A 67-year-old man presented to the rheumatology clinic with uncontrolled rheumatoid arthritis, which was being treated with leflunomide and prednisone. He had previously not responded to gold, methotrexate and cyclosporin. His other medical history included partial gastrectomy, diabetes mellitus and chronic renal impairment.
In preparation for treatment with a tumour necrosis factor (TNF) receptor antagonist, a plain chest radiograph and tuberculin skin test were performed. The radiograph was clear, but the tuberculin skin response was strongly positive at 26 mm. The patient had received BCG vaccination more than 50 years earlier. His tuberculosis risk factors were a family history in his grandfather, and being from Eastern Europe. Given these findings, isoniazid was initiated for treatment of latent tuberculosis, with a proposed treatment plan of 6 months.
Two months later, the patient presented with fever, night sweats and a painful left hip with reduced range of movement. Ultrasound showed a large collection extending from the hip joint. The hip joint aspirate showed a mild neutrophilic infiltrate, but no organisms were detected and polymerase chain reaction (PCR) testing for Mycobacterium tuberculosis was negative.
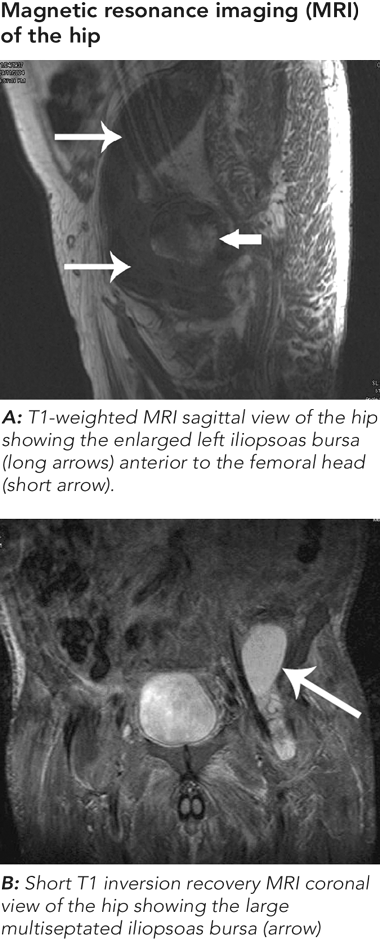
Magnetic resonance imaging (MRI) of the hip revealed a large iliopsoas collection with femoral head signal changes and flattening (Figures). An infective cause was suspected, so arthroscopic lavage of the left hip and computed tomography (CT)-guided aspiration of the iliopsoas collection were performed. The aspirate removed 50 mL of fluid containing mildly increased neutrophils, but showed no evidence of M. tuberculosis by microscopy, culture or PCR. Nuclear technetium-99 scintigraphy showed uptake only in the femoral head, suggestive of osteonecrosis, with a differential diagnosis of osteomyelitis. A subsequent CT-guided biopsy of the psoas collection wall did not show any evidence of tuberculosis by histology, culture or PCR.
Two months later, a repeat CT scan showed resolution of the psoas collection, but persistence of the left hip effusion. The patient was treated with quadruple antituberculosis therapy for 2 months, but this was ceased because of diarrhoea secondary to Clostridium difficile. Over the next 4 months, several attempts to sequentially administer one to two antituberculosis medications were interrupted by recurrent episodes of pseudomembranous colitis caused by C. difficile infection, leading to total withdrawal of antituberculosis medications.
Over the ensuing months, the left hip pain continued to worsen. Tuberculosis was still considered the most likely diagnosis and an arthroscopic biopsy of the left hip synovium was performed. This showed a non-specific chronic synovitis, but no granulomas and no acid-fast bacilli on PCR testing or culture.
The patient underwent a total hip replacement 8 months after his initial presentation with left hip pain. Histology of the hip revealed osteonecrosis of the femoral head, synovial inflammation from rheumatoid arthritis and no evidence of tuberculosis. The iliopsoas collection was thought to be due to a giant iliopsoas bursa that did not recur after aspiration.
Our patient had an enlarged iliopsoas bursa associated with osteonecrosis of the femoral head mimicking a tuberculous psoas abscess.
Rheumatoid arthritis is a recognised cause of giant iliopsoas bursae.1-3 Other conditions leading to an enlarged iliopsoas bursa include acute trauma and overuse injuries. Infections can also result in iliopsoas bursitis or abscess formation.4 A number of organisms have been reported, with pyogenic bacteria, most commonly Staphylococcus aureus, implicated in most cases.5,6 Tuberculosis, once a well recognised causative agent of iliopsoas abscesses, is now less frequently reported in the Western world.6
Anti-TNF therapies are being increasingly used for treatment of inflammatory arthropathies, but can cause reactivation of tuberculosis.7 Patients with rheumatoid arthritis treated with anti-TNF agents have higher than background rates of tuberculosis, and are more likely to develop extrapulmonary or disseminated disease.8-10 There are mechanistic reasons why this may occur, specifically relating to inhibition of T-cell numbers and activation,11 as well as interference with granuloma formation.10,12
Assessment for tuberculosis in patients being considered for anti-TNF therapy should include clinical history, particularly previous tuberculosis exposure, prior tuberculosis treatment or BCG vaccination, physical examination, chest radiograph, and in appropriate cases, tuberculin skin testing.13 Patients with abnormal radiographs or who are at high risk should be assessed by a tuberculosis specialist.
False positive tuberculin skin tests are seen both with previous BCG vaccination and with environmental mycobacteria.14 Interferon ? tests have the advantage of being less influenced by prior BCG vaccination and show stronger correlation in groups with tuberculosis exposure compared with tuberculin skin tests.14 A significant problem with tuberculin skin tests is the potential for false negative results in the context of immunosuppressive therapy. Patients on immunosuppressive treatment may also show increased rates of indeterminate results using the interferon ? tests.15
Latent tuberculosis is defined as having no signs or symptoms of tuberculosis, a positive tuberculin skin test (allowing for the specific clinical condition), and certain risk factors such as typical tuberculosis chest radiograph abnormalities or an immunosuppressive condition or treatment.14,16 In our patient, the tuberculin skin test was positive and he had both immunosuppressive disease and treatment. However, we found no tissue-specific histopathological or microbiological evidence for tuberculosis, despite multiple interventions.
Current guidelines suggest that latent tuberculosis in the context of an abnormal chest radiograph should be treated either with isoniazid alone or with isoniazid and rifampicin, ideally before initiation of anti-TNF therapy.13 Of note, even after sustained prophylactic anti-tuberculous treatment, some patients may still develop tuberculosis reactivation following treatment with anti-TNF agents.13,17
Although the incidence of tuberculosis in patients from non-tuberculosis-endemic countries such as Australia is generally low,18 previously common extrapulmonary manifestations of tuberculosis such as iliopsoas abscesses may need to be considered more carefully once again. Furthermore, in patients treated with anti-TNF agents, given the imperfect screening tests for tuberculosis, especially in immunosuppressed patients, increased vigilance is needed for both extrapulmonary and disseminated tuberculosis. In this context, screening early in the course of inflammatory arthritis may be very useful.
- 1. Coventry MB, Polley HF, Weiner AD. Rheumatoid synovial cyst of the hip; report of three cases. J Bone Joint Surg Am 1959; 41-A: 721-730.
- 2. Kataoka M, Torisu T, Nakamura M, Uchida K. Iliopsoas bursa of the rheumatoid hip joint. A case report and review of the literature. Clin Rheumatol 1995; 14: 358-364.
- 3. Generini S, Matucci-Cerinic M. Iliopsoas bursitis in rheumatoid arthritis. Clin Exp Rheumatol 1993; 11: 549-551.
- 4. Johnston CA, Wiley JP, Lindsay DM, Wiseman DA. Iliopsoas bursitis and tendinitis. A review. Sports Med 1998; 25: 271-283.
- 5. Huang JJ, Ruaan MK, Lan RR, Wang MC. Acute pyogenic iliopsoas abscess in Taiwan: clinical features, diagnosis, treatments and outcome. J Infect 2000; 40: 248-255.
- 6. Mallick IH, Thoufeeq MH, Rajendran TP. Iliopsoas abscesses. Postgrad Med J 2004; 80: 459-462.
- 7. Crum NF, Lederman ER, Wallace MR. Infections associated with tumor necrosis factor-alpha antagonists. Medicine (Baltimore) 2005; 84: 291-302.
- 8. Gomez-Reino JJ, Carmona L, Valverde VR, et al; BIOBADASER Group. Treatment of rheumatoid arthritis with tumor necrosis factor inhibitors may predispose to significant increase in tuberculosis risk: a multicenter active-surveillance report. Arthritis Rheum 2003; 48: 2122-2127.
- 9. Strangfeld A, Listing J. Infection and musculoskeletal conditions: bacterial and opportunistic infections during anti-TNF therapy. Best Pract Res Clin Rheumatol 2006; 20: 1181-1195.
- 10. Gardam MA, Keystone EC, Menzies R, et al. Anti-tumour necrosis factor agents and tuberculosis risk: mechanisms of action and clinical management. Lancet Infect Dis 2003; 3: 148-155.
- 11. Hamdi H, Mariette X, Godot V, et al; RATIO (Recherche sur Anti-TNF et Infections Opportunistes) Study Group. Inhibition of anti-tuberculosis T-lymphocyte function with tumour necrosis factor antagonists. Arthritis Res Ther 2006; 8: R114.
- 12. Mohan AK, Cote TR, Siegel JN, et al. Infectious complications of biologic treatments of rheumatoid arthritis. Curr Opin Rheumatol 2003; 15: 179-184.
- 13. British Thoracic Society Standards of Care Committee. BTS recommendations for assessing risk and for managing Mycobacterium tuberculosis infection and disease in patients due to start anti-TNF-alpha treatment. Thorax 2005; 60: 800-805.
- 14. National Collaborating Centre for Chronic Conditions. Diagnosis. In: Clinical diagnosis and management of tuberculosis and measures for its prevention and control. London: Royal College of Physicians of London, 2006; 27-50. http://guidance.nice.org.uk/CG33/guidance (accessed Aug 2007).
- 15. Ferrara G, Losi M, Meacci M, et al. Routine hospital use of a new commercial whole blood interferon-gamma assay for the diagnosis of tuberculosis infection. Am J Respir Crit Care Med 2005; 172: 631-635.
- 16. Furst DE, Cush J, Kaufmann R, et al. Preliminary guidelines for diagnosing and treating tuberculosis in patients with rheumatoid arthritis in immunosuppressive trials or being treated with biological agents. Ann Rheum Dis 2002; 61 Suppl 2: ii62-ii63.
- 17. Imperato AK, Smiles S, Abramson SB. Long-term risks associated with biologic response modifiers used in rheumatic diseases. Curr Opin Rheumatol 2004; 16: 199-205.
- 18. Roche P, Bastian I, Krause V, et al; National Tuberculosis Advisory Committee. Tuberculosis notifications in Australia, 2005. Commun Dis Intell 2007; 31: 71-80.





None identified.