Rates of preterm births, low birth-weight and perinatal mortality in the Australian Indigenous population have remained unacceptably high over the past decade, reflecting failure of policy and health care delivery.1,2 Improving perinatal outcomes is heavily dependent on improving the social determinants of health,3 but the health sector has an opportunity to intervene and influence outcomes by providing good antenatal care.4
Since late 1999, health service providers in Townsville, North Queensland, have worked closely with the Indigenous community to improve antenatal services. This collaboration has resulted in an integrated model of shared antenatal care, the Mums and Babies program, delivered from the Townsville Aboriginal and Islanders Health Service (TAIHS). Initial evaluation of this program showed improved access and a reduction in preterm births, but unchanged perinatal mortality.5
Townsville has an Indigenous population of 7675 (5.0% of the population), and at the last census there were 16 875 Indigenous people (5.2%) in the Townsville region (70% Aboriginal and 30% Torres Strait Islander descent).6 TAIHS is an Aboriginal medical service with a 10-member elected board and over 100 staff members. Most Indigenous births in Townsville occur at the Townsville Hospital, the tertiary referral centre for North Queensland.
The Mums and Babies program, which has been described previously,5 commenced on 1 January 2000, integrating three formerly independent providers of antenatal care: TAIHS, and Queensland Health services — the Community Child Health Service and the Institute of Women’s and Children’s Health at Townsville Hospital. The program has a young-family focus (not the traditional antenatal–postnatal care model), and is open to all pregnant women and families with children under the age of 8 years. The program has evolved within a quality improvement framework, including annual clinical audit, client survey and regular program refinement.
Multivariate logistic regression modelling was used to identify significant predictors of inadequate antenatal care attendance (four or fewer visits). Results are presented as odds ratios with 95% CIs. The final model was adjusted for confounders. To place perinatal outcomes in context, results were compared with published state2 and national data,1 which were assumed to be the true population values.
The demographic characteristics of the PreMB group (historical controls) were similar to those of the intervention group, except that in the MB group there were significantly more non-Indigenous women (P < 0.05) and parity was higher (P < 0.01). All women in the PreMB group were residents of Townsville (P < 0.01) (Box 1).
There was a significant increase in the total number of antenatal care visits per pregnancy among the MB group compared with the PreMB group (P < 0.001; Box 2). Townsville-based women made significantly more antenatal care visits (P < 0.001) and presented earlier (P < 0.001) than non-Townsville-based women. The independent risk factors for inadequate antenatal care are shown in Box 3.
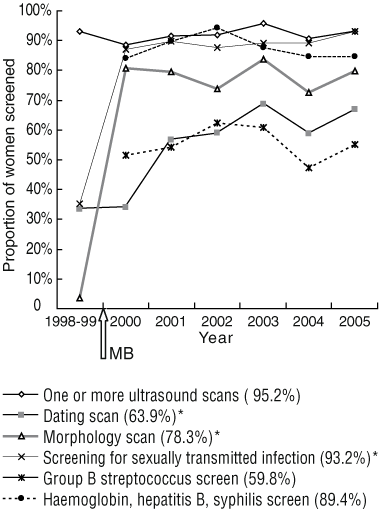
Pregnancy ultrasound scanning and other screening activities over time are shown in Box 4. For the MB group, the morphology scan was performed at a median of 20 weeks’ gestation (IQR, 18–23) over the study period. The trends shown in Box 4 were also seen in the Townsville-based subgroup at slightly higher rates (3%–5% higher). Women in the MB group missing out on screening tests (either an ultrasound scan, or screening for sexually transmitted infections or a minimum blood screen) were significantly more likely to be non-Townsville residents (Townsville residents, 95/533 [17.8%] v non-Townsville residents, 87/248 [35.1%]; P = 0.029).
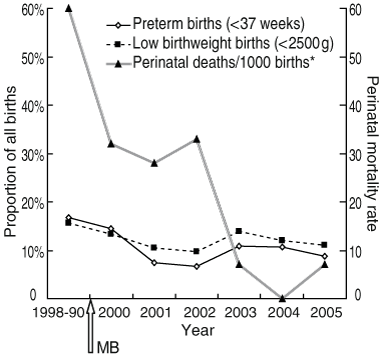
There were improvements in all perinatal outcomes for the MB group compared with the PreMB group, but this improvement only reached significance for perinatal mortality (P = 0.014, Box 5). Similarly, of the improved outcomes, only perinatal mortality reached statistical significance over time (P < 0.01, Box 6). However, among Townsville-based women, there were significant improvements in perinatal outcomes in the MB group compared with the PreMB group: reductions in preterm births (from 14/83 [16.9%] to 45/518 [8.7%]; P < 0.05) and perinatal mortality rate (from 5/83 [60/1000 births] to 6/533 [11/1000 births]; P < 0.01); and an increase in mean birthweight (from 3045 g [95% CI, 2861–3229 g] to 3244 g [95% CI, 3184–3304 g]; P < 0.05), respectively.
The proportion of preterm births in the MB group (9.5%) was similar to that for non-Indigenous births in Queensland (8.0%),2 and in Australia generally (7.6%),1 but significantly lower than the proportion of preterm births to Indigenous women in Queensland in 2000–2004 (13.0%) (Box 5) and in Australia in 2003 (14.1%), respectively (P < 0.05).1,2
The initial 4 years of the Mums and Babies program in Townsville improved access to quality antenatal care and significantly improved preterm birth rates, but not perinatal mortality rates.5 The program has now been running for 7 years. This article extends the evaluation to 781 births over a 6-year period and shows previously reported gains have been sustained, and the reduction in preterm births has now translated into significantly reduced perinatal deaths.
The provision of perinatal care services that are community-based and -focused has been advocated as fundamental to the goal of improving obstetric outcomes in Indigenous communities.7 Recognising the link with chronic disease,8-10 the federal government in 2005 decided to provide significantly increased support for maternal and child health services for Indigenous communities through the Healthy for Life program.11 The Mums and Babies program in Townsville is a community-driven example of how this Healthy for Life policy initiative translates into action.
Use of the Mums and Babies program increased rapidly from its start, and access has been maintained over the 6 years. At least 60% of Townsville-based pregnant Indigenous women are using the service,5 with about 25% returning for care of subsequent pregnancies. The timeliness of the first visit and the number of antenatal visits improved significantly. Although well short of the standard antenatal visits schedule,12 the median number of seven antenatal care visits falls within the bounds of the World Health Organization models focusing on quality rather than quantity of antenatal care.13 Residence outside Townsville was a strong predictor of inadequate antenatal attendance, as was attendance at TAIHS before the commencement of the program. The other predictor for inadequate care — parity (> 4 pregnancies) — suggests that the team needs to further explore the barriers to attendance that these women experience. However, overall, this sustained access to antenatal care suggests that the program has successfully engaged pregnant women — a connection that should endure through the subsequent childhood years.
The proportion of preterm births in the MB group has remained lower than that for whole-of-population figures for Indigenous women in Queensland and is not dissimilar to figures for non-Indigenous women in Queensland2 and Australia.1
The study’s major limitation of selection bias — both the historical control and MB groups were self-selected — means the causative factors for these improvements in perinatal outcome remain debatable. Is it due to accurate dating of pregnancies, or differences in socioeconomic status of the Indigenous community in Townsville? The demographic profile suggests that the women in the MB group carry a significant risk load and are not of high socioeconomic status;14 and there have been no other initiatives in Townsville directed at improving pregnancy care for Indigenous women during the study period. Therefore, we believe that the improvements in perinatal outcome in the intervention group are a result of the model of antenatal care developed through the Mums and Babies program: completion of key clinical activities, together with the brief intervention for risk factors afforded by improved access to care.
Finally, the project offers potential population health gains. It generates rich, prospectively collected data that may be useful in the future and may help ameliorate the overwhelming Indigenous burden of chronic disease.8-10,15 Another significant impact is the capacity building at TAIHS, a key action in effecting health promotion, empowering people to take greater control of their health and thereby reduce health inequity.16 This has resulted in part from the framework of the program and its longevity. A quality improvement framework and continuous evaluation of this project — key components of change management17 — have played a significant role in introducing a culture of quality18 to medical service delivery at TAIHS. Evaluation has encouraged staff to engage in further education, enabled TAIHS to participate in community-focused research projects that have added value to service delivery, enhanced primary prevention activity, and helped retain staff. The net result has been the development of sustainable health infrastructure within the organisation and a commitment to quality in health service delivery.
1 Demographic characteristics of women attending TAIHS for shared antenatal care, 2000–2005 (MB group) compared with a historical control, 1998–1999 (PreMB group)*
2 Patterns of antenatal visits for women attending TAIHS for antenatal care, 2000–2005 (MB group), compared with a historical control, 1998–1999 (PreMB group)
3 Multivariate logistic regression analysis of independent predictors of inadequate antenatal care attendance*
4 Antenatal screening of all women attending TAIHS, 2000–2005, showing the increased proportion of women in the MB group screened
 | |||||||||||||||
5 Perinatal outcomes for Indigenous births to women attending TAIHS (MB group), 2000–2005 compared with a historical control (PreMB group), 1998–1999, and with Indigenous births in Queensland 2000–20042
6 Perinatal outcomes for Indigenous births to women attending TAIHS for shared antenatal care, 1998–2005
Received 8 February 2007, accepted 10 April 2007
- Kathryn S Panaretto1
- Melvina R Mitchell1
- Lynette Anderson1
- Sarah L Larkins1,2
- Vivienne Manessis1
- Petra G Buettner2
- David Watson3
- 1 Townsville Aboriginal and Islanders Health Service, Townsville, QLD.
- 2 James Cook University, Townsville, QLD.
- 3 Women's and Children's Health Institute, Townsville Hospital, Townsville, QLD.
None identified.
- 1. Laws PJ, Sullivan EA. Australia’s mothers and babies 2003 Sydney: Australian Institute of Health and Welfare National Perinatal Statistics Unit, 2005. (AIHW Catalogue No. PER 29; Perinatal Statistics Series No. 16.) http://www.npsu.unsw.edu.au/NPSUweb.nsf/resources/AMB_1999-2002/$file/ps16.pdf (accessed Apr 2007).
- 2. Queensland Council on Obstetric and Paediatric Morbidity and Mortality. Maternal, perinatal and paediatric mortality and morbidity in Queensland, 2000–2004. Brisbane: QCOPMM, 2005.
- 3. Lumley J. Defining the problem: the epidemiology of preterm birth. BJOG 2003; 110 Suppl 20: 3-7.
- 4. Main D. The epidemiology of preterm birth. Clin Obstet Gynecol 1988; 31: 521-532.
- 5. Panaretto KS, Lee H, Mitchell M, et al. Impact of a collaborative shared antenatal care program for urban indigenous women: prospective cohort study. Med J Aust 2005; 182: 514-519. <MJA full text>
- 6. Australian Bureau of Statistics. Population distribution, Indigenous Australians, 2001. Canberra: ABS, 2002. (Catalogue No. 4705.0.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/Lookup/4705.0Main+Features12001?OpenDocument (accessed Apr 2007).
- 7. O’Connor MC, Bush A. Pregnancy outcomes of Australian Aboriginals and Torres Strait Islanders. Med J Aust 1996; 164: 516-517.
- 8. Barker DJ, Winter PD, Osmond C, et al. Weight in infancy and death from ischaemic heart disease. Lancet 1989; 2: 577-580.
- 9. Barker DJ. Birthweight and hypertension. Hypertension 2006; 48: 357-358.
- 10. Singh G, Hoy W. The association between birthweight and current blood pressure: a cross-sectional study in an Australian Aboriginal community. Med J Aust 2003; 179: 532-535. <MJA full text>
- 11. Australian Government Department of Health and Ageing. Healthy for life. 2006. http://www.health.gov.au/healthyforlife (accessed Apr 2007).
- 12. Hunt JM, Lumley J. Are recommendations about routine antenatal care in Australia consistent and evidence-based? Med J Aust 2002; 176: 255-259. <MJA full text>
- 13. Carroli G, Villar J, Piaggio G, et al. WHO systematic review of randomised controlled trials of routine antenatal care. Lancet 2001; 357: 1565-1570.
- 14. Panaretto K, Lee H, Mitchell M, et al. Risk factors for preterm, low birth weight and small for gestational age birth in urban Aboriginal and Torres Strait Islander women in Townsville. Aust N Z J Public Health 2006; 30: 163-170.
- 15. Zhao Y, Guthridge S, Magnus A, Voss T. Burden of disease and injury in Aboriginal and non-Aboriginal populations in the Northern Territory. Med J Aust 2004; 180: 498-502. <MJA full text>
- 16. World Health Organization. Health promotion. The Bangkok Charter for health promotion in a globalized world. http://www.who.int/healthpromotion/conferences/6gchp/bangkok_charter/en/ (accessed Apr 2007).
- 17. Lamb MC, Cox MAA. Implementing change in the national health service. J Manag Med 1999; 13: 288-297.
- 18. Weber V, Joshi M. Effecting and leading change in health care organisations. Jt Comm J Qual Improv 2000; 26: 388-399.





Abstract
Objective: To evaluate the impact of a sustained, community-based collaborative approach to antenatal care services for Indigenous women.
Design: Prospective quality improvement intervention, the Mums and Babies program, in a cohort of women attending Townsville Aboriginal and Islanders Health Service, 1 January 2000 – 31 December 2005 (MB group), compared with a historical control group (PreMB group), 1 January 1998 – 30 June 1999.
Main outcome measures: Proportion of women having inadequate antenatal care and screening; perinatal indicators.
Results: The number of antenatal visits per pregnancy increased from three (interquartile range [IQR], two to six) in the PreMB group to six (IQR, four to ten) in the MB group (P < 0.001). There were significant improvements in care planning, completion of cycle-of-care, and antenatal education activities throughout the study period. About 90% of all women attending for antenatal care were screened for sexually transmitted diseases, 89% had measurement of haemoglobin level, and serological tests for hepatitis B and syphilis (minimum antenatal screening). There was increased attendance for dating and morphology scans. In the MB group compared with the PreMB group, there was a significant reduction in perinatal mortality (14 v 60 per 1000 births; P = 0.014).
Conclusion: Sustained access to a community-based, integrated, shared antenatal service has improved perinatal outcomes among Indigenous women in Townsville.