Cardiovascular disease is the leading cause of death in Australia.1 Most of these deaths are unexpected and occur outside the hospital, and survival rates have been poor (< 5%).2,3 When emergency medical services arrive early, most cardiac arrest patients are found in ventricular fibrillation (VF).4
Defibrillation is the definitive treatment for VF, but is rarely successful if the duration of VF extends beyond 10 minutes.5,6 An audit of ambulance case records in Melbourne in 1995 showed that the mean ambulance response time (from processing of 000 call to ambulance arrival at scene) to cardiac arrest patients was 9.4 minutes (Box 1).3 When additional delays were factored into the response, such as delays in dialling 000, more than half the patients were defibrillated more than 10 minutes after the onset of VF.
To reduce emergency service response times and time to defibrillation for cardiac arrest patients, the Emergency Medical Response (EMR) pilot program was established in Melbourne in 1998. The simultaneous dispatch of fire fighters (trained in cardiopulmonary resuscitation [CPR] and equipped with automatic external defibrillators) and ambulance paramedics to suspected cases of cardiac arrest significantly reduced response times (Box 1).7 Based on results from the pilot program, in February 2000 the Victorian Government expanded the program across all of metropolitan Melbourne serviced by the Fire Brigade. This article describes the first year of the expanded program.
Ethics approval for data collection and analysis was obtained from the Monash University Standing Committee on Ethics in Research Involving Humans.
The Metropolitan Fire and Emergency Services Board (MFESB) is an urban fire service staffed by professional fire fighters. All 47 fire stations (with 58 fire trucks staffed by personnel trained for the EMR program) were involved in the expanded program, and 1337 (91%) fire fighters were trained to be first-responders, with training continuing throughout 2001. The MFESB services an area of about 1096 km2 with a population of about 2 million people (Box 2).
Fire fighters were trained and equipped to respond to ambulance events and provide basic life support, including the use of a shock advisory defibrillator (which recommends when a shock is required), until the ambulance service arrived (Box 3). Training comprised an eight-day course, which provided three-year certification. In addition, ambulance paramedics provided continuing education in critical skill areas through regular (programmed) visits to fire stations.
Between 7: 00 and 22:30, the Metropolitan Ambulance Service has 68 ambulances responding each day, each staffed by two paramedics trained to perform CPR and defibrillation for VF or pulseless ventricular tachycardia. At other times there are 49 ambulances responding. Additionally, there are 17 mobile intensive care ambulances, each staffed by two paramedics trained to perform defibrillation and advanced life support, including intravenous administration of vasoactive and antiarrhythmic drugs and tracheal intubation. Ambulance treatment protocols for cardiac arrest patients are based on published national recommendations and involve the administration of CPR and advanced life support drugs, plus defibrillation when the rhythm is VF or ventricular tachycardia.8 Ambulance paramedics do not initiate resuscitation when patients are in asystole or pulseless electrical activity and there is clear evidence of prolonged cardiac arrest, or if a local medical officer instructs them not to resuscitate.
Both ambulances and fire trucks are dispatched from a central communications centre, which responds to an emergency phone number of 000 for metropolitan Melbourne via a computerised protocol-based dispatch system. The highest medical emergencies are those where the subject is suspected to be unconscious or non-breathing. When the dispatcher identifies a high priority event, the closest available ambulance, mobile intensive care ambulances and fire engine are dispatched simultaneously.
The overriding responsibility of patient care lies with the mobile intensive care ambulance paramedics. If fire fighters arrive first, patient care is handed over to ambulance paramedics as soon as the first ambulance arrives. In addition, if an ambulance arrives at the patient first, they can "call-off" the dispatched fire fighters.
Results of the first 12 months of the EMR program are summarised in Box 4 and Box 5.
In the controlled EMR study,7 mean time to defibrillation was reduced from 10.1 to 8.6 minutes, and this was maintained in the expanded EMR program (8.75 minutes). Although this is an improvement, defibrillation should ideally be achieved within six minutes of receipt of call, because after this the probability of survival decreases sharply.9
To significantly increase survival rates a community approach is needed. Since 1991, the American Heart Association has promoted the concept of the "chain of survival" to explain the systematic changes necessary for successful resuscitation of victims of cardiac arrest.10 The elements of this are early access to emergency care, early cardiopulmonary resuscitation, early defibrillation, and early advanced cardiac life support.
Early access: Witnesses to a cardiac arrest are often agitated and do not immediately call for the emergency medical service. One study of cardiac arrests in western Melbourne found that 20% of bystanders called a local medical officer or relative first.3 Consideration of ways to increase public awareness of the need to call 000 immediately for cardiac arrest patients would be valuable.
Early cardiopulmonary resuscitation: Forty-seven per cent of witnessed arrests received CPR from a bystander during this program. However, the quality of CPR and how quickly it was initiated are unknown and will require further research. Earlier effective CPR might improve the low survival rate in Melbourne.5,11 The Victorian Government is currently offering free CPR lessons to the public through the "Key to Survival" program. In time we will be able to see if this initiative increases bystander CPR participation rates.
Early defibrillation: In addition to the MFESB, other professional groups may warrant consideration as first responders to cardiac arrests.12 The concept of public-access defibrillation, where defibrillators are placed in public buildings/sites, also needs to be explored through studies which map the location of arrest from VF.13
Early advanced cardiac life support: Even with the introduction of rapid defibrillation, a significant group of patients will rely on the ambulance to provide advanced cardiac life support.14 The Metropolitan Ambulance Service has implemented a program in which all ambulance paramedics will eventually be trained in the use of the laryngeal mask airway device and the administration of intravenous adrenalin. This initiative should improve the efficiency of defibrillation in borderline cases.
Resuscitation was not initiated by the EMR in more than 50% of cardiac arrest patients because of evidence of prolonged cardiac arrest, raising the issue of the specificity of current dispatch criteria. This will be assessed in the future through the Victorian Ambulance Cardiac Arrest Registry, which captures data on all cardiac arrest patients attended by ambulance in Victoria.
An important future analysis will involve the cost-effectiveness of the EMR program. Currently, the number of VF patients is too small to assess this. However, most of the cost was in the start-up of the program, the training and in a wage increase for fire fighters, which was implemented as part of an industrial agreement.
As the number of VF patients is small, maintaining confidence among fire fighters is one of the challenges. In addition, the EMR program has expanded the role and activities required of them. However, results from a study using focus groups and a questionnaire suggest that the fire fighters have adapted well to their new role and view their skills as an important addition to their current expertise.15 Fire fighter motivation and skills have been maintained through regular in-station training sessions and the dissemination of information through newsletters and an in-house television channel.
The current program has been successful in maintaining reduced response times to cardiac arrest patients in Melbourne. Further research is needed to better establish the effect of the program on long-term survival and quality of life. Investigations of other strategies to deploy automatic external defibrillators are also an important priority.
1: The Emergency Medical Response (EMR) program: history and early results
In 1995, an observational study of out-of-hospital cardiac arrest in western Melbourne indicated that ambulance response times required improvement and that survival was poor. During a six-month audit, ambulance paramedics attended 361 patients assumed to have a primary cardiac event, of which 113 (31%) were initially in ventricular fibrillation (VF). Only 3% of all patients and 9% of VF patients survived to discharge from hospital. The average time from receipt of call to arrival of ambulance at the scene was 9.4 (SD, 3.6) minutes.3 In July 1998, a prospective controlled trial began in Melbourne. Fire fighters trained in cardiopulmonary resuscitation and equipped with automatic external defibrillators were added as an extra tier to the existing two-tiered ambulance response. The trial consisted of a control area (277 km2 ambulance dispatch only) and a pilot area (171 km2 simultaneous ambulance and fire dispatch). |
At 12 months, the mean EMR response time to cardiac arrests was reduced by 1.6 (95% CI, 1.2–2.0) minutes, from 7.5 minutes in the control area to 5.9 minutes in the pilot area. Mean time to defibrillation for patients whose initial recorded rhythm was VF was reduced by 1.5 (95% CI, 0.1–3.0) minutes, from 10.1 minutes in the control area to 8.6 minutes in the pilot area. Survival for patients who were in VF on arrival of the EMR was 29% in the pilot area and 18% in the control area (P = 0.368). Survival for patients whose cardiac arrest was witnessed by a bystander and who were in VF on arrival of the EMR was 36% in the pilot area and 23% in the control area (P = 0.363).7 In February 2000, the simultaneous dispatch of fire vehicles with ambulances was expanded across all of Melbourne serviced by the Metropolitan Fire Brigade (about 2 million population; see Box 2). |
||||||||||
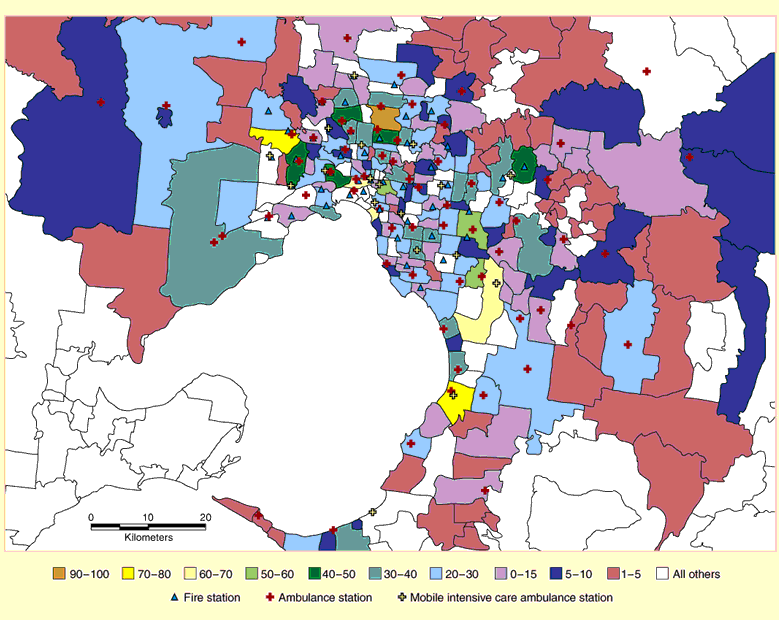
2: Map of the Melbourne metropolitan area included in the expanded Emergency Medical Response program, and the number of high priority events, by postcode per year
3: Fire fighters in the Emergency Medical Response program

Fire fighters trained in cardiopulmonary resuscitation and equipped with automatic external defibrillators are dispatched to suspected cardiac arrests simultaneously with ambulances.
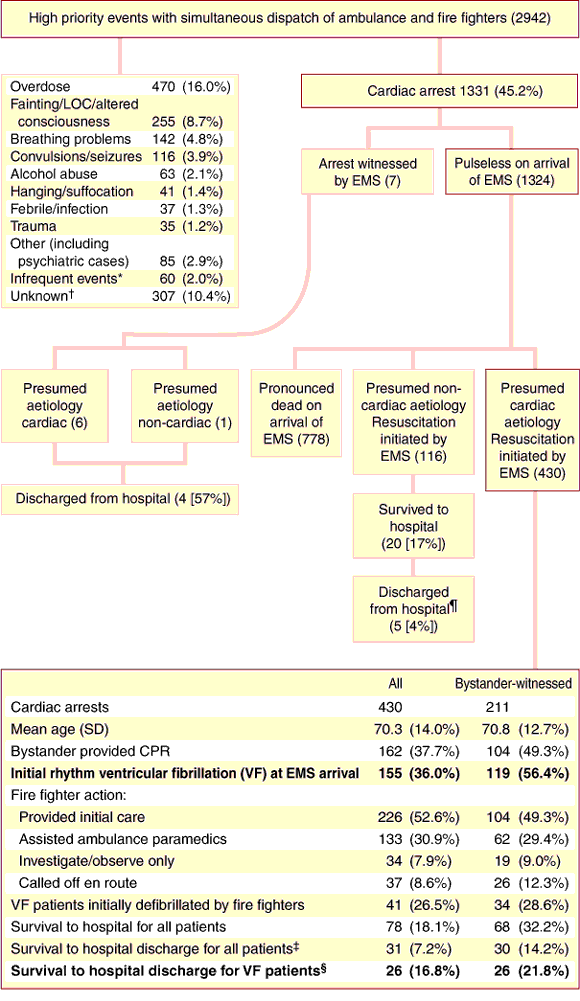
4: Results of the first 12 months of the Emergency Medical Response (EMR) program
Patient survival
2942 high priority events (see Box 5 for diagnoses)
Fire fighters provided initial care at 770 (26%) of these events, and assisted ambulance paramedics at a further 10% of the events.
The most common form of care provided by fire fighters was administering oxygen (34%).
Resuscitation was initiated in 430 patients with cardiac arrest of presumed cardiac aetiology, of whom 155 were in ventricular fibrillation (VF).
Fire fighters provided initial defibrillation to 41 (26.5%) of these patients, and to one patient who presented with a non-shockable rhythm but reverted to VF during treatment.
31 (7.3%) cardiac arrest patients for whom the EMR initiated resuscitation survived to hospital discharge.
Fire fighters provided initial care to 13 (42%) of the survivors, and assisted paramedics in treatment of 8 (26%) other survivors.
For most patients who survived (71%), response time was 6 min or less. Response time was not more than 10 min for any survivors.
Of 74 VF patients initially treated by fire fighters, 10 (14%) survived to hospital discharge, compared with 16 (21%) of 77 VF patients initially treated by paramedics (P = 0.237).
Survival to hospital discharge for witnessed VF arrests was 21.8%.
Response times
The mean EMR response time to cardiac arrest patients (from processing of 000 call to arrival of EMR) was 6 min (see Table), similar to that achieved in the pilot program.
45% of patients were in ventricular fibrillation (VF) when response time was ≤ 2 min, compared with 8% in VF when response time was ≥ 10 min. No patients were in VF when response time was > 14 min.
The mean time to defibrillation for patients in VF was 8.75 minutes (SD, 2.07 minutes).
Response time (minutes) |
|||||||||||
Mean (95% CI) |
Median (95% CI) |
90th percentile (95% CI) |
|||||||||
Combined ambulance and fire fighters |
6.0 (5.9–6.1) |
6.0 (5.9–6.1) |
8.0 (7.8–8.2) |
||||||||
First ambulance on scene |
7.1 (7.0–7.3) |
7.0 (6.8–7.2) |
10.0 (9.8–10.2) |
||||||||
Mobile intensive care ambulance |
8.7 (8.5–9.0) |
8.0 (7.7–8.3) |
13.0 (12.6–13.4) |
||||||||
Fire fighters |
6.8 (6.6–7.0) |
6.0 (5.8–6.2) |
9.0 (8.8–9.2) |
||||||||
- Karen L Smith1
- John J McNeil2
- on behalf of the Emergency Medical Response Steering Committee
- Department of Epidemiology and Preventive Medicine, Monash Medical School, Monash University, Melbourne, VIC.
The data collection and analysis of the EMR program was funded by the Department of Human Services (DHS), Victoria. Karen Smith is supported by a fellowship from the National Health and Medical Research Council. The Emergency Medical Response Steering Committee consists of Professor John McNeil, Mr Greg Sassella (Metropolitan Ambulance Service), Mr Peter Akers (MFESB), Mr Bruce Esplin (Department of Justice, VIC), Mr Trevor Sutherland (DHS), Mr Alan Richards (MFESB) and Mr Michael Morton (DHS). The authors would like to acknowledge Mr Greg Young (Metropolitan Ambulance Service) for his assistance with the map of the EMR area.
None identified.
- 1. Australian Institute for Health and Welfare. Heart, stroke and vascular diseases: Australian facts 2001. Canberra: AIHW, National Heart Foundation of Australia, and National Stroke Foundation of Australia, 2001. (Report no. CVD 14.)
- 2. Meyer ADM, Cameron PA, Smith KL, et al. Out-of-hospital cardiac arrest. Med J Aust 2000; 172: 73-76.
- 3. Bernard S. Outcome from prehospital cardiac arrest in Melbourne, Australia. Emerg Med 1998; 10: 25-29.
- 4. Eisenberg MS, Horwood BT, Cummins RO, et al. Cardiac arrest and resuscitation: a tale of 29 cities. Ann Emerg Med 1990; 19: 179-186.
- 5. Valenzuela TD, Roe DJ, Cretin S, et al. Estimating effectiveness of cardiac arrest interventions. A logistic regression survival model. Circulation 1997; 96: 3308-3313.
- 6. Smith KL, Cameron PA, Peeters A, et al. Automatic external defibrillators: changing the way we manage ventricular fibrillation. Med J Aust 2000; 172: 384-388.
- 7. Smith KL, Peeters A, McNeil JJ. Results from the first twelve months of a fire first-responder program in Australia. Resuscitation 2001; 49: 143-150.
- 8. The Advanced Life Support Committee of the Australian Resuscitation Council. Adult Advanced Life Support. Med J Aust 1993; 159: 616-621.
- 9. Nichol G, Stiell IG, Laupacis A, et al. A cumulative meta-analysis of the effectiveness of defibrillator-capable emergency medical services for victims of out-of-hospital cardiac arrest. Ann Emerg Med 1999; 34: 517-525.
- 10. Cummins RO, Ornato JP, Thies WH, et al. Improving survival from sudden cardiac arrest: the "chain of survival" concept. A statement for health professionals from the Advanced Cardiac Life Support Subcommittee and the Emergency Cardiac Care Committee, American Heart Association. Circulation 1991; 83: 1832-1847.
- 11. Gallagher EJ, Lombardi G, Gennis P. Effectiveness of bystander cardiopulmonary resuscitation and survival following out-of-hospital cardiac arrest. JAMA 1995; 274: 1922-1925.
- 12. White RD, Asplin BR, Bugliosi TF, et al. High discharge survival rate after out-of-hospital ventricular fibrillation with rapid defibrillation by police and paramedics. Ann Emerg Med 1996; 28: 480-485.
- 13. Becker L, Eisenberg M, Fahrenbruch C, et al. Public locations of cardiac arrest. Implications for public access defibrillation. Circulation 1998; 97: 2106-2109.
- 14. Mann CJ, Guly H. Paramedic interventions increase the rate of return of spontaneous circulation in out of hospital cardiac arrests. Accid Emerg Med 1997; 14: 149-150.
- 15. Smith KL, Rich D, Pastoriza Pinol J, et al. Acceptance of a medical first-responder role by fire fighters. Resuscitation 2001; 51: 33-38.






Abstract
The Emergency Medical Response (EMR) program is a Victorian Government initiative in which fire fighters trained in cardiopulmonary resuscitation and equipped with automatic external defibrillators are dispatched to suspected cardiac arrests simultaneously with ambulance paramedics across metropolitan Melbourne.
During the first 12 months (February 2000 to February 2001) of the expanded EMR program, 2942 events involved simultaneous dispatch of ambulance paramedics and fire fighters.
In 430 events, patients had suffered a cardiac arrest of presumed cardiac cause, and resuscitation was attempted by the emergency medical services.
Fire fighters provided the initial defibrillation to 41 (26.5%) patients presenting in ventricular fibrillation.
Survival to hospital discharge for bystander-witnessed ventricular fibrillation cardiac arrests was 21.8%.
The mean emergency services (fire and ambulance) response time to cardiac arrest patients was 6.03 (SD, 1.65) minutes.
The mean time to defibrillation for ventricular fibrillation patients was 8.75 (SD, 2.07) minutes.