To the Editor: In the preceding article, we report on a substantial rise in prevalence rates of gonorrhoea in a population in remote Central Australia.1 This rise occurred in the context of a sustained major reduction in sexually transmitted infections (STIs) in the region, achieved by a comprehensive program of STI control, described in the article1 and previously.2
We found that the gonorrhoea outbreak was not due to penicillin resistance of the causative organism, and we hypothesise that it was due to the introduction and dominance of a more infectious clone.3,4 This rise in gonorrhoea in a region widely acknowledged to have the most successful STI control program in the country prompted several commentators to argue that both this program, and screening as a measure for STI control in remote Indigenous communities, had failed, and to advocate a range of other approaches.5
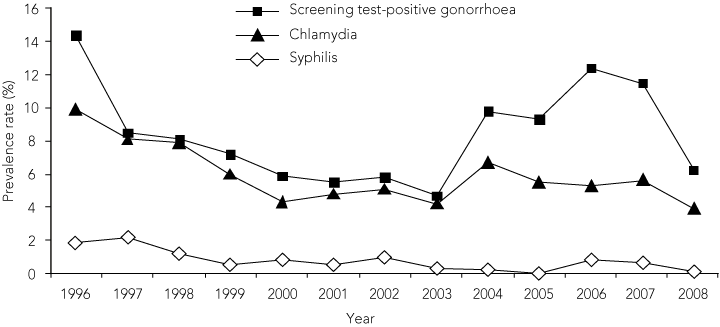
We recently completed the analysis of the 2008 annual population-wide STI screen, which achieved a 78% participation rate among eligible participants. These data strongly suggest that the gonorrhoea outbreak seen over the previous 4 years has been controlled (Box). Furthermore, the current prevalence rates are among the lowest seen in the past decade. These findings suggest that a comprehensive STI control program, such as that delivered by the Nganampa Health Council, can not only reduce STI rates, but also control outbreaks, provided the program is sustained.
- Rae-Lin Huang1
- Paul J Torzillo1
- Adrienne C Kirby2
- 1 Nganampa Health Council, Alice Springs, NT.
- 2 NHMRC Clinical Trials Centre, University of Sydney, Sydney, NSW.
- 1. Huang R-L, Torzillo PJ, Hammond VA, et al. Epidemiology of sexually transmitted infections on the Anangu Pitjantjatjara Yankunytjatjara Lands: results of a comprehensive control program. Med J Aust 2008; 189: 442-445.
- 2. Miller PJ, Torzillo PJ, Hateley W. Impact of improved diagnosis and treatment on prevalence of gonorrhoea and chlamydial infection in remote aboriginal communities on Anangu Pitjantjatjara Lands. Med J Aust 1999; 170: 429-432.
- 3. Choudery B, Risley CL, Ghani AC, et al. Identification of individuals with gonorrhoea within sexual networks: a population-based study. Lancet 2006; 368: 139-146.
- 4. Sarafian SK, Knapp JS. Molecular epidemiology of gonorrhea. Clin Microbiol Rev 1989; 2 Suppl: S49-S55.
- 5. Bowden FJ, Fethers K. “Let’s not talk about sex”: reconsidering the public health approach to sexually transmissible infections in remote Indigenous populations in Australia. Med J Aust 2008; 188: 182-184. <MJA full text>