The mortality rates for heart disease outside Australian capital cities are 30% higher in men and 21% higher in women than rates in the cities, and the average life expectancy for rural residents is about 1 year less than for their metropolitan counterparts.1,2
Several causes for these mortality differences have been suggested, including older age distribution, higher proportions of Indigenous people, and decreased socioeconomic status.3 Decreased access to immediate emergency medical care might also be partly responsible.
Many deaths from heart disease occur outside the hospital and present as sudden cardiac arrest (SCA). The reported survival rates for out-of-hospital SCA in Australia vary from 3% to 71%,4-13 but few studies have specifically examined whether there are differences in outcomes between urban and rural cardiac arrests.
Victoria has an area of 227 000 square kilometres and a population of 4.6 million, of whom most (3.0 million) live in the capital city, Melbourne.14 The ambulance service in Victoria comprises Rural Ambulance Victoria (RAV) and the Metropolitan Ambulance Service (MAS). Both RAV and MAS use a two-tier system of ambulance paramedics, most of whom have some advanced life support skills (laryngeal mask airway, intravenous adrenaline), and intensive care paramedics, who are authorised to perform endotracheal intubation and administer a range of cardiac drugs. The cardiac arrest protocols follow the recommendations of the Australian Resuscitation Council.15,16
There are operational differences between MAS and RAV. MAS uses computerised dispatching (Advanced Medical Priority Dispatch System, Priority Dispatch Corporation, Salt Lake City, Utah, USA) and RAV uses a manual call-taking and dispatch system. In addition, MAS and the Metropolitan Fire and Emergency Services Board operate a joint emergency medical response first-response program.17 Finally, MAS dispatches intensive care paramedics to all suspected cardiac arrests, whereas this level of skill is variably available in RAV.
We analysed data from the VACAR complying with the Utstein methods of reporting18 for adults (> 17 years), in cardiac arrest on arrival of the emergency medical service (EMS), with collapse witnessed by a bystander, and with cardiac arrest of presumed cardiac cause. The dataset included variables considered to be associated with outcome, including EMS response time, the application of bystander cardiopulmonary resuscitation (CPR), EMS interventions (including the insertion of an endotracheal tube), return of spontaneous circulation (presence of a pulse for > 30 seconds after EMS arrival), arrival at the emergency department with a palpable pulse, and survival to hospital discharge.
The patients were defined as urban or rural based on the Australian Bureau of Statistics Australian Standard Geographical Classification (ABS-ASGC). Case locality assignment was undertaken using geospatial information system software (MapInfo Professional, version 7.5, MapInfo Corporation, Sydney, NSW), and ABS-ASGC Urban Centre/Locality Structure boundaries were applied using ABS-ASGC datasets.19
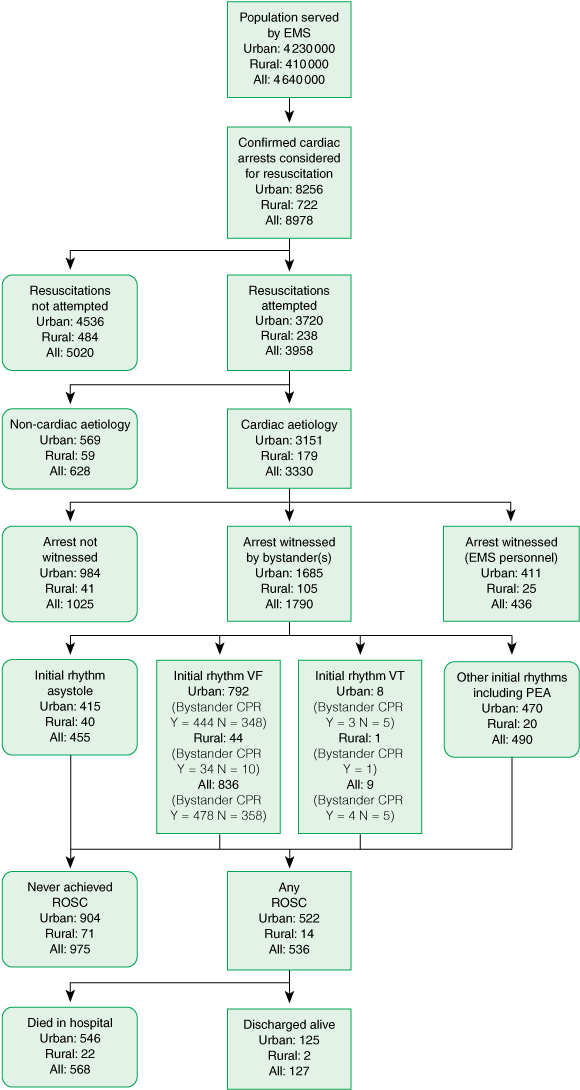
During the 24 months, RAV and MAS attended 8978 cardiac arrests (Box 1). The overall rate of cardiac arrest was 147.8/100 000 persons per year (rural, 119.1/100 000 persons per year; urban, 149.3/100 000 persons per year). The disparity between urban and rural rates may be due to an ambulance not being called in the more rural or remote settings.
Of the 8978 cardiac arrests, resuscitation was commenced in 3958 (44%). Of these, 3330 (37%) were of presumed cardiac aetiology. Other causes are summarised in Box 2.
There were 1790 (20%) bystander-witnessed cardiac arrests. The median age for men was 69 years (IQR, 58–77 years) and for women was 74 years (IQR, 65–82 years). Demographic characteristics for these patients are summarised in Box 3. There was a significant difference in the rate of bystander-initiated CPR between urban and rural localities (urban, 48.4% [95% CI, 46.0%–50.8%]; rural, 65.7% [95% CI, 56.5%–74.9%]). The urban group were significantly older (P = 0.025). Patients in the urban group were more likely than those in rural areas to have an endotracheal tube inserted as part of their management (P < 0.001).
The initial cardiac rhythm was ventricular fibrillation in 46.8% of patients on arrival of ambulance (Box 3). This rhythm was more common in urban areas than in rural areas (urban, 47.1%; 95% CI, 44.9%–49.6%; rural, 42.0%; 95% CI, 32.6%–52.0%). Ventricular tachycardia was very rare as the presenting cardiac rhythm.
Because of the small numbers of survivors to hospital discharge, the analysis of baseline variables in a logistic regression model used survival to hospital as the dependent variable rather than hospital discharge. Regression analysis identified a number of factors associated with survival to hospital (Box 4 and Box 5). Independent factors associated with survival were distance to ambulance station, sex, endotracheal tube insertion, and presenting rhythm.
Patients in rural areas may have been expected to have worse outcomes because of longer times between collapse and defibrillation, but few studies have specifically examined the locality of the SCA, or compared rural and urban arrests. In one study, the overall survival rate to hospital was 13.9% (110/793), and survival rates were 9% in rural areas, 14% in suburban areas, and 23% in urban areas.20 On the other hand, a study of 137 SCA patients found no difference in survival to hospital when patients were grouped by “city arrest” (10 survivors) or “country arrest” (12 survivors) (P = 1.0) or hospital discharge (3 survivors each group; P = 1.0), although that study had small patient numbers.21 A third study of 1956 patients with SCA in Scotland compared survival rates in different postcode districts with different ambulance response times.22 Survival to hospital admission was greater in areas where the median response time was less than 10 minutes (13.5% v 8.1%; P < 0.05). There was greater survival to discharge in these areas, but this was not significant (4.1% v 3.2%; P = 0.42). There was also a close correlation between distance travelled and response time (P < 0.01).
Improving outcomes following cardiac arrest in rural areas requires improvements in each link of the “chain of survival”.23 The first link is the call to the ambulance. In rural areas in Victoria, manual call-taking and dispatching is used, and this might be associated with delays or inaccuracy in dispatch time recording. Computerised dispatching may improve ambulance responses to cardiac arrest. One study comparing computerised dispatch with standard call-taking procedures found a doubling in the number of cardiac arrests correctly identified compared with a non-computerised system.24 It would be expected that a case identified as suspected cardiac arrest at dispatch would have a faster ambulance response and concurrent allocation of intensive care paramedic support.
The third link in the chain of survival is early defibrillation. This usually depends on ambulance response time. In rural areas, there was a mean response time of 14 minutes, compared with 8 minutes in urban areas. Decreasing ambulance response times by several minutes across a large, sparsely populated area would be very costly, and more cost-effective means of delivering rapid defibrillation need to be considered. For example, in the urban areas serviced by MAS, firefighters also respond to cardiac arrests.17,25 Because of the inner-urban location of this program, there was a minimal difference in the response times of firefighters compared with EMS, and only a small effect on survival rate.17 However, a firefighter or police first-responder program implemented where ambulance response times are longer may have a more beneficial effect.26
For cardiac arrests outside the home, public access defibrillation programs reduce the time to defibrillation and increase survival.27 We found that cardiac arrest outside the home was more frequent among the rural group (46.4%) than among the urban patients (33%). However, one study found that few rural places have sufficient SCAs to justify placement of defibrillators for public use.28 Alternatively, defibrillators could be placed in the homes of patients at high risk of SCA; this strategy is currently under investigation.29
Finally, the use of advanced cardiac life support (defined as endotracheal intubation and intravenous adrenaline) by paramedics may increase the number of patients who are transported alive to hospital, although this may not result in improved survival to hospital discharge. We found those who were intubated had a significantly higher chance of surviving to hospital than those who were not (adjusted OR, 3.46; 95% CI, 2.49–4.80; P < 0.001). One study examined the effect of the introduction of advanced cardiac life support for SCA patients in 17 cities in Ontario, Canada.30 The researchers enrolled 5638 patients, and the rate of survival to hospital after SCA improved significantly (from 10.9% before introduction of advanced cardiac life support to 14.6% after; P < 0.001). However, the rate of survival to hospital discharge was not changed (before, 5.0%; after, 5.1%; P = 0.83). On the other hand, in a study that examined timing of endotracheal intubation and outcome,31 survival was 46% for patients with SCA who were intubated in less than 12 minutes, compared with 23% for patients intubated after 12 minutes. The adjusted odds ratio of survival for the late intubation group compared with the early intubation group was 0.42 (95% CI, 0.26–0.69). These results indicate there may be a benefit in the widespread training of ambulance paramedics in endotracheal intubation of SCA patients in rural areas, and this warrants further research.
There may be subtle but important differences in ambulance management in urban compared with rural areas that we were unable to measure. For example, there are fewer (usually two) ambulance staff at a rural cardiac arrest, compared with urban cardiac arrests (generally four, plus firefighters), which limits the number of interventions that can be performed concurrently. One strategy to address this issue is the introduction of a portable machine that performs external chest compression (eg, Autopulse Resuscitation System, Zoll Medical Australia Pty Ltd, Lane Cove, NSW). This device may allow the ambulance staff to focus on defibrillation and advanced life-support measures. This machine has been used by the San Francisco ambulance service.32 When applied in SCA patients after a mean (SD) response time of 15 (5) minutes, more patients arrived with a pulse at hospital when Autopulse had been used (39%) compared with manual CPR (29%) (P = 0.003). However, the article did not report differences in outcomes at hospital discharge.
1 Adapted Utstein templates for out-of-hospital cardiac arrests in Victoria from January 2002 to December 2003
3 Demographic characteristics of people who suffered bystander-witnessed cardiac arrests of cardiac aetiology over a 2-year period
* Mann–Whitney U test. CPR = cardiopulmonary resuscitation. IQR = interquartile range. |
|||||||||||||||
Received 22 December 2005, accepted 1 May 2006
- Paul A Jennings1
- Peter Cameron2
- Tony Walker1
- Stephen Bernard3,2
- Karen Smith3
- 1 Rural Ambulance Victoria, Geelong, VIC.
- 2 Department of Epidemiology and Preventive Medicine, Monash University, Melbourne, VIC.
- 3 Metropolitan Ambulance Service, Melbourne, VIC.
We would like to thank the following for their contribution to this study: Jason Muller, Geospatial Information System analyst, RAV, for coding geographical data and developing maps; Vanessa Barnes, Research Officer, Victorian Ambulance Cardiac Arrest Registry, for assisting with data acquisition; and Michael Bailey, for statistical assistance.
None identified.
- 1. Sexton PT, Sexton T-LH. Excess coronary mortality among Australian men and women living outside the capital city statistical divisions. Med J Aust 2000; 172: 370-374. <MJA full text>
- 2. Voss T, Begg S. The Victorian burden of disease study. Melbourne: Victorian Government Department of Human Services, 1999.
- 3. Hayes LJ, Quine S, Taylor R. New South Wales trends in mortality differentials between small rural and urban communities over a 25-year period, 1970–1994. Aust J Rural Health 2005; 13: 71-76.
- 4. Bernard S. Outcome from prehospital cardiac arrest in Melbourne, Australia. Emerg Med 1998; 10: 25-29.
- 5. Bett JH. Experience with a mobile coronary care unit in Brisbane. Ann Emerg Med 1989; 18: 969-974.
- 6. Brennan RJ, Luke C. Failed prehospital resuscitation following out-of-hospital cardiac arrest: are further efforts in the emergency department warranted? Emerg Med 1995; 7: 131-138.
- 7. Finn JC, Jacobs IG, Holman CD, Oxer HF. Outcomes of out-of-hospital cardiac arrest patients in Perth, Western Australia, 1996–1999. Resuscitation 2001; 51: 247-255.
- 8. Jackson T, Cameron P. Prehospital defibrillation in Geelong. Emerg Med 1993; 5: 184-187.
- 9. Jacobs IG, Oxer HF. A review of pre-hospital defibrillation by ambulance officers in Perth, Western Australia. Med J Aust 1990; 153: 662-664.
- 10. Jennings P, Pasco J. Survival from out-of-hospital cardiac arrest in the Geelong region of Victoria, Australia. Emerg Med (Fremantle) 2001; 13: 319-325.
- 11. Sammel NL, Taylor K, Selig M, O’Rourke MF. New South Wales intensive care ambulance system. Med J Aust 1981; 2: 546-550.
- 12. Scott IA, Fitzgerald GJ. Early defibrillation in out-of-hospital sudden cardiac death: an Australian experience. Arch Emerg Med 1993; 10: 1-7.
- 13. Wassertheil J, Keane G, Fisher N, Leditschke JF. Cardiac arrest outcomes at the Melbourne Cricket Ground and Shrine of Remembrance using a tiered response strategy — a forerunner to public access defibrillation. Resuscitation 2000; 44: 97-104.
- 14. Australian Institute of Health and Welfare. Rural, regional and remote health: a study on mortality. Rural Health Series No. 2. Canberra: AIHW, 2003. (AIHW Cat. No. PHE45.)
- 15. Rural Ambulance Victoria, Metropolitan Ambulance Service. Clinical practice guidelines. http://www.rav.vic.gov.au/CPGindex.asp (accessed Dec 2005).
- 16. Australian Resuscitation Council. Guidelines. http://www.resus.org.au (accessed Apr 2006).
- 17. Smith KL, McNeill JJ; Emergency Medical Response Steering Committee. Cardiac arrests treated by ambulance paramedics and fire fighters. Med J Aust 2002; 177: 305-309. <MJA full text>
- 18. Cummins RO, Chamberlain DA, Abramson NS, et al. Recommended guidelines for uniform reporting of data from out-of-hospital cardiac arrest: the Utstein style. A statement for health professionals from a task force of the American Heart Association, the European Resuscitation Council, the Heart and Stroke Foundation of Canada, and the Australian Resuscitation Council. Circulation 1991; 84: 960-975.
- 19. Australian Bureau of Statistics. Australian Standard Geographical Classification (ASGC), 2001. Canberra: ABS, 2001. (ABS Cat. No. 1216.0.)
- 20. Vukmir RB. The influence of urban, suburban, or rural locale on survival from refractory prehospital cardiac arrest. Am J Emerg Med 2004; 22: 90-93.
- 21. Layon AJ, Gabrielli A, Goldfeder BW, et al. Utstein style of rural out-of-hospital cardiac arrest [OOHCA]: total cardiopulmonary resuscitation (CPR) time inversely correlates with hospital discharge rate. Resuscitation 2003; 56: 59-66.
- 22. Lyon RM, Cobbe SM, Bradley JM, Grubb NR. Surviving out of hospital cardiac arrest at home: a postcode lottery? Emerg Med J 2004; 21: 619-624.
- 23. Langhelle A, Nolan J, Herlitz J, et al. Recommended guidelines for reviewing, reporting, and conducting research on post-resuscitation care: the Utstein style. Resuscitation 2005; 66: 271-283.
- 24. Heward A, Damiani M, Hartley-Sharpe C. Does the use of the Advanced Medical Priority Dispatch System affect cardiac arrest detection? Emerg Med J 2004; 21: 115-118.
- 25. Smith KL, Peeters A, McNeil JJ. Results from the first 12 months of a fire first-responder program in Australia. Resuscitation 2001; 49: 143-150.
- 26. White RD, Bunch TJ, Hankins DG. Evolution of a community-wide early defibrillation programme experience over 13 years using police/fire personnel and paramedics as responders. Resuscitation 2005; 65: 279-283.
- 27. Hallstrom AP, Ornato JP, Weisfeldt M, et al. Public-access defibrillation and survival after out-of-hospital cardiac arrest. N Engl J Med 2004; 351: 637-646.
- 28. Portner ME, Pollack ML, Schirk SK, Schlenker MK. Out-of-hospital cardiac arrest locations in a rural community: where should we place AEDs? Prehospital Disaster Med 2004; 19: 352-355.
- 29. Seattle Institute for Cardiac Research. The Home AED Trial (HAT). http://www.sicr.org/hatmain.html (accessed May 2006).
- 30. Stiell IG, Wells GA, Field B, et al. Advanced cardiac life support in out-of-hospital cardiac arrest. N Engl J Med 2004; 351: 647-656.
- 31. Shy BD, Rea TD, Becker LJ, Eisenberg MS. Time to intubation and survival in prehospital cardiac arrest. Prehosp Emerg Care 2004; 8: 394-399.
- 32. Casner M, Anderson D, Isaacs SM. The impact of a new CPR assist device on rate of return of spontaneous circulation in out-of-hospital cardiac arrest. Prehosp Emerg Care 2005; 9: 61-67.





Abstract
Objective: To compare the survival rate from out-of-hospital cardiac arrest in rural and urban areas of Victoria, and to investigate the factors associated with these differences.
Design: Retrospective case series using data from the Victorian Ambulance Cardiac Arrest Registry.
Setting: All out-of-hospital cardiac arrests occurring in Victoria that were attended by Rural Ambulance Victoria or the Metropolitan Ambulance Service.
Participants: 1790 people who suffered a bystander-witnessed cardiac arrest between January 2002 and December 2003.
Results: Bystander cardiopulmonary resuscitation was more likely in rural (65.7%) than urban areas (48.4%) (P = 0.001). Urban patients with bystander-witnessed cardiac arrest were more likely to arrive at an emergency department with a cardiac output (odds ratio [OR], 2.92; 95% CI, 1.65–5.17; P < 0.001), and to be discharged from hospital alive than rural patients (urban, 125/1685 [7.4%]; rural, 2/105 [1.9%]; OR, 4.13; 95% CI, 1.09–34.91). Major factors associated with survival to hospital admission were distance of cardiac arrest from the closest ambulance branch (OR, 0.87; 95% CI, 0.82–0.92), endotracheal intubation (OR, 3.46; 95% CI, 2.49–4.80), and the presence of asystole (OR, 0.50; 95% CI, 0.38–0.67) or pulseless electrical activity (OR, 0.73; 95% CI, 0.56–0.95) on arrival of the first ambulance crew.
Conclusions: Survival rates differ between urban and rural cardiac arrest patients. This is largely due to a difference in ambulance response time. As it is impractical to substantially decrease response times in rural areas, other strategies that may improve outcome after cardiac arrest require investigation.