Fifty years ago, cervical cancer was the number one cause of cancer death among women in developed countries. Today, it is relatively uncommon, ranking below the top 10 causes.1 However, Aboriginal and Torres Strait Islander women in Australia have not been part of this progress. Cervical cancer is still the number one cause of cancer death among these women, whose risk of death from cervical cancer is more than 10 times that of non-Indigenous women.2,3 These statistics are of particular concern, as cervical cancer is one of the most preventable of cancers: experts in Australia and overseas have estimated that regular screening with Pap smears can prevent 90% of squamous cell carcinomas of the cervix.4 To date, information on Pap smear screening of Indigenous women has been limited to data from before-and-after case studies of successful interventions in a single community, and there have been only limited comparisons with non-Indigenous women.5-12
Each State and Territory of Australia has a Pap smear registry. The functions of the registries include reminding women to attend for screening, providing a "safety net" to ensure follow-up of women with abnormal smears, keeping a record of women's cervical screening histories, assisting laboratories in quality assurance programs, and monitoring participation. It was initially hoped that the registries could be used to monitor cervical cancer screening among Indigenous women. Unfortunately, this has not occurred, mainly because of the difficulty of capturing "Indigenous" status on pathology forms.13
The purpose of our study was to determine the cervical screening participation rate among women living in rural and remote Indigenous communities in Queensland. We also wished to examine variation in participation across the communities.
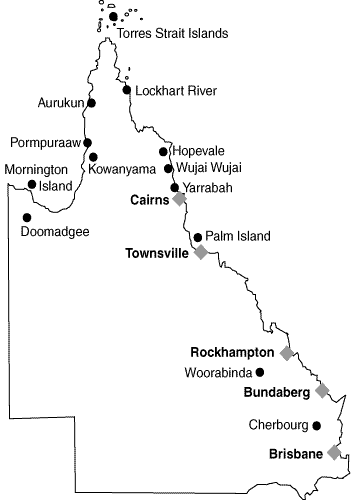
We obtained data from the Queensland Health Pap Smear Registry for the period March 1999 to February 2001. Our analysis was restricted to women aged 20–69 years, as this is the target group for the program.14 Women living in 13 discrete rural and remote Indigenous communities (Box 1) were identified, based on their reported place of usual residence, for any smear taken during the 24-month period. By identifying Indigenous women in this way (rather than by "Indigenous" status as reported on pathology forms) we were able to present information on screening participation for a large number of Indigenous women in several different communities. We obtained permission from the Aboriginal and Torres Strait Islander Health Unit of Queensland Health to analyse community-specific data. In presenting our results, we have concealed the identity of individual communities.
Based on self-reported Indigenous status, 80% of people living in the Torres Strait Islands and 92% living in Aboriginal communities on the mainland are Indigenous.15 Women in the rest of Queensland, of which less than 2% are Indigenous,15 were used as the comparison group. Indigenous women in our study comprise a fifth of all Indigenous women in Queensland.15 Women from other States who were screened in Queensland were omitted from the analysis.
In keeping with the national performance indicators,14 we calculated the "biennial participation percentage" (ie, the proportion of women undergoing screening in the two-year period studied) by dividing the number of women who had had at least one Pap smear in the two-year period by the number of eligible women (based on population data, adjusted for age-specific hysterectomy fractions [Box 2]).
Population data for the communities studied were based on non-confidential information (aggregated by age) from CentreLink. Official population estimates from the Australian Bureau of Statistics for areas as small as the Indigenous communities were only available for the year 1996, and we considered these too out-of-date to be used in our study. CentreLink was considered the most accurate source of data to estimate the number of women aged 20–69 living in the rural and remote Indigenous communities. The social circumstances in these communities are such that duplication of identity in the CentreLink database is considered extremely rare.
Population estimates for the rest of Queensland were based on the 2000 estimated resident population provided by the Australian Bureau of Statistics,19 after subtracting the populations of the Indigenous communities.
All populations considered in our study were adjusted for the age-specific proportions of women who had had a hysterectomy. For non-Indigenous women we used the results from the 1997 Queensland Health Women's Health Survey, a statewide telephone survey of 1100 women.18 For each five-year age group the hysterectomy fractions from this survey were similar to those from the 1995 National Health Survey16 (which are currently used in national reporting14) and the 1997 NSW Health Survey17 (Box 2).
Hysterectomies are thought to be less common among Indigenous than non-Indigenous women.14 To examine this issue, we obtained hospital discharge data on the incidence of hysterectomies for women living in the 13 Indigenous communities for the five-year period 1995/1996 to 1999/2000. This is not a long enough time series to estimate hysterectomy fractions (prevalence) for Indigenous women.20 However, it did confirm that the incidence of hysterectomy among Indigenous women (1.6 per 1000 women) was lower than that for women in the rest of Queensland (5.3 per 1000 women). There was no significant variation in hysterectomy rates across the 13 Indigenous communities (Mantel–Haenszel test for heterogeneity: χ2 = 15.2; 12 degrees of freedom; P = 0.30). To estimate the hysterectomy fractions for Indigenous women, we applied the relative risk for the lower incidence of hysterectomy for Indigenous versus non-Indigenous women to the hysterectomy fractions from the Queensland Health Women's Health Survey (Box 2). After applying the hysterectomy fractions we were left with 7795 eligible women in the Indigenous communities and 942 403 eligible women in the rest of Queensland.
We then ran a series of simulations to determine the effect of using different hysterectomy fractions. The estimates of participation in the Indigenous communities were two percentage points higher when we used the unadjusted fractions from the Queensland Health Women's Health Survey. The use of different hysterectomy fractions has little effect on the estimated participation percentage for Indigenous women, as they are relatively young and within the lower age categories the hysterectomy fractions are small and do not vary much (Box 2). The ranking of the communities and the variation across communities also did not change with the use of different hysterectomy fractions.
As in the other States, registration on the Queensland Health Pap Smear Registry is voluntary and women may decide not to be included (ie, "opt off"). The opt-off rate across the whole of Queensland is 1.5%, which is similar to the rates in other States.16 However, anecdotal evidence suggested that the opt-off rate was higher in some of the Indigenous communities because of concerns about privacy. To allow for this possibility, we obtained non-identifying information from relevant pathology laboratories for women in the Indigenous communities who elected to opt off. This consisted only of counts of the women who opted off and their ages (grouped into five-year categories). This information changed the overall estimate of participation by less than one percentage point and did not affect the ranking of the individual communities or the variation across communities. The results presented here are based only on data from the Queensland Health Pap Smear Registry and exclude women who opted off.
The average age of Indigenous women is much lower than the average age of non-Indigenous women — this is the case even when the analysis is restricted to the target group for cervical cancer screening (20–69 years). For example, 65.3% of women who live in the 13 Indigenous communities are under 40 years old, compared with 34.6% of women in the rest of Queensland. To take into account variation in screening rates by age, we directly age-standardised the participation percentages based on 1991 Australian standard population data.21 The national cervical screening program uses the same statistical procedure in its reports.14
We used the statistical package STATA22 to fit a random-effects, logistic regression model with five-year age groups as fixed effects and Indigenous community as a random effect. This is a way of partitioning the variation in the participation percentages across the 13 communities into that due to chance (binomial variation) and that due to the true underlying differences among the communities (systematic variation). It is the latter variation that was of interest in our study. (If the 95% CI associated with the systematic variation does not include zero, then the variation across communities is considered to be due to factors other than the play of chance.)
Outside the Indigenous communities, the biennial participation percentage for Queensland during the two-year period studied was 59.1% (95% CI, 59.0%–59.2%). This is similar to the figure of 59.2% reported from New South Wales for 1999–2000,23 but lower than the percentages reported from some other States (eg, Victoria, 69.2%24).
Overall, the biennial participation percentage for women living in the Indigenous communities was 41.1%. This was 30% lower (risk ratio, 0.70; 95% CI, 0.67–0.72) than that for the rest of Queensland (Box 3). However, there was considerable variation among communities (range, 19.9%–63.5%) (Box 4). The estimate of the systematic variation from the random-effects model was 0.522 (95% CI, 0.482–0.566), indicating that the variation across communities could not be attributed to chance alone.
Our study provides information on participation in cervical cancer screening for the 7795 eligible women who live in 13 rural and remote Indigenous communities in Queensland. Their overall participation rate was 30% lower than that for the rest of the State. This is of particular concern given that among these women mortality rates from cervical cancer are at least 10 times higher than the State average.3
We also found considerable variation across the communities that could not be attributed solely to chance. Our study did not determine the reasons for the differences in cervical screening rates among the 13 communities. However, it is important to note that in the four communities with participation rates of over 50% cervical cancer screening was seen as part of primary healthcare. Two features of this were a commitment to training primary healthcare workers and the active maintenance of local information systems. Communities with lower participation did not have these features.
Interestingly, the few case studies of interventions that increased screening coverage among Indigenous women have also emphasised primary healthcare. For example, a report from an Aboriginal medical service in Darwin recommended that screening should be part of primary healthcare, as this provided scope for opportunistic screening.9 Another report from a remote community in the Northern Territory stressed the importance of a culturally appropriate, community-based program integrated with the local primary healthcare service.10 A description of a screening program in remote Western Australia emphasised training Aboriginal health workers and providing women with a choice of service provider.11
Our cautious inferences and those from case studies are not definitive. For example, there may be differences among communities in our study, other than the way healthcare services are delivered, that might affect participation. Ideally, the strategy of strengthening primary healthcare to improve participation in cervical cancer screening should be tested in a large longitudinal study involving multiple communities (randomised if possible).
Besides low participation, other problems that affect cervical screening in Indigenous communities include the relatively high proportion of technically unsatisfactory smears (mostly due to inflammation) and difficulties following up women with screen-detected abnormalities. These and other problems are not discussed here, but all require attention and perhaps separate solutions.
The statistically significant variation in participation across the communities in our study suggests that the problem of low participation among Indigenous women is not intractable. Achieving participation rates similar to the highest percentages found in our study would be of major benefit to Indigenous women.
2: Hysterectomy fractions from several Australian surveys (ie, proportion of women who have had a hysterectomy, by age group)
Age (years) |
|||||||||||
Survey |
20–24 |
25–29 |
30–34 |
35–39 |
40–44 |
45–49 |
50–54 |
55–59 |
60–64 |
65–69 |
|
1995 National Health Survey16 |
0.2% |
0.7% |
2.0% |
8.1% |
14.8% |
20.9% |
31.5% |
31.5% |
32.2% |
31.2% |
|
1997 NSW Health Survey17 |
0.1% |
0.9% |
1.9% |
3.8% |
9.9% |
18.6% |
25.1% |
36.2% |
33.4% |
37.5% |
|
1997 Queensland Health Women's Health Survey*18 |
0.1% |
0.9% |
2.1% |
4.0% |
7.0% |
13.0% |
35.5% |
32.7% |
35.0% |
39.0% |
|
Estimates for Indigenous communities†‡ |
0 |
0 |
0.6% |
1.2% |
2.1% |
3.9% |
10.8% |
9.9% |
10.6% |
11.8% |
|
* Used to adjust the populations of non-Indigenous women in our survey. † Used to adjust the populations of women in the 13 Indigenous communities in our survey. ‡ Based on the 1997 Queensland Health Women's Health Survey and the incidence of hysterectomies among women in the 13 Indigenous communities, according to unpublished data from the Queensland Hospital Admitted Patients data collection. |
|||||||||||
3: Participation in cervical cancer screening over a two-year period by women aged 20–69 years in 13 rural and remote Indigenous communities compared with the rest of Queensland
Indigenous communities |
Rest of Queensland |
||||||||||
Number of women eligible for screening |
7795 |
942 403 |
|||||||||
Number of women screened |
3206 |
562 753 |
|||||||||
Age-standardised* biennial participation percentage† (95% CI) |
41.5% (40.2%–42.7%) |
59.1% (59.0%–59.2%) |
|||||||||
Age-adjusted‡ risk ratio (95% CI) |
0.70 (0.67–0.72) |
1 |
|||||||||
* Directly age-standardised to the 1991 Australian standard population.21† Biennial participation percentage = proportion of women undergoing screening over a two-year period. ‡ Age-adjusted using the Mantel–Haenszel technique. |
|||||||||||
4: Age-standardised* biennial participation percentages† (with 95% CI) for 13 rural and remote Indigenous communities
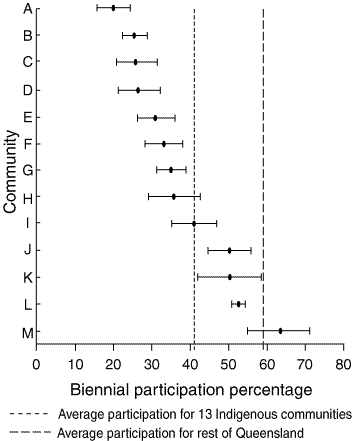
* Directly age-standardised to the 1991 Australian standard population.21 † Biennial participation percentage = proportion of women undergoing cervical screening over a two-year period.
Received 3 April 2002, accepted 5 July 2002
- Michael D Coory1
- Jennifer M Muller2
- Nathan A M Dunn3
- Patricia S Fagan4
- 1 For editorial comment, see Hunt and Geia
- 2 Queensland Health, Brisbane, QLD.
- 3 Office for Aboriginal and Torres Strait Islander Health, Commonwealth Department of Health and Ageing, Canberra City, ACT.
None identified.
- 1. Austin RM, McLendon WW. The Papanicolaou smear. JAMA 1997; 277: 754-755.
- 2. O'Brien ED, Bailie RS, Jelfs PL. Cervical cancer mortality in Australia: contrasting risk by Aboriginality, age and rurality. Int J Epidemiol 2000; 29: 813-816.
- 3. Coory M, Thompson A, Ganguly I. Cancer among people living in rural and remote Indigenous communities in Queensland. Med J Aust 2000; 173: 301-304.
- 4. Australian Health Ministers' Advisory Committee. Cervical cancer screening in Australia: options for change. Canberra: AGPS, 1991.
- 5. Wain GV. Cervical cancer screening in Australia: let's keep it in perspective. Med J Aust 1996; 164: 261-262.
- 6. Guest C, Mitchell H, Plant A. Cancer of the uterine cervix and screening of Aboriginal women. Aust N Z J Obstet Gynaecol 1990; 30: 243-247.
- 7. Reath JS, Patel M, Moodie R. Cervical cytology in central Australian Aboriginal women. Aust Fam Physician 1991; 20: 601-606.
- 8. Mak DB, Straton JA. The Fitzroy Valley Pap Smear Register. Med J Aust 1993; 158: 163-166.
- 9. Hunt JM, Gless GL, Straton JA. Pap smear screening at an urban Aboriginal health service: report of a practice audit and an evaluation of recruitment strategies. Aust N Z J Pubic Health 1998; 22: 720-725.
- 10. Gilles MT, Crewe S, Granites IN, Coppola A. A community-based cervical screening program in a remote Aboriginal community in the Northern Territory. Aust N Z J Public Health 1995; 19: 477-481.
- 11. Mak D, Straton JA. Effects of sustainability of a cervical screening program in remote Aboriginal Australia. Aust N Z J Public Health 1997; 21: 67-70.
- 12. Reath J, Usherwood T. Improving cervical screening in a remote Aboriginal community. Aust N Z J Public Health 1998; 22: 659-663.
- 13. Baille R, Sibthorpe B, Anderson I, Smith L. Data for diagnosis, monitoring and treatment in Indigenous health: the case of cervical cancer. Aust N Z J Public Health 1998; 22: 303-306.
- 14. Cervical screening in Australia, 1999-2000. Canberra: Australian Institute of Health and Welfare, 2002.
- 15. Australian Bureau of Statistics. Census of population and housing. CDATA96. Canberra: ABS, 1996. (Catalogue No. 2019.0.)
- 16. Australian Bureau of Statistics. National Health Survey: summary of results. Canberra: ABS, 1995. (Catalogue No. 4364.0.)
- 17. New South Wales Department of Health. Cervical cancer screening in New South Wales: annual statistical report 1999. Westmead, NSW: Cervical Screening Program, 2001.
- 18. Queensland Health. Women's Health Survey: primary results. Brisbane: Queensland Health, 1997.
- 19. Australian Bureau of Statistics. Estimated resident population by age and sex: Australian States and Territories, 2000. Canberra: ABS, 2000. (Catalogue No. 3201.0.)
- 20. Taylor R, Rushworth RL. Hysterectomy fractions in New South Wales, 1971–2006. Aust N Z J Public Health 1998; 22: 759-764.
- 21. Australian Bureau of Statistics. Estimated resident population by age and sex: Australian States and Territories, June 1987 to June 1992. Canberra: ABS, 1995. (Catalogue No. 3201.0.)
- 22. StataCorp. STATA statistical software, Release 7.0. College Station, Texas: StataCorp, 2001.
- 23. Wain G, Ross J, Taylor R, et al. Cervical cancer screening in New South Wales. Annual statistical report 2000. NSW Cervical Screening Program and NSW Pap Test Register. Sydney: NSW Department of Health, 2001.
- 24. Mitchell H, Higgins V, Burrows C. Victorian Cervical Cytology Registry statistical report 1999. Melbourne: Victorian Cervical Cytology Registry, 2000.





Abstract
Objective: To investigate the extent of participation in cervical cancer screening among women who live in discrete rural and remote Indigenous communities in Queensland.
Design: Descriptive analysis of data from the Queensland Health Pap Smear Registry for the period March 1999 to February 2001.
Subjects: Women aged 20–69 years who had given their address of usual residence as one of 13 discrete rural and remote Indigenous communities in Queensland.
Main outcome measures: Proportion of women who participated in cervical screening over a two-year period ("biennial participation percentage") and variation in participation across the 13 communities.
Results: Overall, the biennial participation percentage in the Indigenous communities was 41.1%. This was 30% lower (risk ratio, 0.70; 95% CI, 0.67–0.72) than that for the rest of Queensland. There was statistically significant variation among communities, with biennial participation percentage ranging from 19.9% to 63.5%.
Conclusions: The variation in participation across the communities suggests that the problem of low participation among Indigenous women is not intractable. Achieving participation rates similar to the highest rates found in our study would be of major benefit to Indigenous women.