although it may or may not be related to the principal diagnosis.
Explanatory variables of interest related to characteristics of the patient, the episode of care, and the hospital. Patient characteristics included age group, sex, area of residence20 and Indigenous status as recorded by the hospital (Box 2). Studies in individual hospitals have shown that the proportion of Indigenous patients correctly identified varies widely, from below 50% to almost 100%.14 The focus of this analysis is on patients identified as Indigenous rather than all Indigenous patients.
Hospital characteristics included type of hospital and hospital category (public hospitals only) (Box 2).17
Characteristics of the episode included principal diagnosis (ICD-9-CM codes), whether or not it was a same-day admission, and, for public hospital patients, patient accommodation status (Box 2).
Statistical analysis was performed using Stata.21 Logistic regression was used to assess the relationship between explanatory variables of interest and the probability of having a principal procedure recorded. Odds ratios (OR) and 95% CI are reported. Public and private hospitals were analysed separately. Public hospital data were further stratified by principal diagnosis at the level of ICD-9-CM chapters (eg, circulatory diseases, injury) and for 23 more specific groups of conditions (eg, asthma, epilepsy) for which there were at least 500 separations of patients identified as Indigenous.
The study was approved by the Joint Institutional Ethics Committee of the Royal Darwin Hospital and the Menzies School of Health Research.
A total of 4 867 368 acute, non-dialysis separations were recorded in Australia (excluding the ACT) in 1997–98. About 66% of these were for public hospitals and 34% were for private hospitals. Overall, 75% of separations had a principal procedure recorded. In about 2% of separations the patients were identified as Indigenous, with 97% of these being recorded for public hospitals.
In public hospitals, a principal procedure was recorded in 68% of separations. The proportion was considerably lower for patients identified as Indigenous (45% of separations) than for other patients (69% of separations). A difference was apparent regardless of sex, age, place of residence, type of admission, patient accommodation status, or hospital category (Box 2). For all patients, procedures were more likely to be recorded in principal referral and other major hospitals, for same-day admissions, for private patients and for patients from urban areas.
After adjusting for the factors shown in Box 2, patients identified as Indigenous were significantly less likely than other patients to have a principal procedure recorded, both overall and for every ICD-9-CM chapter, except infectious/parasitic diseases and injury (Box 3). The difference was especially marked for diseases of the circulatory, digestive and genitourinary systems and for congenital anomalies, with adjusted odds ratios of about 0.5 for each of these disease categories. In general, adjustment for hospital category resulted in a greater attenuation of the odds ratios for Indigenous status than did adjustment for other factors.
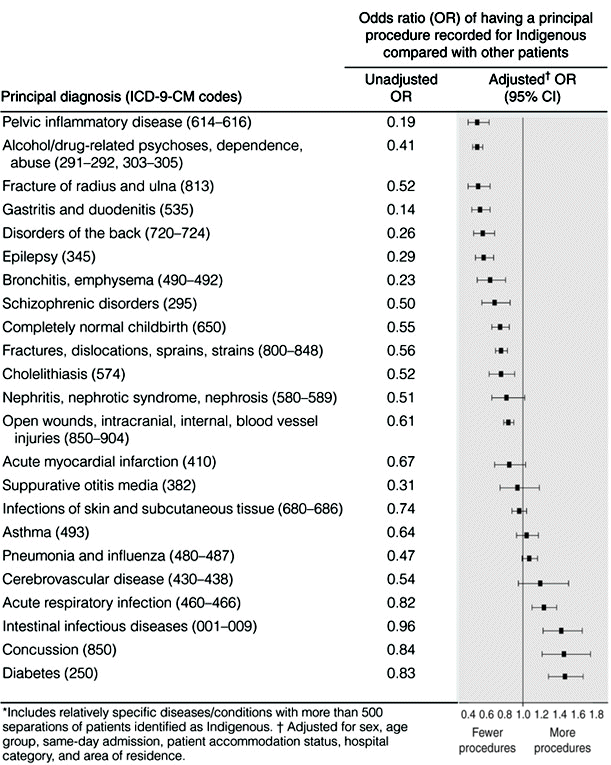
There are important heterogeneities within ICD-9-CM chapters with respect to the appropriateness of and need for procedures. Although it is critical to look at more specific diseases and conditions, it is difficult to do so because of the relatively small numbers of separations of patients identified as Indigenous for most principal diagnoses. Box 4 presents the relative odds of having a recorded principal procedure for conditions with at least 500 separations of patients identified as Indigenous. For each disease/condition, patients identified as Indigenous were less likely than other patients to have a principal procedure recorded. After adjusting for other factors, the disparities were reduced or eliminated (and changed direction in some cases), but, for 12 of the diseases/conditions, patients identified as Indigenous remained significantly less likely than other patients to have a principal procedure recorded.
Most separations (89%) in private hospitals in New South Wales, Queensland, South Australia and Western Australia had a principal procedure recorded, and the proportion was similar regardless of recorded Indigenous status across a range of other variables (Box 2).
My analysis confirms a preliminary report14 that patients identified as Indigenous are less likely than other patients to have a principal procedure recorded, at least in public hospitals. This disparity is partly explained by characteristics of the patient, the episode and, to a larger extent, the hospital, but a considerable difference remains. Within some disease categories, patients identified as Indigenous had only half the odds of other patients in public hospitals of having a procedure recorded, even after adjusting for other factors.
In private hospitals, the probability of having a recorded procedure was similar for all patients. This may reflect the influence of private health insurance. Patients in private hospitals were more likely than those in public hospitals to have a procedure recorded, regardless of whether they were identified as Indigenous. Within public hospitals, private rather than public patients were more likely to have a principal procedure recorded (especially those identified as Indigenous). However, most patients identified as Indigenous were public patients in public hospitals, the group least likely to have a procedure recorded. This is consistent with the relatively low rate of private health insurance coverage of Indigenous people in Australia.13
These results from Australian public hospitals are largely consistent with previous studies in the United States showing a significantly reduced probability of having a range of procedures among African-American hospital patients.8,11,12 Another study found that whites had higher utilisation rates for more discretionary procedures, while blacks had higher rates for medical rather than surgical admissions.9 Finally, a study found that, among patients considered eligible, based on discharge diagnosis, for high-technology procedures with scope for clinical discretion, blacks were significantly less likely to receive five of the nine procedures, and were not significantly more likely to receive any.6
The recorded principal procedure may have been for a condition other than the principal diagnosis, but, given the high burden of morbidity among Indigenous Australians,13 this would more easily explain a higher rather than a lower probability of patients identified as Indigenous having a procedure recorded. It is also possible that some procedures were performed but not recorded.
Decisions about procedures should generally be made in consultation with the patient. It was not possible in this analysis to determine the role played by patient choice, but informed decision-making by patients requires adequate understanding of available options. For some Indigenous patients, this may be limited by communication difficulties due to patient–doctor differences in language, culture, priorities, and so on. One possible indication of failed communication processes and/or lack of shared understanding is that patients identified as Indigenous are much more likely than other patients to leave hospital against medical advice.14 Inadequate communication can lead to potentially useful procedures not being performed, as well as to procedures being performed on patients who did not fully consent.
Having a procedure is not always better than not having one. Concerns about overservicing and unnecessary surgery have been raised,22 and the AIHW monitors variation in rates of sentinel procedures.17 However, given the relatively high mortality rate of Indigenous Australians,13,23 it seems unlikely that the lower probability of having a (recorded) procedure has resulted in overall health benefits for this group.
In my analysis, it was only possible to distinguish between patients identified as Indigenous and other patients. It is not known to what extent the results apply to Indigenous patients who were not correctly identified and therefore included in the "other" group. It could be argued that the experiences of such people are less relevant if discriminatory treatment is responsible for any of the disparity. However, not all discrimination is interpersonal (ie, the result of individual behaviours).24 Institutional factors ("the system") may also result in unfair treatment, often unintentional, for members of some groups. For example, any underservicing in remote areas disproportionately affects Indigenous people simply because they are more likely than other Australians to live there.13 The potential for discrimination exists at multiple points within the healthcare system, including access to services, diagnosis, referral, treatment and outcome. Work is urgently needed to characterise more fully the nature, level, sources and consequences of institutional and interpersonal discrimination so that we can reduce unfair treatment, ensure equitable care and improve outcomes for the most disadvantaged Australians.
1: Principal diagnosis and principal procedure — an example
A 27-year-old man is admitted as a public patient to a major referral hospital with abdominal pain, nausea and vomiting. After examination, an abdominal x-ray is performed, and he is provisionally diagnosed as having acute appendicitis. He has an appendicectomy and the diagnosis is confirmed. Three days after surgery, while still in hospital, he develops a wound abscess, which requires incision and drainage. For this patient, the principal diagnosis is acute appendicitis (ICD-9 code 540) and the principal procedure is appendicectomy (ICD-9 code 47.0).
2: Proportion of separations with a principal procedure recorded — Australian public and private hospitals, 1997–98
|
|
|
||||||||||||||
|
Identified as Indigenous |
Identified as Indigenous |
||||||||||||||
|
|
|||||||||||||||
|
|
|||||||||||||||
3: Unadjusted and adjusted relative odds of having a principal procedure recorded for patients (separations) identified as Indigenous in public hospitals, 1997–98
4: Relative odds (adjusted and unadjusted) of having a principal procedure recorded for patients (separations) identified as Indigenous in public hospitals, by principal diagnosis,* 1997–98
 |
Received 17 May 2001, accepted 17 August 2001
- Joan Cunningham1
- Menzies School of Health Research, Casuarina, NT.
I am supported by a fellowship from the Menzies Foundation. The Cooperative Research Centre for Aboriginal and Tropical Health provided funding to purchase the data. I gratefully acknowledge the contribution of Mary Beneforti (National Centre for Aboriginal and Torres Strait Islander Statistics), who co-authored the preliminary report that prompted this analysis.
None declared.
- 1. Giles WH, Anda RF, Casper ML, et al. Race and sex differences in rates of invasive cardiac procedures in US hospitals. Arch Intern Med 1995; 155: 318-324.
- 2. Ford ES, Cooper RS. Racial/ethnic differences in health care utilization of cardiovascular procedures: a review of the evidence. Health Serv Res 1995; 30: 237-252.
- 3. Whittle J, Conigliaro J, Good CB, Lofgren RP. Racial differences in the use of invasive cardiovascular procedures in the Department of Veterans Affairs medical system. N Engl J Med 1993; 329: 621-627.
- 4. Wenneker MB, Epstein AM. Racial inequalities in the use of procedures for patients with ischaemic heart disease in Massachusetts. JAMA 1989; 261: 253-257.
- 5. Franks AL, May DS, Wenger NK, et al. Racial differences in the use of invasive cardiovascular procedures after acute myocardial infarction in Medicare beneficiaries. Ethn Dis 1993; 3: 213-220.
- 6. Giacomini MK. Gender and ethnic differences in hospital-based procedure utilization in California. Arch Intern Med 1996; 156: 1217-1224.
- 7. Soucie JM, Neylan JF, McClellan W. Race and sex differences in the identification of candidates for renal transplantation. Am J Kidney Dis 1992; 19: 414-419.
- 8. Escarce JJ, Epstein KR, Colby DC, Schwartz JS. Racial differences in the elderly's use of medical procedures and diagnostic tests. Am J Public Health 1993; 83: 948-954.
- 9. Gittelsohn AM, Halpern J, Sanchez RL. Income, race and surgery in Maryland. Am J Public Health 1991; 81: 1435-1441.
- 10. Wilson MG, May DS, Kelly JJ. Racial differences in the use of total knee arthroplasty for osteoarthritis among older Americans. Ethn Dis 1994; 4: 57-67.
- 11. Harris DR, Andrews R, Elixhauser A. Racial and gender differences in use of procedures for black and white hospitalized adults. Ethn Dis 1997; 7: 91-105.
- 12. Mort EA, Weissman JS, Epstein AM. Physician discretion and racial variation in the use of surgical procedures. Arch Intern Med 1994; 154: 761-767.
- 13. Australian Bureau of Statistics, Australian Institute of Health and Welfare. The health and welfare of Australia's Aboriginal and Torres Strait Islander peoples. Canberra: ABS, 1999. (Catalogue No. 4704.0)
- 14. Cunningham J, Beneforti M. Hospital statistics, Aboriginal and Torres Strait Islander Australians, 1997-98. Canberra: ABS, 2000. (Catalogue No. 4711.0)
- 15. Australian Institute of Health and Welfare. Australian hospital statistics, 1997-98. Canberra: AIHW, 1999.
- 16. National Coding Centre. The Australian version of the International classification of diseases, 9th revision, clinical modification (ICD-9-CM), 2nd ed. Sydney: University of Sydney; 1996.
- 17. Australian Institute of Health and Welfare. Australian hospital statistics, 1998-99. Canberra: AIHW, 2000.
- 18. Eagar K, Hindle D. A short introduction to casemix. Canberra: Commonwealth Department of Human Services and Health; 1994. (National Casemix Education Series, No. 1.)
- 19. National Health Data Committee. National health data dictionary, version 7.0. Canberra: AIHW, 1998.
- 20. Department of Primary Industries and Energy, Department of Human Services and Health. Rural, Remote and Metropolitan Area Classification, 1991 Census edition. Canberra: AGPS; 1994.
- 21. Stata [computer program], release 6.0. College Station, Texas: Stata Corporation, 1999.
- 22. Leape LL. Unnecessary surgery. Annu Rev Public Health 1992; 13: 363-383.
- 23. Cunningham J, Paradies Y. Mortality of Aboriginal and Torres Strait Islander Australians, 1997. Canberra: Australian Bureau of Statistics; 2000.
- 24. Lott B, Maluso D, editors. The social psychology of interpersonal discrimination. New York: The Guilford Press, 1995.





Abstract
Objectives: To determine whether hospital patients identified as Indigenous are less likely than other inpatients to have a principal procedure recorded, and the extent to which any disparity in procedure use can be explained by differences in patient, episode and hospital characteristics.
Design: Retrospective analysis of routinely collected administrative data from the National Hospital Morbidity Database (NHMD).
Setting: Australian public and private hospitals.
Patients: All patients included in the NHMD whose episode type was recorded as acute and whose separation occurred between 1 July 1997 and 30 June 1998. Patients admitted for routine dialysis treatment were excluded.
Main outcome measure: Whether a principal procedure was recorded.
Results: In public hospitals, patients identified as Indigenous were significantly less likely than other patients to have a principal procedure recorded, even after adjusting for patient, episode and hospital characteristics (adjusted odds ratio [OR], 0.67; 95% CI, 0.66–0.68). This disparity was apparent for most diseases and conditions. In private hospitals, no significant difference was observed (adjusted OR, 0.94; 95% CI, 0.83–1.06).
Conclusions: The disparity in procedure use after adjustment for relevant factors indicates that in Australian public hospitals there may be systematic differences in the treatment of patients identified as Indigenous.