A recent editorial in the Bulletin of the World Health Organization called for international agencies and ministries of health to work together to implement integrated quality improvement processes in clinical practice, with the aim of scaling up delivery of health interventions to meet the Millennium Development Goals.1 The current Australian Government program, Healthy for Life,2 provides a mechanism for doing this in primary care services for Aboriginal and Torres Strait Islander peoples. With funding of $102.4 million over 4 years, the program aims
In general, CQI aims to facilitate ongoing improvement by using objective data to analyse and improve processes.3,4 Emphasis is placed on efficient and effective functioning of organisational systems.5,6 CQI involves an ongoing cycle of gathering data on how well organisational systems are functioning, and developing and implementing improvements. An essential starting point is systematic and objective assessment of performance and of the systems supporting good performance.7 Good quality information is needed, so that goals can be set and strategies developed for improving key areas. An emphasis on participation by the people being studied, and flexibility in the approach, makes modern CQI very similar to action research, both being characterised by “cyclical activities involving examination of existing processes, change, monitoring the apparent effects of the change and further change”.8
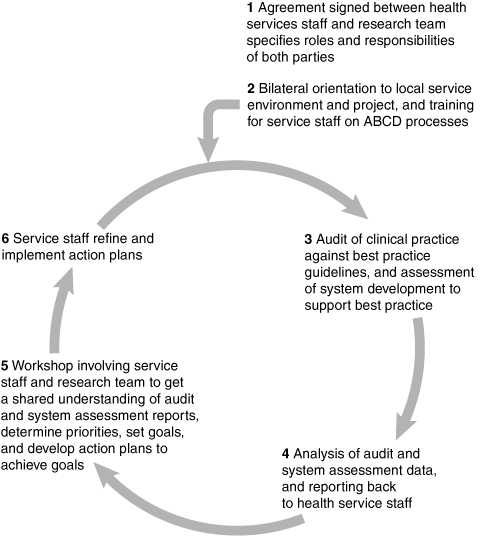
Features of the ABCD CQI approach (Box 1) include:
Assessing clinical performance across the scope of best-practice services for chronic illness care rather than selected (“indicator”) services. This is done by auditing records of service delivery and clinical and laboratory findings in a sample of patient records. For example, the diabetes audit covers over 20 services specified in widely accepted best-practice guidelines, and the preventive services audit covers about 10 services specified in guidelines for preventive care for a generally well adult (eg, the 2-yearly Adult Health Check for Aboriginal and Torres Strait Islander people).9,10
Structured assessment of health centre systems to support best practice. This is based on the Assessment of Chronic Illness Care scale,10,11 which analyses the status of key aspects of primary care service systems (eg, design of work flow and staff roles and responsibilities; arrangements for working with other agencies and community members; information systems; systems to support clinical best practice (including the availability of guidelines and access to specialist advice).
Emphasising participation in all aspects of the approach. The ABCD approach is guided by widely accepted principles of community-based research, which stress the importance of partnerships (Box 2).12
Trends over two ABCD CQI cycles to date have shown improvements in primary care systems (eg, business plans specifying roles, responsibilities and goals for diabetes care); in adherence to best-practice clinical guidelines (eg, an increased proportion of people with diabetes having regular testing of glycated haemoglobin [HbA1c] levels); and in intermediate health outcomes (eg, normalisation of HbA1c levels).13
Evidence of the effectiveness of modern CQI approaches in the manufacturing,14,15 service16 and health care17,18 industries abound. The most substantial experience of CQI is in the manufacturing and business sectors, and research in these areas highlights leadership, people management and customer focus as components of CQI interventions that strongly predict performance.19 People management appears to be particularly important in the service sector,17 including a commitment to increasing employees’ knowledge of, and empowerment to engage in, CQI processes.15,16 The intensity of interventions has been shown to explain a significant proportion of the variation in performance,16 with greater benefit likely if interventions are implemented as designed.17 Furthermore, international comparisons suggest a degree of culture specificity in what works where.15
In the clinical context, research suggests CQI approaches are most effective when they focus on organisational priorities; there is good engagement of high-level managers; the intervention is clearly formulated; the organisation is ready for change; there is a relationship of trust with practitioners; there is revision of professional roles; there are adequate information systems; and the external environment is supportive.19,20
The strength of the evidence of the effectiveness of CQI is limited by the quality of research study designs, the extent to which confounders are measured and controlled for in data analysis, and the heterogeneous nature and varying intensity of CQI interventions.20 However, the CQI concept has intuitive appeal. Proponents of CQI believe that while the language may change, the tools and vision of CQI will persist because they are adaptive.18 It is this positive view of the promise of CQI that is perhaps most supportive of the call for leading international and national health agencies to implement integrated CQI processes in clinical practice.1
Key features of modern CQI approaches make them well suited to the Indigenous Australian setting and to the principles of Indigenous research and service delivery. The participatory approach and the customer focus of CQI, and the combination of scientific and humanistic professional values,15,16,19 adhere to the principles and values of Aboriginal and Torres Strait Islander peoples, as expressed in recent national statements on research21,22 and cultural respect.23 In these same statements, the emphasis given to tackling underlying causes (eg, human resource capacity and social conditions, including unemployment), to capacity building (including, specifically, community capacity to understand and use data), and to improving outcomes is also central to CQI,18,19 as is the development of positive models and a culture of self-evaluation rather than blame.1 CQI also provides a structure to refine and re-invigorate programs to promote sustainability.13
Early evidence of the acceptability of CQI approaches and their impact on Indigenous primary care services is emerging from our recent and ongoing research.10,13 Comments by stakeholders reinforce our perceptions (Box 3).
2 Principles of community-based research guiding the ABCD research project12
Recognise each participating health service team as a distinct unit with common interests and needs.
Build on strengths and resources within the health team and the community. These may include skills and assets of individuals, networks of positive relationships and social structures, and processes that contribute to the ability of the health team and community to work together to improve health.
Facilitate collaborative partnerships in all phases of research. Our goal is for all parties to participate equally in the research process.
Integrate knowledge and action for mutual benefit of all partners. We aim to build a body of knowledge that can be integrated with local health team and community efforts to address their issues of concern.
Promote a co-learning and empowering process that attends to social inequalities. We place an emphasis on reciprocal transfer of knowledge, skills, capacity and power. For example, the research team gains a deeper understanding of the context and challenges of the local health service, and the health team gains skills in collecting, analysing and acting on data collected.
Use a cyclical/iterative process. This includes partnership development and the ongoing refinement of the cycle outlined in Box 1.
Address health issues from positive and ecological perspectives. We emphasise achievements in service delivery and health outcomes, and encourage consideration of biomedical, social, cultural and political factors as determinants of health and disease.
Disseminate findings and knowledge gained to all partners. We aim to share research findings in language that is understandable and in a way that respects all contributions to the process and informs action to improve health.
- Ross S Bailie1
- Damin Si2
- Lyn O'Donoghue3
- Michelle Dowden4
- Menzies School of Health Research, Charles Darwin University, Darwin, NT.
We thank Gwenda Gless, Peter Wordsworth and Tarun Weeramanthri for providing comments from health professionals. Ross Bailie’s research is funded by a National Health and Medical Research Council Fellowship grant (#283303). The ABCD project is funded by the Australian Health Ministers’ Advisory Council and by the Cooperative Research Centre for Aboriginal Health.
None identified.
- 1. Siddiqi K, Newell JN. Putting evidence into practice in low-resource settings. Bull World Health Organ 2005; 83: 882.
- 2. Commonwealth Department of Health and Ageing. Healthy for Life. http://www.health.gov.au/healthyforlife (accessed Mar 2007).
- 3. Graham N. Quality in health care: theory, application and evolution. Gaithersburg, Md: Aspen Publishers, 1995.
- 4. Clark GB, Sarewitz S, Aziz K, et al. Continuous quality improvement: essential management approaches. Approved guideline GP-22A. Wayne, Pa: National Committee for Clinical Laboratory Standards, 1999.
- 5. Duggan JM. Quality in healthcare in the United Kingdom: lessons for Australia. Med J Aust 1999; 170: 121-124.
- 6. Berwick DM. Continuous improvement as an ideal in health care. N Engl J Med 1989; 320: 53-56.
- 7. McLaughlin CP, Kaluzny AD, editors. Continuous quality improvement in health care: theory, implementation, and applications. Gaithersburg, Md: Aspen Publishers, 1994.
- 8. Lilford R, Warren R, Braunholtz D. Action research: a way of researching or a way of managing? J Health Serv Res Policy 2003; 8: 100-104.
- 9. Central Australian Rural Practitioner Association. CARPA standard treatment manual: a clinic manual for primary health care practitioners in remote and rural communities in Central and Northern Australia. 4th ed. Alice Springs, NT: CARPA, 2003.
- 10. Si D, Bailie R, Connors C, et al. Assessing health centre systems for guiding improvement in diabetes care. BMC Health Serv Res 2005; 5: 56.
- 11. Bonomi AE, Wagner EH, Glasgow RE, VonKorff M. Assessment of chronic illness care (ACIC): a practical tool to measure quality improvement. Health Serv Res 2002; 37: 791-820.
- 12. Israel BA, Schulz AJ, Parker EA, Becker AB. Review of community-based research: assessing partnership approaches to improve public health. Annu Rev Public Health 1998; 19: 173-202.
- 13. Bailie R, Si D, Dowden M, Lonergan K. Audit and best practice for chronic disease: project final report. Darwin: Menzies School of Health Research, 2007.
- 14. Adam EE, Corbett LM, Flores BE, et al. An international study of quality improvement approach and firm performance. Int J Oper Prod Manag 1997; 17: 842-873.
- 15. Samson D, Terziovski M. The relationship between total quality management practices and operational performance. J Oper Manage 1999; 17: 393-409.
- 16. Prajogo DI. The comparative analysis of TQM practices and quality performance between manufacturing and service firms. Int J Serv Ind Manag 2006; 16: 217-228.
- 17. Blumenthal D, Kilo CM. A report card on continuous quality improvement. Milbank Q 1998; 76: 625-648, 511.
- 18. Shortell SM, Bennett CL, Byck GR. Assessing the impact of continuous quality improvement on clinical practice: what it will take to accelerate progress. Milbank Q 1998; 76: 593-624, 510.
- 19. Wensing M, Wollersheim H, Grol R. Organizational interventions to implement improvements in patient care: a structured review of reviews. Implement Sci 2006; 1: 2.
- 20. Shojania KG, Grimshaw JM. Evidence-based quality improvement: the state of the science. Health Aff (Millwood) 2005; 24: 138-150.
- 21. National Health and Medical Research Council. The NHMRC road map: a strategic framework for improving ATSI health through research. http://www.nhmrc.gov.au/publications/synopses/_files/r28.pdf (accessed Apr 2007).
- 22. National Health and Medical Research Council. Values and ethics: guidelines for ethical conduct in Aboriginal and Torres Strait Islander health research. Canberra: NHMRC, 2003: 1-24. http://www.nhmrc.gov.au/ethics/human/conduct/guidelines/_files/e52.pdf (accessed Apr 2007).
- 23. Australian Health Ministers’ Advisory Council Standing Committee on Aboriginal and Torres Strait Islander Health Working Party. Cultural respect framework for Aboriginal and Torres Strait Islander Health, 2004-2009. Adelaide: Department of Health South Australia, 2004. http://www.health.gov.au/internet/wcms/publishing.nsf/Content/health-oatsih-pubs-crf.htm/$FILE/Cultural_Respect_Framework.pdf (accessed Apr 2007).





Abstract
The Australian government’s Healthy for Life program is supporting capacity development in Indigenous primary care using continuous quality improvement (CQI) techniques.
An important influence on the Healthy for Life program has been the ABCD research project. The key features contributing to the success of the project are described. The ABCD research project:
uses a CQI approach, with an ongoing cycle of gathering data on how well organisational systems are functioning, and developing and then implementing improvements;
is guided by widely accepted principles of community-based research, which emphasise participation; and
adheres to the principles and values of Indigenous health research and service delivery.
The potential for improving health outcomes in Aboriginal and Torres Strait Islander communities using a CQI approach should be strengthened by clear clinical and managerial leadership, supporting service organisations at the community level, and applying participatory-action principles.