Over the past decade, wide international interest in improving preventive health services has led to the development of preventive care guidelines in various countries, including the United States,1 Canada2 and Australia.3 Furthermore, tailored guidelines have been introduced to accommodate the needs of specific populations such as Aboriginal and Torres Strait Islander peoples.4
Despite wide distribution of preventive care guidelines, delivery of preventive services in practice is suboptimal. A national survey undertaken in the US revealed that, among adults, 55% of recommended preventive care was provided.5 A study of remote Aboriginal communities in the Northern Territory showed that, on average, 40%–50% of preventive services were delivered, in line with guidelines, to well adults aged over 16 years.6 Improving this level of delivery or uptake of preventive services is a particular challenge in the Aboriginal population, which has exceptionally high and increasing rates of chronic disease.
A number of studies have demonstrated that neither dissemination of preventive care guidelines alone7 nor a favourable attitude toward preventive services among health care providers8 is sufficient to affect the actual delivery of preventive services. It has become increasingly apparent that improving the quality of chronic illness care and preventive care will require reorientation of health care systems. The chronic care model (CCM) described by Bodenheimer et al9 provides a framework for understanding systems that could support chronic illness care and guide organisational development. Research shows that CCM-oriented interventions have been effective in improving chronic illness care,10 and the model has also been recommended as a template for improving preventive care.11 However, there is a lack of empirical evidence to support such recommendations.
We developed a CCM-oriented quality improvement intervention to support Aboriginal community health centre staff to improve their primary care systems for chronic illness care and preventive care. The impact of the intervention on disease management has been reported elsewhere.12 Here we report on changes in the delivery of preventive services in Aboriginal primary care services to adults who had no known diagnosis of chronic disease that occurred in association with our systems-oriented intervention and consider the application of the chronic care model to preventive care.
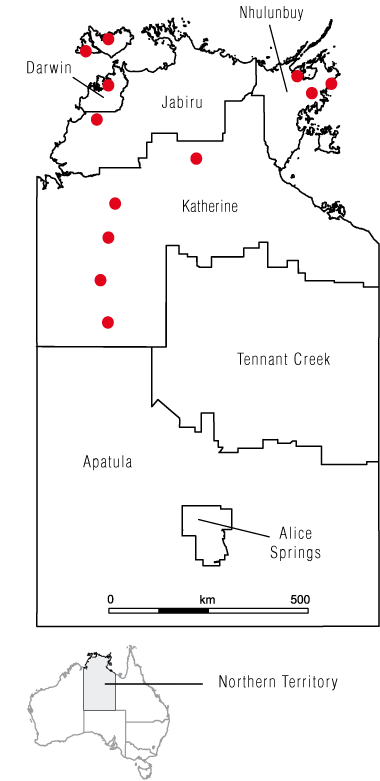
Our study was conducted in the Top End of the NT, an area occupying 522 561 km2, with an estimated resident population of 153 687 in 2003.13 Aboriginal people comprise about 30% of the total population of the NT, and over 70% of them live outside the major service centres. A majority of Aboriginal people access primary health care through community health centres, which are operated under a variety of funding and governance models.14 From a total of 53 Aboriginal community health centres in the Top End, we selected 12 health centres that we considered to reflect the diversity of centres in the region in terms of governance arrangements, geographic location and community size (Box 1).
The intervention study was conducted between January 2002 and December 2005 and featured two annual cycles of assessment, feedback, action planning, implementation and reassessment. The approach, rationale and principles underpinning the research are based on modern continuous quality improvement theory and participatory community-based research and have been reported previously.15
Two instruments were used for assessment.
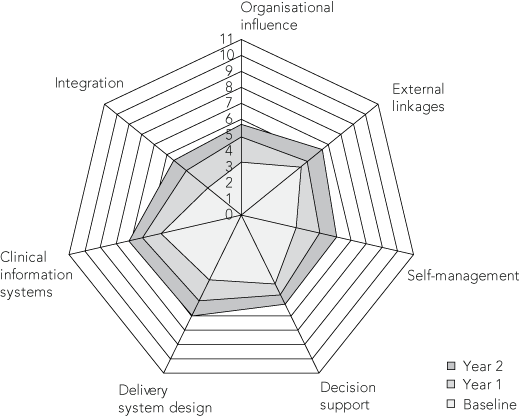
Firstly, an adapted version of the Assessment of Chronic Illness Care (ACIC) scale16 was used to evaluate the state of health centre system development with regard to prevention and management of chronic illness. The adapted version of the scale included 34 items that were grouped into seven components (six as outlined in the CCM, plus an integration component). Based on health centre staff consensus, each item was given a score indicating the state of development, ranging from 0 (not at all) to 11 (fully developed).17,18 The mean was calculated from individual item scores to create a component score, and the mean of the seven component scores formed the overall system score for the community health centre. The scale served both as a measurement tool and an intervention tool, as the discussion of system components led to better understanding among staff of the quality of systems and consideration of how systems could be improved.
Our standardised audit form was based on previous research work in this area,6 and included a list of 12 scheduled services (listed in Box 4) that local clinical guidelines recommend for delivery to adults aged 16–49 years on an annual basis (except for pneumococcal vaccine, which was scheduled for delivery every 5 years).19 A service was assessed as delivered if there was a record of delivery within the specific period preceding the audit.
At each participating health centre, 10% of the records audited at baseline were selected randomly and audited again 1–2 months later by the same auditor for the same calendar period. Each health centre contributed three records, so that the total reliability audit sample comprised 36 records. Intra-rater reliability for audit items, measured by κ statistics,20 ranged from 0.79 to 0.93.
Study participants at baseline, Year 1 and Year 2 audits had similar age and sex compositions (Box 2). There were similar attendance rates at health centres within the previous 12 months at baseline and Year 1 audits, but a fall in attendance at the Year 2 audit. Of adults attending health centres within the 12 months before the baseline audit, the primary reason for the most recent visit was acute care (75%), followed by well person’s check (12%), sexual health (8%) and immunisation (5%). This pattern of attendance remained largely unchanged over the study period.
The status of health centre system development (as reflected in the ACIC scale) is visually illustrated in the form of a spider plot (Box 3). Participating health centres experienced marked improvements across each system component over the study period.
During the course of the study, implementation of actions to change systems varied between participating health centres. Those most relevant to improving preventive care were related to “external linkages” (including outreach and health promotion type initiatives) and “organisational influence” (including use of management processes to demonstrate interest in preventive care and securing new resources) components of the CCM. However, other initiatives covered the scope of CCM components: for example, development of local language concepts (self-management support); training by visiting specialists (decision support); revision of team roles and use of interpreters (delivery system design); and review of information system function and development of reminder systems (clinical information systems). The range of actions and strategies relevant to improving preventive services was relatively limited in comparison to those relevant to diabetes management.12
Changes in delivery of individual preventive services from baseline to Year 2 are shown in Box 4. Of the 12 services measured, four services (counselling on diet, physical activity, smoking and alcohol), which had very low levels of delivery at baseline, achieved statistically significant improvements at the Year 2 audit. Other services showed little improvement. The delivery of one service, pneumococcal vaccination, actually declined significantly, from 35% at baseline to 25% at Year 2.
The improvements in health centre systems that occurred during our quality improvement intervention were associated with little or no improvement in delivery of preventive services to well adults. This is in contrast to improvements that occurred in delivery of care to people with diabetes over the same period.12 The delivery of preventive services relating to counselling on lifestyle changes, which had a low level of delivery at baseline, showed the greatest percentage improvements. Important measures such as monitoring waist circumference, blood pressure and blood glucose level, and delivery of pneumococcal vaccination, showed no improvement.
In contrast to our experience, a Canadian study of a focused intervention for adults attending health check-ups showed a significantly higher level of delivery of preventive services in the intervention group (72%) compared with the control group (49%).21 Such focused interventions are likely to miss many opportunities, as only those adults attending for health check-ups are targeted. Indeed, our data showed that only about 10% of adults attended community health centres primarily for a well person check. Hence there is a need for broad system interventions. A continuous quality improvement intervention on delivery of preventive services in primary care settings in the US22 showed similarly disappointing findings to ours. The authors ascribed the failure of the intervention to two major factors: (i) relatively high rates of preventive service delivery at baseline, which left a relatively small margin for further improvement; and (ii) inadequate implementation of the intervention to change systems. By contrast, in our study, delivery of preventive services at baseline was low, leaving ample room for improvement.
The principal reason for failure to improve delivery of preventive services in our study appears to lie in the focus and implementation of change in health centres. Health service providers in our study tended to emphasise strategies and actions related to chronic illness management,12 rather than preventive services for generally well adults. Information presented to health centre staff as part of the intervention clearly drew attention to low levels of delivery of preventive services. However, the response in terms of identified strategies for improving preventive care and actual delivery of care was poor compared with strategies for chronic disease management. The improvements in chronic disease management were achieved despite significant ongoing constraints on financial, staffing and other resources, and the same should be achievable for preventive care.
In the broader context, there has been an increasingly positive policy environment in Australia for promoting delivery of preventive services. This includes the introduction of specific Medicare Benefits Scheme (MBS) items in 1999 to reimburse general practitioners for providing preventive services for all Australians aged over 75 years and for Indigenous people over the age of 55 years.23 This initiative was expanded in 2004 to include Indigenous people aged 15–54 years.24 However, a recently published evaluation showed that the uptake of preventive service MBS items among Indigenous populations has been slow.25 In our study, half of participating centres reported some use of the MBS items,16 but it was not possible to determine the specific effect of this in our study. Moreover, while the MBS rebates provide incentives for individual (and private) GPs to deliver preventive services, they may have less effect in motivating practitioners working in remote Indigenous community health centres, who are usually in salaried positions. Moreover, rebates are not currently claimable by remote area nurses or Aboriginal health workers. This example is just one illustration of the need for system development at health centre level to help implement higher level policy initiatives at the coalface.
1 Distribution of the 12 participating community health centres in the Top End of the Northern Territory
- Damin Si1
- Ross S Bailie1
- Michelle Dowden1
- Lynette O’Donoghue1
- Christine Connors2
- Gary W Robinson3
- Joan Cunningham1
- John R Condon1
- Tarun S Weeramanthri2
- 1 Menzies School of Health Research, Charles Darwin University, Darwin, NT.
- 2 Northern Territory Department of Health and Community Services, Darwin, NT.
- 3 School for Social and Policy Research, Charles Darwin University, Darwin, NT.
We gratefully acknowledge the support of staff and management of the participating community health centres. Our project was funded by the Australian Health Ministers’ Advisory Council and the Cooperative Research Centre for Aboriginal Health. Damin Si’s work is supported by a National Health and Medical Research Council (NHMRC) Population Health Capacity Building Grant. Ross Bailie’s work is supported by an NHMRC Senior Research Fellowship. Joan Cunningham’s work is supported by an NHMRC Career Development Award.
None identified.
- 1. United States Preventive Services Task Force. Guide to clinical preventive services, 2005. http://www.ahrq.gov/clinic/pocketgd05 (accessed Sep 2007).
- 2. Canadian Task Force on the Periodic Health Examination. The Canadian guide to clinical preventive health care. Ottawa: Health Canada, 1994.
- 3. The National Preventive and Community Medicine Committee of the Royal Australian College of General Practitioners. Guidelines for preventive activities in general practice. Aust Fam Physician 2002; 31: S1-S61.
- 4. National Aboriginal Community Controlled Health Organisation. National guide to a preventive health assessment in Aboriginal and Torres Strait Islander peoples. Melbourne: Royal Australian College of General Practitioners, 2005. http://www.racgp.org.au/guidelines/nationalguide (accessed Sep 2007).
- 5. McGlynn EA, Asch SM, Adams J, et al. The quality of health care delivered to adults in the United States. N Engl J Med 2003; 348: 2635-2645.
- 6. Bailie RS, Togni SJ, Si D, et al. Preventive medical care in remote Aboriginal communities in the Northern Territory: a follow-up study of the impact of clinical guidelines, computerised recall and reminder systems, and audit and feedback. BMC Health Serv Res 2003; 3: 15.
- 7. Feder G, Eccles M, Grol R, et al. Clinical guidelines: using clinical guidelines. BMJ 1999; 318: 728-730.
- 8. Solberg LI, Brekke ML, Kottke TE. How important are clinician and nurse attitudes to the delivery of clinical preventive services? J Fam Pract 1997; 44: 451-461.
- 9. Bodenheimer T, Wagner EH, Grumbach K. Improving primary care for patients with chronic illness. JAMA 2002; 288: 1775-1779.
- 10. Piatt GA, Orchard TJ, Emerson S, et al. Translating the chronic care model into the community: results from a randomized controlled trial of a multifaceted diabetes care intervention. Diabetes Care 2006; 29: 811-817.
- 11. Glasgow RE, Orleans CT, Wagner EH. Does the chronic care model serve also as a template for improving prevention? Milbank Q 2001; 79: 579-612.
- 12. Bailie R, Si D, Dowden M, et al. Improving organisational systems for diabetes care in Australian Indigenous communities. BMC Health Serv Res 2007; 7: 67.
- 13. Australian Bureau of Statistics. Regional statistics, Northern Territory, 2004. Canberra: ABS, 2004. (ABS Cat. No. 1362.7.)
- 14. Condon J, Warman G, Arnold L, editors. The health and welfare of Territorians. Darwin: Epidemiology Branch, Territory Health Services, 2001.
- 15. Bailie R, Si D, Dowden M, O’Donoghue L. Indigenous health: effective and sustainable health services through continuous quality improvement. Med J Aust 2007; 186: 525-527. <MJA full text>
- 16. Si D, Bailie R, Connors C, et al. Assessing health centre systems for guiding improvement in diabetes care. BMC Health Serv Res 2005; 5: 56.
- 17. Improving Chronic Illness Care. Assessment of chronic illness care, version 3.5. http://www.improvingchroniccare.org/downloads/acic_v3.5a.pdf (accessed: Sep 2007).
- 18. Bonomi AE, Wagner EH, Glasgow RE, VonKorff M. Assessment of chronic illness care (ACIC): a practical tool to measure quality improvement. Health Serv Res 2002; 37: 791-820.
- 19. Central Australian Rural Practitioner Association. CARPA standard treatment manual: a clinic manual for primary health care practitioners in remote and rural communities in Central and Northern Australia. 4th ed. Alice Springs: CARPA, 2003.
- 20. Altman DG. Practical statistics for medical research. London: Chapman and Hall, 1991.
- 21. Dubey V, Mathew R, Iglar K, et al. Improving preventive service delivery at adult complete health check-ups: the Preventive health Evidence-based Recommendation Form (PERFORM) cluster randomized controlled trial. BMC Fam Pract 2006; 7: 44.
- 22. Solberg LI, Kottke TE, Brekke ML, et al. Failure of a continuous quality improvement intervention to increase the delivery of preventive services. A randomized trial. Eff Clin Pract 2000; 3: 105-115.
- 23. Australian Government Department of Health and Ageing. Enhanced Primary Care Program (EPC). http://www.health.gov.au/epc (accessed Jul 2007).
- 24. Australian Government Department of Health and Ageing. Enhanced Primary Care Program (EPC). Medicare health checks for Aboriginal and Torres Strait Islander Australians — fact sheet. http://www.health.gov.au/internet/wcms/publishing.nsf/Content/pacd-medicare-healthchecks-factsheet.htm (accessed Sep 2007).
- 25. Kelaher M, Dunt D, Thomas D, Anderson I. Comparison of the uptake of health assessment items for Aboriginal and Torres Strait Islander people and other Australians: implications for policy. Aust New Zealand Health Policy 2005; 2: 21.





Abstract
Objective: To describe changes in delivery of preventive services among adults in Aboriginal communities that occurred in association with a systems-oriented intervention.
Design, setting and participants: A quality improvement intervention with a 2-year follow-up was undertaken at 12 Aboriginal community health centres in the Northern Territory between January 2002 and December 2005. The study involved 360 well adults aged 16–49 years who had no known diagnosis of chronic disease.
Intervention: Two annual cycles of assessment, feedback workshops, action planning, and implementation of system changes. Assessment included a structured review of health service systems and an audit of clinical records.
Main outcome measures: Adherence to guideline-scheduled preventive services including taking basic measurements, laboratory investigations, lifestyle counselling and pneumococcal vaccination.
Results: Of 12 preventive services measured, delivery of four services showed improvement over the study period: counselling on diet increased from 3% to 8% (P = 0.018); counselling on physical activity from 2% to 8% (P = 0.006); counselling on smoking from 2% to 11% (P = 0.003); and counselling on alcohol from 2% to 10% (P = 0.007). There was no improvement in important measures such as monitoring of waist circumference, blood pressure and blood glucose level, and delivery of pneumococcal vaccination.
Conclusion: Our systems-oriented intervention was associated with some improvement in counselling activities, but no significant improvement in delivery of other preventive services. The main reason may be that implementation focused more on chronic illness management than preventive services for generally well adults.