Changes have been made to the aged-care system over the past decade to help older people stay in their own homes for longer, with the introduction of various programs such as the Home and Community Care Program1 and the Extended Aged Care at Home package.2 However, the number of people in residential aged care has continued to rise.3
In 2005, there were 151 910 people living in residential aged-care facilities (RACFs) in Australia.3 RACFs have previously been known as hostels or nursing homes. They provide high-level medical and residential care to people who are unable to live in the community because of illness and disability, particularly older people.3
Published data reveal that the GP workforce attending RACFs has changed over the past two decades.4 GPs who attend RACFs are more likely to be older4,5 and more likely to be male4 than GPs who do not. According to the Bettering the Evaluation and Care of Health (BEACH) study of general practice, in 2005–06, 46.1% of GPs reported attending an RACF in the 4 weeks before participation in the study.6
For the period April 2004 to March 2006, we conducted a secondary analysis of data from the BEACH study, a continuous national study of general practice activity. The methods, the reliability and validity of these methods, and the representativeness of the sample have been discussed in detail elsewhere.6,7 Briefly, each year we approach GPs randomly selected by the Department of Health and Ageing from Medicare data. Typically, about 1000 GPs (about 30% of those approached) agree to participate. Each GP records details for 100 consecutive patient encounters, the combined results building an annual database of about 100 000 encounters. Compared with all GPs in the sample frame, younger GPs (< 35 years) were under-represented in our final sample. We corrected for this by post-stratification weighting. The final weighted dataset demonstrated high precision for the age–sex distribution of patients at encounter compared with that for all Group A1 (general practice) MBS-claimed items of service.6
Our study compares the content of encounters at which the GP recorded an MBS item number for attendance at an RACF with all BEACH encounters recorded during the same period. Morbidity was classified according to the International Classification of Primary Care, 2nd edition (ICPC-2).8 Pathology and imaging tests and clinical and procedural treatments were coded using ICPC-2 PLUS,9 a more specific interface terminology classified according to ICPC-2. Results are reported as a proportion of encounters or a rate per 100 encounters, with 95% confidence intervals, adjusted for the cluster study design. For comparisons between groups, non-overlapping confidence intervals indicate statistically significant differences at the 0.05 level.
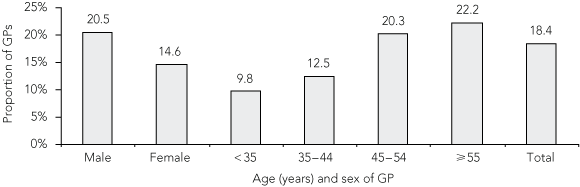
During the study period, 1970 GPs recorded details of 197 000 encounters, 2310 (1.2%) of which were claimable under the MBS as items relating to RACF consultations. There were 360 GPs (18.4% of participants) who recorded at least one RACF consultation. The likelihood of recording at least one RACF consultation increased with the age of the GP: those aged ≥ 45 years were more likely to have recorded an RACF consultation than those aged < 45 years. GPs attending RACF consultations were more likely to be male than female (Box 1).
There were no significant differences in the number of reasons for encounter or number of problems managed between RACF consultations and all BEACH encounters, but there were significantly more chronic problems managed at RACF consultations. Recording of non-prescribed medications (both advised over-the-counter medications and GP-supplied medications) was significantly lower for RACF patients than for all patients. However, there was no difference in the rate of prescribed medications recorded (Box 2).
At RACF encounters there were significantly fewer non-pharmacological treatments (including both clinical and procedural treatments); referrals (to specialists and, marginally, to allied health providers); and pathology and imaging tests ordered (Box 2).
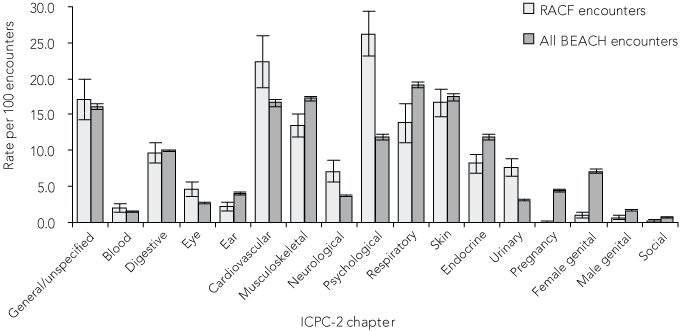
The most frequently managed problems at RACF consultations included psychological problems (particularly dementia/Alzheimer’s disease [managed at 33 times the usual rate] and schizophrenia) and circulatory problems (particularly stroke, heart failure and atrial fibrillation/flutter) (Box 3, Box 4). While hypertension was the second most frequently managed problem at RACF consultations, it was managed significantly less often (5.9 per 100 encounters; 95% CI, 4.7–7.2) than at all BEACH encounters (9.1 per 100 encounters; 95% CI, 8.8–9.4) (results not tabled).
Other problems managed more often at RACF consultations included neurological problems (reflected in the higher management rates of Parkinson’s disease and epilepsy); urological problems (specifically urinary tract infections); and problems relating to the eye (particularly conjunctivitis). Most musculoskeletal problems recorded in RACF consultations involved management of osteoarthritis and fractures (Box 3, Box 4).
At RACF consultations, administrative procedures, chronic skin ulcers and constipation were also managed significantly more often (Box 4). It is notable that there was no difference in the management rate of depression for RACF encounters and all BEACH encounters (3.3 per 100 encounters [95% CI, 2.5–4.1] v 4.0 per 100 encounters [95% CI, 3.8–4.1], respectively) (results not tabled).
Dementia is the problem most frequently managed by GPs in RACFs in Australia, at a rate much higher than in everyday general practice. It has been estimated that, in 2006, 190 000 Australians had diagnosed dementia.10 Recent data suggest that between 380 30011 and 465 00010 Australians will have dementia by 2030–31. It is estimated that up to half of the residents in RACFs have dementia, the majority requiring high-level care.10 It therefore has an enormous impact on the workload of GPs in this setting.
Some of the chronic diseases managed by GPs in RACFs are associated with profound or severe activity restriction in older people.12 Projections indicate an increase of about 70% in older people with profound disability by the year 2031.13
Other chronic conditions with high relative management rates included epilepsy, schizophrenia and Parkinsonism. Each of these conditions is linked with functional decline in older people, which may explain their higher management rates in RACFs, where both their physical and medical needs can be met.14-16
The number of problems managed at RACF consultations did not differ from the average for all BEACH encounters (1.5 per consultation). Given the reported high management rates of chronic disease, we expected this rate might be higher. However, in the RACF setting, the GP is working as part of a multidisciplinary team, and it is possible that some aspects of patient care are dealt with by other team members, reducing the number of problems managed by the GP. Another hypothesis relates to claim rates on MBS general practice items, with the highest rates occurring in people aged ≥ 75 years or more (a mean of 10.0 attendances per year, compared with an overall mean of 4.9 attendances per year).17 High attendance rates may have an impact on the number of problems managed per encounter: GPs may treat the same number of problems during a single consultation, but may see the patient more often. Multiplying the average number of attendances by the number of problems managed per consultation would increase the total number of problem contacts with an RACF patient.
We identified low referral rates at RACF consultations, particularly to specialists (but also, marginally, to allied health professionals). Given that the MBS has offered rebates for GP involvement in multidisciplinary care for older patients in RACFs in recent years, such as multidisciplinary care plans,18 low referral rates may reflect difficulties involved in getting such patients to specialist services. In the case of allied health providers, it may also indicate the availability of on-site services such as physiotherapy.
The differences identified in our study reflect the challenges that GPs face when working in RACFs and point to areas in which additional support may be needed. It has been stated that the increasing number of GPs with specialised interest areas may have a negative impact on the number of GPs willing to attend RACFs.19 However, perhaps residential aged care is a form of specialisation in itself. Acknowledging that residential aged care differs from everyday practice for GPs and providing education and resources where needed may help to redress current workforce shortages in aged care. The recently announced increase in MBS remuneration for RACF attendances may also encourage more GPs to manage patients in this setting.20
1 Age- and sex-specific proportion of GPs attending RACFs
 | |||||||||||||||
|
GP = general practitioner. RACF = residential aged-care facility. | |||||||||||||||
2 Comparison of RACF encounters with all BEACH study encounters, expressed as rate per 100 encounters (95% CIs)
3 Comparison of problems managed in RACFs with all BEACH study encounters, by ICPC-2 chapter
 | |||||||||||||||
|
BEACH = Bettering the Evaluation and Care of Health. ICPC-2 = International Classification of Primary Care, 2nd edition.8 RACF = residential aged-care facility. | |||||||||||||||
- Julie O’Halloran1
- Helena Britt2
- Lisa Valenti3
- Australian GP Statistics and Classification Centre, University of Sydney, Sydney, NSW.
We wish to thank the GPs who participated in the BEACH study between April 2004 and March 2006. Over the study period, BEACH was supported by the Australian Government Department of Health and Ageing, AstraZeneca (Australia), Roche Products, Janssen Cilag, Merck Sharp and Dohme (Australia), Pfizer Australia and the National Prescribing Service.
None identified.
- 1. Australian Government Department of Health and Ageing. Home and Community Care Program overview. Canberra: DoHA, 2005. http://www.health.gov.au/internet/wcms/Publishing.nsf/Content/hacc-index.htm (accessed Apr 2007).
- 2. Australian Government Department of Health and Ageing. Extended Aged Care at Home packages. Canberra: DoHA, 2007. http://www.health.gov.au/internet/wcms/Publishing.nsf/Content/ageing-commcare-each.htm (accessed Apr 2007).
- 3. Australian Institute of Health and Welfare. Residential aged care in Australia 2004–05: a statistical overview. Canberra: AIHW, 2006. (AIHW Cat. No. AGE 45; Aged Care Statistics Services No. 22.) http://www.aihw.gov.au/publications/index.cfm/title/10303 (accessed Jun 2007).
- 4. Lewis GA, Pegram RW. Residential aged care and general practice: workforce demographic trends, 1984–2000. Med J Aust 2002; 177: 84-86. <MJA full text>
- 5. Charles J, Britt H, Valenti L. The independent effect of age of general practitioner on clinical practice. Med J Aust 2006; 185: 105-109. <MJA full text>
- 6. Britt H, Miller GC, Charles J, et al. General practice activity in Australia 2005–06. Canberra: Australian Institute of Health and Welfare, 2007. (AIHW Cat. No. GEP 19; General Practice Series No. 19.) http://www.aihw.gov.au/publications/index.cfm/title/10377 (accessed Jun 2007).
- 7. Britt H, Miller G, Bayram C. The quality of data on general practice — a discussion of BEACH reliability and validity. Aust Fam Physician 2007; 36: 36-40.
- 8. Classification Committee of the World Organization of Family Doctors. International Classification of Primary Care, 2nd ed (ICPC-2). Oxford: Oxford University Press, 1997.
- 9. Family Medicine Research Centre. ICPC-2 PLUS: the BEACH coding system. Sydney: FMRC, 2005. http://www.fmrc.org.au/icpc2plus/ (accessed Feb 2007).
- 10. Australian Institute of Health and Welfare. Dementia in Australia: national data analysis and development. Canberra: AIHW, 2007. (AIHW Cat. No. AGE 53.) http://www.aihw.gov.au/publications/index.cfm/title/10368 (accessed Jun 2007).
- 11. Jorm AF, Dear KBG, Burgess NM. Projections of future numbers of dementia cases in Australia with and without prevention. Aust N Z J Psychiatry 2005; 39: 959-963.
- 12. Australian Bureau of Statistics. Disability, ageing and carers, Australia: summary of findings, 2003. Canberra: ABS, 2004. (ABS Cat. No. 4430.0.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/Lookup/4430.0Main+Features12003 ?OpenDocument (accessed Apr 2007).
- 13. Giles LC, Cameron ID, Crotty M. Disability in older Australians: projections for 2006–2031. Med J Aust 2003; 179: 130-133. <MJA full text>
- 14. Stephen LJ, Brodie MJ. Epilepsy in elderly people. Lancet 2000; 355: 1441-1446.
- 15. Harvey PD, Bertisch H, Friedman JI, et al. The course of functional decline in geriatric patients with schizophrenia: cognitive-functional and clinical symptoms as determinants of change. Am J Geriatr Psychiatry 2003; 11: 610-619.
- 16. Fleischman DA, Wilson RS, Schneider JA, et al. Parkinsonian signs and functional disability in old age. Exp Aging Res 2007; 33: 59-76.
- 17. Britt H, Miller GC, Knox S, et al. General practice activity in the states and territories of Australia 1998–2003. Canberra: AIHW, 2004. (AIHW Cat. No. GEP 15; General Practice Series No. 15.)
- 18. Australian Government Department of Health and Ageing. Medicare Benefits Schedule book. Canberra: DoHA, 2006.
- 19. Wilkinson D, Dick MLB, Askew DA. General practitioners with special interests: risk of a good thing becoming bad? Med J Aust 2005; 183: 84-86. <MJA full text>
- 20. Australian Government Department of Health and Ageing. Aged care — improved health services for residents of aged care homes. Canberra: DoHA, 2007. http://www.health.gov. au/internet/budget/publishing.nsf/Content/budget2007-afact13.htm (accessed May 2007).





Abstract
Objectives: To describe the patients seen and the clinical activity undertaken by general practitioners during encounters at residential aged-care facilities (RACFs), and to ascertain how these differ from all GP encounters in Australia as a whole.
Design and participants: A secondary analysis of encounter data from the Bettering the Evaluation and Care of Health (BEACH) study, April 2004 to March 2006, comparing RACF consultations (identified by Medicare item numbers) with all BEACH study encounters in Australia. Participants were a random sample of GPs who had claimed at least 375 general practice Medicare items in the 3 months prior to the study.
Main outcome measures: Differences in the characteristics of GPs and patients at RACF consultations, morbidities managed, and treatments provided to patients.
Results: Over the study period there were 2310 RACF encounters out of a total of 197 000 BEACH encounters; 360/1970 GPs (18.4%) recorded at least one RACF consultation. GPs aged ≥ 45 years were more likely to record at least one RACF consultation than those aged < 45 years. Patients were predominantly women (70.7%), and 83.4% were aged ≥ 75 years. At RACF consultations, problems managed significantly more often included chronic problems, as well as psychological, neurological, urological, circulatory, eye and musculoskeletal problems. Dementia was the most common problem managed, at 33 times the usual management rate in everyday practice. Significantly fewer medications, non-pharmacological treatments, referrals, pathology and imaging tests were recorded at RACF consultations.
Conclusion: GP encounters at RACFs involve the management of chronic and complex conditions, including some not frequently seen in everyday general practice. The provision of additional education and resources where required may assist with workforce shortages in this setting.