Cardiac arrest is a time-critical medical emergency, with a reported incidence in Australia of 0.72 cases per 1000 population per year.1 Rapid access to defibrillation is important, as ventricular fibrillation (VF) is a common, early cardiac arrest rhythm that responds to electric shock.2,3 However, VF deteriorates to a non-shockable rhythm with time,4 and defibrillation is rarely successful if the duration of VF extends beyond 10 min.5,6
In August 1997, Victoria’s Metropolitan Ambulance Service (MAS) had a 90th percentile response time to Code 1 emergencies (time-critical case, ambulance proceeds with lights and sirens) of 14 min.7 Similar response times have been achieved since then and, in 2005, the Code 1 90th percentile response time was 15 min (Mr Ian Patrick, Victorian MAS, October 2005, personal communication). In an attempt to reach a key performance indicator of 12 min for time-critical emergencies, the MAS introduced initiatives to reduce response times. One such initiative was the development of volunteer First Responder groups, including Hatzolah which is described here.
A first responder has been defined by the Australian Resuscitation Council as “a person competent in advanced first aid, which includes oxygen therapy and the use of an automated external defibrillator, working within a medically supervised and accountable system”.8 First responders, including firefighters and civilian groups trained and equipped with automatic defibrillators, can respond simultaneously with the MAS to cases of suspected cardiac arrest and other medical emergencies. The mean (SD) combined firefighters and ambulance response time to cardiac arrest patients has been reported as 6.0 (1.7) min and the mean time to defibrillation for patients with VF as 8.8 (2.1) min.9 Importantly, for most patients who survived (71%), response times were 6 min or less; response time was no more than 10 min for any survivors.9
Hatzolah is derived from the Hebrew word, lehatsil, meaning to save. The original Hatzolah was a First Responder agency formed by Orthodox New York Jews in 1973 to provide a service to the local community. They were trained in basic first aid and cardiopulmonary resuscitation (CPR), and were equipped with oxygen. Since then, Hatzolah First Responder groups have expanded to over 1000 units in New York State. Other Hatzolah groups have been established all over the United States and in other countries including Israel, the United Kingdom, Canada, Mexico, South Africa and Australia.10,11
Hatzolah, at its core, is a religious organisation. Under rabbinical directive, it operates according to halakhic (Jewish legal) principles. One such principle is known as pikuah nefesh, the duty to save the life of one’s fellow human being, should he or she be in mortal danger. Another is the understanding that “a person who saves one life is as if he saved a whole world” (Talmud; Tractate Sanhedrin 8: 1). As a demonstration of the religious principle of preserving or saving life on the Sabbath, the religious first responders of Hatzolah are able to drive and perform clinical duties, in compliance with the directive that “Shabbat, like all the mitzvot [commandments], is pushed aside by danger to human life” (Rambam, Zmanim 2: 1).
Hatzolah is funded entirely from private donations from within the community it serves.
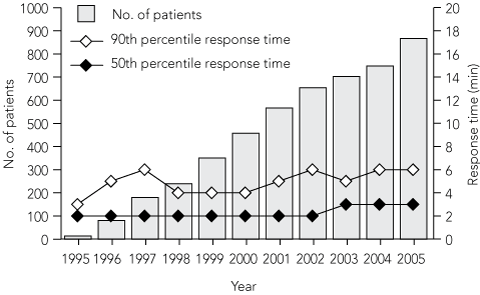
In its first 11 years of service (1995–2005, inclusive), there was a linear rise in attendances by Hatzolah — it is currently attending about 2.5 patients daily (Box 1). A large range of patient complaints are managed, although the most common are injuries related to falls, chest pain and respiratory distress (Box 2).
Hatzolah response times to all emergencies in 1995–2005 were short, with yearly median times of 3 min or less (Box 1). These times were considerably less than the MAS 2001–2002 median response time of 8 min.7 Hatzolah’s 90th percentile response times have remained stable at 5–6 min. These times are also less than the 90th percentile response times of the MAS in 2001–2002 of 13–14 min.7
As cardiac arrest is a time-critical event, a first responder’s performance in this circumstance is important. Between March 1996 and December 2004, Hatzolah attended 72 “cardiac arrest” calls, with a median response time of 2 min. Of these calls, 35 patients had true cardiac arrests and their details are described in Box 3. Overall, the Hatzolah response times to these patients were very short, and they were the first to attend the patient in 29 instances (83%). Overall, few patients (6; 17%) received bystander CPR before Hatzolah arrived. Nineteen patients (54%) were resuscitated and transported from the scene alive, and 16 patients (46%) died at the scene. These two patient groups were comparable, although significantly more patients who were transported had a shockable cardiac rhythm (VF). In total, 11 patients (31%) had VF; nine of these patients (82%) survived to be transported to hospital, and five survived (45%) to hospital discharge. These five patients represented an overall survival to hospital discharge of 14%.
In out-of-hospital cardiac arrests, the concept of “chain of survival” predicts that more people survive when a sequence of “early access to emergency medical services, basic life support, defibrillation and advanced care” occurs as rapidly as possible.4 Yet in Australia, the mean ambulance response time to cardiac arrest is 8–10 min, even in metropolitan areas.9,12 In its first 11 years of operation, Hatzolah demonstrated that it can respond to an emergency rapidly, often before the MAS. This has been important, particularly for patients with cardiac arrest, as they can initiate basic life support (CPR and defibrillation) before the availability of advanced life support.
The number of patients with cardiac arrest attended by Hatzolah is relatively small. For these patients, the rate of bystander CPR was low compared with the rates of 22% and 34% reported in Melbourne1 and international13 studies, respectively. Despite this, the rate of survival to hospital was greater than the rates of 18.1% and 12.6% reported in another Melbourne study9 and in one large prospective cohort study,14 respectively. Furthermore, the rate of survival to hospital discharge was greater than the 3.0%–7.2% reported elsewhere.9,12-14 The finding that the majority of patients with VF were resuscitated and transported is consistent with reports that VF arrests have a better survival rate that non-VF arrests.15-17
- Tony Chan1
- George Braitberg1
- Danny Elbaum2
- David McD Taylor1
- 1 Austin Health, Melbourne, VIC.
- 2 Hatzolah Melbourne, Melbourne, VIC.
None identified.
- 1. Bernard S. Outcome from prehospital cardiac arrest in Melbourne Australia. Emerg Med (Fremantle) 1998; 10: 25-29.
- 2. Cummins RO. From concept to standard of care? Review of the clinical experience with automated external defibrillators. Ann Emerg Med 1989; 18: 1269-1275.
- 3. Wassertheil J, Keane G, Fisher N, Leditschke JF. Cardiac arrest outcomes at the Melbourne Cricket Ground and Shrine of Remembrance using a tiered response strategy — a forerunner to public access defibrillation. Resuscitation 2000; 44: 97-104.
- 4. Cummins RO, Ornato JP, Thies WH, Pepe PE. Improving survival from sudden cardiac arrest: the “chain of survival” concept: a statement for health professionals from the Advanced Cardiac Life Support Subcommittee and the Emergency Cardiac Care Committee, American Heart Association. Circulation 1991; 83: 1832-1847.
- 5. Valenzuela TD, Roe DJ, Nichol G, et al. Outcomes of rapid defibrillation by security officers after cardiac arrest in casinos. N Engl J Med 2000; 343: 1206-1209.
- 6. Smith KL, Cameron PA, Peeters A, et al. Automatic external defibrillators: changing the way we manage ventricular fibrillation. Med J Aust 2000; 172: 384-388.
- 7. Melbourne Metropolitan Ambulance Service. Response times. http://www.ambulance-vic.com.au/Main-home/What-We-Do/How-were-performing/Response-times.html (accessed Jul 2006).
- 8. First Responder. Australian Resuscitation Council Guideline 11.11. February 2006. http://www.resus.org.au/public/guidelines/index.htm (accessed May 2007).
- 9. Smith KL, McNeil JJ, on behalf of the Emergency Medical Response Steering Committee. Cardiac arrests treated by ambulance paramedics and firefighters. The Emergency Medical Response Program. Med J Aust 2002; 177: 305-309. <MJA full text>
- 10. Hatzolah Kiryas Tosh [website]. http://hatzolah.com (accessed Jul 2006).
- 11. Chevra Hatzolah [website]. http://hatzolah.org.au (accessed Jul 2006).
- 12. O’Rourke MF. Surviving cardiac arrest. Med J Aust 2002; 177: 284-285. <MJA full text>
- 13. Nichol G, Steen P, Herlitz J, et al. International Resuscitation Network Registry: design, rationale and preliminary results. Resuscitation 2005; 65: 265-277.
- 14. Stiell I, Nichol G, Wells G, et al. Health-related quality of life is better for cardiac arrest survivors who receive citizen cardiopulmonary resuscitation. Circulation 2003; 108: 1939-1944.
- 15. Marenco JP, Wang PJ, Link MS, et al. Improving survival from sudden cardiac arrest: the role of the automated external defibrillator. JAMA 2001; 285: 1193-1200.
- 16. White RD, Bunch TJ, Hankins DG. Evolution of a community-wide early defibrillation programme. Experience over 13 years using police/fire personnel and paramedics as responders. Resuscitation 2005; 65: 279-283.
- 17. Herlitz J, Engdahl J, Svensson L, et al. Factors associated with an increased chance of survival among patients suffering from an out-of-hospital cardiac arrest in a national perspective in Sweden. Am Heart J 2005; 149: 61-66.







Abstract
“First responders” are people trained in advanced first aid who can respond at the same time as, and often more quickly than, ambulance services to suspected medical emergencies.
Hatzolah is a volunteer First Responder group, based on halakhic (Jewish legal) principles, in a localised area of metropolitan Melbourne with the highest density of Holocaust survivors outside Israel. Low numbers of “call-outs” to Victoria’s Metropolitan Ambulance Service (MAS) from this community suggested that many were reluctant to make contact with a “uniformed” external agency.
Hatzolah is an autonomous organisation operating under adapted MAS clinical practice guidelines and clinical governance processes. Hatzolah responders undergo an 18-month MAS training course comprising first aid, cardiopulmonary resuscitation, the use of semiautomated defibrillators, and oxygen therapy.
We describe the first 11 years (1995–2005) of the Hatzolah service. The number of patients attended to annually has risen steadily, peaking at 867 in 2005. The most frequent reasons for call-outs were falls (19.4%), chest pain (9.7%), or respiratory distress (7.6%). Hatzolah’s median response times were 2 or 3 min for all cases. They attended 35 patients with cardiac arrest (median response time, 2 min), and arrived before the MAS to 29 call-outs (83%). Nineteen patients (54%) with cardiac arrest were resuscitated and transported from the scene alive. Among those transported, significantly more had a shockable cardiac rhythm (50% v 13%, P = 0.03). Five (14%) survived to hospital discharge.
Hatzolah has evolved into an organisation providing a complementary service to the MAS. It serves as a model for the establishment of other metropolitan community First Responder groups.