In response to the growing evidence-base supporting primary health care . . . a number of countries have embarked on significant primary health care reforms . . . challenges being experienced are:
an increased proportion of gross domestic product (GDP) spending on health and inappropriate use of hospital services for ambulatory care sensitive conditions;
the ageing of populations and an increasing burden of chronic disease . . . ;
problems with inequitable access to primary care services . . . ; and
a lack of integration of primary care services with other parts of the health system . . .1
We describe the approaches piloted by academic practices of the University of Newcastle (Box 1) and University of Queensland (Box 2) in taking up the challenges identified in that review. These approaches meet the review’s challenges to the “new” primary care1 in the ways described below.
Cessnock Uni-Clinic provides the clinical environment to develop extended roles for women’s health nurses, practice/triage nurses, dietitians, mental health and drug and alcohol nurses, and other non-medical primary health care providers. The New South Wales Health Integrated Primary Health Care and Community Services Program (IPHCCSP; http://www.health.nsw.gov.au/pubs/2005/integrated_phcc_eoi.pdf) sees Cessnock as a lead site and integration is now proceeding well.
Inala Primary Care uses the Australian Government Department of Health and Ageing’s “Lifescripts” lifestyle intervention11 and a motivational counselling approach with its GPs and practice nurses. It also actively identifies those at risk of lifestyle-related illness for group, individual or family sessions with the Inala Chronic Disease Management Service team or the community health service.
Cessnock Uni-Clinic has created a thriving general practice presence in a health service void. The Inala approach has allowed a chronically understaffed outer urban general practice to reach full staffing potential in 2007. The reorientation of triage and chronic disease management services around a model of partnered clinical management between doctors and nurses has encouraged and invigorated all clinicians to focus on an accessible, evidence-based care model. These successes reinforce the experience of programs such as More Allied Health Services (MAHS), which have demonstrated an ability to attract health care workers to difficult areas by offering role flexibility and innovative models of practice.12
Exemplars of innovative practice are possible only where local vision, leadership, and clinician and community commitment allow them to gestate and grow.13 The historical “disconnect” between general practice, acute care and community health services results in a fragmented, inefficient system that serves patients poorly. Redressing this arrangement requires political will and leadership, clear organisational roles and responsibilities, a commitment to services orientated around community need, and local integrated governance arrangements.13
The difficulties stemming from Australia’s system of health care funding and delivery being divided among federal and state governments are much reported.14,15 A number of settings have now been able to overcome these challenges16 and many more could follow suit with the cultural changes described above.
Effective evaluation of change in practice across community and hospital sectors, and the impact of such change on both consumers and the health care system, is sadly lacking in Australia. Queensland Health has recently moved to redress this, with one of the criteria for the multimillion-dollar state innovation grants being the requirement to have methods robust enough for publication.17 Academic departments should be strong partners in such projects.
Clinicians and communities are thirsty for better coordinated and more easily accessible care.14 Creating incentives — clinical, organisational, and business-related — that encourage efficient integrated approaches to patients and communities would be an excellent start. General practice sees nearly 90% of the Australian community each year;18 no other setting or service group can achieve this level of contact. Better use of general practice as the “hub” for other community and acute care “spokes” would allow more efficient use of scarce resources in both the public and private health sectors. The broadening team of health care workers in many practices now allows a much broader scope of preventive and comprehensive care in general practice than has been previously possible.
a focus on important community health needs;
matching service style to the available workforce, the broader health environment and an evidence basis for effective care;
carefully managing the change process with practice personnel and local stakeholders;
taking time to choose the right clinical model of care, communication infrastructure, professional training, and governance arrangements to make the innovation a sustained reality;
measuring and reviewing progress and deliverables regularly; and
being bold, well researched and relevant to the local communities.

1 University of Newcastle approach: Cessnock Uni-Clinic
Cessnock has some of the worst health and socioeconomic indicators in Australia.2 The rate of diabetes in Cessnock is among the highest in New South Wales.3 It has the highest premature rate of death from heart disease in NSW and nationally, as well as very high rates of mental health, drug and alcohol problems, teenage pregnancies and single parenthood.3 Unemployment rates are higher than the state average, with a rate for 15–19-year-old males of 29.8%.4 In 2004, Cessnock had around one general practitioner per 2850 population, and an ongoing reduction over 30 years in the number of GPs had created major local problems with access to care.
provided over 66 460 medical services in 43 222 patient visits;
commenced comprehensive care for over 200 patients with diabetes;
identified and managed 290 patients with asthma;
conducted comprehensive health care plans for more than 521 citizens aged over 75 years;
provided 139 dietitian services;
completed more than 1357 cervical cancer Pap smears;
provided 111 clinical placements for University of Newcastle medical, nursing and dietetics students;
a full-time equivalent staff of two GPs (who also provide weekend and night cover through the hospital), two general practice registrars, 2.1 advanced practice nurses, one triage nurse, one women’s health nurse, 0.6 midwives, one dietitian, one operations director, one administration manager and 3.8 receptionists.
All staff are salaried. The clinic receives no subsidies.
We see Cessnock as a health care delivery laboratory and have made every detail of its operation widely available. It has drawn widespread approbation from the community, health care professionals, federal and state governments, and at conferences.5,6 The question we set out to answer has been answered successfully. By using GPs as team leaders, reserving their high-order skills for where they are truly needed, we have demonstrated a viable and sustainable model of care for areas that find it difficult to recruit health care professionals and deliver health care.

2 University of Queensland approach: Inala Primary Care
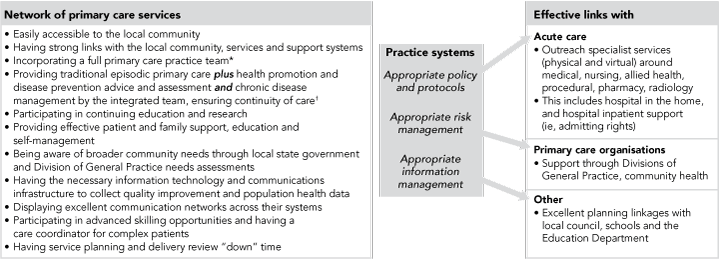
In 2003, the University of Queensland (UQ) became involved in an integrated service delivery initiative — the Brisbane South Centre for Health Service Integration (BSCHSI) — involving Queensland Health (QH), the Brisbane Inner South Division of General Practice and Mater Health Services, Brisbane. This involved a collocation of key personnel from each organisation, supported by a validated set of integration strategies designed to develop a unified health care culture.7-9 This approach highlighted important challenges for general practice in building on the success of the initiative, and in 2005, the BSCHSI partners supported an expanded framework for general practice to further develop its capacity to support local communities. The Brisbane South Comprehensive Primary Care Network Model10 identified the characteristics of an integrated general practice/primary care network able to respond to the challenges and opportunities ahead in the Australian health care system (Figure). The model was deliverable through private general practice or through a standalone community health/general practice setting.
Brisbane South Comprehensive Primary Care Network Model
- Claire L Jackson1
- John E Marley2,3
- 1 University of Queensland, Brisbane, QLD.
- 2 University of Newcastle, Newcastle, NSW.
- 3 University of Adelaide, Adelaide, SA.
John Marley is a Director of Hunter Uni-Clinics, the trustee for the Cessnock Uni-Clinic. Claire Jackson is a board member of Inala Primary Care.
- 1. McDonald J, Cumming J, Harris M, et al. Systematic review of comprehensive primary health care models. Australian Primary Health Care Research Institute. Sydney: Research Centre For Primary Health Care and Equity, University of New South Wales, Sep 2006. http://www.anu.edu.au/aphcri/Domain/PHCModels/Final_25_McDonald.pdf (accessed Jun 2007).
- 2. Hunter Valley Research Foundation. Hunter region facts. Population and demography. http://www.hvrf.com.au/pages/design/links/uploaded/Yearbook_Population_000.pdf (accessed Jun 2007).
- 3. Hunter Public Health Unit. State of health in the Hunter report. Newcastle: Hunter Area Health Service, 2003. http://www.hunter.health.nsw.gov.au/hph/soh/soh_complete.pdf (accessed Jun 2007).
- 4. Cessnock City Council. Cessnock LGA at a glance — population and census statistics. http://www.cessnock.nsw.gov.au/Cessnock/index.asp?id=40 (accessed Jun 2007).
- 5. Marley J. Maximising doctor input using other professions. Practice made perfect? The sequel. NSW Rural Doctors Network Conference; May 2006; Sydney. http://www.nswrdn.com.au/client_images/246159.pdf (accessed Jun 2007).
- 6. Marley J. Tomorrow’s teams. Rural Doctor’s Association of South Australia Annual Conference; Nov 2006; Adelaide. http://www.rdasa.com.au/conference/documents/JohnMarley-CessnockUni-ClinicModel.pdf (accessed Jun 2007).
- 7. Jackson C, Nicholson C, Kardash C, et al. Creating an integrated vision by co-locating health organisations — herding cats or a meeting of minds? Aust Health Rev 2007; 31: 256-266.
- 8. Nicholson C, Jackson C, Wright B, et al. Online referral and OPD booking from the GP desktop. Aust Health Rev 2006; 30: 397-404.
- 9. Jackson C, Nicholson C, Davison B, McGuire T. Training the primary care team — a successful interprofessional education initiative? Aust Fam Physician 2006; 35: 829-832.
- 10. Jackson C. Working from the ground up. 2005 National Health Care Reform Conference; Sep 2005; Adelaide. http://www.archi.net.au/events/26/reform05/ground_up (accessed Jun 2007).
- 11. Australian Government Department of Health and Ageing. Lifescripts. http://www.health.gov.au/internet/wcms/publishing.nsf/Content/health-pubhlth-strateg-lifescripts-index.htm (accessed Jun 2007).
- 12. Australian Government Department of Health and Ageing. More allied health services (MAHS) program. http://www.health.gov.au/internet/wcms/publishing.nsf/content/health-pcd-programs-mahs (accessed Jun 2007).
- 13. Jackson CL, Nicholson C, Doust J, et al. Integration, coordination and multidisciplinary care in Australia: growth via optimal governance arrangements. Australian Primary Health Care Research Institute. Brisbane: University of Queensland, Sep 2006. http://www.anu.edu.au/aphcri/Domain/MultidisciplinaryTeams/Final_1_Jackson.pdf (accessed Jun 2007).
- 14. Van Der Weyden MB, Armstrong RM. Evidence and Australian health policy [editorial]. Med J Aust 2004; 180: 607-608. <MJA full text>
- 15. Menadue J. Healthcare reform: possible ways forward. Med J Aust 2003; 179: 367-369. <MJA full text>
- 16. Advanced Community Care Association [website]. http://www.accasa.org.au/ (accessed Jun 2007).
- 17. Queensland Government. Queensland Health. Clinical Practice Improvement Centre. Clinical networks implementation guide. http://www.health.qld.gov.au/cpic/documents/Networks_Implement.pdf (accessed Jun 2007).
- 18. Royal Australian College of General Practitioners. Guidelines for preventive activities in general practice (the red book). 6th ed. Melbourne: RACGP, Sep 2005: vii. http://www.racgp.org.au/guidelines/redbook (accessed Jun 2007).





Abstract
An innovative team approach and integration of care across sectors, including general practices, community health services, allied health professionals and hospitals, can deliver high-quality comprehensive care in disadvantaged areas while providing teaching and research opportunities and community service.
Academic general practice departments are committed to supporting and evaluating such models.
A governance infrastructure that encourages strong partnerships across health care sectors is essential.
With broad health partnership support, bulk-billing is viable in an Australian general practice team model providing health care to the disadvantaged.