Overcrowding causes dysfunction in the emergency department (ED): it is associated with longer waiting times,1 increased delays in admission to hospital,2 and even with transmission of infectious disease (during the outbreak of severe acute respiratory disease [SARS] in Canada).3 Delays in transfer to an inpatient bed from the ED are associated with increased inpatient length of stay,4,5 but there have been few studies of the relationship between ED overcrowding and patient outcomes. An understanding of the human cost of overcrowding is important to guide appropriate distribution of health care resources.
A recent study to validate a measure of ED overcrowding based on the number of patients receiving treatment (“occupancy”)6 noted a trend (P = 0.08) towards increased inpatient mortality at 10 days in patients presenting at times of ED overcrowding. This prompted further study, which is reported here, with the aim of quantifying any such relationship.
Of the possible definitions of ED overcrowding, the simplest and least subjective is occupancy with patients under treatment. Occupancy is included in all of the validated overcrowding measures in common use.7 The 75th centile of occupancy for the time of day has been previously suggested as an overcrowding threshold for our hospital, based on an association with waiting times.8
Long-term trends: ED occupancy has increased over time due to access block (delay in obtaining inpatient beds), and mortality might be expected to increase because of the ageing population.
Seasonal: Both ED occupancy and mortality rates increase in winter.
Day of the week: ED activity and occupancy peak on Mondays in most centres.
Time of day: ED occupancy usually peaks in the evening, absolute mortality (deaths per shift) during the day, and relative mortality (deaths per presentation) overnight.
Inter-hospital transfer: Tertiary centres in particular are likely to delay inter-hospital transfers (ie, incoming patients) at times of overcrowding, or patients may be discharged early to their hospital of origin and death will not be recorded by the tertiary hospital.
Ambulance bypass: Where bypass is a significant feature of the emergency medical system, there will be a decrease in presentations at times of overcrowding, but possibly an increase in the relative mortality of ambulance patients, as the most critically ill are transported to hospital regardless of bypass status.
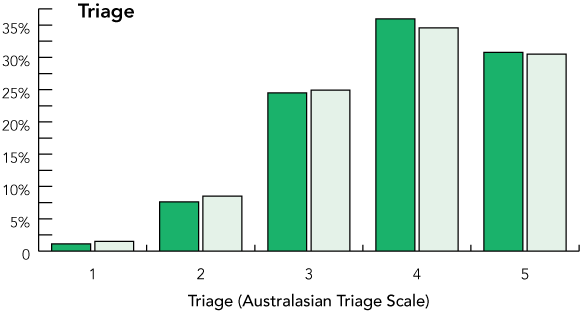
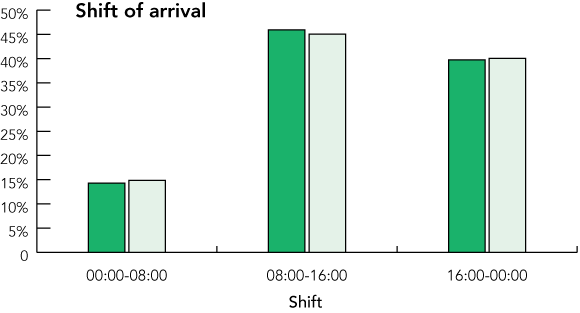
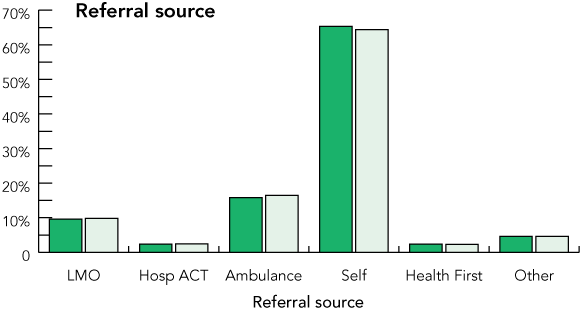
Of the 756 OC shifts, 20 were excluded because an insufficient number of similar NOC shifts was available. The two cohorts were well matched for baseline characteristics (Box 1, Box 2), although there was a small but significant excess of presentations categorised into more urgent triage categories,9 and a slight excess of presentations on night shift in the OC cohort. The latter is thought to represent delays in ambulance arrival on OC evening shifts.
Patients in the OC cohort received inferior care in terms of standard performance measures (Box 3). They were much less likely to commence treatment within Australasian College for Emergency Medicine triage threshold times,9 much more likely to leave without being assessed, and much more likely to experience access block.
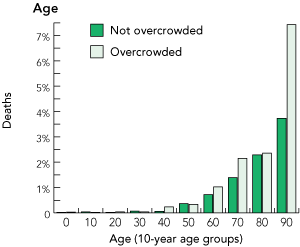
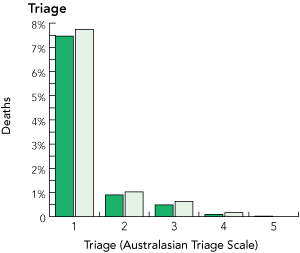
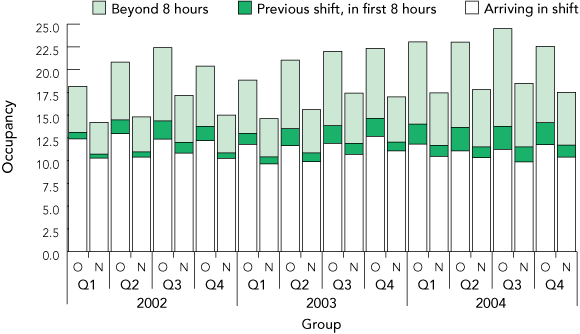
On subgroup analysis, the excess mortality was reasonably evenly distributed during the study period, although it was concentrated in older patients (Box 4). The mortality rate by triage category was significantly different between the groups (Box 4 and Box 5) (P = 0.014, excluding Category 5 because of low numbers). The mean occupancy was 21.6 in OC shifts and 16.4 in NOC shifts, with most of the excess being due to patients with prolonged ED stays (Box 6).
More patients presented during OC shifts, they were triaged as having slightly higher acuity, and they received care at a much lower performance level by standard measures. Given the methods used, the possibility that a “sicker” cohort of patients contributed to both overcrowding (as defined) and to mortality rates cannot be excluded. However, the patients presenting during each shift (in whom mortality was measured) accounted for only a small proportion of the difference in occupancy between OC and NOC shifts (15% greater occupancy by new arrivals in OC shifts), most being due to patients already in the ED from previous shifts (58% greater occupancy by previous shift patients in OC shifts) (Box 6).
Physical and staff capacity is reached or exceeded at times of ED overcrowding,12 and it is plausible that patients presenting at these times receive a lower quality of care because the available resources are stretched too thinly. ED overcrowding is caused by insufficient available inpatient beds (access block,13 or high hospital occupancy14), and it is also plausible that the situation in the ED represents a marker of global hospital dysfunction and that some deaths are related to inpatient issues such as inappropriate discharge or admission to an “outlier” ward (as opposed to the “home” ward where staff are experienced in the relevant specialty). If reduced quality of care is the cause of increased mortality, it is likely to also cause increased morbidity. Further studies using recognised quality audit tools are justified.
3 Standard performance indicators
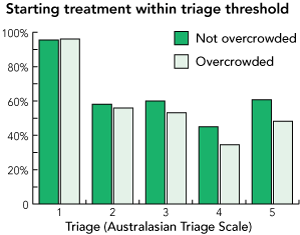
Proportion of patients presenting to the emergency department (ED) whose medical assessment and treatment began within the triage thresholds defined by the Australasian College for Emergency Medicine9 and the Australian Council on Healthcare Standards.10
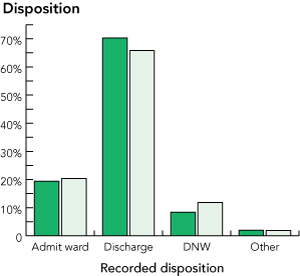
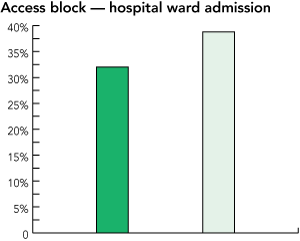
Access block (proportion of patients admitted after > 8 hours total time in ED), calculated here for admissions to the hospital wards only. The standard definition11 would have included some of the “Other” patients but these data were not available in this statistical study.
4 Distribution of 10-day mortality by subgroup. The y axis represents the actual number of deaths in each subgroup in overcrowded (OC) and not overcrowded (NOC) cohorts
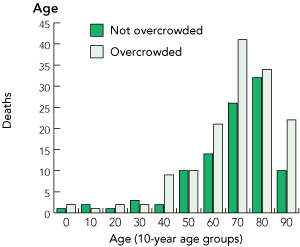
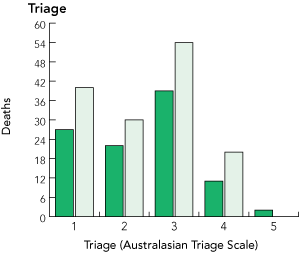
There were 7% more presentations and 43% more deaths in the OC cohort compared with the NOC cohort.
Received 3 July 2005, accepted 19 December 2005
- 1. Dunn R. Reduced access block causes shorter emergency department waiting times: an historical control observational study. Emerg Med (Fremantle) 2003; 15: 232-238.
- 2. Schull MJ, Morrison LJ, Vermeulen M, Redelmeier DA. Emergency department overcrowding and ambulance transport delays for patients with chest pain. CMAJ 2003; 168: 277-283.
- 3. Fernandes CM. Emergency department overcrowding: what is our response to the “new normal”? Acad Emerg Med 2003; 10: 1096-1097.
- 4. Richardson DB. The access block effect: relationship between delay to reaching an inpatient bed and inpatient length of stay. Med J Aust 2002; 177: 492-495. <MJA full text>
- 5. Liew D, Liew D, Kennedy MP. Emergency department length of stay independently predicts excess inpatient length of stay. Med J Aust 2003; 179: 524-526. <MJA full text>
- 6. Richardson DB. Validation of the refined overcrowding scale: a case-control study. [Abstract] Acad Emerg Med 2004; 12: 5.
- 7. Hwang U, Concato J. Care in the emergency department: how crowded is overcrowded? Acad Emerg Med 2004; 11: 1097-1101.
- 8. Richardson DB. Prospective validation of point occupancy definition of overcrowding. [Abstract] Acad Emerg Med 2004; 11: 462.
- 9. Australasian College for Emergency Medicine. The Australasian Triage Scale. Emerg Med (Fremantle) 2002; 14: 335-336.
- 10. Australian Council on Healthcare Standards. Clinical indicators — emergency medicine. Version 2. Sydney: ACHS; 2002.
- 11. Australasian College for Emergency Medicine. Standard terminology. Emerg Med (Fremantle) 2002; 14: 337-340.
- 12. Trzeciak S, Rivers EP. Emergency department overcrowding in the United States: an emerging threat to patient safety and public health. Emerg Med J 2003; 20: 402-405.
- 13. Fatovich DM, Nagree Y, Sprivulis P. Access block causes emergency department overcrowding and ambulance diversion in Perth, Western Australia. Emerg Med J 2005; 22: 351-354.
- 14. Forster AJ, Stiell I, Wells G, et al. The effect of hospital occupancy on emergency department length of stay and patient disposition. Acad Emerg Med 2003; 10: 127-133.





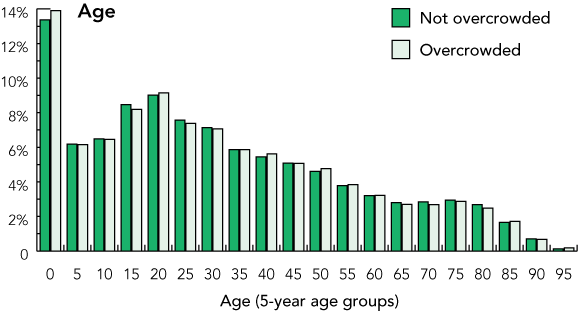
Abstract
Objective: To quantify any relationship between emergency department (ED) overcrowding and 10-day patient mortality.
Design and setting: Retrospective stratified cohort analysis of three 48-week periods in a tertiary mixed ED in 2002–2004. Mean “occupancy” (a measure of overcrowding based on number of patients receiving treatment) was calculated for 8-hour shifts and for 12-week periods. The shifts of each type in the highest quartile of occupancy were classified as overcrowded.
Participants: All presentations of patients (except those arriving by interstate ambulance) during “overcrowded” (OC) shifts and during an equivalent number of “not overcrowded” (NOC) shifts (same shift, weekday and period).
Main outcome measure: In-hospital death of a patient recorded within 10 days of the most recent ED presentation.
Results: There were 34 377 OC and 32 231 NOC presentations (736 shifts each); the presenting patients were well matched for age and sex. Mean occupancy was 21.6 on OC shifts and 16.4 on NOC shifts. There were 144 deaths in the OC cohort and 101 in the NOC cohort (0.42% and 0.31%, respectively; P = 0.025). The relative risk of death at 10 days was 1.34 (95% CI, 1.04–1.72). Subgroup analysis showed that, in the OC cohort, there were more presentations in more urgent triage categories, decreased treatment performance by standard measures, and a higher mortality rate by triage category.
Conclusions: In this hospital, presentation during high ED occupancy was associated with increased in-hospital mortality at 10 days, after controlling for seasonal, shift, and day of the week effects. The magnitude of the effect is about 13 deaths per year. Further studies are warranted.