Practice nurses are now employed in nearly 60% of Australia’s general practices, and are being allocated an increasing number of items in the Medicare Benefits Schedule.1 In addition, substantial financial support is provided for general practices to employ practice nurses, who are seen as a strategy to address primary-care workforce shortages. However, there is a policy vacuum around developments in practice nursing. Here, we raise issues that will affect the sustainability of the practice-nurse workforce if not addressed more systematically.
In the United Kingdom, Canada and the United States, considerable literature provides evidence about the roles and outcomes of practice nursing, demonstrating the value of practice nurses to primary care delivery.2 Australian studies of the practice-nurse workforce are largely exploratory and descriptive, with little evidence cited about models of practice or outcomes.3
Amid perceived threats to clinical practice and funding,1 some general practitioners appear ambivalent about practice nursing. The nursing profession in Australia has also displayed ambivalence about the developments in practice nursing, somewhat reluctantly accepting that practice nursing is now established as a field of practice in the primary-care sector. Perhaps these politics have undermined progress on workforce data collection, funding models, educational opportunities and career pathways, which is well developed for other health professions. Nonetheless, the size of the practice-nurse workforce and levels of health system activity generated by these nurses warrant much closer attention. To keep pace with other developed countries, we need to strengthen policy and evidence frameworks for practice nursing in Australia, so as to support quality outcomes and a better understanding of the contributions of practice nurses to the health system.
Australia has well established and comprehensive sources of information for the medical workforce.4 Yet, despite the acknowledged importance of health workforce data collections, data on the practice-nurse workforce are as yet insufficient for the development of effective policy and planning.5 A forthcoming data source will be the annual nursing labour force survey which, from 2006, has included practice nurses.
Data about the activity of practice nurses are also insufficient. General practice data collections focus largely on GPs and give only a partial picture of the roles and functions of practice nurses. Medicare statistics show that 3.4 million practice-nurse Medicare item numbers were claimed in 2006, representing 3.2% of all Medicare items for general practice (see Box 1).6 The 2006 BEACH (Bettering the Evaluation and Care of Health) report indicated that practice-nurse activity was recorded in 3.9% of GP–patient encounters in 2006.7 However, these figures seriously underestimate the contribution of practice nurses to the delivery of primary health care, because they are centred on the activity of the GP. They do not take account of activities such as contributions to other Medicare items (eg, Health Assessments, Practice Incentive Payments [PIPs] and GP Management Plans); services not claimed on Medicare; and other functions of practice nurses, such as clinical organisation, practice administration, and integration.8 Preliminary data from a new national study of practice-nurse activity indicate that only 39% of practice-nurse consultations were eligible for a Medicare rebate.9
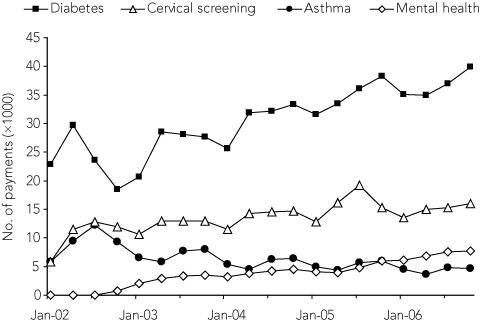
Medicare Benefits Schedule item numbers have been introduced for practice nursing without cost–benefit analysis or a sound evidence framework about how they might optimise population health outcomes. Data collections for PIPs take into account the work undertaken by nurses that attract PIP to general practices without directly attributing this work to them. Some PIPs are provided over and above fee-for-service payments to the practice, for management of clinical conditions such as asthma, diabetes, cervical screening and mental health. However, while PIP payments have been increasing (see Box 2),10 there are no data on who performs the clinical work that attracts these payments. As the delivery of primary care changes to include a range of health professions within the general practice context, data collections of primary care activity must also change to capture the full range of service providers, to inform economic analysis of activity and more accurately attribute contributions by different professionals.
The most suitable model of practice for practice nurses has not been debated. Consequently, the strengths and weaknesses of different models — often framed as either the substitution or collaborative model — are not well understood. The substitution model conceptualises the role of practice nurses as primarily delegated, assuming that the nurse undertakes a delegated subset of a GP’s tasks and functions, with no scope of practice outside this subset. This view is implicit in the Australian Government’s Nursing in General Practice Initiative, which is to “relieve workforce pressure in general practice”.11 In contrast, a collaborative practice model assumes that the practice nurse is an autonomous provider — an independent professional with the ability to effectively manage an episode of patient care. This is reflected in the new Chronic Disease Management items, which indicate that a practice nurse can (under certain circumstances) act autonomously, while also being a member of a multidisciplinary team in a Team Care Arrangement.12 Collaborative professional autonomous models are also supported by the competency standards for nurses in general practice, whereby nurses take personal responsibility for their own competence and adherence to professional nursing standards.13
The evidence suggests a wide variation in practice-nurse roles, ranging from traditional delegation of tasks and assistance to doctors, through to advanced, independent practice in areas such as preventive care, disease management and care coordination.3,8,14 Contextual factors that shape models of practice include the professional characteristics of the nurse, the business orientation of the practice, and the needs of the local population.3 Systematic investigation is now required to provide evidence about which models work most effectively for better health outcomes in the context of satisfaction for practice nurses and GPs.
Other professional issues that remain unresolved in the development of the practice-nurse workforce include supervision, professional indemnity, funding arrangements, education and training, and the lack of a systematic approach to policy development and evaluation. Registration boards require a nurse’s primary supervisor to also be a nurse — supervision by GPs is not sufficient. Systems for management of this responsibility are yet to be established. There is also concern that the relative professional isolation of practice nurses creates a vulnerability to pressure to perform tasks beyond the recognised scope of practice.15
Watts et al found that education for practice nurses is not adequate to meet the demands of their current or future roles.8 Indeed, there is no comprehensive framework for the education of practice nurses. Although the Australian Government has offered scholarships for education in some clinical areas through the Nursing in General Practice Training and Support Initiative: 2005–09, these scholarships have not been tied to a quality audit of the programs of study. Seventy-three per cent of nurses working in general practice in Australia are aged over 40 years,1 and are likely to have come from the hospital setting, with little training or experience in primary care. A strategy is needed to provide education and training pathways to support nurses to gain levels of expertise (basic to advanced) based on knowledge, skill and competencies. These pathways would allow practice nurses to advance through a career framework, as has been developed in the UK and New Zealand.8
A strengthened practice-nurse workforce has the potential to drive change and improve the delivery of many aspects of primary care, as well as to relieve workload pressures on GPs, but there are challenges in establishing an effective and sustainable practice-nurse workforce. For the work of practice nurses to be seen as contributing to the larger primary care national agenda, high-quality data collections are needed that will permit analysis of their actual practice, the quality of care they provide, and its outcomes. In addition, practice nurses need a quality education and career framework that will attract those seeking an alternative to hospital careers. Policy development in primary care has been reactive to the needs of general practice and workforce shortages, without a genuine understanding of, or commitment to, professional support for the practice-nurse workforce. Box 3 shows specific suggestions for a more proactive and evidence-based approach to developing primary care nursing policy and practice.
3 Recommendations for future development of policy on practice nurses
Tracking of the practice-nurse workforce.
Collection of data on primary care activity by provider type, linked to health outcomes and quality of care.
Framework for an education and career pathway for practice nurses.
Development of guidelines for practice nurse supervision.
Clear guidelines about professional-indemnity requirements for practice nurses.
Nationally consistent standards for the development of the practice-nurse role.
An evidence-based approach to the development of policies related to practice nursing.
- Helen Keleher1
- Catherine M Joyce2
- Rhian Parker3
- Leon Piterman4
- School of Primary Health Care, Monash University, Melbourne, VIC.
None identified.
- 1. Australian Divisions of General Practice. National Practice Nurse Workforce Survey. Canberra: ADGP, 2006.
- 2. Horrocks S, Anderson E, Salisbury C. Systematic review of whether nurse practitioners working in primary care can provide equal care to doctors. BMJ 2002; 324: 819-823.
- 3. Halcomb EJ, Patterson E, Davidson PM. Evolution of practice nursing in Australia. J Adv Nurs 2006; 55: 376-390.
- 4. Productivity Commission. Australia’s health workforce. Research report. Canberra: Productivity Commission, 2005.
- 5. Australian Health Ministers Conference. National Health Workforce Strategic Framework. Sydney: AHMC, 2004.
- 6. Medicare Australia. Medicare statistics. http://www.medicare.gov.au/providers/health_statistics/statistical_reporting/medicare.shtml (accessed Apr 2007).
- 7. Australian Institute of Health and Welfare. General practice activity in Australia 2005–2006. Canberra: AIHW, 2007. (AIHW Cat. No. GEP 19.)
- 8. Watts I, Foley L, Hutchinson R, et al. General practice nursing in Australia. Melbourne and Canberra: Royal Australian College of General Practitioners and Royal College of Nursing, Australia, 2004.
- 9. Joyce C, Piterman L. The Practice Nurse Work Survey: nurses working together with general practitioners. Presentation at the General Practice and Primary Health Care Research Conference, Sydney, May 2007.
- 10. Medicare Australia. General practice statistics reports. http://www.medicareaustralia.gov.au/statistics/imd/forms/gpStatistics.shtml (accessed May 2007).
- 11. Australian Government Department of Health and Ageing. Guidelines for the Divisions Network Nursing in General Practice program. Canberra: Commonwealth of Australia, 2006.
- 12. Australian Government Department of Health and Ageing. Chronic disease management (CDM) Medicare items. Q & As. Updated with 1 November 2006 MBS fees. Canberra: Commonwealth of Australia, 2006. http://www.health.gov.au/internet/wcms/publishing.nsf/Content/pcd-programs-epc-chronicdisease (accessed Apr 2007).
- 13. Australian Nursing Federation. Competency standards for nurses in general practice. Canberra: ANF, 2006. http://www.anf.org.au/nurses_gp/ (accessed Apr 2007).
- 14. Healthcare Management Advisors. Evaluation of the 2001 nursing in general practice initiative. Canberra: Australian Government Department of Health and Ageing, 2005. http://www.health.gov.au/internet/wcms/publishing.nsf/Content/pcd-nursing-eval (accessed May 2007).
- 15. Halcomb EJ, Davidson PM, Daly JP, et al. Nursing in Australian general practice: directions and perspectives. Aust Health Rev 2005; 29: 156-166.





Abstract
Almost 60% of general practices now employ at least one practice nurse.
Australian Government initiatives to support the expansion of practice nursing are not consistently based on strong evidence about effectiveness, outcomes or efficiencies.
Reviews from other countries suggest that practice nurses can achieve good health outcomes, but there is little information about the Australian practice-nurse workforce, funding models to support their work, scope of their practice, or its outcomes.
Australian practice nursing lacks a career structure and an education framework to advance nurses’ skills and knowledge.
To maximise the contribution of nurses in primary care, a more systematic approach is needed, with a stronger evidence base for policy to support effective outcomes.