In 1999, the Australian Institute of Health and Welfare (AIHW) reported on the burden of disease and injury in Australia,1 and showed that in 1996 the Northern Territory (NT) had the highest burden of fatal disease and injury among Australian states and territories.
Within Australia, the NT population is distinctive in many ways. In 2001, it was about 198 000, making up only 1% of the Australian population; it has a high proportion of Aboriginal and Torres Strait Islander people (29%, compared with 2.4% for Australia as a whole); and most of the Aboriginal population lives in rural and remote areas.2,3 It is well documented that Aboriginal death rates far exceed those for the non-Aboriginal population in the NT.4,5 Aboriginals have a life expectancy 20 years less than other Australians.6 Circulatory disease, respiratory disease and injury were the main causes of death in the Aboriginal population in the NT during 1979–1995.
While there is general consensus that Aboriginal and Torres Strait Islander people have a greater need for healthcare services than other Australians, the evidence for this is generally limited to mortality and to reports on the high prevalence of infectious diseases and lifestyle disorders.7 There is a lack of documented evidence to enable a comparison of the health status of Aboriginal and non-Aboriginal populations through a summary measure of both fatal and non-fatal health outcomes, and a study of the burden of disease and injury in Aboriginal people is long overdue.1,8
The disability-adjusted life-year (DALY) is a population-based health measure to inform health investment (see Box 1). In the World Health Report, the World Health Organization (WHO) has adopted the DALY as a standard measure of reporting and comparing population health for individual countries.9
Our study uses the DALY method to determine the burden of disease within the NT population compared with that in the national population, and also quantifies the differences in burden of disease between the NT Aboriginal and NT non-Aboriginal populations.
The calculation of the DALY is similar to that of the quality-adjusted life-year (QALY), a measure widely used in social and medical research.10 The DALY combines years of life lost (YLL) due to premature mortality and years lost due to disability (YLD), with time as the common metric to quantify healthy life lost due to fatal or non-fatal diseases, injuries and selected risk factors.11,12 To make a consistent and meaningful comparison with national results, we used the same case definitions, disease stages, disability weights and disease sequelae as the national study.1 Following the classification scheme used by the national study, we used 22 groups of disease and injury categories, most of which correspond to chapter-level groups of the International classification of diseases – ninth revision (ICD-9) codes. Estimates of burden of disease were made for a comprehensive set of 176 disease and injury categories.
In some key areas, methods vary from those of the 1996 Burden of Disease and Injury in Australia study.1 First, separate analyses were made for Aboriginal and non-Aboriginal populations in recognition of both the high proportion of Aboriginal people in the NT population and different disease patterns in the two groups. Second, because of the small population size in the NT, data for 5 years (from 1994 to 1998) were combined for the analyses of YLL and YLD.
The estimated resident population was obtained from the Australian Bureau of Statistics (ABS).13 The Aboriginal population was derived using ABS experimental estimates of the Aboriginal and Torres Strait Islander population.14 Mortality data for the period 1994–1998 were also available from the ABS, which gathers death data from the Registrars of Births, Deaths and Marriages in each state and territory, and then codes the underlying cause of death using the ICD-9. Since 1999, the ABS has coded causes of death using the International classification of diseases – tenth revision (ICD-10). About 9% of the death data for 1998 were coded according to the ICD-10 because of late registration. Backward mapping was used to recode the ICD-10 causes of death to ICD-9. The 1999 and 2000 mortality data were used for corrections of late registrations. Data sources for estimating YLD are summarised in Box 2. In general, a hierarchical checklist was used to rank the potential relevance of available data sources. Local disease register or surveillance data were considered most relevant, followed by local epidemiological surveys, national or interstate disease register or surveillance systems, national or interstate epidemiological surveys, local service activity data, international epidemiological studies and, last in the hierarchy, expert opinion.
We undertook a comprehensive literature search to identify all the key diseases that were found to be either more or less common in Aboriginal people. By using DisMod II, separate disease models were established for the Aboriginal and non-Aboriginal populations to summarise the available epidemiological information of each specific condition with internally consistent measures of incidence, prevalence, remission, mortality and duration.21
The most reliable source for YLD estimates was disease registry or surveillance system data (51 disease or injury categories, making up 11% of total YLD). Information from local or interstate epidemiological studies was applied to 12 disease categories (31% of YLD), while 38 disease categories (18% of YLD) relied on public hospital inpatient episode data for conditions for which there was a great likelihood of admission. Hospital admission rate ratios were applied to another 13 disease categories (15% of YLD) to derive YLD estimates for Aboriginal people. These hospital admission rate ratios were derived from public hospital and population data for 1994 to 1998. A unique hospital registration number is available for each individual admitted to any NT public hospital, and this was used to eliminate repeated admissions of the same patient to NT hospitals at different times and locations for the same condition. A rate ratio greater than 1 indicates that hospital admission for Aboriginal people is more common than for non-Aboriginal people. Both principal diagnosis and associated multiple secondary diagnoses were used to identify specific conditions. This method assumes that the NT non-Aboriginal incidence is consistent with the national average incidence and that the likelihood of admission for a given disease is similar for Aboriginal and non-Aboriginal people.
For the remaining 62 disease categories (25% of YLD), we found no conclusive evidence of a different incidence or prevalence among Aboriginal compared with non-Aboriginal people. Therefore, national “average” incidence, duration and prevalence from the national study were applied for these categories.
Between 1 January 1994 and 30 December 1998, a total of 127 900 DALYs were lost in the NT. The male to female ratio was 1.36, which is disproportionate to the population sex ratio of 1.11. NT Aboriginal people were over-represented in total DALYs (47.4% of DALYs in 29% of the population). The leading causes for the total NT burden of disease and injury were cardiovascular disease, mental disorders, cancers, unintentional injury and chronic respiratory disease. Compared with the national average, the NT has markedly higher proportions of both unintentional and intentional injury, acute respiratory infections and neonatal disorders. NT Aboriginal people had a higher proportion of DALYs attributable to cardiovascular disease, acute respiratory infections, diabetes and neonatal disorders than NT non-Aboriginal people (Box 3).
Comparing specific diseases, ischaemic heart disease, road traffic accidents and substance abuse disorders were the leading contributors to total disease burden for both Aboriginal and non-Aboriginal males. Among Aboriginal females, type 2 diabetes, ischaemic heart disease and otitis media were the major contributors, while, for non-Aboriginal females, affective disorder, anxiety disorder and asthma were more prominent.
After age-standardisation, the burden of disease in DALYs per 1000 population was 17% higher in males than females. Overall burden of disease and injury in the NT during 1994–1998 was 183.2 DALYs lost per 1000 population, which exceeded the Australian rate of 137.11 by 34%. The burden of disease and injury for NT Aboriginal people was 339.9 DALYs per 1000 — 2.5 times higher than the Australian rate. The rate for NT non-Aboriginals was 137.7 DALYs per 1000, which is similar to the Australian rate. The magnitude of the differential between males and females was similar for both groups (Box 4).
Box 5 shows the rate ratios of age-standardised rates for YLL and YLD between the NT Aboriginal and NT non-Aboriginal populations. The age-standardised mortality burden (YLL) for NT Aboriginal people was substantially higher than that for NT non-Aboriginal people. The largest disparity existed in fatal genitourinary diseases and diabetes mellitus. The overall disability burden (YLD) was also higher in Aboriginal people than in their non-Aboriginal counterparts. The greatest discrepancy was in nutritional disorders, acute respiratory infections and intentional injuries.
Aboriginal people bear a higher burden of disease and injury per head of population than non-Aboriginal people for all age groups. This peaks in the 35–54-years age groups, where Aboriginal people bear 4.1 times the burden of disease and injury of non-Aborignal people (Box 6). Aboriginal people experience DALY rates at the level of non-Aboriginal people who are 20 to 30 years older, with DALY rates in Aboriginal people aged 45–54 years exceeding those of non-Aboriginal people aged 65–74 years.
The strength of using the DALY is that it summarises both mortality and morbidity information, and facilitates meaningful comparisons when setting healthcare service priorities, identifying disadvantaged population groups and evaluating health interventions.11 Our analyses of DALYs by age, sex and Aboriginality show that NT Aboriginal adults experience levels of health comparable to those of non-Aboriginal people 20–30 years older, and that a gap exists in both fatal and non-fatal health outcomes. Much of this discrepancy occurs in diseases with preventable and environmental antecedents such as diet, lifestyle, education and physical activity, which are amenable to intervention.22,23 Some of the gaps show sex differences; for example, nutritional disorders (YLL) and intentional injuries (YLD) affect more Aboriginal women than men. The causes for these differences warrant further investigation.
The DALY has the capacity to inform questions of both the need for and equity of distribution of healthcare funding.1,24 It provides a more equitable system than the crude “per capita” method for comparing health status for the purpose of allocating health resources. Linking burden-of-disease data with expenditure data for the financial year 1996–97 indicates that federal health funding for the whole of Australia was $7890 per DALY, and $6413 per DALY in the NT. This is a level almost 20% below the national average, before consideration of the higher costs of healthcare services in an environment complicated by remoteness and cultural complexity.25
By providing an alternative and more precise tool to assess and monitor needs for healthcare in the NT, our study is a step toward more effective and efficient resource allocation, particularly if the burden of disease information can be linked with evaluating the cost-effectiveness of potential interventions. Nevertheless, our study remains exploratory because of potential inaccuracies in the data used. We judged that the quality of data sources varied from “excellent” in disease surveillance systems to “reasonable” for the extrapolation method of national averages. The quality of some datasets has been validated in the past. A previous NT study showed a very high level of agreement (94%) between interviews and NT hospital data on Indigenous status,26 and, with regard to underidentification of Aboriginal population, “the error of closure” has been reported as being lowest in the NT.27 Since 1997, the ABS has changed from manual coding to autocoding. The trend in autocoding sensitive diseases such as pneumonia was examined and found to have minimal impact on results.28 The precision of the YLD estimates is not quantifiable in the usual statistical sense of deriving a confidence interval, because of the diversity of the data sources used.1 Simulation modelling and sensitivity analysis are planned for the next phase of this study, and will more formally quantify the uncertainty around DALY estimates. In a next phase, we also plan to include estimation of the burden attributable to important modifiable risk factors such as tobacco, alcohol and blood pressure.
1: Glossary
DALY: Disability-adjusted life-year. A time-based measure of health status used to summarise the burden of premature mortality and disability.
DisMod: A disease-modelling software package.
QALY: Quality-adjusted life-year. A generic measure of health outcome.
YLD: Years lost due to disability. To estimate YLD on a population basis, the number of non-fatal cases is multiplied by the average duration of the disease and a weight that reflects the severity of the disease on a scale from 0 (perfect health) to 1 (dead).
YLL: Years of life lost due to premature mortality. To estimate YLL on a population basis, the number of people who died at a specific age is combined with the remaining standard life expectancy at that age. This study calculated YLL at a given age on the basis of the same cohort life expectancy used in the national study (with life expectancy at birth of 81.5 years for males and 85.7 years for females).
2: Data sources used for this study
A. Disease registers, surveillance and notification systems
◆ Northern Territory Cancer Registry; ◆ Northern Territory Perinatal Data Collection; ◆ National Congenital Malformations Registry; ◆ Northern Territory Notifiable Diseases Databases; ◆ Northern Territory HIV/AIDS Databases; ◆ Tasmanian Insulin-Treated Diabetes Register; ◆ Victorian Huntington’s Chorea Register; ◆ Australian Sentinel Practice Research Network; ◆ Australian and New Zealand Register of Dialysis and Transplant Patients (ANZDATA); ◆ Northern Territory Growth Assessment and Action Program Database.
B. National population health surveys
◆ National Health Survey 1995, ABS; ◆ South Australian Dental Surveys 1988 to 1996; ◆ National Oral Health Survey 1988–89; ◆ Child Dental Health Survey 1996; ◆ National Women’s Longitudinal Health Survey; ◆ Active Australia Baseline Survey 1997; ◆ National Mental Health Survey 1997, ABS; ◆ Survey of Disability, Ageing and Carers 1998, ABS; ◆ National Drug Strategy Household Survey.
C. Health service activity data
◆ Northern Territory Hospital Morbidity Data; ◆ Northern Territory Emergency Department Dataset; ◆ Medicare claims database; ◆ National survey of general practice (BEACH).
D. Epidemiological studies
◆ nephritis/nephrosis;15 ◆ type 2 diabetes;16 ◆ substance abuse;17 ◆ otitis media;18 ◆ affective disorder;19 ◆ anxiety disorders;20 ◆ other interstate or international studies (see details in Mathers et al1).
ABS = Australian Bureau of Statistics.
3: Top 15 leading causes of disease burden, Northern Territory 1994–1998
|
DALYs × 1000 (%) |
||||||||||
Major disease category* |
NT Aboriginal |
NT non- Aboriginal |
Northern Territory |
Australia 1996‡ |
|||||||
Male |
|
|
|
|
|||||||
Cardiovascular disease |
6.2 (19.1%) |
5.9 (14.2%) |
12.1 (16.4%) |
298.7 (22.4%) |
|||||||
Mental disorders† |
3.0 (9.3%) |
6.9 (16.7%) |
9.9 (13.4%) |
164.2 (12.3%) |
|||||||
Unintentional injury |
3.8 (11.9%) |
5.8 (14.1%) |
9.6 (13.1%) |
98.9 (7.4%) |
|||||||
Malignant neoplasms |
2.3 (7.0%) |
6.1 (14.8%) |
8.4 (11.4%) |
252.1 (18.9%) |
|||||||
Chronic respiratory disease |
2.5 (7.8%) |
2.9 (7.1%) |
5.4 (7.4%) |
95.0 (7.1%) |
|||||||
Intentional injury |
1.6 (5.1%) |
3.1 (7.5%) |
4.7 (6.4%) |
52.3 (3.9%) |
|||||||
Acute respiratory infections |
2.9 (9.1%) |
0.4 (1.1%) |
3.4 (4.6%) |
14.5 (1.1%) |
|||||||
Nervous system and sense organ disorders |
1.2 (3.6%) |
2.2 (5.3%) |
3.3 (4.5%) |
107.4 (8.1%) |
|||||||
Neonatal disorders |
1.6 (4.9%) |
1.5 (3.6%) |
3.1 (4.2%) |
16.6 (1.2%) |
|||||||
Diabetes mellitus |
1.7 (5.2%) |
1.0 (2.4%) |
2.7 (3.6%) |
39.4 (3.0%) |
|||||||
Diseases of the digestive system |
1.0 (3.0%) |
1.1 (2.7%) |
2.1 (2.8%) |
33.9 (2.5%) |
|||||||
Infectious and parasitic diseases |
1.0 (3.1%) |
1.0 (2.3%) |
2.0 (2.7%) |
28.3 (2.1%) |
|||||||
Congenital abnormalities |
0.9 (2.7%) |
0.8 (1.9%) |
1.7 (2.2%) |
17.6 (1.3%) |
|||||||
Genitourinary disease |
0.6 (1.8%) |
0.6 (1.5%) |
1.2 (1.6%) |
34.5 (2.6%) |
|||||||
Musculoskeletal disease |
0.2 (0.6%) |
1.0 (2.3%) |
1.1 (1.6%) |
34.5 (2.6%) |
|||||||
Total |
32.4 (100%) |
41.2 (100%) |
73.6 (100%) |
1331.3 (100%) |
|||||||
Female |
|
|
|
|
|||||||
Mental disorders† |
2.9 (10.1%) |
5.8 (22.3%) |
8.7 (16.0%) |
169.7 (14.4%) |
|||||||
Cardiovascular disease |
4.4 (15.7%) |
2.6 (10.1%) |
7.1 (13.0%) |
249.9 (21.2%) |
|||||||
Malignant neoplasms |
1.9 (6.7%) |
4.0 (15.3%) |
5.9 (10.8%) |
226.5 (19.2%) |
|||||||
Chronic respiratory disease |
2.3 (8.2%) |
2.1 (8.2%) |
4.5 (8.2%) |
83.8 (7.1%) |
|||||||
Unintentional injury |
1.9 (6.8%) |
1.7 (6.7%) |
3.6 (6.7%) |
44.3 (3.8%) |
|||||||
Diabetes mellitus |
2.2 (7.8%) |
0.8 (3.2%) |
3.0 (5.6%) |
35.5 (3.0%) |
|||||||
Acute respiratory infections |
2.5 (8.8%) |
0.5 (1.9%) |
3.0 (5.5%) |
15.2 (1.3%) |
|||||||
Neonatal disorders |
1.4 (5.1%) |
1.3 (5.0%) |
2.7 (5.1%) |
13.9 (1.2%) |
|||||||
Nervous system and sense organ disorders |
1.1 (3.8%) |
1.5 (5.7%) |
2.6 (4.7%) |
128.0 (10.9%) |
|||||||
Musculoskeletal disease |
0.5 (1.9%) |
1.4 (5.3%) |
1.9 (3.5%) |
55.4 (4.7%) |
|||||||
Genitourinary disease |
1.0 (3.7%) |
0.8 (3.0%) |
1.8 (3.4%) |
27.4 (2.3%) |
|||||||
Congenital abnormalities |
0.9 (3.2%) |
0.7 (2.8%) |
1.7 (3.0%) |
14.8 (1.3%) |
|||||||
Intentional injury |
1.0 (3.5%) |
0.6 (2.2%) |
1.6 (2.9%) |
14.5 (1.2%) |
|||||||
Diseases of the digestive system |
0.8 (2.8%) |
0.7 (2.7%) |
1.5 (2.8%) |
30.5 (2.6%) |
|||||||
Infectious and parasitic diseases |
0.8 (2.8%) |
0.5 (1.9%) |
1.3 (2.4%) |
16.9 (1.4%) |
|||||||
Total |
28.2 (100%) |
26.1 (100%) |
54.3 (100%) |
1179.0 (100%) |
|||||||
DALYs = Disability-adjusted life-years. NT = Northern Territory. * Ranked in order of total DALYs for the Northern Territory for males and females. † = Mental disorders include substance abuse. ‡ Data from The burden of disease and injury in Australia.1 |
|||||||||||
4: Age-standardised DALY rate per 1000 population, by sex and Aboriginality, for the Northern Territory in 1994–1998, compared with Australia in 1996
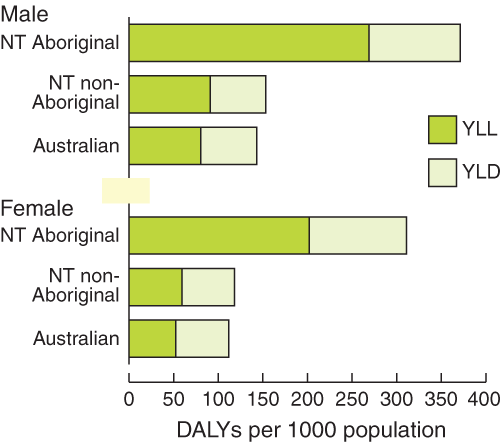
DALY = disability-adjusted life-years. YLL = Years of life lost due to premature mortality. YLD = Years lost due to disability.
5: Age-standardised burden of disease rate ratios (Aboriginal v non-Aboriginal), by sex, Northern Territory 1994–1998
|
Years of life lost due to premature mortality |
Years lost due to disability |
|||||||||
|
Male |
Female |
Male |
Female |
|||||||
Infectious and parasitic diseases |
4.4 |
8.5 |
1.3 |
2.0 |
|||||||
Acute respiratory infections |
13.8 |
7.5 |
12.2 |
13.0 |
|||||||
Maternal conditions |
0 |
0.1 |
0.0 |
5.7 |
|||||||
Neonatal disorders |
2.3 |
2.1 |
1.1 |
1.3 |
|||||||
Nutritional disorders* |
3.5 |
10.7 |
14.5 |
14.4 |
|||||||
Malignant neoplasms |
1.6 |
1.4 |
0.6 |
0.7 |
|||||||
Other neoplasms |
0 |
3.5 |
2.2 |
2.5 |
|||||||
Diabetes mellitus |
10.8 |
9.1 |
3.7 |
4.9 |
|||||||
Endocrine and metabolic disorders |
4.7 |
8.0 |
3.2 |
3.6 |
|||||||
Mental disorders |
3.0 |
5.2 |
1.1 |
1.1 |
|||||||
Nervous system and sense organ |
2.7 |
1.7 |
1.7 |
2.1 |
|||||||
Cardiovascular disease |
3.6 |
4.0 |
1.9 |
2.2 |
|||||||
Chronic respiratory disease |
3.6 |
4.5 |
1.7 |
1.6 |
|||||||
Diseases of the digestive system |
2.9 |
4.3 |
1.2 |
1.2 |
|||||||
Genitourinary diseases |
20.8 |
10.4 |
1.5 |
1.5 |
|||||||
Skin diseases |
5.0 |
3.8 |
2.5 |
2.1 |
|||||||
Musculoskeletal diseases |
3.6 |
2.8 |
0.7 |
0.8 |
|||||||
Congenital abnormalities |
2.3 |
2.4 |
1.5 |
1.6 |
|||||||
Oral health |
0 |
0 |
4.1 |
4.3 |
|||||||
Unintentional injuries |
2.4 |
3.2 |
1.0 |
1.8 |
|||||||
Intentional injuries |
1.4 |
3.1 |
7.9 |
17.1 |
|||||||
Total |
3.0 |
3.4 |
1.6 |
1.9 |
|||||||
* Includes protein-energy malnutrition (stunting, wasting and developmental disability), iron-deficiency anaemia and other nutritional deficiencies. |
|||||||||||
- Yuejen Zhao1
- Steve Guthridge2
- Anne Magnus3
- Theo Vos4
- 1 Health Gains Planning, Northern Territory Department of Health and Community Services, Casuarina, NT.
- 2 Health Surveillance and Evaluation Section, Victorian Department of Human Services, Melbourne, VIC.
- 3 School of Public Health, University of Queensland, Brisbane, QLD.
The study was conducted within the Northern Territory Department of Health and Community Services with technical support from the Victorian Department of Human Services.
None identified.
- 1. Mathers C, Vos T, Stevenson C. The burden of disease and injury in Australia. Canberra: AIHW, 1999. (Catalogue no. PHE 17.)
- 2. Australian demographic statistics, December quarter 2001. Canberra: Australian Bureau of Statistics, 2002. (Catalogue no. 3101.0.)
- 3. Population distribution, Aboriginal and Torres Strait Islander Australians 2001. Canberra: Australian Bureau of Statistics, 2002. (Catalogue no. 4705.0.)
- 4. Condon J, Warman G, Arnold L. The health and welfare of Territorians. Darwin: Territory Health Services, Epidemiology Branch, 2001.
- 5. Dempsey K, Condon J. Mortality in the Northern Territory 1979–1997. Darwin: Territory Health Services, 1999.
- 6. Deaths 2001 Australia. Canberra: Australian Bureau of Statistics, 2002. (Catalogue no. 3302.0.)
- 7. Deeble J, Mathers C, Smith L, et al. Expenditures on health services for Aboriginal and Torres Strait Islander people. Canberra: Australian Institute of Health and Welfare, 1998. (AIHW cat no. HWE 6.)
- 8. Pike A, Baade P, Harper C, et al. Quantifying the burden of disease and injury in Queensland 1996–1998. Information circular 61. Brisbane: Health Information Centre, Queensland Health, 2002.
- 9. The World Health Report, 2002: reducing risks, promoting healthy life. Geneva: World Health Organization, 2002.
- 10. Nord E. Methods for quality adjustment of life years. Soc Sci Med 1992; 34: 559-569.
- 11. Murray CJL. Quantifying the burden of disease: the technical basis for disability-adjusted life years. Bull World Health Organ 1994; 72: 429-445.
- 12. The Victorian Burden of Disease Study: mortality. Melbourne: Victorian Government Department of Human Services, 1999.
- 13. Population by age and sex, Australian states and territories. Canberra: Australian Bureau of Statistics, 2001. (Catalogue no. 3201.0.)
- 14. Experimental estimates of the Aboriginal and Torres Strait Islander population, 1991–1996. Canberra: Australian Bureau of Statistics, 1998. (Catalogue no. 3230.0.)
- 15. Hoy W. Renal disease in Australian Aboriginals: community health programs are critical to containing the renal disease epidemic. Med J Aust 1996; 165: 126-127.
- 16. Guest CS, O’Dea K. Diabetes in Aborigines and other Australian populations. Aust J Pub Health 1992; 16: 340-349.
- 17. Brady M. Aboriginal drug and alcohol use: recent developments and trends. Aust N Z J Public Health 1997; 21: 3-4.
- 18. Boswell J. Presentation of early otitis media in “Top End” Aboriginal infants. Aust N Z J Public Health 1997; 21:100-102.
- 19. Zubrick SR, Silburn SR, Burton P, et al. Mental health disorders in children and young people: scope, cause and prevention. Aust N Z J Psychiatry 2000; 34: 570-578.
- 20. Cairney S, Maruff P, Clough AR. The neurobehavioural effects of kava. Aust N Z J Psychiatry 2002; 36: 657-662.
- 21. Barendregt JJ, van Oortmarssen GJ, Vos T, Murray CJL. A generic model for the assessment of disease epidemiology: the computational basis of DisMod II. Popul Health Metrics 2003; 1(4): 1-8.
- 22. Hoy W, Mathews J, McCredie D, et al. The multidimensional nature of renal disease: rates and associations of albuminuria in an Australian Aboriginal community. Kidney Int 1998; 54:1296-1304.
- 23. Bennett S. Cardiovascular risk factors in Australia: trends in socioeconomic inequalities. J Epidemiol Community Health 1995; 49: 363-372.
- 24. Deeble J. Resource allocation in public health. Melbourne: National Public Health Partnership, 1999.
- 25. Health expenditure, Australia 2000–01. Canberra: Australian Institute of Health and Welfare, 2002. (Catalogue no. HWE 20.)
- 26. Condon JR, Williams DJ, Pearce MC, et al. Northern Territory hospital morbidity dataset: validation of demographic data 1997. Darwin: Territory Health Services, 1998.
- 27. Population Issues: Indigenous Australians, 1996. Australian Bureau of Statistics Occasional Paper. Canberra: ABS, 1999. (Catalogue no. 4708.0.)
- 28. McKenzie K, Tong S, Walker S, Sadkowsky K. Evolution in classifying mortality statistics. Sydney: National Centre for Classification in Health, 2002.





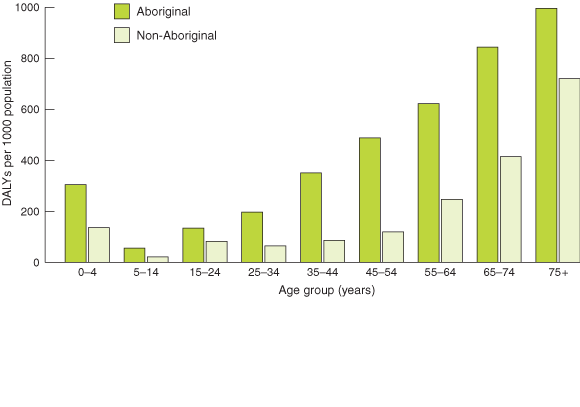
Abstract
Objective: To quantify the burden of disease and injury for the Aboriginal and non-Aboriginal populations in the Northern Territory.
Design and setting: Analysis of Northern Territory data for 1 January 1994 to 30 December 1998 from multiple sources.
Main outcome measures: Disability-adjusted life-years (DALYs), by age, sex, cause and Aboriginality.
Results: Cardiovascular disease was the leading contributor (14.9%) to the total burden of disease and injury in the NT, followed by mental disorders (14.5%) and malignant neoplasms (11.2%). There was also a substantial contribution from unintentional injury (10.4%) and intentional injury (4.9%). Overall, the NT Aboriginal population had a rate of burden of disease 2.5 times higher than the non-Aboriginal population; in the 35–54-year age group their DALY rate was 4.1 times higher. The leading causes of disease burden were cardiovascular disease for both Aboriginal men (19.1%) and women (15.7%) and mental disorders for both non-Aboriginal men (16.7%) and women (22.3%).
Conclusions: A comprehensive assessment of fatal and non-fatal conditions is important in describing differentials in health status of the NT population. Our study provides comparative data to identify health priorities and facilitate a more equitable distribution of health funding.