Compared with Australian infants, Indigenous Australian infants have lower birthweights, a greater risk of preterm birth and higher infant mortality.1-3 Several risk factors for poorer outcomes have been identified, including rurality, socioeconomic and educational disadvantage, smoking and access to services.3-6 Most of the data on these risk factors come from Indigenous people living in rural and remote parts of Australia, or in the western states, where identification of Indigenous people in routine data collections is thought to be more reliable.7,8 However, most Indigenous people live in urban areas on the eastern seaboard, where they represent a low proportion of the total population (2%) and so remain largely invisible. There are limited data on the health and wellbeing of these urban Indigenous populations.
It is generally assumed that issues relating to Indigenous health are related to poverty, yet data relating to socioeconomic status have not been widely reported.2,9 However, research suggests that factors other than socioeconomic differences affect the health of Indigenous people, including dispossession, discrimination, sense of control and power, identity and stress, and that these contribute to and help to explain what are often seen as intractable health and social problems.5-8
The primary study factor was socioeconomic status. As there was limited information available on socioeconomic status in the ODP, we applied the 1996 Australian Bureau of Statistics Socio-Economic Indexes for Areas (SEIFA) index of relative socioeconomic disadvantage, based on maternal suburb of residence.10 This enabled us to rank mothers according to socioeconomic status of their suburb of residence and identify five quintile groups of about equal numbers (ranked from most [Quintile 1] to least [Quintile 5] disadvantaged). We compared the birth outcomes and maternal risk factors for mothers in the most disadvantaged group (three suburbs; Quintile 1) to the remainder (29 suburbs).
Several potential maternal risk factors for birth outcomes including age, single-parent status, and smoking were examined. Maternal age was classified to indicate mothers who were aged less than 20 years at delivery (higher risk group11,12). Mothers were classified as single (also a higher risk group13) if they reported that they were not married or in a de-facto relationship. Mothers were classified as current smokers if smoking during pregnancy was noted in the ODP.
During 2002, 1706 infants were born at the hospital to mothers residing in the LGA. Ninety of these infants were identified as being Indigenous.14
The birth outcomes and risk factors for Indigenous and non-Indigenous infants are compared in Box 1. The mean birthweight for Indigenous infants was lower than that of non-Indigenous infants, and the difference (127 g; 95% CI, 2–254 g) was statistically significant (t1700 = 2.0; P = 0.05). Also, a statistically significant higher proportion of Indigenous (compared with non-Indigenous) infants had birthweights less than 2500 g (Box 1). Apgar scores at 1 minute did not differ between Indigenous and non-Indigenous infants (t1686 = − 2.9; P = 0.8). The proportion of infants admitted to the special-care nursery or neonatal intensive care unit did not differ significantly between the two groups. However, mothers of Indigenous infants were significantly more likely to be aged less than 20 years, to be a single parent, and to smoke during pregnancy than mothers of non-Indigenous infants.
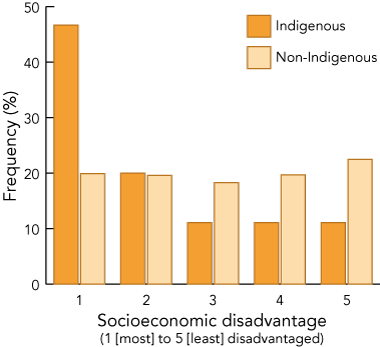
The distribution of Indigenous and non-Indigenous infants by socioeconomic status (based on SEIFA scores) is shown in Box 2. Indigenous infants were more likely to reside in the most socioeconomically disadvantaged areas (Quintile 1) than non-Indigenous infants. Notably, Indigenous infants and their families were found in all five quintile groups.
Box 3 shows that there were no differences in birthweight between Indigenous infants in all quintiles and non-Indigenous infants in Quintile 1. However, the mean birthweight of Indigenous infants in Quintile 1 was 204 g (95% CI, 6–402 g) lower than that of non-Indigenous infants in this quintile (3101 g v 3305 g; t360 = 2.0; P = 0.04). In addition, Indigenous infants in Quintile 1 were more likely to have a low birthweight (< 2500g) than non-Indigenous infants in Quintile 1 (χ21 = 4.4; P = 0.03), and to require admission to special-care nursery or neonatal intensive care unit (χ21 = 4.4; P = 0.04). Mothers of Indigenous infants from Quintile 1 were significantly more likely than mothers of non-Indigenous infants from this quintile to be single (χ21 = 4.5; P = 0.03), to be aged less than 20 years (χ21 = 5.7; P = 0.02), and to smoke during pregnancy (χ21 = 8.0; P = 0.005).
Finally, linear regression models were constructed to further explore risk factors for reduced birthweight (Box 4). In univariate models, lower birthweight was associated with infants’ Indigenous status, and mothers’ single-parent status, smoking and residence in particularly disadvantaged suburbs, but not with mothers’ age of less than 20 years. When all variables were included, lower birthweight was associated with mothers smoking and residing in particularly disadvantaged suburbs, but not with infants’ Indigenous status or mothers’ single-parent status. Interactions between infants’ Indigenous status, mothers’ smoking and mothers’ residence in particularly disadvantaged suburbs were not statistically significant.
This was an exploratory study designed to evaluate the feasibility of identifying Indigenous infants from a population-based clinical record system and extracting the clinical records. There were a number of limitations. First, limited reliable data on socioeconomic status were available. The SEIFA index10 was an ecological summary measure of the area, and may not reflect individual variation in socioeconomic status. While the 1996 index was used for this study,10 our subsequent work with later indices showed that the three suburbs that we included in Quintile 1 did not change. Because of the relatively small size of our study and other data-quality issues relating to the data source, there was limited statistical power to include an extensive range of study and outcomes factors.
Our findings suggest that socioeconomic status does not completely explain the poorer birth outcomes for Indigenous infants. Despite being represented in all five SEIFA Quintiles, Indigenous infants overall had similar outcomes to those of non-Indigenous infants from Quintile 1, and Indigenous infants in Quintile 1 had significantly worse outcomes. These findings concur with those of other Australian research showing differences in mortality rates between Indigenous and non-Indigenous Australians at every socioeconomic level.1,6,15 International research has also indicated that some minority populations, such as African Americans, Inuit, Māori and Scandinavian Sami, are disadvantaged in terms of health at every level of socioeconomic status, regardless of how this is measured.2,11-13,16
Maternal sociodemographic factors, including socioeconomic status, younger age, smoking status and single-parent status, also have a role in birth outcomes.2,3,9 In this study, when we controlled for these factors in multivariate analysis, the association with lower birthweight for Indigenous infants disappeared, suggesting that, superficially, these factors (rather than Indigenous status) explained the observed difference between Indigenous and non-Indigenous birthweights. We suggest that caution is required in interpreting these results, as higher rates of smoking, disadvantage and single-parent status were observed among mothers of Indigenous infants. In controlling for the impact of these factors, we may have inadvertently controlled for more subtle factors associated with being Indigenous that were not measured in the data.
There are also issues specific to Indigenous communities that may explain the differences in birth outcomes between Indigenous and non-Indigenous infants.9 Dispossession has been the subject of an emerging debate, with sociopolitical explanations such as discrimination, sense of control and power, identity, and stress possibly being critical.10,11 Informal discussions with local Indigenous health workers after we analysed the data elicited perceptions of high chronic stress levels among mothers of Indigenous infants, resulting from feelings of disempowerment, complex identity issues and social isolation.
1 Comparison of demographic characteristics and birth outcomes (showing 95% CIs) for Indigenous and non-Indigenous infants born at an outer urban hospital in 2002 to mothers residing in the hospital’s local government area
3 Comparison of birth outcomes and risk factors (showing 95% CIs) between Indigenous infants and non-Indigenous infants residing in the most socioeconomically disadvantaged areas (Quintile 1) born at an outer urban hospital in 2002 to mothers residing in the hospital’s local government area
Received 10 December 2007, accepted 6 August 2008
- Angela T Titmuss1
- Elizabeth Harris2
- Elizabeth J Comino2
- 1 Alice Springs Base Hospital, Alice Springs, NT.
- 2 Centre for Health Equity Training, Research and Evaluation, University of New South Wales, Sydney, NSW.
We acknowledge the support of the Macarthur Aboriginal Home Visiting Team, in particular Sharon Nicholson and Cheryl Woodall, and Tharawal Aboriginal Corporation. Dr Upali Jayasinghe provided statistical advice. This study was facilitated by an earlier grant from the Health Research Foundation Sydney South West to develop part of the methods used in this study.
None identified.
- 1. Najman JM, Williams GM, Bor W, et al. Obstetrical outcomes of Aboriginal pregnancies at a major urban hospital. Aust J Public Health 1994; 18: 185-189.
- 2. Pink B, Allbon P. The health and welfare of Australia’s Aboriginal and Torres Strait Islander peoples 2008. Canberra: Australian Bureau of Statistics and Australian Institute of Health and Welfare, 2008. (ABS Cat. No. 4704.0; AIHW Cat. No. IHW 21.) http://www.aihw.gov.au/publications/index.cfm/title/10583 (accessed Sep 2008).
- 3. de Costa C, Child A. Pregnancy outcomes in urban Aboriginal women. Med J Aust 1996; 164: 523-526.
- 4. Graham S, Pulver LR, Wang YA, et al. The urban–remote divide for Indigenous perinatal outcomes. Med J Aust 2007; 186: 509-512. <MJA full text>
- 5. Roberts CL, Algert CS. The urban and rural divide for women giving birth in NSW, 1990–1997. Aust N Z J Public Health 2000; 24: 291-297.
- 6. Panaretto KS, Mitchell MR, Anderson L, et al. Sustainable antenatal care services in an urban Indigenous community: the Townsville experience. Med J Aust 2007; 187: 18-22. <MJA full text>
- 7. NSW Health. Better practice guidelines to improve the level of Aboriginal and Torres Strait Islander identification within the NSW public health system. Sydney: NSW Health, 2000.
- 8. Ring IT, Brown N. Indigenous health: chronically inadequate responses to damning statistics. Med J Aust 2002; 177: 629-631. <MJA full text>
- 9. Daly A, Smith D. Indicators of risk to the well-being of Australian Indigenous children. Aust Rev Public Aff (ARPA) 2005; 6: 39-57. http://www.australianreview.net/journal/v6/n1/daly_smith.html (accessed Sep 2008).
- 10. Australian Bureau of Statistics. Census of population and housing: Socio-Economic Indexes for Areas (SEIFA), Australia — data only, 1996. Canberra: ABS, 1996. (ABS Cat. No. 2033.0.55.001.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/Lookup/2033.0.55.001Main+ Features11996?OpenDocument (accessed Sep 2008).
- 11. Kupek E, Petrou S, Vause S, Maresh M. Clinical, provider and sociodemographic predictors of late initiation of antenatal care in England and Wales. BJOG 2002; 109: 265-273.
- 12. Jonas O, Roder D, Chan A. The association of low socioeconomic status in metropolitan Adelaide with maternal demographic and obstetric characteristics and pregnancy outcome. Eur J Epidemiol 1992; 8: 708-714.
- 13. Bradley T, Cupples M, Irvine H. A case control study of a deprivation triangle: teenage motherhood, poor educational achievement and unemployment. Int J Adolesc Med Health 2002; 14: 117-123.
- 14. Comino EJ, Titmuss A, Harris E, et al. Identification of Aboriginal infants at an urban hospital. J Paediatr Child Health 2007; 43: 623-626.
- 15. Paradies Y, Cunningham J. Placing Aboriginal and Torres Strait Islander health in an international context. Aust N Z J Public Health 2002; 26: 11-16.
- 16. Eades S, Read AW, Stanley FJ, et al. Bibbulung Gnarneep (“solid kid”): causal pathways to poor birth outcomes in an urban Aboriginal birth cohort. J Paediatr Child Health 2008; 44: 342-346.





Abstract
Objectives: To explore the role of socioeconomic status and Aboriginality on birthweight at an urban hospital.
Design, participants and setting: Extraction of data on the demographic characteristics (socioeconomic status, mothers’ single-parent status, age and smoking status) and infants’ birthweight from a clinical record system. Infants delivered at an outer urban hospital to mothers residing in the local government area during 2002 were included. Infants were identified and results interpreted in consultation with Indigenous health workers.
Main outcome measure: Infant birthweight.
Results: Indigenous infants had a lower mean birthweight than non-Indigenous infants (difference, 127 g), and were more likely to weigh < 2500 g. Mothers of Indigenous infants were more likely to be single, aged < 20 years and to smoke during pregnancy. Lower birthweight was associated with lower socioeconomic status for Indigenous and non-Indigenous infants. Indigenous infants in the most socioeconomically disadvantaged quintile in this study were at higher risk and had a mean birthweight 204 g less than non-Indigenous infants in the same quintile. In multivariate analysis, differences in birthweight were associated with socioeconomic status and smoking during pregnancy.
Conclusions: For both Indigenous and non-Indigenous infants, birthweights were associated with socioeconomic status. Differences between Indigenous and non-Indigenous infants were largely explained by low socioeconomic status and smoking during pregnancy.