Perceptions of adequacy of the Australian medical workforce seem to veer from predictions of surplus to warnings of shortage with a frequency that is somewhat perplexing. Australia is not alone in this, with the United Kingdom, Canada and the United States experiencing similar cycles of variation in opinion.1-3
There is, at present, concern about an impending general shortage in the medical workforce in Australia.4,5 Given the serious consequences of shortages (or oversupply), relegating medical workforce planning to the “too hard” basket is simply not an option. Australia has been at the forefront of developing medical workforce planning approaches, and the methods used continue to evolve. But this evolution is not keeping pace with system-wide developments and emerging issues. There are unprecedented changes taking place in many of the key determinants of medical workforce supply and demand in Australia. Some of these — such as the increasing number of women in the workforce, changing lifestyle expectations, and globalisation — are being identified and monitored.4,6 But other important factors are not being routinely measured. These include trends in the profile of Australian medical graduates, availability of face-to-face clinical time, attrition from the medical workforce, and supply and demand for other health professionals. In an increasingly complex environment, new workforce planning issues are emerging, such as reallocation of tasks to other health professionals and reskilling of medical practitioners for changed roles.7 These conditions create an imperative for reconsidering our approach to medical workforce planning. Here we review the key changes and issues and describe the features that are required for an effective approach to medical workforce planning.
The profile of Australian medical graduates is undergoing rapid change. A third of Australian medical school places are now for graduate-entry programs, with a corresponding increase in the proportion of older students (Box 1). In addition to having less time to spend in the medical workforce, graduate-entry-program graduates may follow different career pathways compared with graduates of traditional programs. They may be less likely to see medicine as a “career for life”,8 but we simply do not know at this stage. The number of international fee-paying students commencing medical degrees in Australian universities continues to increase (Box 1). It has traditionally been assumed in workforce planning that these students return to their home countries on completion of their training. But a significant number of these students are remaining in the Australian medical workforce, assisted by recent changes to regulations.9
The increasing amount of non-clinical work undertaken by doctors appears to be reducing the effective supply of doctors available to provide medical services. The most recent data from the national medical labour force series indicate that 7.5% of the medical workforce are employed in primarily non-clinical pursuits.10 Furthermore, many doctors in primarily clinical roles are choosing to spend a proportion of time in non-clinical work, such as research and teaching.11 Clinicians must also spend considerable time meeting requirements relating to professional accountability and continuing improvement.12 Insurance and credentialling requirements associated with clinical practice (particularly procedural work) are making part-time work more difficult financially. This is likely to affect workforce participation patterns, particularly the current pattern of gradual transition into retirement.13
Changes in the supply and demand of non-medical health professionals are an increasingly important factor in medical workforce planning. New models of care — particularly those associated with managing chronic illness — and changes in licensing and funding arrangements, as well as increased numbers of other health professionals, have changed the market for medical services. There is greater competition in the market for primary healthcare services, in particular. The latest National Health Survey indicated that 21.8% of Australians had consulted a general practitioner in the preceding fortnight and 13.1% had consulted other health professionals.14 There is evidence that the use of “alternative” medicine providers is increasing in Australia.15 The number of allied health professionals in Australia is increasing at a much greater rate than the number of medical practitioners. Between 1996 and 2001, the number of GPs increased by 10% (and specialists by 6%), while the number of allied health professionals increased by 20% (unpublished Australian Bureau of Statistics census data). Recent developments, including private insurance rebates for a range of health providers, new roles for nurses, and Medicare-sponsored access to allied health professionals, add to this changed context. At present, it is unknown how such increased access to other healthcare providers may affect the demand for medical services.
The possibility of other healthcare providers, particularly nurses, substituting for doctors in performing certain tasks is another key emerging issue. There have been a growing number of calls for consideration of substitution in Australia.4,16 There have been developments in this field to date, most notably with nurse practitioners and in rural and remote healthcare service provision, but a strategic approach to significant skill-mix changes is yet to emerge. This is looming as a major workforce planning issue for the future, and its implications should be examined in workforce models.
Another emerging issue is distribution within the medical workforce. The balance between numbers of GPs, specialists and career medical officers is beginning to come under scrutiny. The reasons for this include the introduction in 1997 of compulsory postgraduate training for general practice. Recruitment problems in general practice are occurring in the United States and the United Kingdom, and there are signs that Australia is also heading in this direction.17,18 In the United Kingdom, reskilling of medical practitioners to work in different medical specialties has been identified as an important issue.7 Monitoring of trends in career choices, exploring associated issues such as possibilities for retraining, and developing strategies in the face of insufficient interest in general practice careers to meet identified requirements will all be key future workforce planning issues.
There is anecdotal evidence that the rate of attrition from the medical workforce is increasing, due, in part, to dissatisfaction with current working conditions, particularly in general practice.5 It also seems likely that the general societal trend towards greater fluidity in career pathways is having an impact on the medical profession.8
A more effective approach to medical workforce planning needs to have three key features:
effective monitoring of all key factors affecting supply and demand;
a systems-level perspective; and
a dynamic approach.
A basic requirement for effective planning is that all key drivers of supply and demand are identified and that there is ongoing, systematic collection of good-quality data to monitor trends over time in these factors. A number of good quality data collections exist in Australia that are used in workforce planning, including health labour force surveys by the Australian Institute of Health and Welfare, Medicare provider statistics, and census data. But significant gaps remain. The key drivers of medical workforce supply and demand, together with current gaps in data collection, are outlined in Box 2. Additional problems are the failure to incorporate the available data on some factors into modelling, and a total lack of longitudinally linked data. This makes it particularly difficult to monitor flows into and out of the workforce. These problems must be addressed. In some cases, it would be relatively straightforward to create longitudinal linkages. With annual medical labour force surveys, for example, registration numbers could be used to link records between years and thus provide information on flows using existing data.
While some elements of the current Australian approach to medical workforce planning are world class, at a broad level there is fragmentation and a narrowness of scope. To date, the Australian Medical Workforce Advisory Committee has undertaken reviews of particular disciplines within the medical workforce and provided analysis of specific issues, such as overseas-trained doctors and the rural and remote workforce. But at no stage has this work been integrated into a “big picture” of the total Australian medical workforce.
A systems perspective means integrating medical workforce planning with workforce planning for other health professionals, and with workforce development, service planning and financial planning for the healthcare system. Such integration opens the door to greater scope and flexibility for developing policy responses to identified workforce issues. This, in turn, increases the buffer so that shocks to the system — sharp rises in demand or drops in supply — can be absorbed more easily without significantly affecting access to services.
While the need for integration is recognised in Australia and elsewhere, planning agencies and policymakers continue to struggle with how to put this into practice.1-3,6 The recent UK review of future requirements for health services provides some indications.19 The review first estimated requirements and then estimated both the financial and human resources needed to meet those requirements. A range of scenarios were considered, including different skill-mix configurations within the health workforce.
In Australia, there have been important steps towards developing more integrated planning. These include the establishment of the Australian Health Workforce Officials Committee and the Australian Health Workforce Advisory Committee, as well as a national review of the nursing workforce.20 Further development of integrated planning processes is required to generate new strategies to address emerging problems such as anticipated gaps in the medical workforce.
Effective workforce planning approaches must be able to account for a large number of variables simultaneously and to adjust for changes in these variables over time. This requires sophisticated, dynamic modelling.21 Like other countries, Australia has developed simulation models for projecting supply and demand.1-3,6 Current models are generally spreadsheet-based tools using the “stock and flows” method. Many now include sensitivity analyses, in which a range of scenarios are considered in addition to “base case” projections. While current models provide a good representation of many of the components of supply and demand, some gaps remain in the information base, as discussed above. Furthermore, current models do not capture the uncertainty inherent in complex systems such as health workforce supply and demand.22
In contrast to current deterministic models, stochastic models use random numbers and probabilities to reflect uncertainty.23 As such, they are ideally suited for application to systems with inherent uncertainty. They also enable the performance of “statistical experiments”, in which the impact of possible changes in key determinants is investigated using statistical analysis of the results.24 The need to undertake workforce planning in a planned, cyclic fashion is also well recognised,6 but additional resources are needed to replace ad-hoc planning activities with iterative processes.
No matter how much we improve the “technical” side of workforce planning, projecting future supply and demand for doctors will always be difficult. This is partly because of inherent uncertainties in forecasting, but also a result of the “political” side of the process. Perceptions of workforce adequacy are a product of political processes as well as analytical ones, and policy development is influenced, even more so, by politics.2,25 The success of planning is thus highly dependent on good relationships between the key players.6 The Australian Medical Workforce Advisory Committee has worked hard to develop such relationships in the area of medical workforce planning. This now needs to be extended to incorporate the key players in a system-level integrated planning approach. Without the use of more complex and integrated approaches, it will be difficult to monitor and respond to major planning issues.
1: Characteristics of students commencing medical degrees in Australia, 1989–2002*
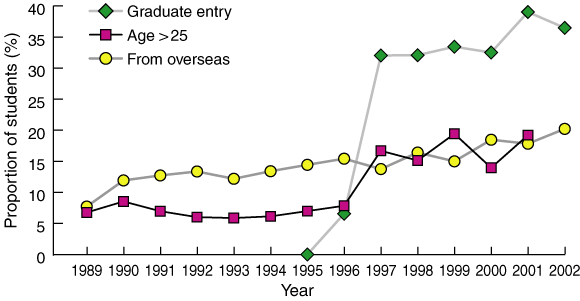
* Source: Department of Science, Education and Training, University Statistics Section, higher education data (customised dataset RFI 03/312)
2: Key influences on medical workforce supply and demand
Supply of doctors
Entries to the workforce
Graduate profile
Graduate career preferences*
Immigration (permanent and temporary)
Re-entries after temporary exit*
Doctors in practice
Demographic profile
Geographic distribution
Within-profession distribution (generalists, etc)
Lifestyle choices (working hours)
Availability/productivity of clinical time*
Exits from the workforce
Retirements*
Attrition (career change, etc)*
Emigration
Demand for doctors
Population characteristics
Service use patterns
Developments in treatment/diagnostic technology*
Community expectations*
Healthcare system infrastructure and funding models*
Supply of and demand for other health professionals
* These factors are not currently being measured (all other factors are currently being measured as part of ongoing data collections, but all are cross-sectional, with no ongoing longitudinal data collections).
- 1. Curson J. Physician workforce planning: what have we learned? Lessons for planning medical school capacity and IMG policies. Paper presented at the 7th International Medical Workforce Conference; 2003 Sep 11-14; Oxford, UK. Available at: www.healthworkforce.health.nsw.gov.au/amwac/amwac/imwcnew.html (accessed Jan 2004).
- 2. Chan B. Physician workforce planning: what have we learned? Lessons for planning medical school capacity and IMG policies: the Canadian perspective. Paper presented at the 7th International Medical Workforce Conference; 2003 Sep 11-14; Oxford, UK. Available at: www.healthworkforce.health.nsw.gov.au/amwac/amwac/imwcnew.html (accessed Jan 2004).
- 3. Salsberg E. Physician workforce planning: what have we learned? Lessons for planning medical school capacity and IMG policies: the United States experience. Paper presented at the 7th International Medical Workforce Conference; 2003 Sep 11-14; Oxford, UK. Available at: www.healthworkforce.health.nsw.gov.au/amwac/amwac/imwcnew.html (accessed Jan 2004).
- 4. Brooks PM, Lapsley HM, Butt DB. Medical workforce issues in Australia: “tomorrow’s doctors — too few, too far”. Med J Aust 2003; 179: 206-208. <MJA full text>
- 5. Access Economics. Primary health care for all Australians: an analysis of the widening gap between community need and the availability of GP services. Report to the Australian Medical Association. Canberra: Access Economics, 2002.
- 6. Gavel P. Physician workforce planning: what have we learned? An Australian perspective. Paper presented at the 7th International Medical Workforce Conference; 2003 Sep 11-14; Oxford, UK. Available at: www.healthworkforce.health.nsw.gov.au/amwac/amwac/imwcnew.html (accessed Jan 2004).
- 7. UK Department of Health. A health service of all the talents: developing the NHS workforce. Consultation document on the Review of Workforce Planning. April 2000. Available at: www.doh.gov.uk/wfprconsult (accessed Jan 2004).
- 8. Alexander JA, Ramsay JA, Thompson SM. Designing the health workforce for the 21st century. Med J Aust 2004; 180 : 7-9. <MJA full text>
- 9. Senator Kay Paterson, Minister for Health and Ageing. New measure increases medical workforce. Media release, 19 March 2003. Available at: www.health.gov.au/mediarel/yr2003/kp/kp03029.htm (accessed Aug 2003).
- 10. Australian Institute of Health and Welfare. Medical labour force 2001. Canberra: AIHW, 2003. (Catalogue No. HWL 28.)
- 11. Oransky I. Report finds shortage of US physicians by 2020. Lancet 2003; 362: 1291.
- 12. Productivity Commission. General practice administrative and compliance costs. Research report. Canberra: Productivity Commission, 2003.
- 13. Australian Institute of Health and Welfare. Medical labour force 1999. Canberra: AIHW, 2003. (Catalogue No. HWL 24.)
- 14. Australian Bureau of Statistics. National health survey. Summary of results. Canberra: ABS, 2001. (Catalogue No. 4364.0.)
- 15. MacLennan AH, Wilson DR, Taylor AW. The escalating cost and prevalence of alternative medicine. Prev Med 2002; 35: 166-173.
- 16. Brooks PM. The impact of chronic illness: partnerships with other healthcare professionals. Med J Aust 2003; 179: 260-262. <MJA full text>
- 17. Barondess JA. Specialization and the physician workforce: drivers and determinants. JAMA 2000; 284: 1299-1301.
- 18. Lambert TW, Evans J, Goldacre M. Recruitment of UK-trained doctors into general practice: findings from national cohort studies. Br J Gen Pract 2002; 52: 364-371.
- 19. Wanless D. Securing our future health: taking a long-term view. Final report. London: HM Treasury, 2002.
- 20. Senate Community Affairs Committee. The patient profession: time for action. Report on the inquiry into nursing. Canberra: SCAC, 2002.
- 21. Murphy GT, O’Brien-Pallas L. How do health human resources policies and practices inhibit change? A plan for the future. Discussion paper No. 30. Toronto, Canada: Commission on the Future of Health Care in Canada, 2002.
- 22. Plsek PE, Greenhalgh T. The challenge of complexity in health care. BMJ 2001; 323: 625-628.
- 23. Mihram GA. Simulation: statistical foundations and methodology. New York: Academic Press, 1972.
- 24. Banks J, Carson JS, Nelson BL, Nicol DM, editors. Discrete event system simulation. 3rd ed. New Jersey: Prentice Hall, 2001.
- 25. Weiner JP. Prepaid group practice staffing and US physician supply: lessons for workforce policy. Health Affairs 2004; Web exclusive W4-43. Available at: www.healthaffairs.org/WebExclusives.php (accessed Feb 2004).





Abstract
There are concerns that Australia is facing an impending shortage in the medical workforce, and there are significant changes occurring in key determinants of medical workforce supply and demand.
To date, workforce planning has not taken into account the full range of dynamic variables that are involved, nor accounted for their inherent uncertainty and complex interactions.
Future planning will require more careful monitoring and dynamic modelling within a full healthcare system perspective.