Australian Aboriginal people in the Northern Territory have poor health compared with the Australian general population. Average birthweights have been low since they were first recorded in the early 1960s, and, despite recent improvements, rates of low birthweight are still more than twice those in non-Aboriginal babies.1 Intrauterine growth retardation is the main cause of low birthweight, with teenage pregnancy, maternal malnutrition, smoking, alcohol use, infections, social stress and poor antenatal care all contributing.2 Since the early 1980s epidemic rates of type 2 diabetes, cardiovascular and renal disease have developed among Aboriginal people.
The fetal origins hypothesis links low birthweight to chronic disease in adult life and proposes that adaptations by the fetus to promote survival under less-than-ideal conditions lead to persistent changes in structure and function.3 Evidence for such an effect has come from animal studies (showing lower nephron numbers4 and hypertension5 in offspring of protein-depleted mothers) as well as from epidemiological studies. A recent systematic review (80 studies with more than 444 000 subjects) showed a small but consistent inverse relationship between birthweight and later blood pressure, with a 1 kg increase in birthweight associated with an average 1–2 mmHg decrease in systolic blood pressure.6
Blood pressure correlates positively with current body size.6 The influences of birth size and adult size can be combined into one unifying life course hypothesis. This hypothesis proposes that adverse intrauterine events lead to adaptations, which, in the face of further adverse events, manifest in adult life as chronic conditions including cardiovascular disease, type 2 diabetes and hypertension.7
We examined the relationships between blood pressure and birthweight and current body mass index in a group of children and adults in one Aboriginal community living on two islands off the northern coast of Australia.
Our study involved a subset of the participants in a community-wide screening program for whom birthweights were available.8
Between January 1992 and October 1998, a community-wide screening program examined the rates and associations of renal disease and cardiovascular risk factors in a remote Aboriginal community. Community members had high rates of chronic disease, renal failure and chronic disease deaths.9
Using standard techniques, height was measured to the nearest 0.1 cm on a wall-mounted stadiometer and weight to 0.1 kg on a beam balance. Blood pressure was measured on the right arm in the seated position with an automated blood pressure instrument (Dinamap, Critikon, GE Medical Systems, Tampa, Florida) and appropriate-size cuffs.
Birthweight and length were collected from health records at the local community health clinic and the regional hospital. Birthweight records have been kept since 1958, although the records are incomplete until the mid 1960s (up until that time many babies were still being born in the bush). Thus, the study population was less than 43 years old. Birth lengths and gestational age were available less consistently.
The associations of systolic blood pressure and diastolic blood pressure with birthweight and ponderal index (birthweight [kg]/birth length [m3]) were examined in linear regression models. Because of the strong cohort effect on birthweight, adjustment for age was included for both children and adults.
High blood pressure was defined as systolic blood pressure ≥ 140 mmHg and/or diastolic blood pressure ≥ 90 mmHg (World Health Organization) or as systolic blood pressure ≥ 130 mmHg and/or diastolic blood pressure ≥ 85 mmHg (levels of concern in high-risk populations).10 The associations of high blood pressure with low birthweight were examined in logistic regression models. In addition, adults were analysed by categories based on birthweight (low or normal birthweight) and current body mass index (BMI; overweight ≥ 25 kg/m2 or normal).
All analyses were carried out using the STATA statistical package.11
The community-wide screening program included 81.6% of the total population (1473/1805). Birthweights were available for 767 (71%) of the screening participants aged 7–43 years; 311 children (7–17 years of age) and 456 adults (199 women and 257 men).
Box 1 shows the characteristics of the total study population divided into adults and children. Adult women had significantly higher mean BMI (kg/m2) than adult men (24.5 [95% CI, 23.7–25.4] v 22.2 [95% CI, 21.6–22.7]), but did not differ significantly otherwise (data not shown).
The proportion of the population whose birthweight was known decreased with age, and the proportion of overweight subjects increased with age (Box 2). Mean birthweights increased from 2.69 kg in the 1970s to 2.96 kg in the 1990s.
In adults, a multiple regression model for systolic blood pressure, incorporating birthweight, current weight, age and sex, explained 20.0% of the variance in systolic blood pressure. An increase in birthweight of 1 kg was associated with a decrease in systolic blood pressure of 2.9 mmHg (95% CI, 0.3–5.5 mmHg). The effect in women was significant and greater than in men (4.7 mmHg [95% CI, 0.5–8.6 mmHg] v 1.4 mmHg [95% CI, 1.7–5.0 mmHg]). This is shown graphically in Box 3. In these multiple regression models, age was not significantly associated with blood pressure reduction.
There was no association between birthweight and blood pressure in children, before or after taking current weight into account.
In Box 4 the odds ratio of low-birthweight adults having high blood pressure (≥ 130/85 mmHg) relative to people of higher birthweight (adjusted for current age and BMI) was 2.3 (95% CI, 1.3–3.5). This effect was more marked in women. The population-attributable risk of high blood pressure (≥ 130/85 mmHg) if birthweight was low (< 2.5 kg) was 17%.
Box 5 shows that adults with normal birthweight and normal current BMI had the lowest mean systolic and diastolic blood pressures, and the group with low birthweight and high current BMI had the highest mean blood pressures. For the overweight as well as the normal BMI group, those with low birthweights had higher blood pressures than those with normal birthweights.
This is the first time an inverse relationship between birthweight and blood pressure has been demonstrated in Aboriginal adults. The phenomenon is important in the context of the high rates of low birthweight in remote Aboriginal communities and the detrimental effects of higher blood pressures on the manifestations and complications of the chronic diseases that Aboriginal people currently experience in epidemic proportions. The relationship is evident in young adult life, and will probably become more pronounced with further ageing, given the sharp increase in blood pressures in this group of people as they approach middle age.9 These data complement those from the same Aboriginal community showing an inverse relationship between birthweight and hyperinsulinaemia and birthweight and albuminuria.13,14
A similar relationship between birthweight and blood pressure has been found across the world in different populations, and at different age groups, from the newborn period to adulthood.6 The magnitude of the effect is similar. Other studies have also confirmed the amplifying effect of higher weight on this phenomenon. The apparently more marked effect in women than men has also been noted in some other studies, although the reasons remain unclear. However, a recent meta-analysis did not find a sex difference in the relationship between birthweight and systolic blood pressure.15
Our failure to show any relationship in children between birthweight and blood pressure probably reflects their relative leanness, as few showed early obesity, and only 6.3% were overweight. This accords with previous studies showing that low birthweight was a risk factor for high blood pressure only in overweight children.16 No association was seen in low-birthweight children who remained small.17
This community represents a population in epidemiological and health transition, which has seen significant improvements in infant survival and dramatic changes in diet and exercise over the past 40 years. The current epidemic of chronic disease appears, in part, to be a legacy of the survival of low-birthweight babies who, before the 1960s, would not have survived to adulthood. This effect is compounded by the accelerated changes in lifestyle experienced by this same cohort. Rates of chronic disease can be expected to rise over the intermediate term, as this relatively young cohort ages and as trends for an increase in BMI continue. However, the improving birthweights in this and other Aboriginal communities give some hope for ultimate partial abatement. Similar phenomena are also changing health profiles in other populations in transition.18
Public health interventions to encourage a healthy lifestyle, with well balanced diets and regular exercise to contain weight gain in adult life, must be given priority. People with low birthweight need to be especially targeted to maintain a modest adult BMI to reduce chronic disease risk.
1: Characteristics of the study population (mean, 95% CI)
|
Child* (n = 311) |
Adult (n = 456) |
|||||||||
Age (years) |
13.3 (12.9–13.7) |
28.3 (27.6–28.8) |
|||||||||
Weight (kg) |
42.2 (40.4–44.0) |
64.3 (62.8–65.7) |
|||||||||
Height (cm) |
150.8 (148.9–152.7) |
166.4 (165.7–167.2) |
|||||||||
Body mass index (kg/m2) |
17.8 (17.4–18.2) |
23.2 (22.7–23.7) |
|||||||||
Birthweight (kg) |
2.94 (2.9–3.0) |
2.71 (2.66–2.75) |
|||||||||
Number (%) with low birthweight (< 2.5 kg) |
55 (17.7%) |
157 (34.4%) |
|||||||||
Birth length (cm) (n = 515) |
48.8 (48.5–49.1) |
48.4 (48.0–48.8) |
|||||||||
Ponderal index (kg/m3) (n = 515) |
25.4 (25.0–25.7) |
24.0 (23.5–24.6) |
|||||||||
Systolic blood pressure (mmHg) |
103.8 (102.4–105.2) |
116.8 (115.4–118.1) |
|||||||||
Diastolic blood pressure (mmHg) |
58.6 (57.6–59.7) |
71.1 (70.0–72.1) |
|||||||||
| * 7–17 years. | |||||||||||
2: Birthweights and prevalence of overweight in the study population, by age group
Age (years) |
|||||||||||
7–10 (n = 62) |
11–17 (n = 249) |
18–29 (n = 272) |
30–43 (n = 184) |
||||||||
Percentage of population whose birthweight was known |
98.4% |
91.2% |
70.8% |
51.4% |
|||||||
(62/63) |
(249/273) |
(272/384) |
(184/358) |
||||||||
Mean birthweight in kg (95% CI) |
2.98 |
2.93 |
2.72 |
2.69 |
|||||||
(2.84–3.13) |
(2.88–3.00) |
(2.65–2.88) |
(2.62–2.75) |
||||||||
Percentage with low birthweight (< 2.5 kg) |
16.1% |
18.1% |
33.1% |
36.4% |
|||||||
(10/62) |
(45/249) |
(90/272) |
(67/184) |
||||||||
Percentage overweight (BMI 25 kg/m2)* |
6.5% |
9.2% |
21.0% |
46.2% |
|||||||
(4/62) |
(23/249) |
(57/272) |
(85/184) |
||||||||
* Conversion of child BMI to adult BMI equivalent of > 25 kg/m2 (corresponding to the 88th centile in girls and the 90th centile in boys).12 BMI = body mass index. |
|||||||||||
3: Multiple regression model — systolic blood pressure and birthweight
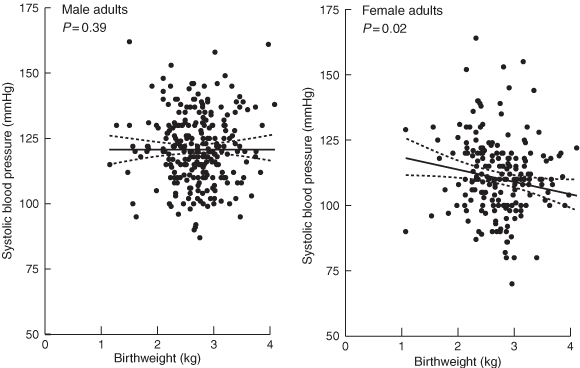
Systolic blood pressure and birthweight in adults by sex, adjusted for age and current weight.
4: Systolic and diastolic blood pressure (BP) (mmHg) and rates of hypertension in adults, by birthweight category, adjusted for age and current body mass index (and adjusted for sex in the “Total” category)
|
Birthweight < 2.5 kg |
Birthweight ≥ 2.5 kg |
Odds ratio (95% CI) |
||||||||
Systolic BP (95% CI) |
|||||||||||
Women |
115.5 (112.3–118.7) |
108.6 (106.1–111.1)* |
|
||||||||
Men |
123.5 (120.8–126.3) |
119.8 (118.0–121.8) |
|
||||||||
Total |
120.1 (118.0–122.2) |
114.9 (114.9–116.5)* |
|
||||||||
Diastolic BP (95% CI) |
|||||||||||
Women |
69.7 (67.5–71.9) |
66.9 (65.2–68.6) |
|
||||||||
Men |
75.3 (73.1–77.5) |
72.9 (71.2–74.2) |
|
||||||||
Total |
72.8 (71.2–74.4) |
70.2 (69.0–71.3) |
|
||||||||
Percentage with systolic BP ≥ 140 or diastolic BP ≥ 90 (95% CI) |
|||||||||||
Women (n = 199) |
5.8% (2.1%–15.0%) |
2.4% (0.8%–7.3%) |
2.5 (0.6–9.5) |
||||||||
Men (n = 257) |
13.9% (7.7%–23.8%) |
8.5% (5.1%–14.2%) |
1.7 (0.7–3.7) |
||||||||
Total (n = 456) |
9.6% (5.8%–15.7%) |
5.2% (3.1%–8.6%) |
1.9 (0.9–3.7) |
||||||||
Percentage with systolic BP ≥ 130 or diastolic BP ≥ 85 (95% CI) |
|||||||||||
Women (n = 199) |
17.3% (9.8%–28.7%) |
6.4% (3.1%–12.6%) |
3.6 (1.2–8.2)* |
||||||||
Men (n = 257) |
41.6% (30.9%–53.3%) |
27.5% (20.9%–35.1%) |
1.9 (1.0–3.7)* |
||||||||
Total (n = 456) |
29.1% (21.9%–37.6%) |
15.8% (11.8%–21.0%) |
2.3 (1.3–3.5)† |
||||||||
* P < 0.05; † P < 0.005 |
|||||||||||
5: Blood pressure in adults for categories of birthweight and current body mass index (BMI)
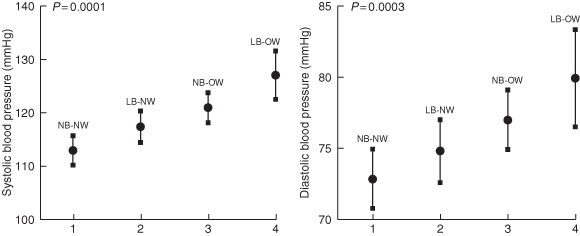
Mean systolic and diastolic blood pressure (95% CI), adjusted for age and sex.
1. NB-NW = Normal birthweight and normal current BMI.
2. LB-NW = Low birthweight and normal current BMI.
3. NB-OW = Normal birthweight and BMI in overweight range.
4. LB-OW = Low birthweight and BMI in overweight range.
- 1. Nasser N, Sullivan EA. Australia's mothers and babies 1999. Sydney: AIHW National Perinantal Statistics Unit, 2001. (Perinatal Statistics Series no.11.)
- 2. Sayers S, Powers J. Risk factors for Aboriginal low birthweight, intrauterine growth retardation and preterm birth in the Darwin Health Region. Aust N Z J Public Health 1997; 21: 524-530.
- 3. Barker DJ, Godfrey KM, Osmond C, Bull A. The relation of fetal length, ponderal index and head circumference to blood pressure and the risk of hypertension in adult life. Paediatr Perinat Epidemiol 1992; 6: 35-44.
- 4. Merlet-Bénichou C, Vilar J, Lelievre-Pegorier M, et al. Fetal nephron mass: its control and deficit. Adv Nephrol Necker Hosp 1997; 26: 19-45.
- 5. Ingelfinger JR, Woods LL. Perinatal programming, renal development, and adult renal function. Am J Hypertens 2002; 15(2 Pt 2): 46S-49S.
- 6. Huxley RR, Shiell AW, Law CM. The role of size at birth and postnatal catch-up growth in determining systolic blood pressure: a systematic review of the literature. J Hypertens 2000; 18: 815-831.
- 7. Ben-Shlomo Y, Smith GD. Deprivation in infancy or in adult life: which is more important for mortality risk? Lancet 1991; 337: 530-534.
- 8. Hoy WE, Mathews JD, McCredie DA, et al. The multidimensional nature of renal disease: rates and associations of albuminuria in an Australian Aboriginal community. Kidney Int 1998; 54: 1296-1304.
- 9. Hoy WE, Norman RJ, Hayhurst BG, Pugsley DJ. A health profile of adults in a Northern Territory Aboriginal community, with an emphasis on preventable morbidities. Aust N Z J Public Health 1997; 21: 121-126.
- 10. Report of the Joint National Committee on Detection, Evaluation, and Treatment of High Blood Pressure. A cooperative study. JAMA 1977; 237: 255-261.
- 11. Stata statistical software, release 7.0. College Station, Tex: Stata Corporation, 2001.
- 12. Cole TJ, Bellizzi MC, Flegal KM, Dietz WH. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 2000; 320: 1240-1243.
- 13. Hoy WE, Rees M, Kile E, et al. Low birthweight and renal disease in Australian Aborigines. Lancet 1998; 352: 1826-1827.
- 14. Hoy WE, Singh GR. Birth weight and risk for noncommunicable chronic diseases in Australian Aborigines. Nephrology 2003; 8 (Suppl): A 105.
- 15. Lawlor DA, Ebrahim S, Smith GD. Is there a sex difference in the association between birth weight and systolic blood pressure in later life? Findings from a meta-regression analysis. Am J Epidemiol 2002; 156: 1100-1104.
- 16. Jern S, Hansson L, Hedner T. The enigmatic association of birth weight with blood pressure. Blood Press 1997; 6: 196.
- 17. Rahiala E, Tenhola S, Vanninen E, et al. Ambulatory blood pressure in 12-year-old children born small for gestational age. Hypertension 2002; 39: 909-913.
- 18. Bavdekar A, Yajnik CS, Fall CH, et al. Insulin resistance syndrome in 8-year-old Indian children: small at birth, big at 8 years, or both? Diabetes 1999; 48: 2422-2429.





Abstract
Objectives: To study the relationship of blood pressure to birthweight and current body mass index in a population with high rates of low birthweight (< 2.5 kg).
Design: A cross-sectional population screening program conducted between 1992 and 1998, with retrospective retrieval of birthweights.
Setting: A remote coastal Australian Aboriginal community with a high prevalence of diabetes, cardiovascular and renal disease.
Participants: Eighty-two per cent of the community members (1473/1805) were screened. Birthweights were available for 767 (71%) of the screened participants aged 7–43 years.
Main outcome measures: The association between birthweight and current blood pressure, accounting for current body mass index.
Results: Mean birthweights were low, and 18% of children and 35% of adults had been low-birthweight babies. In children (7–17 years), blood pressure was not correlated with birthweight, but in adults there was an inverse correlation — a 1 kg increase in birthweight was associated with a 2.9 mmHg (95% CI, 0.3–5.5 mmHg) decrease in systolic blood pressure, after adjusting for age, sex and current weight. Overweight adults with low birthweight had the highest blood pressures.
Conclusions: Low birthweight is significantly associated with higher blood pressure in adult life, and the effect is amplified by higher current weight. Given the high rates of low birthweight in Aboriginal people in remote areas, and the detrimental effect of higher blood pressures on chronic diseases (currently present in epidemic proportions), interventions should focus on improving birthweights and on weight control in adolescents and adults. Special attention should be paid to children with low birthweight to avoid their becoming overweight in adult life.