"Access block" refers to the situation where patients requiring emergency hospital admission spend an unreasonable amount of time in an emergency department (ED) because they are unable to gain access to appropriate hospital inpatient beds.1,2 Access block is regarded as the major issue currently facing emergency medicine in Australasia.3
Access block is linked to increased ED waiting time for medical care4 and leads to ED overcrowding. This overcrowding is generally accepted to decrease efficiency and possibly quality of care2,3,5 and has also been linked to adverse events.6 However, there have been no published studies examining the relationship between access block and patient outcomes in hospital. Inpatient length of stay (LOS) is one of the simplest measures of hospital outcome and resource use. This study aimed to investigate the relationship between access block in the ED and inpatient LOS.
This was a retrospective cohort study of all patients admitted through the ED to an inpatient bed at the Canberra Hospital, Australian Capital Territory, during 1999. The hospital is a 500-bed mixed adult and paediatric tertiary hospital serving a population of about 500 000.
The hospital's information system (CARESYS7) was queried to identify all patients admitted with the ED as the referral source. These data were compared with a similar list generated from the hospital Emergency Department Information System (EDIS8). Where discrepancies were found between the databases, the patient's medical record was reviewed.
Patients who were admitted only to the ED and subsequently discharged or transferred to other hospitals were excluded, as were those who were already inpatients at the time of ED presentation.
Demographic and clinical patient data were derived from the EDIS dataset. I assessed stay in the ED, presence of access block and LOS using standard definitions from the Australasian College for Emergency Medicine,1 Australian Council for Healthcare Standards,9 and the National Health Data Dictionary.10
For each patient, total ED time was calculated as the difference to the nearest minute between the recorded time of arrival in the ED and the recorded time of transfer to a ward. Access block was defined as a total ED time of more than eight hours.
Hospital LOS was calculated as the number of midnights between transfer from the ED and discharge from hospital. For the purposes of the study, transfer from the ED was taken as the start of the admission, although it is hospital practice to perform the clerical process of admission in the ED for patients who have a prolonged delay to reaching an inpatient bed or are required to stay in the ED overnight. LOS of zero ("non-overnight" admission) was entered as one day.
Data were processed using a spreadsheet.11 LOS was compared between those who experienced access block and those who did not. To allow meaningful subgroup analysis, LOS values were truncated at a maximum of 10 days. To identify any possible artefact, calculations were repeated without truncation and with different definitions of LOS (including overall midnights in hospital and hours of stay).
The study was approved by the Australian Capital Territory Health Ethics Committee.
During 1999, there were 48 430 presentations to the ED, with 11 906 admissions eligible for the study. Patient records were consulted to resolve discrepancies between the source databases for 334 admissions (2.8%).
Mean total ED time was 4 h 28 m. Access block occurred in 919 admissions (7.7%), and the access-block group had a mean total ED time of 10 h 30 m, compared with 3 h 58 m in the no-block group.
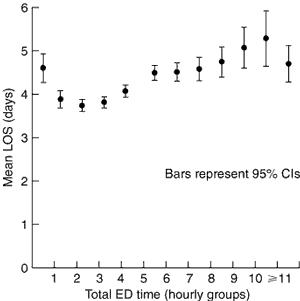
Mean LOS was 4.2 days (after LOS truncation at 10 days — in 14% of admissions) and 5.9 days (without truncation). The relationship between mean LOS and total ED time is shown in Box 1.
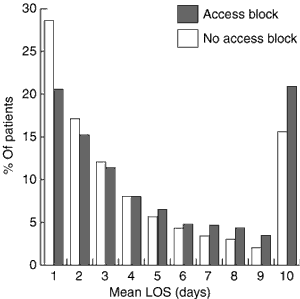
LOS distribution by presence of access block is shown in Box 2. The access-block group had a lower proportion of patients with LOS of one day than the no-block group (21% v 29%), but a higher proportion of patients with LOS of four or more days (54% v 49%; P = 0.03, χ2 test). Mean LOS in the access-block group was 4.9 days (95% CI, 4.7–5.1), compared with 4.1 days in the no-block group (95% CI, 4.0–4.2; P < 0.0001, t test). Repeat analyses with different definitions of LOS and without truncation at 10 days gave similar results.
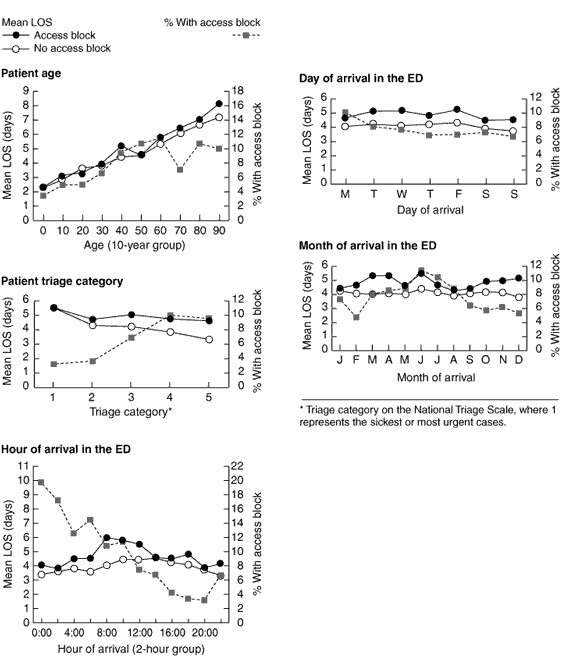
Mean LOS in the presence or absence of access block is shown in Box 3 by patient characteristics and times of arrival in the ED. LOS was longer in the access-block group than the no-block group in all age groups over 40 years in all triage categories except category 1 (the sickest patients on the National Triage Scale12), and for arrivals in the ED on all days of the week, in all months except January, and at most times of the day, with the effect greater during daylight hours. The percentage of cases with access block is also shown in Box 3. Generally, the group with the longest LOS did not have the highest percentage of cases with access block, although the difference in percentage with access block between the two least urgent triage categories was small.
Medical staff entered ED diagnoses from a shortlist available on the EDIS computer system. Mean LOS by a selection of diagnoses is shown in Box 4. LOS was longer in access-block patients across a wide range of diagnoses, although this trend reached significance only for respiratory and renal diagnoses.
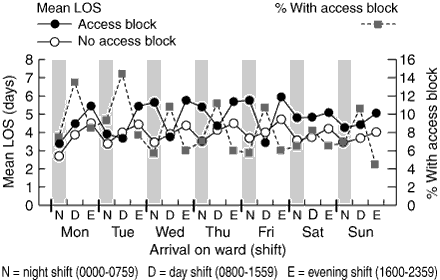
More detailed analysis of LOS by time of arrival on the inpatient ward (equivalent to time of ED departure) is shown in Box 5. There was no significant difference in LOS between the access-block and no-block groups among patients who arrived on the inpatient ward during "office hours" (weekdays, 0800 to 1600), but a significant difference among those who arrived outside these hours — 5.2 days (access-block group) v 4.1 days (no-block group) (Box 4).
Mine is the first study to demonstrate a relationship between access block in the ED and a measure of patient outcome outside this department. Patients who experienced access block had a mean inpatient LOS 0.8 days longer than those who had no access block. This amounted to 19% of the average LOS in the first 10 days after ED presentation. Considering the average additional 6.5 hours that access-block patients spent in the ED, this is more than 24 hours extra in hospital from ED presentation to discharge. Altogether, the excess inpatient LOS (compared to average no-block inpatient LOS) for access-block patients amounted to over 700 bed-days per year.
The access-block effect on LOS was relatively independent of the severity of patient illness and diagnosis, but appeared to be greatest in patients who arrived on inpatient wards outside office hours.
Proving an association does not prove cause and effect. Although the available data do not allow the reasons for the access-block effect on LOS to be identified, they allow some possible explanations to be examined.
The obvious possibility that access-block patients were "sicker", requiring longer "work-up" in the ED and then longer duration of care on the ward, appears to be refuted by the results. The access-block effect on LOS was seen in all triage categories except category 1 (the sickest patients), and also at all ages over 40 years, despite considerable differences in mean LOS between subgroups. Furthermore, in the subgroup analyses, the rate of access block was generally not highest in the group with the longest LOS.
It is also possible that some feature of presentation, such as time of arrival in the ED, causes both longer ED time and longer inpatient stay (eg, because of difficulty in accessing investigations). However, the access-block effect persisted across a wide range of patient characteristics and most times of arrival in the ED. Although both access block and LOS increased in June, this coincided with a period of recognised hospital overload.
A third possibility is that when it is difficult to access inpatient beds the mix of patients admitted may differ. Patients with minor conditions requiring only a short stay may be more likely to be treated with alternatives to inpatient admission (eg, discharge, admission to the ED only, or transfer elsewhere). This would account for the relative deficiency of patients with LOS of one day in the access-block group, but not for the excess of patients with LOS over seven days. Also, the low rate of access block (7.7% of all admissions from the ED) makes it unlikely that there were many times when large numbers were managed using alternatives to admission.
Fourthly, patients who experience access block may receive different treatment from the no-block group. For example, care during a prolonged stay in the ED may differ from that in an inpatient ward, or patients may be more likely to be admitted to outlying rather than "home" wards, where staffing or organisational issues may prolong LOS. Data on patient diagnoses were limited, but the access-block effect appeared to occur across a range of diagnostic categories. This possibility requires further investigation.
There were insufficient data to be certain if the relationship between LOS and total ED time was linear with outliers, or U-shaped with a gradually increasing "tail". An initial U-shape is credible: patients with very short ED times would not have been investigated in the ED, so are likely to have been "sicker" (eg, those transferred rapidly to theatre) than those with the "normal" ED time of 3–4 hours. Whatever the exact nature of the relationship, these data support the use of an ED time of eight hours as the threshold for access block — patient groups with ED time over this level had mean LOS exceeding that of all groups with shorter ED time.
A final possibility is that the access-block effect may be a function of the inpatient rather than the ED system of care. The strong relationship between the access-block effect and time of arrival on the inpatient ward, with the greatest effect for arrival during the evening, night or weekend shift, is the best evidence for this. It suggests that ward functions that occur in office hours may be associated with shorter LOS. For example, access-block patients arriving on the ward out of office hours are unlikely to be reviewed immediately by the regular inpatient team.
This study is limited by the nature of the data available, which derive from a single centre and include limited clinical details. A prospective case–control study would allow better identification of the factors that contribute to the access-block effect and should consider whether patients are managed with alternatives to inpatient admission and whether they are admitted to home or outlier wards, as well as recognised diagnostic coding. If the access-block effect occurs within Diagnosis Related Groups, it would have ramifications for funding models as well as major implications for management of hospital patient flow.
3: Mean length of stay (LOS), by patient characteristics and time of arrival in the emergency department (ED)
4: Mean length of stay (95% CI), by diagnosis* and time of arrival on the inpatient ward
Subgroup |
n |
% With access block |
No access block |
Access block |
|||||||
ED diagnosis (inclusions) |
|||||||||||
Abdominal pain (abdominal pain, cause not specified) |
179 |
15% |
3.65 (3.20–4.11) |
4.08 (2.86–5.29) |
|||||||
Surgical (acute fractures, acute abdomen) |
1489 |
7% |
4.15 (3.98–4.33) |
4.85 (4.20–5.52) |
|||||||
Overdose (all overdose/poisoning) |
116 |
13% |
2.72 (2.21–3.24) |
3.40 (1.66–5.14) |
|||||||
Cardiac (chest pain, AMI, angina) |
513 |
3% |
3.96 (3.69–4.22) |
5.64 (3.70–7.59) |
|||||||
Respiratory (asthma, pneumonia, COAD) |
815 |
6% |
4.12 (3.91–4.34)† |
5.61 (4.63–6.58)† |
|||||||
Renal (renal failure) |
51 |
10% |
6.61 (5.58–7.63)† |
10.00 (NC)† |
|||||||
Time of arrival on the inpatient ward |
|||||||||||
Office hours (0800–1600) |
1884 |
12% |
4.00 (3.84–4.16) |
3.94 (3.53–4.35) |
|||||||
Non-office hours |
10022 |
7% |
4.10 (4.04–4.17) |
5.17 (4.92–5.43) |
|||||||
Total |
11 906 |
7.7% |
4.09 (4.03–4.18) |
4.89 (4.65–5.09) |
|||||||
ED = emergency department. AMI = acute myocardial infarction. COAD = chronic obstructive airways disease. NC = not calculated (all LOS values truncated at 10 days). * Selected diagnostic groups entered by staff in the ED database. † Difference was statistically significant only for respiratory and renal diagnoses. |
|||||||||||
- Drew B Richardson1
- Emergency Department, Canberra Hospital, Garran, ACT.
None identified.
- 1. Australasian College for Emergency Medicine. Policy document — standard terminology. Emerg Med (Aust) 2002; 14: 337-340.
- 2. Integrated Bed Management Committee. Access block strategy. Sydney: New South Wales Health, 1999.
- 3. Baggoley C. President's message. Emerg Med (Aust) 1998; 10: 269-271.
- 4. Richardson DB. Association of access block with decreased ED performance [abstract]. Acad Emerg Med 2001; 8: 575-576.
- 5. Schneider S, Zwemer F, Doniger A, et al. Rochester New York: a decade of emergency department overcrowding. Acad Emerg Med 2001; 8: 1044-1050.
- 6. Erikson CA, McErlean M, Bartfield JM, Verdile VP. Relationship between maloccurrences and ED census and staffing [abstract]. Acad Emerg Med 2001; 8: 499.
- 7. CARESYS [computer program]. Christchurch NZ: Cardinal Healthcare Pty Ltd, 2000.
- 8. EDIS [computer program]. Version NT 7.3.6.4. Sydney: HAS Solutions Pty Ltd, 2000.
- 9. Australian Council on Healthcare Standards. Clinical indicators – emergency medicine. Version 2. Sydney: ACHS; 2002.
- 10. Australian Institute of Health and Welfare. National health data dictionary. Version 10. Canberra: AIHW, 2001: 415.
- 11. Microsoft Excel 97 [computer program]. Seattle, Wa: Microsoft Corporation, 1997.
- 12. Australasian College for Emergency Medicine. National triage scale. Emerg Med (Aust) 1994; 6: 145-146.





Abstract
Objectives: To investigate the relationship between access block in the emergency department (ED) (defined as total time from arrival to transfer from the ED over eight hours) and inpatient length of stay (LOS).
Design and setting: Retrospective cohort study of all admissions through the ED to a tertiary hospital in Canberra, Australian Capital Territory, during 1999.
Main outcome measures: Total time in the ED and LOS, calculated in days from ED departure to hospital discharge (non-overnight admissions were assigned LOS of one day, and all LOS were truncated at 10 days).
Results: 11 906 admissions were included, and 919 experienced access block (7.7%). Mean LOS was 4.9 days in those who experienced access block (95% CI, 4.7–5.1), compared with 4.1 days in the no-block group (95% CI, 4.0–4.2; P < 0.0001). Subgroup analysis showed that this "access block effect" occurred across different severities of illness and diagnoses. A strong relationship was found between longer LOS and arrival of access-block patients on the inpatient ward outside office hours (0800–1600 weekdays).
Conclusions: This is the first study to show an association between access block and a measure of outcome outside the ED. If the effect of access block on LOS is reproduced in other settings, there are major implications for hospital management.